Abstract
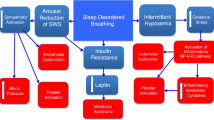
Obstructive sleep apnea (OSA) is characterized by upper airway collapse and airflow reduction despite respiratory effort, resulting in intermittent hypoxia and arousals, leading to a cascade of hemodynamic, autonomic, inflammatory, and metabolic effects, responsible for its adverse cardiovascular effect. OSA is an independent risk factor for cardiovascular disease, and its prevalence in patients presenting with acute coronary syndromes is up to 69 %. Furthermore, OSA has been associated with increased risk of adverse events after an acute coronary syndrome. Continuous positive airway pressure is considered the mainstay of treatment of OSA and has been shown to reduce the risk of cardiovascular events. However, the proper time to start treatment in the acute setting is unknown. A prospective randomized clinical trial is currently underway to answer this question.



Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Somers VK, White DP, Amin R, et al. Sleep apnea and cardiovascular disease: an American Heart Association/American College of Cardiology Foundation Scientific Statement from the American Heart Association Council for High Blood Pressure Research Professional Education Committee, Council on Clinical Cardiology, Stroke Council, and Council on Cardiovascular Nursing. J Am Coll Cardiol. 2008;52:686–717.
Mooe T, Rabben T, Wiklund U, Franklin KA, Eriksson P. Sleep disordered breathing in men with coronary artery disease. Chest. 1996;109:659–63.
Peker Y, Carlson J, Hedner J. Increased incidence of coronary artery disease in sleep apnoea: a long-term follow-up. Eur Respir J. 2006;28:596–602.
Yumino D, Tsurumi Y, Takagi A, Suzuki K, Kasanuki H. Impact of obstructive sleep apnea on clinical and angiographic outcomes following percutaneous coronary intervention in patients with acute coronary syndrome. Am J Cardiol. 2007;99:26–30.
Cepeda-Valery B, Slipczuk L, Figueredo VM, et al. Association between obesity and infarct size: insight into the obesity paradox. Int J Cardiol. 2013;167:604–6.
Shah NA, Yaggi HK, Concato J, Mohsenin V. Obstructive sleep apnea as a risk factor for coronary events or cardiovascular death. Sleep Breath. 2010;14:131–6. This study found that OSA was an independent risk factor for cardiovascular events, including myocardial infarction.
Schafer H, Koehler U, Ewig S, et al. Obstructive sleep apnea as a risk marker in coronary artery disease. Cardiology. 1999;92:79–89.
Shahar E, Whitney C, Redline S, et al. Sleep-disordered breathing and cardiovascular disease: cross-sectional results of the Sleep Heart Health Study. Am J Respir Crit Care Med. 2001;163:19–25.
Gottlieb DJ, Yenokyan G, Newman AB, et al. Prospective study of obstructive sleep apnea and incident coronary heart disease and heart failure: the Sleep Heart Health Study. Circulation. 2010;122:352–60. This study is the 8-year follow-up of the Sleep Heart Health Study, a large population based study of patients free of coronary artery disease, and showed that OSA was a significant predictor of incident coronary artery disease, myocardial infarction, revascularization procedure, or cardiovascular death.
Mooe T, Franklin KA, Holmström K, Rabben T, Wiklund U. Sleep disordered breathing and coronary artery disease: long-term prognosis. Am J Respir Crit Care Med. 2001;164:1910–3.
Szymanski FM, Filipiak KJ, Hrynkiewicz-Szymanska A, et al. Clinical characteristics of patients with acute coronary syndrome at high clinical suspicion for obstructive sleep apnea syndrome. Hell J Cardiol. 2013;54:348–55.
Konecny T, Sert Kuniyoshi F, Orban M, et al. Under-diagnosis of sleep apnea in patients after acute myocardial infarction. J Am Coll Cardiol. 2010;56(9):742–3.
Carlson JT, Rangemark C, Hedner JA. Attenuated endothelium dependent vascular relaxation in patients with sleep apnea. J Hypertens. 1996;14:577–84.
Bradley TD, Hall MJ, Ando S, Floras JS. Hemodynamic effects of simulated obstructive apneas in humans with and without heart failure. Chest. 2001;119:1827–35.
Hamilton GS, Meredith IT, Walker AM, Solin P. Obstructive sleep apnea leads to transient uncoupling of coronary blood flow and myocardial work in humans. Sleep. 2009;32:263–70.
Steiner S, Jax T, Evers S, Hennersdorf M, Schwalen A, Strauer BE. Altered blood rheology in obstructive sleep apnea as a mediator of cardiovascular risk. Cardiology. 2005;104:92–6.
Lévy P, Pépin JL, Arnaud C, Baguet JP, Dematteis M, Mach F. Obstructive sleep apnea and atherosclerosis. Prog Cardiovasc Dis. 2009;5:400–10.
Drager LF, Bortolotto LA, Lorenzi MC, et al. Early signs of atherosclerosis in obstructive sleep apnea. Am J Respir Crit Care Med. 2005;172:613–8.
Minoguchi K, Yokoe T, Tazaki T, et al. Increased carotid intima-media thickness and serum inflammatory markers in obstructive sleep apnea. Am J Respir Crit Care Med. 2005;172:625–30.
Baguet JP, Hammer L, Levy P, et al. The severity of oxygen desaturation is predictive of carotid wall thickening and plaque occurrence. Chest. 2005;128:3407–12.
Sorajja D, Gami AS, Somers VK, et al. Independent association between obstructive sleep apnea and subclinical coronary artery disease. Chest. 2008;133:927–33.
