Abstract
Purpose of Review
A biomarker point-of-care (POC) test that supplements the psychiatric interview and improves detection of patients at risk for suicide would be of value, and assays of autonomic nervous system (ANS) activity would satisfy the logistical requirements for a POC test. We performed a selective review of the available literature of ANS assays related to risk for suicide.
Recent Findings
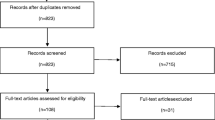
We searched PubMed and Web of Science with the strategy: “suicide OR suicidal” AND “electrodermal OR heart rate variability OR pupillometry OR pupillography.” The search produced 119 items, 21 of which provided original data regarding ANS methods and suicide. These 21 studies included 6 for electrodermal activity, 14 for heart rate variability, and 1 for the pupillary light reflex. The 21 papers showed associations between ANS assays and suicide risk in a direction suggesting underlying hyperarousal in patients at risk for suicide.
Summary
ANS assays show promise for future development as POC tests to supplement clinical decision making in estimating risk for suicide.

Similar content being viewed by others
Data Availability
Not applicable.
Code Availability
Not applicable.
References
Ivey-Stephenson AZ, Crosby AE, Jack SPD, Haileyesus T, Kresnow-Sedacca M-J. Suicide trends among and within urbanization levels by sex, race/ethnicity, age group, and mechanism of death - United States 2001–2015. MMWR Surveill Summ. 2017;66(18):1–9.
Stone DM, Simon TR, Fowler KA, Kegler SR, Yuan K, Holland KM, et al. Vital Signs: Trends in State Suicide Rates - United States 1999–2016 and Circumstances Contributing to Suicide - 27 States, 2015. MMWR Morb Mortal Wkly Rep. 2018;67(22):617–24.
Drapeau C, McIntosh J. U.S.A. suicide: 2018 official data. American Assoc Suicidology. 2020. http://www.suicidology.org.
Center for Disease Control and Prevention. Underlying Cause of Death, 1999-2019 Results 2020 [Available from: https://wonder.cdc.gov/controller/datarequest/D76;jsessionid=41EF14BB836E66D863EB056ABD50.
McCall W, Black C. The link between suicide and insomnia: theoretical mechanisms. Curr Psychiatry Rep. 2013;15:389.
Bae S, Lee Y, Cho IH, Kim S, Im J, Cho S. Risk factors for suicidal ideation of the general population. J Korean Med Sci. 2013;28:602–7.
Arsenault-Lapierre G, Kim C, Turecki G. Psychiatric diagnoses in 3275 suicides: a meta-analysis. BMC Psychiatry. 2004;4:37.
Blair-West GW, Cantor CH, Mellsop GW, Eyeson-Annan ML. Lifetime suicide risk in major depression: sex and age determinants. J Affect Disord. 1999;55(2–3):171–8.
Palmer BA, Pankratz VS, Bostwick JM. The lifetime risk of suicide in schizophrenia: a reexamination. Arch Gen Psychiatry. 2005;62(3):247–53.
Schaffer A, Sinyor M, Kurdyak P, Vigod S, Sareen J, Reis C, et al. Population-based analysis of health care contacts among suicide decedents: identifying opportunities for more targeted suicide prevention strategies. World Psychiatry. 2016;15(2):135–45.
Bernecker S, Zorumski K, Gutierrez P, Joiner T, King A, Liu H, et al. Predicting suicide attempts among soldiers who deny suicidal ideation in the Army Study to Assess Risk and Resilience in Servicemembers (Army STARRS). Behav Res Ther. 2019;120: 103350. https://doi.org/10.1016/j.brat.2018.11.018.
Williams C, Davidson J, Montgomery I. Impulsive suicidal behavior. J Clin Psychol. 1980;36:90–4.
Simon T, Swann A, Powell K, Potter L, Kresnow M-J, O’Carroll P. Characteristics of impulsive suicide attempts and attempters. Suicide Life Threat Behav. 2001;32(s1):49–59.
Deisenhammer E, Ing C-M, Strauss R, Kemmler G, Hinterhuber H, Weiss E. The duration of the suicidal process: how much time is left for intervention between consideration and accomplishment of a suicide attempt? J Clin Psychiatry. 2009;70(1):19–24.
Cummins B, Ligler F, Walker G. Point-of-care diagnostics for niche applications. Biotechnol Adv. 2016;34(3):161–76.
