Abstract
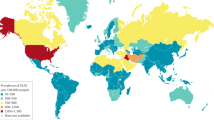
Nearly 27 million people have an opioid use disorder (OUD) according to the 2016 Global Burden of Disease study, most of which occur in the US where opioids are a common class of medication used to treat acute and chronic pain. In 2016 alone, more than 60 million patients had at least one prescription for opioids filled or refilled. Over the past decade, prescription rates have risen astronomically and have created an epidemic in the US dubbed the “opioid crisis.” In this regard, there has been an increase in overdoses and OUD diagnoses. Several studies have found dysregulation of balance between several neurotransmitters involved in the neural circuitry that subserves several behavioral domains, such as reward recognition, motivation, learning, and memory, affect, stress, and executive function, that contribute to the manifestation of craving. On the horizon is a new treatment approach consisting of the neuropeptide oxytocin, which may be involved in the overlapping mechanisms of stable attachment formation and coping with stress. Through this mechanism, it can shift processing from novelty and reward-seeking to an appreciation of familiarity and thus reduce stress and increase resilience in the face of addiction. It has been hypothesized that there is a connection between the glutaminergic and oxytocinergic systems, making oxytocin a possible therapeutic agent in reducing drug-induced actions seen in OUD patients. This manuscript will review the potential and feasible use of oxytocin in treating OUD.
Similar content being viewed by others
References
Hagemeier NE. Introduction to the opioid epidemic: the economic burden on the healthcare system and impact on quality of life. Am J Manag Care. 2018;24(10 Suppl):S200–6.
Vadivelu N, Kai AM, Kodumudi V, Sramcik J, Kaye AD. The opioid crisis: a comprehensive overview. Curr Pain Headache Rep. 2018;22(3):16. https://doi.org/10.1007/s11916-018-0670-z.
Taylor JL, Samet JH. Opioid use disorder. Ann Intern Med. 2022;175(1):ITC1–16. https://doi.org/10.7326/AITC202201180.
Strang J, et al. Opioid use disorder. Nat Rev Dis Primer. 2020;6(1):3. https://doi.org/10.1038/s41572-019-0137-5.
Edinoff AN, et al. Alternative options for complex, recurrent pain states using cannabinoids, psilocybin, and ketamine: a narrative review of clinical evidence. Neurol Int. 2022;14(2):423–36. https://doi.org/10.3390/neurolint14020035.
Edinoff AN, et al. Naltrexone implant for opioid use disorder. Neurol Int. 2021;14(1):49–61. https://doi.org/10.3390/neurolint14010004.
Tops M, Koole SL, IJzerman H, Buisman-Pijlman FTA. Why social attachment and oxytocin protect against addiction and stress: Insights from the dynamics between ventral and dorsal corticostriatal systems. Pharmacol Biochem Behav. 2014;119:39–48. https://doi.org/10.1016/j.pbb.2013.07.015.
McLellan AT, Lewis DC, O’Brien CP, Kleber HD. Drug dependence, a chronic medical illness: implications for treatment, insurance, and outcomes evaluation. JAMA. 2000;284(13):1689–95. https://doi.org/10.1001/jama.284.13.1689.
Wang S-C, Chen Y-C, Lee C-H, Cheng C-M. Opioid addiction, genetic susceptibility, and medical treatments: a review. Int J Mol Sci. 2019;20(17):E4294. https://doi.org/10.3390/ijms20174294.
GBD 2016 Disease and Injury Incidence and Prevalence Collaborators, Global, regional, and national incidence, prevalence, and years lived with disability for 328 diseases and injuries for 195 countries, 1990–2016: a systematic analysis for the Global Burden of Disease Study 2016. Lancet Lond Engl. 2017;390(10100):1211–1259. https://doi.org/10.1016/S0140-6736(17)32154-2.
Hedegaard H, Miniño AM, Warner M. Drug overdose deaths in the United States, 1999–2017. NCHS Data Brief. 2018;329:1–8.
Daley DC, Smith E, Balogh D, Toscaloni J. Forgotten but not gone: the impact of the opioid epidemic and other substance use disorders on families and children. Commonwealth. 2018;20. https://doi.org/10.15367/com.v20i2-3.189.
Hedegaard H, Bastian BA, Trinidad JP, Spencer M, Warner M. Drugs most frequently involved in drug overdose deaths: United States, 2011–2016. Natl Vital Stat Rep Cent Dis Control Prev Natl Cent Health Stat Natl Vital Stat Syst. 2018;67(9):1–14.
Lueptow LM, Shashkova EC, Miller MG, Evans CJ, Cahill CM. Insights into the neurobiology of craving in opioid use disorder. Curr Anesthesiol Rep. 2020;10(4):378–87. https://doi.org/10.1007/s40140-020-00420-7.
Robinson TE, Berridge KC. The neural basis of drug craving: an incentive-sensitization theory of addiction. Brain Res Brain Res Rev. 1993;18(3):247–91. https://doi.org/10.1016/0165-0173(93)90013-p.
Berridge KC, Robinson TE. Liking, wanting, and the incentive-sensitization theory of addiction. Am Psychol. 2016;71(8):670–9. https://doi.org/10.1037/amp0000059.
Koob GF. Neurobiology of opioid addiction: opponent process, hyperkatifeia, and negative reinforcement. Biol Psychiatry. 2020;87(1):44–53. https://doi.org/10.1016/j.biopsych.2019.05.023.
Shulman M, Wai JM, Nunes EV. Buprenorphine treatment for opioid use disorder: an overview. CNS Drugs. 2019;33(6):567–80. https://doi.org/10.1007/s40263-019-00637-z.
