Abstract
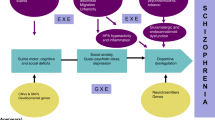
Over the past 2 decades, increased efforts have focused on identifying those at genetic or clinical risk for psychosis and promoting interventions that may alter the onset or trajectory of schizophrenia. We review studies published between 2010–2013 that: (1) investigate at-risk states for psychosis in larger epidemiological studies; (2) identify causes of certain clinical presentations of the schizophrenia phenotype and (3) investigate focused and multidisciplinary approaches to treat early clinical symptoms. The article places these recent studies within the context of prior research and the concept of potential measures to prevent or ameliorate the onset of psychosis.
Similar content being viewed by others
References
Recent papers of particular interest have been highlighted as: *Of importance **Of major importance
National Institute of Mental Health NIoM. 2013; Available from: http://www.nimh.nih.gov/statistics/1schiz.shtml.
Wu EQ, Birnbaum HG, Shi L, Ball DE, Kessler RC, Moulis M, et al. The economic burden of schizophrenia in the United States in 2002. J Clin Psychiatry. 2005;66(9):1122–9.
Fusar-Poli P, Borgwardt S. Predictive power of attenuated psychosis syndrome: is it really low? The case of mild cognitive impairment. Schizophr Res. 2012;135(1–3):192–3.
Brewer WJ, Francey SM, Wood SJ, Jackson HJ, Pantelis C, Phillips LJ, et al. Memory impairments identified in people at ultra-high risk for psychosis who later develop first-episode psychosis. Am J Psychiatry. 2005;162(1):71–8.
Gooding DC, Tallent KA, Matts CW. Clinical status of at-risk individuals 5 years later: further validation of the psychometric high-risk strategy. J Abnorm Psychol. 2005;114(1):170–5.
Kwapil TR. Social anhedonia as a predictor of the development of schizophrenia-spectrum disorders. J Abnorm Psychol. 1998;107(4):558–65.
Chapman LJ, Chapman JP, Kwapil TR, Eckblad M, Zinser MC. Putatively psychosis-prone subjects 10 years later. J Abnorm Psychol. 1994;103(2):171–83.
McGorry PD, Yung AR, Phillips LJ. The "close-in" or ultra high-risk model: a safe and effective strategy for research and clinical intervention in prepsychotic mental disorder. Schizophr Bull. 2003;29(4):771–90.
Phillips LJ, Yung AR, McGorry PD. Identification of young people at risk of psychosis: validation of Personal Assessment and Crisis Evaluation Clinic intake criteria. Aust N Z J Psychiatry. 2000;34 Supplement:S164-9.
McGlashan TH, Miller TJ, Woods SW, Rosen JL, Hoffman RE, Davidson L. Structured Interview for Prodromal Syndromes, Version 4.0. Prime Clinic Yale School of Medicine: New Haven, CT; 2003.
Fusar-Poli P, Bonoldi I, Yung AR, Borgwardt S, Kempton MJ, Valmaggia L, et al. Predicting psychosis: meta-analysis of transition outcomes in individuals at high clinical risk. Arch Gen Psychiatry. 2012;69(3):220–9. Meta-analysis included 2,502 clinical high-risk patients from 27 studies published through January 2011. The risk of developing psychosis in ultra-high risk individuals was 18 % at 6-month follow-up, 22% at 1year, 29 % at 2years and 36% after 3 years. Risk was moderated by the age of participants, treatments, diagnostic criteria and publication year.
Tsuang MT, Van Os J, Tandon R, Barch DM, Bustillo J, Gaebel W, et al. Attenuated psychosis syndrome in DSM-5. Schizophr Res. 2013;150(1):31–5.
Linscott RJ, van Os J. An updated and conservative systematic review and meta-analysis of epidemiological evidence on psychotic experiences in children and adults: on the pathway from proneness to persistence to dimensional expression across mental disorders. Psychol Med. 2013;43(6):1133–49. Conducted a meta-analysis of incidence and prevalence of psychotic experiences in 61 cohorts. The median annual incidence of psychotic experiences was 2.5%, and the prevalence was 7.2%. Approximately 20% of those reporting psychotic experiences developed persistent symptoms, with approximately 7.4% developing a psychotic disorder.
