Abstract
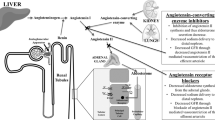
The velocity of chronic kidney disease (CKD) progression is only partly dependent on the nature and activity of the underlying disease process. Activation of the renin-angiotensin-aldosterone system (RAAS) is a crucial, and often universal, event responsible for the pathophysiologic mechanisms that accelerate CKD progression. Thus, it would appear that interruption of the RAAS through the use of angiotensin-converting enzyme inhibitors, angiotensin receptor blockers, mineralocorticoid receptor antagonists, or direct renin inhibitors can play a principal role in slowing CKD progression, regardless of the cause. Unfortunately, applying this generalized approach to all forms of CKD has been delayed by the lack of strong, evidence-based data. The aim of this review is to provide the most current evidence available for the use of RAAS blockade as a method of slowing the progression of the various forms of CKD.


Similar content being viewed by others
Abbreviations
- AASK:
-
African American Study of Kidney Disease
- ACCOMPLISH:
-
Avoiding Cardiovascular Events through Combination Therapy in Patients Living with Systolic Hypertension
- ALTITUDE:
-
Aliskiren Trial in Type 2 Diabetes Using Cardio-Renal Endpoints
- AVOID:
-
Aliskiren in the Evaluation of Proteinuria in Diabetes
- HALT PKD:
-
Halt Progression of Polycystic Kidney Disease
- HKVIN:
-
Hong Kong Study using Valsartan n IgA Nephropathy
- IDNT:
-
Irbesartan in Diabetic Nephropathy Trial
- MDRD:
-
Modification of Diet in Renal Disease
- ONTARGET:
-
Ongoing Telmisartan Alone and in Combination with Ramipril Global Endpoint Trial
- REIN:
-
Ramipril Efficacy in Nephropathy
- RENAAL:
-
Reduction of Endpoints in NIDDM with the Angiotensin II Antagonist Losartan
- VA NEPHRON-D:
-
Veterans Affairs Nephropathy in Diabetes
References
Papers of particular interest, published recently, have been highlighted as: • Of importance
Eijkelkamp WB, Zhang Z, Remuzzi G, et al.: Albuminuria is a target for renoprotective therapy independent from blood pressure in patients with type 2 diabetic nephropathy: post hoc analysis from the Reduction of Endpoints in NIDDM with the Angiotensin II Antagonist Losartan (RENAAL) trial. J Am Soc Nephrol 2007, 18:1540–1546.
Anavekar NS, Gans DJ, Berl T, et al.: Predictors of cardiovascular events in patients with type 2 diabetic nephropathy and hypertension: a case for albuminuria. Kidney Int Suppl 2004:S50–S55.
Norris KC, Greene T, Kopple J, et al.: Baseline predictors of renal disease progression in the African American Study of Hypertension and Kidney Disease. J Am Soc Nephrol 2006, 17:2928–2936.
Atkins RC, Briganti EM, Lewis JB, et al.: Proteinuria reduction and progression to renal failure in patients with type 2 diabetes mellitus and overt nephropathy. Am J Kidney Dis 2005, 45:281–287.
Brenner BM, Cooper ME, de Zeeuw D, et al.: Effects of losartan on renal and cardiovascular outcomes in patients with type 2 diabetes and nephropathy. N Engl J Med 2001, 345:861–869.
Kidney Disease Outcomes Quality Initiative (K/DOQI): K/DOQI clinical practice guidelines on hypertension and antihypertensive agents in chronic kidney disease. Am J Kidney Dis 2004, 43(5 Suppl 1):S1–S290.
Kunz R, Friedrich C, Wolbers M, Mann JF: Meta-analysis: effect of monotherapy and combination therapy with inhibitors of the renin angiotensin system on proteinuria in renal disease. Ann Intern Med 2008, 148:30–48.
Jennings DL, Kalus JS, Coleman CI, et al.: Combination therapy with an ACE inhibitor and an angiotensin receptor blocker for diabetic nephropathy: a meta-analysis. Diabet Med 2007, 24:486–493.
Rossing K, Schjoedt KJ, Smidt UM, et al.: Beneficial effects of adding spironolactone to recommended antihypertensive treatment in diabetic nephropathy: a randomized, double-masked, cross-over study. Diabetes Care 2005, 28:2106–2112.
• Mehdi UF, Adams-Huet B, Raskin P, et al.: Addition of angiotensin receptor blockade or mineralocorticoid antagonism to maximal angiotensin-converting enzyme inhibition in diabetic nephropathy. J Am Soc Nephrol 2009, 20:2641–2650. This double-blind, placebo-controlled trial showed that the addition of spironolactone, but not losartan, to a regimen including maximal ACE inhibition afforded greater renoprotection in diabetic nephropathy.
