Abstract
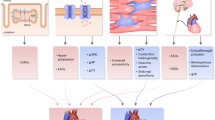
Heart failure is a major public health concern that is frequently complicated by ventricular arrhythmias. Sustained ventricular tachycardia is associated with an increased risk for progressive heart failure and sudden death. We summarize the current management strategies for ventricular tachycardia in heart failure patients, including implantable cardioverter-defibrillator therapy, pharmacologic therapy, catheter ablation techniques, ventricular assist device therapy, and heart transplantation.
Similar content being viewed by others
Abbreviations
- ALIVE:
-
Azimilide Postinfarct Survival Evaluation
- ANDROMEDA:
-
Antiarrhythmic Trial with Dronedarone in Moderate to Severe CHF Evaluating Morbidity Decrease
- CAPRICORN:
-
Carvedilol Post-Infarct Survival Control in Left Ventricular Dysfunction
- CHF-STAT:
-
Congestive Heart Failure Survival Trial of Antiarrhythmic Therapy
- CIBIS-II:
-
Cardiac Insufficiency Bisoprolol Study II
- COPERNICUS:
-
Carvedilol Prospective Randomized Cumulative Survival
- GESICA:
-
Grupo de Estudio de la Sobrevida en la Insuficiencia Cardiaca en Argentina
- MERLIN TIMI-36:
-
Metabolic Efficiency with Ranolazine for Less Ischemia in Non-ST Elevation Acute Coronary Syndromes
- MERIT-HF:
-
Metoprolol CR/XL Randomized Intervention Trial in Congestive Heart Failure
- SCD-HeFT:
-
Sudden Cardiac Death in Heart Failure
- SHIELD:
-
Shock Inhibition Evaluation with Azimilide
References
Papers of particular interest, published recently, have been highlighted as: • Of importance
Lloyd-Jones D, Adams RJ, Brown TM, et al. Heart disease and stroke statistics–2010 update: a report from the American Heart Association. Circulation. 2010;121(7):e46–215.
Luu M, Stevenson WG, Stevenson LW, et al. Diverse mechanisms of unexpected cardiac arrest in advanced heart failure. Circulation. 1989;80:1675–80.
Doval HC, Nul DR, Grancelli HO, et al. Nonsustained ventricular tachycardia in severe heart failure: independent marker of increased mortality due to sudden death. Circulation. 1996;94(12):3198–203.
Maskin CS, Siskind SJ, LeJemtel TH. High prevalence of nonsustained ventricular tachycardia in severe congestive heart failure. Am Heart J. 1984;107:896–901.
Packer M. Lack of relation between ventricular arrhythmias and sudden death in patients with chronic heart failure. Circulation. 1992;85:I50–6.
Moss AJ, Hall WJ, Cannom DS, et al. Improved survival with an implanted defibrillator in patients with coronary disease at high risk for ventricular arrhythmia. N Engl J Med. 1996;335:1933–40.
Buxton A, Lee K, Fisher J, et al. A randomized study of the prevention of sudden death in patients with coronary artery disease. N Engl J Med. 1999;341:1882–90.
• Myerburg RJ, Reddy V, Castellanos A. Indications for implantable cardioverter-defibrillators based on evidence and judgment. J Am Coll Cardiol. 2009;54(9):747–63. This article is particularly useful to the reader because it thoroughly reviews the evidence behind ICD use for primary and secondary prevention, as well as rare disorders. The authors critically analyze the major studies and point out the limitations in trial design and data interpretation. The authors also discuss the economic impact and issues related to risk stratification.
Poole JE, Johnson GW, Hellkamp AS, et al. Prognostic importance of defibrillator shocks in patients with heart failure. N Engl J Med. 2008;359(10):1009–17.
Sweeney MO. The contradiction of appropriate shocks in primary prevention ICDs: increasing and decreasing the risk of death. Circulation. 2010;122(25):2638–41.
• Saxon L, Hayes DL, Gilliam FR, et al. Long term outcome after ICD and CRT implantation and influence of remote device follow up. Circulation. 2010;122:2359–67. This article presented a study of the largest series of patients followed chronically with ICD and cardiac resynchronization therapy-defibrillator devices, most of whom were implanted for primary prevention indications in the setting of heart failure, showing survivals markedly better if devices are followed on a remote network.
Godemann F, Butter C, Lampe F, et al. Determinants of the quality of life (QoL) in patients with an implantable cardioverter/defibrillator (ICD). Qual Life Res. 13(2):411–6.