Price C. Point of care testing. BMJ. 2001;322:1285–8.
Shaw J. Practical challenges related to point of care testing. Pract Lab Med. 2016;4:22–9.
Fryback D, Thornbury J. The efficacy of diagnostic imaging. Med DecisMaking. 1991;11:88–94.
Zheng L, Wang O, Hao S, Ye C, Liu M, Xia M, et al. Development of an early-warning system for high risk patients for suicide attempt using deep learning and electronic health records. Transl Psychiatry. 2020;10:72. https://doi.org/10.1038/s41398-020-0684-2.
Roy A, Nikolitch K, McGinn R, Jinah S, Klement W, Kaminsky Z. A machine learning approach predicts future risk to suicidal ideation from social media data. NPJ Digit Med. 2020;3:78. https://doi.org/10.1038/s41746-020-0287-6.
Jaroszewski A, Morris R, Nock M. Randomized controlled trial of an online machine learning-driven risk assessment and intervention platform for increasing the use of crisis services. J Consult Clin Psychol. 2019;87(4):370–9.
Desmyter S, van Heeringen C, Audenaert K. Structural and functional neuroimaging studies of the suicidal brain. Prog Neuropsychopharmacol Biol Psychiatry. 2011;35:796–808.
Calati R, Nemeroff C, Lopez-Castroman J, Cohen L, Galynker I. Candidate biomarkers of suicide crisis syndrome: what to test next? A concept paper Int J Neuropsychopharmacol. 2020;23(3):192–5.
Niculescu AB, Le-Niculescu H, Levey DF, Phalen PL, Dainton HL, Roseberry K, et al. Precision medicine for suicidality: from universality to subtypes and personalization. Mol Psychiatry. 2017;22(9):1250–73.
Ribeiro J, Yen S, Joiner T, Siegler I. Capability for suicide interacts with states of heightened arousal to predict death by suicide beyond the effects of depression and hopelessness. J Affect Disord. 2015;188:53–9.
Johnson S, Elliott M, Carver C. Impulsive responses to positive and negative emotions: parallel neurocognitive correlates and their implications. Biol Psychiatry. 2020;87:338–49.
Harle K, Shenoy P, Paulus M. The influence of emotions on cognitive control: feelings and beliefs - where do they meet? Front Hum Neurosci. 2013;7:508. https://doi.org/10.3389/fnhum.2013.00508.
Cha C, Najmi S, Park J, Finn C, Nock M. Attentional bias towards suicide-related stimuli predicts suicidal behavior. J Abnorm Psychol. 2010;119:616–22.
Nock M, Park J, Finn C, Deliberto T, Dour H, Banaji M. Measuring the suicidal mind: implicit cognition predicts suicidal behavior. Psychol Sci. 2010;21(4):511–7.
Randall J, Rowe B, Dong K, Nock M, Colman I. Assessment of self-harm risk using implicit thoughts. Psychol Assess. 2013;25:714–21.
Pollock L, Williams J. Problem-solving in suicide attempters. Psychol Med. 2004;34:163–7.
Keilp J, Sackeim H, Brodsky B, Oquendo M, Malone K, Mann J. Neuropsychological dysfunction in depressed suicide attempters. Am J Psychiatry. 2001;158:735–41.
Keilp J, Gorlyn M, Russell M, Oquendo M, Burke A, Harkavy-Friedman J, et al. Neuropsychological function and suicidal behavior: attention control memory and executive dysfunction in suicide attempt. Psychol Med. 2013;43:539–51.
Keilp J, Gorlyn M, Oquendo M, Burke A, Mann J. Attention deficit in depressed suicide attempters. Psychiatry Res. 2008;159:7–17.
Berridge C. Noradrenergic modulation of arousal. Brain Res Rev. 2008;58(1):1–17.
Carter JR, Grimaldi D, Fonkoue IT, Medalie L, Mokhlesi B, Cauter EV. Assessment of Sympathetic Neural Activity in Chronic Insomnia: Evidence for Elevated Cardiovascular Risk. Sleep. 2018;41(6):zsy048. https://doi.org/10.1093/sleep/zsy048.
Lelkes Z, Porkka-Heiskanen T, Stenberg D. Cholinergic basal forebrain structures are involved in the mediation of the arousal effect of noradrenaline. J Sleep Res. 2013;22:721–6.