Krum H, Nolly H, Workman D, et al.: Efficacy of eplerenone added to renin-angiotensin blockade in hypertensive patients. Hypertension 2002, 40:117–123.
Epstein M, Williams GH, Weinberger M, et al.: Selective aldosterone blockade with eplerenone reduces albuminuria in patients with type 2 diabetes. Clin J Am Soc Nephrol 2006, 1:940–951.
Sato A, Hayashi K, Naruse M, Saruta T: Effectiveness of aldosterone blockade in patients with diabetic nephropathy. Hypertension 2003, 41:64–68.
• Parving HH, Persson F, Lewis JB, et al.: Aliskiren combined with losartan in type 2 diabetes and nephropathy. N Engl J Med 2008, 358:2433–2446. This important study demonstrated that aliskiren combined with losartan conferred greater reduction in proteinuria than placebo in hypertensive individuals with diabetic nephropathy.
• Parving HH, Brenner BM, McMurray JJ, et al.: Aliskiren Trial in Type 2 Diabetes Using Cardio-Renal Endpoints (ALTITUDE): rationale and study design. Nephrol Dial Transplant 2009, 24:1663–1671. This study will determine if adding aliskiren to ACE inhibitor or ARB therapy can reduce cardiovascular and renal events in high-risk patients with type 2 diabetes.
Park S, Bivona BJ, Kobori H, et al.: Major role for ACE-independent intrarenal ANG II formation in type II diabetes. Am J Physiol Renal Physiol 2010, 298:F37–F48.
• Yusuf S, Teo KK, Pogue J, et al.: Telmisartan, ramipril, or both in patients at high risk for vascular events. N Engl J Med 2008, 358:1547–1559. This study showed that the combination of ramipril and telmisartan resulted in more adverse events than either drug alone in patients at high risk of vascular events.
• Fried LF, Duckworth W, Zhang JH, et al.: Design of combination angiotensin receptor blocker and angiotensin-converting enzyme inhibitor for treatment of diabetic nephropathy (VA NEPHRON-D). Clin J Am Soc Nephrol 2009, 4:361–368. This study will determine the long-term renal effects of dual RAAS blockade in patients with diabetic kidney disease.
Randomised placebo-controlled trial of effect of ramipril on decline in glomerular filtration rate and risk of terminal renal failure in proteinuric, non-diabetic nephropathy. The GISEN Group (Gruppo Italiano di Studi Epidemiologici in Nefrologia). Lancet 1997, 349:1857–1863.
Ruggenenti P, Perna A, Remuzzi G: ACE inhibitors to prevent end-stage renal disease: when to start and why possibly never to stop: a post hoc analysis of the REIN trial results. Ramipril Efficacy in Nephropathy. J Am Soc Nephrol 2001, 12:2832–2837.
Maschio G, Alberti D, Janin G, et al.: Effect of the angiotensin-converting-enzyme inhibitor benazepril on the progression of chronic renal insufficiency. The Angiotensin-Converting-Enzyme Inhibition in Progressive Renal Insufficiency Study Group. N Engl J Med 1996, 334:939–945.
Wright JT Jr, Bakris G, Greene T, et al.: Effect of blood pressure lowering and antihypertensive drug class on progression of hypertensive kidney disease: results from the AASK trial. JAMA 2002, 288:2421–2431.
Hou FF, Zhang X, Zhang GH, et al.: Efficacy and safety of benazepril for advanced chronic renal insufficiency. N Engl J Med 2006, 354:131–140.
Jafar TH, Schmid CH, Landa M, et al.: Angiotensin-converting enzyme inhibitors and progression of nondiabetic renal disease. A meta-analysis of patient-level data. Ann Intern Med 2001, 135:73–87.
• Bakris GL, Sarafidis PA, Weir MR, et al.: Renal outcomes with different fixed-dose combination therapies in patients with hypertension at high risk for cardiovascular events (ACCOMPLISH): a prespecified secondary analysis of a randomised controlled trial. Lancet 2010, 375:1173–1181. This double-blind, randomized trial showed that the combination of benazepril and amlodipine conferred greater renoprotection than the combination of benazepril and hydrochlorothiazide in patients with systolic hypertension.
Jafar TH, Stark PC, Schmid CH, et al.: The effect of angiotensin-converting-enzyme inhibitors on progression of advanced polycystic kidney disease. Kidney Int 2005, 67:265–271.