Bardy GH, Lee KL, Mark DB, et al. Amiodarone or an implantable cardioverter–defibrillator for congestive heart failure. N Engl J Med. 2005;352(3):225–37.
Reddy VY, Reynolds MR, Neuzil P, et al. Prophylactic catheter ablation for the prevention of defibrillator therapy. N Engl J Med. 2007;357(26):2657–65.
Zipes DP, Camm AJ, Borggrefe M, Buxton AE, et al. ACC/AHA/ESC 2006 guidelines for management of patients with ventricular arrhythmias and the prevention of sudden cardiac death-executive summary a report of the American College of Cardiology/American Heart Association Task Force and the European Society of Cardiology Committee for Practice Guidelines. J Am Coll Cardiol. 2006;48(5):1064–108.
Echt DS, Liebson PR, Mitchell LB, et al. Mortality and morbidity in patients receiving encainide, flecainide, or placebo. The cardiac arrhythmia suppression trial. N Engl J Med. 1991;324(12):781–8.
MERIT-HF Study Group. Effect of metoprolol CR/XL in chronic heart failure: metoprolol CR/XLrandomized Intervention trial in congestive heart failure (MERIT-HF). Lancet. 1999;353:2001–7.
Lechat P, Brunhuber K, Hofmann R, et al. The cardiac insufficiency bisoprolol study II (CIBIS-II): a randomized trial. Lancet. 1999;353:9–13.
Packer M, Coats AJ, Fowler MB, et al. Effect of carvedilol on survival in severe chronic heart failure. N Engl J Med. 2001;344:1651–8.
Dargie HJ. Effect of carvedilol on outcome after myocardial infarction in patients with left-ventricular dysfunction: the CAPRICORN randomized trial. Lancet. 2001;357:1385–90.
Dorval HC, Nul DR, Grancelli HO, et al. Randomized trial of low-dose amiodarone in severe congestive heart failure. Lancet. 1994;344:493–8.
Deedwania PC, Singh BN, Ellenbogen K. Spontaneous conversion and maintenance of sinus rhythm by amiodarone in patients with heart failure and atrial fibrillation: observations from the veterans affairs congestive heart failure survival trial of antiarrhythmic therapy (CHF-STAT). Circulation. 1998;98:2574–9.
Piccini JP, Berger JS, O’Connor CM. Amiodarone for the prevention of sudden cardiac death: a meta-analysis of randomized controlled trials. Eur Heart J. 2009;30:1245–53.
Korber L, Torp-Peterson C, McMurray JJV, et al. Increased mortality after dronedarone therapy for severe heart failure. N Engl J Med. 2008;358:2678–87.
Waldo AL, Camm AJ, de Ruyter H, et al. Effect of d-sotalol on mortality in patients with left ventricular dysfunction after recent and remote myocardial infarction. The SWORD Investigators. Survival With Oral d-Sotalol. Lancet. 1996;348:7.
Dorian P, Borggrefe M, Al-Khalidi HR, on behalf of the SHock Inhibition Evaluation with azimiLiDE(SHIELD) investigators, et al. Placebo-controlled, randomized clinical trial of azimilide for prevention of ventricular tachyarrhythmias in patients with an implantable cardioverter defibrillator. Circulation. 2004;110:3646–54.
Hohnloser S, Dorian P, Al-Khalidi H, Brum J, Tatla D, Pratt C. Electrical storms in patients with implantable defibrillators: results from Shock Inhibition Evaluation with Azimilide (SHIELD) trial. Circulation. 2005;112:II-492.
• Das MK, Zipes DP. Antiarrhythmic and nonantiarrhythmic drugs for sudden cardiac death prevention. J Cardiovasc Pharmacol. 2010;55:438–49. This review article provides an excellent and comprehensive overview of the current pharmacologic therapy for ventricular arrhythmia and sudden death prevention. The article outlines the key studies related to each drug and serves as a useful reference for the reader.
Morrow DA, Scirica BM, Karwatowska-Prokopczuk E, et al. Effects of ranolazine on recurrent cardiovascular events in patients with non–st-elevation acute coronary syndromes. JAMA. 2007;297(16):1775–83.
