Abstract
Purpose of Review
The aim of this study was to determine the effects of aerobic exercise on peak oxygen uptake (peak VO2), minute ventilation/carbon dioxide production (VE/VCO2 slope), and health-related quality of life (HRQoL) among patients with heart failure (HF) and preserved ejection fraction (HFpEF).
Recent Findings
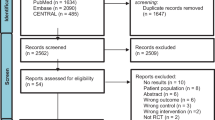
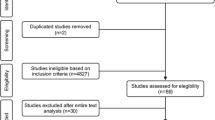
We conducted a Cochrane Library, MEDLINE/PubMed, Physiotherapy Evidence Database, and SciELO search (from 1985 to May 2019) for randomized controlled trials that evaluated the effects of aerobic exercise in HFpEF patients. We calculated the mean differences (MD) and 95% confidence interval (CI). Ten intervention studies were included providing a total of 399 patients. Compared with control, aerobic exercise resulted in improvement in peak VO2 MD 1.9 mL kg−1 min−1 (95% CI 1.3 to 2.5; N = 314) and HRQoL measured by Minnesota Living with Heart Failure MD 5.4 (95% CI − 10.5 to − 0.2; N = 256). No significant difference in VE/VCO2 slope was found between participants in the aerobic exercise group and the control group. The quality of evidence for peak VO2 and HRQoL was assessed as being moderate.
Summary
Aerobic exercise moderately improves peak VO2 and HRQoL and should be considered a strategy of rehabilitation of HFpEF individuals.




Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance
Haykowsky M, Brubaker P, Kitzman D. Role of physical training in heart failure with preserved ejection fraction. Curr Heart Fail Rep. 2012;9(2):101–6.
Tucker WJ, Lijauco CC, Hearon CM, et al. Mechanisms of the improvement in peak VO2 with exercise training in heart failure with reduced or preserved ejection fraction. Heart, Lung and Circulation. 2018;27:9–21.
Montero D, Diaz-Cañestro C. Determinants of exercise intolerance in heart failure with preserved ejection fraction: a systematic review and meta-analysis. Int J Cardiol. 2018;254:224–9.
Ponikowski P, Voors AA, Anker SD, Bueno H, Cleland JG, Coats AJ, et al. 2016 ESC guidelines for the diagnosis and treatment of acute and chronic heart failure: the task force for the diagnosis and treatment of acute and chronic heart failure of the European Society of Cardiology (ESC). Developed with the special contribution of the Heart Failure Association (HFA) of the ESC. Eur J Heart Fail. 2016;18:891–975.
Pandey A, Patel KV, Vaduganathan M, Sarma S, Haykowsky MJ, Berry JD, et al. Physical activity, fitness, and obesity in heart failure with preserved ejection fraction. JACC Heart Fail. 2018;6(12):975–82.
Redfield MM. Heart failure with preserved ejection fraction. N Engl J Med. 2016;375(19):1868–77.
Upadhya B, Haykowsky MJ, Eggebeen J, Kitzman DW. Exercise intolerance in heart failure with preserved ejection fraction: more than a heart problem. JGeriatrCardiol. 2015;12(3):294–304. https://doi.org/10.11909/j.issn.1671-5411.2015.03.013.
Dickstein K, Cohen-Solal A, Filippatos G, JJ MM, Ponikowski P, Poole-Wilson PA, et al. Developed in collaboration with the Heart Failure Association of the ESC (HFA) and endorsed by the European Society of Intensive Care Medicine (ESICM). Eur J Heart Fail. 2008;10:933–89.
Gomes Neto M, Durães AR, Conceição LSR, Saquetto MB, Ellingsen Ø, Carvalho VO. High intensity interval training versus moderate intensity continuous training on exercise capacity and quality of life in patients with heart failure with reduced ejection fraction: a systematic review and meta-analysis. Int J Cardiol. 2018;261:134–41.
Dieberg G, Ismail H, Giallauria F, Smart NA. Clinical outcomes and cardiovascular responses to exercise training in heart failure patients with preserved ejection fraction: a systematic review and meta-analysis. J Appl Physiol (1985). 2015;119(6):726–33.