Kaymaz N, Drukker M, Lieb R, Wittchen HU, Werbeloff N, Weiser M, et al. Do subthreshold psychotic experiences predict clinical outcomes in unselected non-help-seeking population-based samples? A systematic review and meta-analysis, enriched with new results. Psychol Med. 2012;42(11):2239–53.
Wigman JT, van Winkel R, Raaijmakers QA, Ormel J, Verhulst FC, Reijneveld SA, et al. Evidence for a persistent, environment-dependent and deteriorating subtype of subclinical psychotic experiences: a 6-year longitudinal general population study. Psychol Med. 2011;41(11):2317–29.
Poulton R, Caspi A, Moffitt TE, Cannon M, Murray R, Harrington H. Children's self-reported psychotic symptoms and adult schizophreniform disorder: a 15-year longitudinal study. Arch Gen Psychiatry. 2000;57(11):1053–8.
Schimmelmann BG, Walger P, Schultze-Lutter F. The significance of at-risk symptoms for psychosis in children and adolescents. Can J Psychiatry. 2013;58(1):32–40.
Calkins ME, Moore TM, Merikangas KR, Burstein M, Satterthwaite T, Bilker WB, Ruparel K, Chiavacci R, Wolf D, Mentch FD, Qiu H, Connolly J, Sleiman PM, Hakonarson H, Gur RC, Gur RE. The psychosis spectrum in a young community sample: Findings from the Philadelphia Neurodevelopmental Cohort. Under Review. A total of 7,054 children aged 11–21 and their caregivers from the Philadelphia Neurodevelopmental Cohort were screened for major domains of psychopathology and psychosis spectrum symptoms; 20.0 % of medically healthy youths reported significant psychosis spectrum symptoms.
Dominguez MD, Saka MC, Lieb R, Wittchen HU, van Os J. Early expression of negative/disorganized symptoms predicting psychotic experiences and subsequent clinical psychosis: a 10-year study. Am J Psychiatry. 2010;167(9):1075–82.
Addington J, Cornblatt BA, Cadenhead KS, Cannon TD, McGlashan TH, Perkins DO, et al. At clinical high risk for psychosis: outcome for nonconverters. The American journal of psychiatry. 2011;168(8):800–5.
Fusar-Poli P, Yung AR, McGorry P, van Os J. Lessons learned from the psychosis high-risk state: towards a general staging model of prodromal intervention. Psychol Med. 2013:1–8.
Schultze-Lutter F, Ruhrmann S, Picker H, von Reventlow HG, Brockhaus-Dumke A, Klosterkotter J. Basic symptoms in early psychotic and depressive disorders. Br J Psychiatry Suppl. 2007;51:s31–7.
Stefanis NC, Hanssen M, Smirnis NK, Avramopoulos DA, Evdokimidis IK, Stefanis CN, et al. Evidence that three dimensions of psychosis have a distribution in the general population. Psychol Med. 2002;32(2):347–58.
De Loore E, Gunther N, Drukker M, Feron F, Sabbe B, Deboutte D, et al. Persistence and outcome of auditory hallucinations in adolescence: a longitudinal general population study of 1800 individuals. Schizophr Res. 2011;127(1–3):252–6.
Cannon TD, Cadenhead K, Cornblatt B, Woods SW, Addington J, Walker E, et al. Prediction of psychosis in youth at high clinical risk: a multisite longitudinal study in North America. Arch Gen Psychiatry. 2008;65(1):28–37.
Fusar-Poli P, Borgwardt S, Bechdolf A, Addington J, Riecher-Rossler A, Schultze-Lutter F, et al. The psychosis high-risk state: a comprehensive state-of-the-art review. JAMA Psychiatry. 2013;70(1):107–20.
Algon S, Yi J, Calkins ME, Kohler C, Borgmann-Winter KE. Evaluation and treatment of children and adolescents with psychotic symptoms. Curr Psychiatry Rep. 2012;14(2):101–10.