Sander C, Hensch T, Wittekind D, Bottger D, Hegerl U. Assessment of wakefulness and brain arousal regulation in psychiatric research. Neuropsychobiology. 2015;72:195–205.
Vallbo A, Hagbarth K, Wallin B. Microneurography: how the technique developed and its role in the investigation of the sympathetic nervous system. J Appl Physiol. 2004;96:1262–9.
Thorell L, Wolfersdorf M, Straub R, Steyer J, Hodgkinson S, Kaschka W. Electrodermal hyporeactivity as a trait marker for suicidal propensity in uni- and bipolar depression. J Psychiatric Res. 2013;47:1925–31.
Sarchiapone M, Gramaglia C, Iosue M, Carli V, Serretti A, Marangon D, et al. The association between electrodermal activity (EDA) depression and suicidal behavior: a systematic review and narrative synthesis. BMC Psychiatry. 2018;18:22. https://doi.org/10.1186/s12888-017-1551-4.
Jandl M, Steyer J, Kaschka WP. Suicide risk markers in major depressive disorder: a study of electrodermal activity and event-related potentials. J Affect Disord. 2010;123(1–3):138–49.
Thorell LH. Valid electrodermal hyporeactivity for depressive suicidal propensity offers links to cognitive theory. Acta Psychiatr Scand. 2009;119(5):338–49.
Edman G, Asberg M, Levander S, Schalling D. Skin conductance habituation and cerebrospinal fluid 5-hydroxyindoleacetic acid in suicidal patients. Arch Gen Psychiatry. 1986;43(6):586–92.
Wolfersdorf M, Straub R. Electrodermal reactivity in male and female depressive patients who later died by suicide. Acta Psychiatr Scand. 1994;89(4):279–84.
Keller F, Wolfersdorf M, Straub R, Hole G. Suicidal behaviour and electrodermal activity in depressive inpatients. Acta Psychiatr Scand. 1991;83(5):324–8.
Dawson ME, Schell AM. What does electrodermal activity tell us about prognosis in the schizophrenia spectrum? Schizophr Res. 2002;54(1–2):87–93.
Schell AM, Dawson ME, Rissling A, Ventura J, Subotnik KL, Gitlin MJ, et al. Electrodermal predictors of functional outcome and negative symptoms in schizophrenia. Psychophysiology. 2005;42(4):483–92.
Sarchiapone M, Iosue M, Carli V, Amore M, Baca-Garcia E, Batra A, et al. EUDOR-A multi-centre research program: A naturalistic, European Multi-centre Clinical study of EDOR Test in adult patients with primary depression. BMC Psychiatry. 2017;17(1):108.
Zuromski KL, Cero I, Witte TK. Insomnia symptoms drive changes in suicidal ideation: a latent difference score model of community adults over a brief interval. J Abnorm Psychol. 2017;126(6):739–49.
Chesin M, Cascardi M, Tsang W, Smith S. Blunted arousal in response to psychological stress is associated with current suicide ideation. Arch Suicide Res. 2019;24:S381–90.
Hill LK, Hu DD, Koenig J, Sollers JJ 3rd, Kapuku G, Wang X, et al. Ethnic differences in resting heart rate variability: a systematic review and meta-analysis. Psychosom Med. 2015;77(1):16–25.
McNames J, Aboy M. Reliability and accuracy of heart rate variability metrics versus ECG segment duration. Med Biol Eng Comput. 2006;44(9):747–56.
Munoz ML, van Roon A, Riese H, Thio C, Oostenbroek E, Westrik I, et al. Validity of (Ultra-) Short Recordings for Heart Rate Variability Measurements. PLoS One. 2015;10(9):e0138921.
Wilson S, Chesin M, Fertuck E, Keilp J, Brodsky B, Mann J, et al. Heart rate variability and suicidal behavior. Psychiatric Res. 2016;240:241–7.
Tsypes A, James KM, Woody ML, Feurer C, Kudinova AY, Gibb BE. Resting respiratory sinus arrhythmia in suicide attempters. Psychophysiology. 2018;55(2):e12978.
Forkmann T, Meessen J, Teismann T, Sutterlin S, Gaugel S, Mainz V. Resting vagal tone is negatively associated with suicide ideation. J Affect Disord. 2016;194:30–2.
Chang C, Tzeng N, Kao Y, Yeh C, Chang H. The relationships of current suicidal ideation with inflammatory markers and heart rate variability in unmedicated patients with major depressive disorder. Psychiatric Res. 2017;258:449–56.