Aliot EM, Stevenson WG, Almendral-Garrote JM, et al. EHRA/HRS expert consensus on catheter ablation of ventricular arrhythmias: developed in a partnership with the European Heart Rhythm Association (EHRA), a Registered Branch of the European Society of Cardiology (ESC), and the Heart Rhythm Society (HRS); in collaboration with the American College of Cardiology (ACC) and the American Heart Association (AHA). Heart Rhythm. 2009;6(6):886–933.
Stevenson WG, Soejima K. Catheter ablation for ventricular tachycardia. Circulation. 2007;115:2750–60.
Cesario D, Saxon L, Cao M et al.Ventricular tachycardia in the era of ventricular assist devices. J Cardiovasc Elecrophysiol. 2010;1–5.
Abuissa H, Roshan J, Lim B, Asirvatham SJ. Use of the impella microaxial blood pump for ablation of hemodynamically unstable ventricular tachycardia. J Cardiovasc Electrophysiol. 2010;21:485–61.
Friedman PA, Munger TM, Torres N, Rihal C. Percutaneous endocardial and epicardial ablation of hypotensive ventricular tachycardia with percutaneous left ventricular assist in the electrophysiology laboratory. J Cardiovasc Electrophysiol. 2007;18:106–9.
Windecker S. Percutaneous left ventricular assist devices for treatment of patients with cardiogenic shock. Curr Opin Crit Care. 2007;13:521–7.
Cook S, Windecker S. Percutaneous left ventricular assist devices during cardiogenic shock and high-risk percutaneous coronary interventions. Curr Cardiol Rep. 2009;11:369–76.
Farrar DJ, Hill JD, Gray LA, et al. Successful biventricular circulatory support as a bridge to cardiac transplantation during prolonged ventricular fibrillation and asystole. Circulation. 1989;80:147–51.
Pennington DG, Reedy JE, Swartz MT, et al. Univentricular versus biventricular assist device support. J Heart Lung Transplant. 1991;10(2):258–63.
Oz MC, Rose EA, Slater J, et al. Malignant ventricular arrhythmias are well tolerated in patients receiving long-term left ventricular assist devices. J Am Coll Cardiol. 1994;24(7):1688–91.
Harding J, Piacentino III V, Rothman S, et al. Prolonged repolarization after ventricular assist device support is associated with arrhythmias in humans with congestive heart failure. J Card Fail. 2005;11(3):227–32.
• Andersen M, Videbaek R, Boesgaard S, et al. Incidence of ventricular arrhythmias in patients on long-term support with a continuous-flow assist device (HeartMate II). J Heart Lung Transplant. 2009;28(7):733–5. Ventricular arrhythmias continue to be an issue in patients who have received newer-generation continuous-flow MCS devices. This retrospective study calls attention to the problem, and is one of the few articles assessing ventricular arrhythmias in this growing technology.
Bedi M, Kormos R, Winowich S, et al. Ventricular arrhythmias during left ventricular assist device support. Am J Cardiol. 2007;99(8):1151–3.
Ziv O, Dizon J, Thosani A, et al. Effects of left ventricular assist device therapy on ventricular arrhythmias. J Am Coll Cardiol. 2005;45(9):1428–34.
Cantillon DJ, Tarakji KG, Kumbhani DJ, et al. Improved survival among ventricular assist device recipients with a concomitant implantable cardioverter-defibrillator. Heart Rhythm. 2010;7(4):466–71.
Dandamudi G, Ghumman WS, Das MK, Miller JM. Endocardial catheter ablation of ventricular tachycardia in patients with ventricular assist devices. Heart Rhythm. 2007;4(9):1165–9.
Osaki S, Alberte C, Murray MA, et al. Successful radiofrequency ablation therapy for intractable ventricular tachycardia with a ventricular assist device. J Heart Lung Transplant. 2008;27(3):353–6.
Olivari M, Windle J. Cardiac transplantation in patients with refractory ventricular arrhythmias. J Heart Lung Transplant. 2000;19(8):S38–42.
Disclosure
Conflicts of interest: M.W. Fong: none; L. Grazette: none; D. Cesario: has been a consultant for Boston Scientific and has received honoraria from Sanofi-Aventis and Medtronic; M. Cao: none; L. Saxon: has been a consultant for Boston Scientific, Medtronic, and St. Jude Medical.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Fong, M.W., Grazette, L., Cesario, D. et al. Treatment of Ventricular Tachycardia in Patients with Heart Failure. Curr Cardiol Rep 13, 203–209 (2011). https://doi.org/10.1007/s11886-011-0182-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11886-011-0182-5