Pollak TA, McCormack R, Peakman M, Nicholson TR, David AS. Prevalence of anti-N-methyl-d-aspartate (NMDA) antibodies in patients with schizophrenia and related psychoses: a systematic review and meta-analysis. Psychol Med. 2013:1–13.
Barry H, Hardiman O, Healy DG, Keogan M, Moroney J, Molnar PP, et al. Anti-NMDA receptor encephalitis: an important differential diagnosis in psychosis. Br J Psychiatry. 2011;199(6):508–9.
Dalmau J, Gleichman AJ, Hughes EG, Rossi JE, Peng X, Lai M, et al. Anti-NMDA-receptor encephalitis: case series and analysis of the effects of antibodies. Lancet Neurol. 2008;7(12):1091–8.
Tidswell J, Kleinig T, Ash D, Thompson P, Galletly C. Early recognition of anti-N-methyl D-aspartate (NMDA) receptor encephalitis presenting as acute psychosis. Australas Psychiatry. 2013;21(6):596–9.
Benjamin S, Lauterbach MD, Stanislawski AL. Congenital and acquired disorders presenting as psychosis in children and young adults. Child Adolesc Psychiatr Clin N Am. 2013;22(4):581–608.
Armando M, Girardi P, Vicari S, Menghini D, Digilio MC, Pontillo M, et al. Adolescents at ultra-high risk for psychosis with and without 22q11 deletion syndrome: a comparison of prodromal psychotic symptoms and general functioning. Schizophr Res. 2012;139(1–3):151–6.
Tang SX, Yi JJ, Calkins ME, Whinna DA, Kohler CG, Souders MC, McDonald-McGinn DM, Zackai EH, Emanuel BS, Gur RC, Gur RE. Psychiatric disorders in 22q11.2 deletion syndrome are prevalent but undertreated. Psychol Med. 2013:1–11.
Constantinides P, Vincent P. Chronic gamma-hydroxybutyric-acid use followed by gamma-hydroxybutyric-acid withdrawal mimic schizophrenia: a case report. Cases J. 2009;2:7520.
Tarabar AF, Nelson LS. The gamma-hydroxybutyrate withdrawal syndrome. Toxicol Rev. 2004;23(1):45–9.
Salokangas RK, Ruhrmann S, von Reventlow HG, Heinimaa M, Svirskis T, From T, Luutonen S, Juckel G, Linszen D, Dingemans P, Birchwood M, Patterson P, Schultze-Lutter F, Klosterkotter J. Axis I diagnoses and transition to psychosis in clinical high-risk patients EPOS project: prospective follow-up of 245 clinical high-risk outpatients in four countries. Schizophr Res. 2012;138(2–3):192–7. Of 245 young patients with clinical high risk, during 18 month follow-up 37 developed psychosis. Diagnoses of bipolar disorder, unipolar depressive disorder and somatoform disorders were positively correlated with transition to psychosis, while anxiety disorders were negatively correlated.
Kelleher I, Keeley H, Corcoran P, Ramsay H, Wasserman C, Carli V, Sarchiapone M, Hoven C, Wasserman D, Cannon M. Childhood trauma and psychosis in a prospective cohort study: cause, effect, and directionality. The American journal of psychiatry. 2013;170(7):734–41. A total of 1,113 school-based adolescents ages 13–16 years. Children were assessed for trauma and psychotic symptoms at baseline, 3 months and 12 months. Trauma was found to be highly predictive of hallucinations. Relationships between trauma and psychotic symptoms were also bidirectional. Cessation of trauma was correlated with decreased subseqent psychotic symptoms.
Tikka M, Luutonen S, Ilonen T, Tuominen L, Kotimaki M, Hankala J, et al. Childhood trauma and premorbid adjustment among individuals at clinical high risk for psychosis and normal control subjects. Early Interv Psychiatry. 2013;7(1):51–7.