Ecder T, Chapman AB, Brosnahan GM, et al.: Effect of antihypertensive therapy on renal function and urinary albumin excretion in hypertensive patients with autosomal dominant polycystic kidney disease. Am J Kidney Dis 2000, 35:427–432.
Nutahara K, Higashihara E, Horie S, et al.: Calcium channel blocker versus angiotensin II receptor blocker in autosomal dominant polycystic kidney disease. Nephron Clin Pract 2005, 99:c18–c23.
• Chapman AB, Torres VE, Perrone RD, et al.: The HALT polycystic kidney disease trials: design and implementation. Clin J Am Soc Nephrol 2010, 5:102–109. This large, randomized trial will determine the impact of intensive blockade of RAAS and the level of blood pressure control on progressive renal disease in individuals with early and more advanced stages of ADPKD.
Reich HN, Troyanov S, Scholey JW, Cattran DC: Remission of proteinuria improves prognosis in IgA nephropathy. J Am Soc Nephrol 2007, 18:3177–3183.
Praga M, Gutierrez E, Gonzalez E, Morales E, et al.: Treatment of IgA nephropathy with ACE inhibitors: a randomized and controlled trial. J Am Soc Nephrol 2003, 14:1578–1583.
Li PK, Leung CB, Chow KM, et al.: Hong Kong study using valsartan in IgA nephropathy (HKVIN): a double-blind, randomized, placebo-controlled study. Am J Kidney Dis 2006, 47:751–760.
Coppo R, Peruzzi L, Amore A, et al.: IgACE: a placebo-controlled, randomized trial of angiotensin-converting enzyme inhibitors in children and young people with IgA nephropathy and moderate proteinuria. J Am Soc Nephrol 2007, 18:1880–1888.
Russo D, Minutolo R, Pisani A, et al.: Coadministration of losartan and enalapril exerts additive antiproteinuric effect in IgA nephropathy. Am J Kidney Dis 2001, 38:18–25.
Heinze G, Mitterbauer C, Regele H, et al.: Angiotensin-converting enzyme inhibitor or angiotensin II type 1 receptor antagonist therapy is associated with prolonged patient and graft survival after renal transplantation. J Am Soc Nephrol 2006, 17:889–899.
Amuchastegui SC, Azzollini N, Mister M, et al.: Chronic allograft nephropathy in the rat is improved by angiotensin II receptor blockade but not by calcium channel antagonism. J Am Soc Nephrol 1998, 9:1948–1955.
Zaltzman JS, Nash M, Chiu R, Prasad R: The benefits of renin-angiotensin blockade in renal transplant recipients with biopsy-proven allograft nephropathy. Nephrol Dial Transplant 2004, 19:940–944.
Campistol JM, Inigo P, Jimenez W, et al.: Losartan decreases plasma levels of TGF-beta1 in transplant patients with chronic allograft nephropathy. Kidney Int 1999, 56:714–719.
el-Agroudy AE, Hassan NA, Foda MA, et al.: Effect of angiotensin II receptor blocker on plasma levels of TGF-beta 1 and interstitial fibrosis in hypertensive kidney transplant patients. Am J Nephrol 2003, 23:300–306.
Tylicki L, Larczynski W, Rutkowski B: Renal protective effects of the renin-angiotensin-aldosterone system blockade: from evidence-based approach to perspectives. Kidney Blood Press Res 2005, 28:230–242.
Paoletti E, Cassottana P, Amidone M, et al.: ACE inhibitors and persistent left ventricular hypertrophy after renal transplantation: a randomized clinical trial. Am J Kidney Dis 2007, 50:133–142.
Hiremath S, Fergusson D, Doucette S, et al.: Renin angiotensin system blockade in kidney transplantation: a systematic review of the evidence. Am J Transplant 2007, 7:2350–2360.
Andres A, Morales E, Morales JM, et al.: Efficacy and safety of valsartan, an angiotensin II receptor antagonist, in hypertension after renal transplantation: a randomized multicenter study. Transplant Proc 2006, 38:2419–2423.
Disclosure
Dr. Weir has received consulting fees from Amgen, Novartis, NicOx, and Daiichi Sankyo. No other potential conflicts of interest relevant to this article were reported.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lattanzio, M.R., Weir, M.R. Does Blockade of the Renin-Angiotensin-Aldosterone System Slow Progression of All Forms of Kidney Disease?. Curr Hypertens Rep 12, 369–377 (2010). https://doi.org/10.1007/s11906-010-0142-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11906-010-0142-2