Abstract
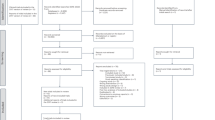
Cardiovascular disease (CVD) remains the leading cause of death in the developed countries and is estimated to be the leading cause of death in the developing countries by the year 2030. The cause for this rise in CVD is the increase in the major CVD risk factors (CVRFs) like hypertension, obesity, diabetes, and hyperlipidemia, which account for 80 % of all CVD deaths worldwide. In order to prevent the increase in CVD, it has been proposed to develop a low-cost polypill containing four to five generic drugs with known effectiveness in the reduction of the CVRFs. This polypill has now been tested in several recent studies for the primary and secondary prevention of CVD and stroke with fairly good results. A Medline search of the English language literature between 2011 and 2015 resulted in the identification of 15 studies with pertinent findings. These findings together with collateral literature will be discussed in this review.
Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance
World Health Statistics. Cardiovascular diseases (CVDs). Available at http://www.who.int/factsheets/fs317/index.html. 2015. Accessed 10 Oct 2015
Dalton AR, Sojak M, Samarasundera E, et al. Prevalence of cardiovascular disease risk amongst the population eligible for the NHS Health Check Programme. Eur J Prev Cardiol. 2013;20:142–50.
Lasiett LJ, Alagona Jr P, Clark 3rd BA, et al. The worldwide environment of cardiovascular disease: prevalence, diagnosis, therapy, and policy issues: a report from the American College of Cardiology. J Am Coll Cardiol. 2012;60:S1–S49.
Sixty-Sixth Assembly. Follow-up to the political declaration of the high-level meeting of the General Assembly on the Prevention and Control of Non-Communicable Diseases. WHA6610, 2013. Available at http://apps.who.int/gb/ebwha/pdf_files/WHA66/A66_R10-en.pdf
Kontis V, Mathers CD, Rehm J, et al. Contribution of six factors to achieving the 25 × 25 non-communicable disease mortality reduction target: a modeling study. Lancet. 2014;384:427–37.
Wald NJ, Law MP. A strategy to reduce cardiovascular disease by more than 80%. BMJ. 2003;326:1419.
Lloyd-Jones DM, Leip EP, Larson MG, et al. Prediction of lifetime risk for cardiovascular disease by risk factor burden at 50 years of age. Circulation. 2006;113:791–8.
Law MR, Wald NJ, Rudnicka A. Quantifying effect of statins on low density lipoprotein cholesterol, ischemic heart disease, and stroke: a systematic review and meta-analysis. BMJ. 2003;326:1423–7.
Law MR, Wald NJ, Thompson SG. By how much and how quickly does reduction in serum cholesterol concentration lower risk of ischemic heart disease? BMJ. 1994;308:367–72.
Homocysteine Lowering Trialists Collaboration. Lowering blood homocysteine with folic acid based supplements. Meta-analysis of randomized trials. BMJ. 1998;316:894–8.
Law MR, Wald NJ, Morris JK, Jordan R. Value of low-dose combination treatment with blood pressure lowering drugs: analysis of 354 randomized trials. BMJ. 2003;326:1427–31.
Antithrombotic Trialists Collaboration. Collaborative meta-analysis of randomized trials on antiplatelet therapy for prevention of death, myocardial infarction, and stroke in high risk patients. BMJ. 2002;324:71–86.
Yusuf S, Pais P, Afzal R, et al. Effects of a polypill (Polycap) on risk factors in middle-aged individuals without cardiovascular disease (TIPS): a phase II, double-blind, randomised trial. Lancet. 2009;373:1341–51.
Malehzadeh F, Marshall T, Pourshams A, et al. A pilot double-blind randomized placebo-controlled trial of the effects of fixed-dose combination therapy (polypill) on cardiovascular risk factors. Int J Clin Pract. 2010;64:1220–7.
Rodgers A, Patel A, Berwanger O, PILL Collaboration Group, et al. An international randomized placebo-controlled trial of four component combination pill (“polypill”) in people with raised cardiovascular risk. PLoS ONE. 2011;6:e19857.
Wald DS, Morris JK, Wald NJ. Randomized crossover trial in people aged 50 and over. PLoS ONE. 2012;7, e41297.
Soliman EZ, Mendis S, Dissanayake WP, et al. A polypill for primary prevention of cardiovascular disease: a feasibility study of the World Health Organization. Trials. 2011;12:3.
Kotseva K, Wood D, DeBacker D, EUROASPIRE Study Group, et al. EUROASPIRE III: a survey on the lifestyle, risk factors, and use of cardioprotective drug therapies in coronary patients from 22 European countries. Eur J Cardiovasc Prev Rehabil. 2009;16:121–37.
Mendis S, Abegunde D, Yusuf S, et al. WHO study on prevention of REcurrence of myocardial infarction and stroke (WHO-PREMISE). Bull World Health Organ. 2005;83:820–9.
Gaziano TA, Opie LH, Weinstein MC. Cardiovascular disease prevention with multidrug regimen in the developing world: a cost-effectiveness analysis. Lancet. 2006;368:679–86.
Mendis S, Fukino K, Cameron A, et al. The availability and affordability of selected essential medicines for chronic diseases in six low-to-medium income countries. Bull World Health Organ. 2007;85:279–88.
Yusuf S, Pais P, Sigamani A, et al. Comparison of risk factor reduction and tolerability of a full-dose polypill (with potassium) versus low-dose polypill (polycap) in individuals at high risk of cardiovascular disease. The second Indian Polycap Study (TIPS-2) Investigators. Circ Cardiovasc Qual Outcome. 2012;5:463–71.