Arseneault L, Cannon M, Fisher HL, Polanczyk G, Moffitt TE, Caspi A. Childhood trauma and children's emerging psychotic symptoms: A genetically sensitive longitudinal cohort study. The American Journal of psychiatry. 2011;168(1):65–72. Interviews of 2,232 children aged 12 revealed that childhood bullying increased RR of psychotic symptoms 2–3 times.
Addington J, Case N, Saleem MM, Auther AM, Cornblatt BA, Cadenhead KS. Substance use in clinical high risk for psychosis: a review of the literature. Psychiatry: Early Interv; 2013.
Kristensen K, Cadenhead KS. Cannabis abuse and risk for psychosis in a prodromal sample. Psychiatry Res. 2007;151(1–2):151–4.
Dragt S, Nieman DH, Schultze-Lutter F, van der Meer F, Becker H, de Haan L, Dingemans PM, Birchwood M, Patterson P, Salokangas RK, Heinimaa M, Heinz A, Juckel G, Graf von Reventlow H, French P, Stevens H, Ruhrmann S, Klosterkotter J, Linszen DH. Cannabis use and age at onset of symptoms in subjects at clinical high risk for psychosis. Acta Psychiatr Scand. 2012;125(1):45–53. Two hundred forty-five help-seeking HR individuals ages 16–35 were assessed for assessed for cannabis consumption at onset of symptoms and followed for a mean duration of 465 days. Age at onset of cannabis use was correlated with earlier age of onset of HR symptoms. Onset of cannabis use preceded symptoms in most participants. No association was found between cannabis use and conversion from HR symptoms to psychosis.
Dragt S, Nieman DH, Becker HE, van de Fliert R, Dingemans PM, de Haan L, et al. Age of onset of cannabis use is associated with age of onset of high-risk symptoms for psychosis. Can J Psychiatry. 2010;55(3):165–71.
Compton MT, Kelley ME, Ramsay CE, Pringle M, Goulding SM, Esterberg ML, et al. Association of pre-onset cannabis, alcohol, and tobacco use with age at onset of prodrome and age at onset of psychosis in first-episode patients. The American journal of psychiatry. 2009;166(11):1251–7.
Addington J, Epstein I, Liu L, French P, Boydell KM, Zipursky RB. A randomized controlled trial of cognitive behavioral therapy for individuals at clinical high risk of psychosis. Schizophr Res. 2011;125(1):54–61.
Morrison AP, French P, Stewart SL, Birchwood M, Fowler D, Gumley AI, et al. Early detection and intervention evaluation for people at risk of psychosis: multisite randomised controlled trial. Bmj. 2012;344:e2233.
Morrison AP, French P, Walford L, Lewis SW, Kilcommons A, Green J, et al. Cognitive therapy for the prevention of psychosis in people at ultra-high risk: randomised controlled trial. Br J Psychiatry. 2004;185:291–7.
Phillips LJ, Nelson B, Yuen HP, Francey SM, Simmons M, Stanford C, et al. Randomized controlled trial of interventions for young people at ultra-high risk of psychosis: study design and baseline characteristics. The Australian and New Zealand journal of psychiatry. 2009;43(9):818–29.
van der Gaag M, Nieman DH, Rietdijk J, Dragt S, Ising HK, Klaassen RM, et al. Cognitive behavioral therapy for subjects at ultrahigh risk for developing psychosis: a randomized controlled clinical trial. Schizophr Bull. 2012;38(6):1180–8.
Morrison AP, French P, Parker S, Roberts M, Stevens H, Bentall RP, et al. Three-year follow-up of a randomized controlled trial of cognitive therapy for the prevention of psychosis in people at ultrahigh risk. Schizophr Bull. 2007;33(3):682–7.
Stafford MR, Jackson H, Mayo-Wilson E, Morrison AP, Kendall T. Early interventions to prevent psychosis: systematic review and meta-analysis. Bmj. 2013;346:f185.
Fisher M, Loewy R, Hardy K, Schlosser D, Vinogradov S. Cognitive interventions targeting brain plasticity in the prodromal and early phases of schizophrenia. Annu Rev Clin Psychol. 2013;9:435–63.