Inami T, Seino Y, Otsuka T, et al. Links between sleep disordered breathing, coronary atherosclerotic burden, and cardiac biomarkers in patients with stable coronary artery disease. J Cardiol. 2012;60:180–6.
Tan A, Hau W, Ho HH, et al. OSA and coronary plaque characteristics. Chest. 2014;145:322–30.
Sharma S, Gebregziabher M, Parker AT, et al. Independent association between obstructive sleep apnea and noncalcified coronary plaque demonstrated by noninvasive coronary computed tomography angiography. Clin Cardiol. 2012;35:641–5.
Alonso-Fernandez A, Garcıa Rıo F, Racionero MA, et al. Cardiac rhythm disturbances an ST segment depression episodes in patients with obstructive sleep apnea-hypopnea syndrome and its mechanisms. Chest. 2005;127:15–22.
Mooe T, Franklin KA, Wiklund U, Rabben T, Holmström K. Sleep-disordered breathing and myocardial ischemia in patients with coronary artery disease. Chest. 2000;117:1597–602.
Kuniyoshi FH, Garcia-Touchard A, Gami AS, et al. Day–night variation of acute myocardial infarction in obstructive sleep apnea. J Am Coll Cardiol. 2008;52:343–6.
Shah N, Redline S, Yaggi HK, et al. Obstructive sleep apnea and acute myocardial infarction severity: ischemic preconditioning? Sleep Breath. 2013;17:819–26. This study found that OSA was associated with smaller infarct size in patients presenting with nonfatal myocardial infarct.
Stephan S, Schueller PO, Schulze VM, Strauer BE. Occurrence of coronary collateral vessels in patients with sleep apnea and total coronary occlusion. Chest. 2010;137:516–20.
Berger S, Aronson D, Lavie P, Lavie L. Endothelial progenitor cells in acute myocardial infarction and sleep-disordered breathing. Am J Respir Crit Care Med. 2013;187:90–8.
Nakashima H, Katayama T, Takagi C, et al. Obstructive sleep apnea inhibits the recovery of left ventricular function in patients with acute myocardial infarction. Eur Heart J. 2006;27:2317–22.
Sert Kuniyoshi FH, Singh P, Gami AS, et al. Patients with obstructive sleep apnea exhibit impaired endothelial function after myocardial infarction. Chest. 2011;140:62–7.
Lee CH, Khoo SM, Chan MY, et al. Severe obstructive sleep apnea and outcomes following myocardial infarction. J Clin Sleep Med. 2011;15(7):616–21.
Schiza SE, Simantirakis E, Bouloukaki I, et al. Sleep disordered breathing in patients with acute coronary syndromes. J Clin Sleep Med. 2012;15(8):21–6.
Romero-Corral A, Caples SM, Lopez-Jimenez F, Somers VK. Interactions between obesity and obstructive sleep apnea: implications for treatment. Chest. 2010;137:711–9.
Marin JM, Carrizo SJ, Vicente E, Agusti AG. Long-term cardiovascular outcomes in men with obstructive sleep apnoea-hypopnoea with or without treatment with continuous positive airway pressure: an observational study. Lancet. 2005;365:1046–53.
Milleron O, Pilliere R, Foucher A, et al. Benefits of obstructive sleep apnea treatment in coronary artery disease: a long term follow-up study. Eur Heart J. 2004;25:728–34.
Franklin KA, Nilsson JB, Sahlin C, Naslund U. Sleep apnea and nocturnal angina. Lancet. 1995;345:1085–7.
Peled N, Abinader EG, Pillar G, Sharif D, Lavie P. Nocturnal ischemic events in patients with obstructive sleep apnea syndrome and ischemic heart disease: effects of continuous positive air pressure treatment. J Am Coll Cardiol. 1999;34:1744–9.
Garcia-Rio F, Alonso-Fernandez A, Armada E, et al. CPAP effect on recurrent episodes in patients with sleep apnea and myocardial infarction. Int J Cardiol. 2013;30(168):1328–35.
Shah N, Kizer JR, Mohsenin V. Obstructive sleep apnea in the acute myocardial infarction setting—should I treat my patient? J Sleep Disor.2013. Treat Care 2:1.
Esquinas C, Sanchez-de-la Torre M, Aldoma A, et al. Rationale and methodology of the impact of continuous positive airway pressure on patients with ACS and nonsleepy OSA: The ISAACC Trial. Clin Cardiol. 2013;36:9:495–501. Methodology of the ISAAC trial: Impact of Continuous Positive Airway Pressure on Patients with Acute coronary syndrome and Non-sleepy OSA.
McEvoy D, Anderson CS, Antic NA, et al. The sleep apnea cardiovascular endpoints (SAVE) trial: rationale and start-up phase. J Thorac Dis. 2010;2(3):138–43.
Compliance with Ethics Guidelines
Conflict of Interest
B. Cepeda-Valery, S. Acharjee, A. Romero-Corral, G. S. Pressman, and A. S. Gami declare that they have no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Author information
Authors and Affiliations
Corresponding author
Additional information
This article is part of the Topical Collection on Management of Acute Coronary Syndromes
Rights and permissions
About this article
Cite this article
Cepeda-Valery, B., Acharjee, S., Romero-Corral, A. et al. Obstructive Sleep Apnea and Acute Coronary Syndromes: Etiology, Risk, and Management. Curr Cardiol Rep 16, 535 (2014). https://doi.org/10.1007/s11886-014-0535-y
Published:
DOI: https://doi.org/10.1007/s11886-014-0535-y