Adolph D, Teismann T, Forkmann T, Wannemuller A, Margraf J. High frequency heart rate variability: evidence for a transdiagnostic association with suicide ideation. Biol Psychiatry. 2018;138:165–71.
Lin Y, Lin C, Sun IW, Hsu CC, Fang CK, Lo MT, et al. Resting respiratory sinus arrhythmia is related to longer hospitalization in mood-disordered repetitive suicide attempters. World J Biol Psychiatry. 2015;16(5):323–33.
Sheridan DC, Baker S, Dehart R, Lin A, Hansen M, Tereshchenko LG, et al. Heart Rate Variability and Its Ability to Detect Worsening Suicidality in Adolescents: A Pilot Trial of Wearable Technology. Psychiatry Investig. 2021;18(10):928–35.
Song B, Yoo S, Kang H, Byeon S, Shin S, Hwang E, et al. Post-traumatic stress disorder, depression, and heart-rate variability among North Korean defectors. Psychiatry Investig. 2011;8(4):297–304.
Lee D, Baek JH, Cho YJ, Hong KS. Association of Resting Heart Rate and Heart Rate Variability With Proximal Suicidal Risk in Patients With Diverse Psychiatric Diagnoses. Front Psychiatry. 2021;12:652340.
Khandoker AH, Luthra V, Abouallaban Y, Saha S, Ahmed KI, Mostafa R, et al. Predicting depressed patients with suicidal ideation from ECG recordings. Med Biol Eng Comput. 2017;55(5):793–805.
Yang X, Daches S, George CJ, Kiss E, Kapornai K, Baji I, et al. Autonomic correlates of lifetime suicidal thoughts and behaviors among adolescents with a history of depression. Psychophysiology. 2019;56(8):e13378.
James KM, Woody ML, Feurer C, Kudinova AY, Gibb BE. Disrupted physiological reactivity among children with a history of suicidal ideation: Moderation by parental expressed emotion-criticism. Biol Psychol. 2017;130:22–9.
Chang H, Chang C, Chen C, Kuo T, Lu R, Huang S. Heart rate variability in patients with fully remitted major depressive disorder. Acta Neuropsychiatr. 2013;25(1):33–42.
Clamor A, Lincoln TM, Thayer JF, Koenig J. Resting vagal activity in schizophrenia: meta-analysis of heart rate variability as a potential endophenotype. Br J Psychiatry. 2016;208(1):9–16.
Wang HT, Yang CM, Chen KR, Chueh KH. Relationship between heart rate variability and aggressive behavior among patients with schizophrenia hospitalized in acute wards. Perspect Psychiatr Care. 2020;56(2):321–9.
Rachow T, Berger S, Boettger MK, Schulz S, Guinjoan S, Yeragani VK, et al. Nonlinear relationship between electrodermal activity and heart rate variability in patients with acute schizophrenia. Psychophysiology. 2011;48(10):1323–32.
Kelbsch C, Strasser T, Chen Y, Feigl B, Gamlin P, Kardon R, et al. Standards in pupillography Front Neurol. 2019;10:129. https://doi.org/10.3389/fneur.2019.00129.
Hall C, Chilcott R. Eyeing up the future of the pupillary light reflex in neurodiagnostics. Diagnostics. 2018;8:19. https://doi.org/10.3390/diagnostics8010019.
Eggert T, Sauter C, Popp R, Zeitlhoffer J, Danker-Hopfe H. The pupillographic sleepiness test in adults: effects of age, gender and time of day on pupillometric variables. Am J Hum Biol. 2012;24:820–8.
Kraemer S, Danker-Hopfe H, Dorn H, Schmidt A, Ehlert I, Herrmann W. Time-of-day variations of indicators of attention: performance, physiologic parameters and self-assessment of sleepiness. Biol Psychiatry. 2000;48:1069–80.
Schumann A, Andrack C, Bar K-J. Differences between sympathetic and parasympathetic modulation in major depression. Prog Neuropsychopharmacol Biol Psychiatry. 2017;79:324–31.
Siegle G, Steinhauer S, Friedman E, Thompson W, Thase M. Remission prognosis for cognitive therapy for recurrent depression using the pupil: utility and neural correlates. Biol Psychiatry. 2011;69:726–33.