Wykes T, Huddy V, Cellard C, McGurk SR, Czobor P. A meta-analysis of cognitive remediation for schizophrenia: methodology and effect sizes. The American journal of psychiatry. 2011;168(5):472–85.
Rauchensteiner S, Kawohl W, Ozgurdal S, Littmann E, Gudlowski Y, Witthaus H, et al. Test-performance after cognitive training in persons at risk mental state of schizophrenia and patients with schizophrenia. Psychiatry Res. 2011;185(3):334–9.
Marker KR. COGPACK 6.0. Markersoftware: Laudenberg; 2001.
Buchanan RW, Carpenter WT. Concept of schizophrenia. In: Sadock BJ, Sadock VA, editors. Kaplan & Sadock's Comprehensive Textbook of Psychiatry. Philadelphia, PA USA; London, UK: Lippincott Williams & Wilkins; 2005. p. 1329.
Bechdolf A, Wagner M, Ruhrmann S, Harrigan S, Putzfeld V, Pukrop R, et al. Preventing progression to first-episode psychosis in early initial prodromal states. Br J Psychiatry. 2012;200(1):22–9.
Urben S, Pihet S, Jaugey L, Halfon O, Holzer L. Computer-assisted cognitive remediation in adolescents with psychosis or at risk for psychosis: a 6-month follow-up. Acta Neuropsychiatrica. 2012;24:328–35.
Liu CC, Chien YL, Hsieh MH, Hwang TJ, Hwu HG, Liu CM. Aripiprazole for drug-naive or antipsychotic-short-exposure subjects with ultra-high risk state and first-episode psychosis: an open-label study. J Clin Psychopharmacol. 2013;33(1):18–23.
McGlashan TH, Zipursky RB, Perkins D, Addington J, Miller T, Woods SW, et al. Randomized, double-blind trial of olanzapine versus placebo in patients prodromally symptomatic for psychosis. The American journal of psychiatry. 2006;163(5):790–9.
Walker EF, Cornblatt BA, Addington J, Cadenhead KS, Cannon TD, McGlashan TH, et al. The relation of antipsychotic and antidepressant medication with baseline symptoms and symptom progression: a naturalistic study of the North American Prodrome Longitudinal Sample. Schizophr Res. 2009;115(1):50–7.
Woods SW, Breier A, Zipursky RB, Perkins DO, Addington J, Miller TJ, et al. Randomized trial of olanzapine versus placebo in the symptomatic acute treatment of the schizophrenic prodrome. Biol Psychiatry. 2003;54(4):453–64.
Ruhrmann S, Bechdolf A, Kuhn KU, Wagner M, Schultze-Lutter F, Janssen B, et al. Acute effects of treatment for prodromal symptoms for people putatively in a late initial prodromal state of psychosis. Br J Psychiatry Suppl. 2007;51:s88–95.
Woods SW, Tully EM, Walsh BC, Hawkins KA, Callahan JL, Cohen SJ, et al. Aripiprazole in the treatment of the psychosis prodrome: an open-label pilot study. Br J Psychiatry Suppl. 2007;51:s96–101.
McGorry PD, Yung AR, Phillips LJ, Yuen HP, Francey S, Cosgrave EM, et al. Randomized controlled trial of interventions designed to reduce the risk of progression to first-episode psychosis in a clinical sample with subthreshold symptoms. Archives of General Psychiatry. 2002;59(10):921–8.
McGorry PD, Nelson B, Phillips LJ, Yuen HP, Francey SM, Thampi A, et al. Randomized controlled trial of interventions for young people at ultra-high risk of psychosis: twelve-month outcome. J Clin Psychiatry. 2013;74(4):349–56.
Cornblatt BA, Lencz T, Smith CW, Olsen R, Auther AM, Nakayama E, et al. Can antidepressants be used to treat the schizophrenia prodrome? Results of a prospective, naturalistic treatment study of adolescents. J Clin Psychiatry. 2007;68(4):546–57.
Fusar-Poli P, Valmaggia L, McGuire P. Can antidepressants prevent psychosis? Lancet. 2007;370(9601):1746–8.