Buresh M, Stern R, Rastegar D. Treatment of opioid use disorder in primary care. BMJ. 2021;373:n784. https://doi.org/10.1136/bmj.n784.
Durrani M, Bansal K. Methadone. In StatPearls, Treasure Island (FL): StatPearls Publishing. 2022. Accessed: 21 Sep 2022. [Online]. Available: http://www.ncbi.nlm.nih.gov/books/NBK562216/.
Koehl JL, Zimmerman DE, Bridgeman PJ. Medications for management of opioid use disorder. Am J Health-Syst Pharm AJHP Off J Am Soc Health-Syst Pharm. 2019;76(15):1097–103. https://doi.org/10.1093/ajhp/zxz105.
Murnane KS, Augustine JM, Quesnel M, Marshall L, Strom JG. A classroom activity to increase student pharmacists confidence in dealing with the opioid epidemic. Am J Pharm Educ. 2019;83(9):7199. https://doi.org/10.5688/ajpe7199.
Jeanelle. Rising fentanyl use challenges current methadone induction protocols. Clin Advis. 2022. https://www.clinicaladvisor.com/home/the-waiting-room/fentanyl-challenges-current-methadone-induction-protocols/ (Accessed 03 Oct 2022).
Randhawa PA, Brar R, Nolan S. Buprenorphine–naloxone ‘microdosing’: an alternative induction approach for the treatment of opioid use disorder in the wake of North America’s increasingly potent illicit drug market. CMAJ Can Med Assoc J. 2020;192(3):E73. https://doi.org/10.1503/cmaj.74018.
Edinoff AN, et al. Oxytocin, a novel treatment for methamphetamine use disorder. Neurol Int. 2022;14(1):1. https://doi.org/10.3390/neurolint14010015.
The oxytocin receptor: from intracellular signaling to behavior | physiological reviews. https://journals.physiology.org/doi/full/10.1152/physrev.00031.2017?rfr_dat=cr_pub++0pubmed&url_ver=Z39.88-2003&rfr_id=ori%3Arid%3Acrossref.org. (Accessed 21 Sep 2022).
Sundar M, Patel D, Young Z, Leong K-C. Oxytocin and addiction: potential glutamatergic mechanisms. Int J Mol Sci. 2021;22(5):2405. https://doi.org/10.3390/ijms22052405.
Russell J, Leng G, Bicknell R. Opioid tolerance and dependence in the magnocellular oxytocin system: a physiological mechanism? Exp Physiol. 1995;80(3):307–40. https://doi.org/10.1113/expphysiol.1995.sp003850.
Fan X-Y, Shi G, He X-J, Li X-Y, Wan Y-X, Jian L-Y. Oxytocin prevents cue-induced reinstatement of oxycodone seeking: involvement of DNA methylation in the hippocampus. Addict Biol. 2021;26(6):e13025. https://doi.org/10.1111/adb.13025.
Fan X-Y, Shi G, Zhao P. Methylation in Syn and Psd95 genes underlie the inhibitory effect of oxytocin on oxycodone-induced conditioned place preference. Eur Neuropsychopharmacol J Eur Coll Neuropsychopharmacol. 2019;29(12):1464–75. https://doi.org/10.1016/j.euroneuro.2019.10.010.
Gannon BM, Rice KC, Murnane KS. MDPV ‘high-responder’ rats also self-administer more oxycodone than their ‘low-responder’ counterparts under a fixed ratio schedule of reinforcement. Psychopharmacology. 2021;238(4):1183–92. https://doi.org/10.1007/s00213-021-05764-4.
Zanos P, et al. The oxytocin analogue carbetocin prevents emotional impairment and stress-induced reinstatement of opioid-seeking in morphine-abstinent mice. Neuropsychopharmacology. 2014;39(4):4. https://doi.org/10.1038/npp.2013.285.
Daigle KM, et al. Maternal responsivity and oxytocin in opioid-dependent mothers. Dev Psychobiol. 2020;62(1):21–35. https://doi.org/10.1002/dev.21897.
Weinberg MK, Tronick EZ. Beyond the face: an empirical study of infant affective configurations of facial, vocal, gestural, and regulatory behaviors. Child Dev. 1994;65(5):1503–15. https://doi.org/10.1111/j.1467-8624.1994.tb00832.x.
Moeini M, Omidi A, Sehat M, Banafshe HR. The effects of oxytocin on withdrawal, craving and stress response in heroin-dependent patients: a randomized, double-blind clinical trial. Eur Addict Res. 2019;25(1):41–7. https://doi.org/10.1159/000496194.
Woolley JD, et al. The effects of intranasal oxytocin in opioid-dependent individuals and healthy control subjects: a pilot study. Psychopharmacology. 2016;233(13):2571–80. https://doi.org/10.1007/s00213-016-4308-8.
Funding
This work was supported by the National Institutes of Health grant RO1 NS120676 to K.S.M.
Author information
Authors and Affiliations
Contributions
All authors listed have made a direct and intellectual contribution to the work and approved for publication.
Corresponding author
Ethics declarations
Conflict of Interest
None.
Human and Animal Rights and Informed Consent statement
This article is based on previously conducted studies and does not contain any new studies with human participants or animals performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Acute Pain Medicine
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Edinoff, A.N., Sall, S., Honore, L.G. et al. The Use of Oxytocin for the Treatment of Opioid Use Disorder. Curr Pain Headache Rep 27, 89–97 (2023). https://doi.org/10.1007/s11916-023-01105-6
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11916-023-01105-6