Kudinova A, Burkhouse K, Siegle G, Owens M, Woody M, Gibb B. Pupillary reactivity to negative stimuli prospectively predicts recurrence of major depressive disorder in women. Psychophysiology. 2016;53:1836–42.
Bär KJ, Boettger MK, Schulz S, Harzendorf C, Agelink MW, Yeragani VK, et al. The interaction between pupil function and cardiovascular regulation in patients with acute schizophrenia. Clin Neurophysiol. 2008;119(10):2209–13.
Morris SK, Granholm E, Sarkin AJ, Jeste DV. Effects of schizophrenia and aging on pupillographic measures of working memory. Schizophr Res. 1997;27(2–3):119–28.
Fountoulakis K, Fotiou F, Iacovides A, Tsiptsios J, Goulas A, Tsolaki M, et al. Changes in pupil reaction to light in melancholic patients. Int J Psychophysiol. 1999;31:121–8.
Bar K-J, Greiner W, Jochum T, Friedrich M, Wagner G, Sauer H. The influence of major depression and its treatment on heart rate variability and pupillary light reflex parameters. J Affect Disord. 2004;82:245–52.
McCall W, Sareddy S, Youssef N, Miller B, Rosenquist P. The pupillary light reflex as a point-of-care test for suicide risk: preliminary results. Psychiatry Res. 2021;295: 113582. https://doi.org/10.1016/j.psychres.2020.113582.
Miller BJ, Sareddy S, Rosenquist PB, McCall WV. Pupillary light reflex markers of suicide risk in a trans-diagnostic sample. Schizophr Res. 2021;235:1–2.
Palagini L, Baglioni C, Ciapparelli A, Gemignani A, Riemann D. REM sleep dysregulation in depression: state of the art. Sleep Med Rev. 2013;17(5):377–90.
Berger M, Riemann D. Symposium: Normal and abnormal REM sleep regulation: REM sleep in depression-an overview. J Sleep Res. 1993;2(4):211–23.
Bar K-J, Schulz S, Koschke M, Harzendorf C, Gayde S, Berg W, et al. Correlations between the autonomic modulation of heart rate, blood pressure and the pupillary light reflex in healthy subjects. J Neurol Sci. 2009;279:9–13.
Venkata Sivakumar A, Kalburgi-Narayana M, Kuppusamy M, Ramaswamy P, Bachali S. Computerized dynamic pupillometry as a screening tool for evaluation of autonomic activity. Neurophysiol Clin. 2020;50(5):321–9.
Okutucu S, Civelekler M, Aparci M, Sabanoglu C, Dikmetas O, Aksoy H, et al. Computerized dynamic pupillometry indices mirrors the heart rate variability parameters. Eur J Med Pharmacol Sci. 2016;20:2099–105.
Kaltsatou A, Kouidi E, Fotiou D, Deligiannis P. The use of pupillometry in the assessment of cardiac autonomic function in elite different type trained athletes. Eur J Appl Physiol. 2011;111(9):2079–87.
Boettger S, Puta C, Yeragani VK, Donath L, Müller HJ, Gabriel HH, et al. Heart rate variability, QT variability and electrodermal activity during exercise. Med Sci Sports Exerc. 2010;42(3):443–8.
Funding
No funding was received for conducting this study.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection, and analysis were performed by William V. McCall. Brian Miller contributed to data collection and presentation. The first draft of the manuscript was written by William V. McCall, and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
Not applicable.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Conflict of Interest
Dr. Miller has nothing to disclose for the present work. In the past 12 months, he received research support from Augusta University, the National Institute of Mental Health, and the Stanley Medical Research Institute; participated in Advisory Boards for Boehringer Ingelheim; and Honoraria from Psychiatric Times. Dr. Rosenquist has nothing to disclose. Dr. McCall has nothing to disclose for the work under consideration. In the past 12 months, he has received research support from PCORI; has been a consultant for Anthem Insurance, Jazz, Sage, Janssen, and Idorsia; and has received royalties from Wolters Kluwer.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Mood Disorders
Rights and permissions
About this article
Cite this article
McCall, W.V., Rosenquist, P.B. & Miller, B.J. Development of Autonomic Nervous System Assays as Point-of-Care Tests to Supplement Clinical Judgment in Risk Assessment for Suicidal Behavior: A Review. Curr Psychiatry Rep 24, 11–21 (2022). https://doi.org/10.1007/s11920-022-01315-6
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11920-022-01315-6