Bowie CR, McLaughlin D, Carrion RE, Auther AM, Cornblatt BA. Cognitive changes following antidepressant or antipsychotic treatment in adolescents at clinical risk for psychosis. Schizophr Res. 2012;137(1–3):110–7.
Susser E, Neugebauer R, Hoek HW, Brown AS, Lin S, Labovitz D, et al. Schizophrenia after prenatal famine. Further evidence Archives of General Psychiatry. 1996;53(1):25–31.
St Clair D, Xu M, Wang P, Yu Y, Fang Y, Zhang F, et al. Rates of adult schizophrenia following prenatal exposure to the Chinese famine of 1959–1961. Jama. 2005;294(5):557–62.
McGrath J, Brown A, St CD. Prevention and schizophrenia–the role of dietary factors. Schizophr Bull. 2011;37(2):272–83.
Das UN. Polyunsaturated fatty acids and their metabolites in the pathobiology of schizophrenia. Prog Neuropsychopharmacol Biol Psychiatry. 2013;42:122–34.
Kidd PM. Omega-3 DHA and EPA for cognition, behavior, and mood: clinical findings and structural-functional synergies with cell membrane phospholipids. Altern Med Rev. 2007;12(3):207–27.
Amminger GP, Schafer MR, Papageorgiou K, Klier CM, Cotton SM, Harrigan SM, et al. Long-chain omega-3 fatty acids for indicated prevention of psychotic disorders: a randomized, placebo-controlled trial. Archives of General Psychiatry. 2010;67(2):146–54.
Tsai GE, Lin PY. Strategies to enhance N-methyl-D-aspartate receptor-mediated neurotransmission in schizophrenia, a critical review and meta-analysis. Curr Pharm Des. 2010;16(5):522–37.
Woods SW, Walsh BC, Hawkins KA, Miller TJ, Saksa JR, D'Souza DC, et al. Glycine treatment of the risk syndrome for psychosis: report of two pilot studies. Eur Neuropsychopharmacol. 2013;23(8):931–40.
Nordentoft M, Thorup A, Petersen L, Ohlenschlaeger J, Melau M, Christensen TO, et al. Transition rates from schizotypal disorder to psychotic disorder for first-contact patients included in the OPUS trial. A randomized clinical trial of integrated treatment and standard treatment Schizophr Res. 2006;83(1):29–40.
D'Souza DC, Abi-Saab WM, Madonick S, Forselius-Bielen K, Doersch A, Braley G, et al. Delta-9-tetrahydrocannabinol effects in schizophrenia: implications for cognition, psychosis, and addiction. Biol Psychiatry. 2005;57(6):594–608.
Kavanagh DJ. Management of co-occurring substance use disorders. In: Mueser KT, Jeste DV, editors. Clinical Handbook of Schizophrenia. NY: Guilford Press; 2008. p. 459–70.
McGorry PD, Hickie IB, Yung AR, Pantelis C, Jackson HJ. Clinical staging of psychiatric disorders: a heuristic framework for choosing earlier, safer and more effective interventions. The Australian and New Zealand Journal of Psychiatry. 2006;40(8):616–22.
Compliance with Ethics Guidelines
Conflict of Interest
James Yi declares that he has no conflict of interest.
Karin E. Borgmann-Winter has received a grant from the National Institute of Mental Health (K23MH079498).
Monica E. Calkins has received grants from the National Institute of Mental Health (K08MH079364, MH089983, MH089924).
There are no relevant disclosures regarding Conflict of Interest for Drs. Hurford and Kohler, and for Mr. Neustadter.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Author information
Authors and Affiliations
Corresponding author
Additional information
This article is part of the Topical Collection on Schizophrenia and Other Psychotic Disorders
Rights and permissions
About this article
Cite this article
Kohler, C., Borgmann-Winter, K.E., Hurford, I. et al. Is Prevention a Realistic Goal for Schizophrenia?. Curr Psychiatry Rep 16, 439 (2014). https://doi.org/10.1007/s11920-014-0439-y
Published:
DOI: https://doi.org/10.1007/s11920-014-0439-y