Nadruz W Jr, West E, Sengeløv M, Santos M, Groarke JD, Forman DE, et al. Prognostic value of cardiopulmonary exercise testing in heart failure with reduced, midrange, and preserved ejection fraction. J Am Heart Assoc. 2017;6(11):e006000.
Moher D, Liberati A, Tetzlaff J, Altman DG, for the PRISMA Group. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. BMJ. 2009;339:b2535.
Higgins JPT, Green S. The Cochrane library. Issue 4. Chichester: John Wiley & Sons; 2006. Cochrane handbook for Systematic Reviews of Interventions 4.2.6 [update September 2006
Olivo SA, Macedo LG, Gadotti IN, Fuentes J, Stanton T, Magee DJ. Scales to assess the quality of randomized controlled trials: a systematic review. PhysTher. 2008;88(2):156–75.
Verhagen AP, de Vet HCW, de Bie RA, Kessels AGH, Boers M, Bouter LM, et al. The Delphi list: a criteria list for quality assessment of randomized clinical trials for conducting systematic reviews developed by Delphi consensus. J Clin Epidemiol. 1998;51(12):1235–41.
Maher CG, Sherrington C, Herbert RD, Moseley AM, Elkins M. Reliability of the PEDro scale for rating of quality randomized controlled trials. Phys Ther. 2003;83(8):713–21.
Wan X, Wang W, Liu J, Tong T. Estimating the sample mean and standard deviation from the sample size, median, range and/or interquartile range. BMC Med Res Methodol. 2014;14:135. https://doi.org/10.1186/1471-2288-14-135.
Higgins JP, Thompson SG, Deeks JJ, Altman DG. Measuring inconsistency in meta-analyses. BMJ. 2003;327:557–60.
Collaboration TC. Available at: www.cochrane.org. [Accessed 3 Feb 2008].
• Maldonado-Martín S, Brubaker PH, Eggebeen J, Stewart KP, Kitzman DW. Association between 6-minute walk test distance and objective variables of functional capacity after exercise training in elderly heart failure patients with preserved ejection fraction: a randomized exercise trial. Arch Phys Med Rehabil. 2017;98(3):600–3 This study demonstrated Peak VO2 improved in the AE.
Kitzman DW, Brubaker P, Morgan T, Haykowsky M, Hundley G, Kraus WE, et al. Effect of caloric restriction or aerobic exercise training on peak oxygen consumption and quality of life in obese older patients with heart failure with preserved ejection fraction: a randomized clinical trial. JAMA. 2016;315(1):36–46.
• Angadi SS, Mookadam F, Lee CD, Tucker WJ, Haykowsky MJ, Gaesser GA. High-intensity interval training vs. moderate-intensity continuous exercise training in heart failure with preserved ejection fraction: a pilot study. J Appl Physiol (1985). 2015;119(6):753–8 This study demonstrated the HIIT improved VO 2 peak and left ventricular diastolic dysfunction grade.
• Kitzman DW, Brubaker PH, Herrington DM, Morgan TM, Stewart KP, Hundley WG, et al. Effect of endurance exercise training on endothelial function and arterial stiffness in older patients with heart failure and preserved ejection fraction: a randomized, controlled, single-blind trial. J Am Coll Cardiol. 2013;62(7):584–92. https://doi.org/10.1016/j.jacc.2013.04.033 Exercise training increased peak VO 2 and quality of life.
Yeh GY, Wood MJ, Wayne PM, Quilty MT, Stevenson LW, Davis RB, et al. Tai chi in patients with heart failure with preserved ejection fraction. Congest Heart Fail. 2013;19(2):77–84.
• Alves AJ, Ribeiro F, Goldhammer E, Rivlin Y, Rosenschein U, Viana JL, et al. Exercise training improves diastolic function in heart failure patients. Med Sci Sports Exerc. 2012;44(5):776–85 Exercise training increased the mean ratio of early to late mitral inflow velocities (E/A ratio) and decreased deceleration time (DT) of early filling in patients with mild and preserved LVEF.