Thom S, Poulter N, Field J, et al. Effects of a fixed-dose combination strategy on adherence and risk factors in patients with or at high risk for CVD. The UMPIRE randomized clinical trial. JAMA. 2013;310:918–29.
Selak V, Elley CR, Bullen C, et al. Effect of fixed dose combination treatment on adherence and risk factor control among patients at high risk of cardiovascular disease: randomised controlled trial in primary care. BMJ. 2014;348:g3318. An interesting study providing information on CVRF control for primary and secondary CVD prevention in addition to patient acceptance and adherence to treatment. This compared fixed-dose combination with usual care and increased patient acceptance and adherence to fixed-dose combination.
Patel A, Cass A, Peiris D, et al. A pragmatic randomized trial of a polypill-based strategy to improve use of indicated preventive treatments in people at high cardiovascular disease risk. Eur J Prev Cardiol. 2015;22:920–30.
Castellano JM, Sanz G, Penalvo JL, et al. A polypill strategy to improve adherence. Results from the FOCUS projects. J Am Coll Cardiol. 2014;64:2071–82.
Sutcliff P, Connock M, Gurung T, et al. Aspirin in primary prevention of cardiovascular disease and cancer: a systematic review of the balance of evidence from reviews of randomized trials. PLoS ONE. 2013;8, e81970.
Bezalel S, Mahlab-Guri K, Asher L, et al. Angiotensin-converting enzyme inhibitor-induced angioedema. Am J Med. 2015;128:120–5.
Patel A, Shah T, Shah G, et al. Preservation of bioavailability of ingredients and lack of drug-drug interactions in a novel five-ingredient polypill (polycap): a five arm phase I crossover trial in healthy volunteers. Am J Cardiovasc Drugs. 2010;10:95–105.
Huffman MD, Perel P, Castellano JM, et al. An application to recommend that fixed-dose combination therapy be added to the WHO model list of essential medicines for secondary prevention of cardiovascular disease (ischemic heart disease and ischemic stroke). http://www.who.int/selection_medicines/expert/20/applications/Aspirin_FDC.pdf Accessed 20 Oct 2015
Huffman MD. The polypill: from promise to pragmatism. PLoS Med. 2015;12, e1001862.
Bryant L, Martini N, Chan J, et al. Could the polypill improve adherence? The patient perspective. J Prim Health Care. 2013;5:28–35.
Laba TL, Hayes A, Lo S, et al. An economic case for a cardiovascular polypill? A cost analysis of the Kanyini GAP trial. Med J Aust. 2014;11:671–3.
Becerra V, Gracia A, Desai K, et al. Cost-effectiveness and public health benefit of secondary cardiovascular disease prevention from improved adherence using a polypill in the UK. BMJ Open. 2015;5:e 007111. This study evaluated the cost effectiveness of the polypill and its public health benefit from improved adherence in secondary prevention of CVD.
Wood F, Salam A, Singh K, et al. Process evaluation of the impact and acceptability of a polypill for prevention of cardiovascular disease. BMJ Open. 2015;5:e 008018. This study evaluated the impact of the polypill on the prevention of cardiovascular disease and discusses patient and doctor acceptance.
Liu H, Massi L, Comm BB, et al. Patients’ and providers perspectives of a polypill strategy to improve cardiovascular prevention in Australian primary health care. A qualitative study set within a pragmatic randomized controlled trial. Circ Cardiovasc Qual Outcome. 2015;8:301–8.
Virdee SK, Greenfield SM, Fletcher K, et al. Would primary care professionals prescribe a polypill to manage cardiovascular risk? A qualitative interview study. BMJ Open. 2013;3:c 002498.
Viera AJ, Sheridan SL, Soliman EZ, et al. Acceptance of a polypill approach to prevent cardiovascular disease: a sample of US physicians. Prev Med. 2011;52:10–5.
Carey KM, Comee MR, Donovan JL, O’Kanaan A. A polypill for all? A critical review of the polypill literature for primary prevention of cardiovascular disease and stroke. Ann Pharmacother. 2012;46:688–95.
Chrysant SG, Chrysant GS. Future of polypill use for the prevention of cardiovascular disease and strokes. Am J Cardiol. 2014;114:641–5.
Chen J, Normand SL, Wang Y, et al. Recent declines in hospitalizations for acute myocardial infarction for Medicare fee-for-service beneficiaries. Progress and continuing challenges. Circulation. 2010;121:1322–8.
Wilmot KA, O’Flaherty M, Capwell S, et al. Coronary heart disease mortality declines in the United States from 1979 through 2011. Evidence for stagnation in young adults, especially women. Circulation. 2015;132:997–1002.
Law MR, Watt HC, Wald NJ. The underlying risk of death after myocardial infarction in the absence of treatment. Arch Intern Med. 2002;162:2405–10.
Bittencourt MS, Blaha MJ, Blankstein R, et al. Polypill therapy, subclinical atherosclerosis, and cardiovascular events—implications for the use of preventive pharmacotherapy: MESA (Multi Ethnic Study of Atherosclerosis). J Am Coll Cardiol. 2014;63:434–43.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Drs. S. Chrysant and G. Chrysant declare no conflicts of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
This article is part of the Topical Collection on Antihypertensive Agents: Mechanisms of Drug Action
Rights and permissions
About this article
Cite this article
Chrysant, S.G., Chrysant, G.S. Usefulness of the Polypill for the Prevention of Cardiovascular Disease and Hypertension. Curr Hypertens Rep 18, 14 (2016). https://doi.org/10.1007/s11906-016-0624-y
Published:
DOI: https://doi.org/10.1007/s11906-016-0624-y