Haykowsky MJ, Brubaker PH, Stewart KP, Morgan TM, Eggebeen J, Kitzman DW. Effect of endurance training on the determinants of peak exercise oxygen consumption in elderly patients with stable compensated heart failure and preserved ejection fraction. J Am Coll Cardiol. 2012;60(2):120–8.
• Smart NA, Haluska B, Jeffriess L, Leung D. Exercise training in heart failure with preserved systolic function: a randomized controlled trial of the effects on cardiac function and functional capacity. Congest Heart Fail. 2012;18(6):295–301 After exercise training, the increment in peak VO 2.
Kitzman DW, Brubaker PH, Morgan TM, Stewart KP, Little WC. Exercise training in older patients with heart failure and preserved ejection fraction: a randomized, controlled, single-blind trial. Circ Heart Fail. 2010;3(6):659–67.
• Gary RA, Sueta CA, Dougherty M, Rosenberg B, Cheek D, Preisser J, etal. Home-based exercise improves functional performance and quality of life in women with diastolic heart failure. Heart Lung 2004;33(4):210–218. Exercise improved in the 6-min walk test.
Agostoni P, Corrà U, Cattadori G, Veglia F, La Gioia R, Scardovi AB, et al. Metabolic exercise test data combined with cardiac and kidney indexes, the MECKI score: a multi parametric approach to heart failure prognosis. Int J Cardiol. 2013;167:2710–8.
Faller H, Störk S, Schowalter M, Steinbüchel T, Wollner V, Ertl G, et al. Is health-related quality of life an independent predictor of survival in patients with chronic heart failure? J Psychosom Res. 2007;63(5):533–8.
Frankenstein L, Nelles M, Hallerbach M, Dukic D, Fluegel A, Schellberg D, et al. Prognostic impact of peak VO2-changes in stable CHF on chronic beta-blocker treatment. Int J Cardiol. 2007;122(2):125–30.
Ades PA, Keteyian SJ, Balady GJ, et al. Cardiac rehabilitation exercise and self-care for chronic heart failure. JACC Heart Fail. 2013;1(6):540–7.
Arnold M, Rajda M, Ignaszewski A, Howlett J, Leblanc M-H. Changes in the Minnesota living with heart failure questionnaire score and clinical outcomes in a large contemporary population of ambulatory heart failure patients in the Canadian heart failure network. J Card Fail. 2012;18(8 Supplement):S79.
Poggio R, Arazi HC, Giorgi M, Miriuka SG. Prediction of severe cardiovascular events by VE/VCO2 slope versus peak VO2 in systolic heart failure: a meta-analysis of the published literature. Am Heart J. 2010;160(6):1004–14.
Sato T, Yoshihisa A, Kanno Y, Suzuki S, Yamaki T, Sugimoto K, et al. Cardiopulmonary exercise testing as prognostic indicators: comparisons among heart failure patients with reduced, mid-range and preserved ejection fraction. Eur J Prev Cardiol. 2017;24(18):1979–87. https://doi.org/10.1177/2047487317739079.
Ingle L. Prognostic value and diagnostic potential of cardiopulmonary exercise testing in patients with chronic heart failure. Euro J Heart Fail. 2008;10:112–8.
Pozehl BJ, Duncan K, Hertzog M, McGuire R, Norman JF, Artinian NT, et al. Study of adherence to exercise in heart failure: the HEART camp trial protocol. BMC Cardiovasc Disord. 2014;14:172.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Mansueto Gomes Neto, André Rodrigues Durães, Lino Sergio Rocha Conceição, Leonardo Roever, Tong Liu7 Gary Tse, Giuseppe Biondi-Zoccai, Ana Lucia Barbosa Goes, Lura Gonzalez Nogueira Alves, Øyvind Ellingsen, and Vitor Oliveira Carvalho declare they have no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Evidence-Based Medicine, Clinical Trials and Their Interpretations
Rights and permissions
About this article
Cite this article
Gomes-Neto, M., Durães, A.R., Conceição, L.S.R. et al. Effect of Aerobic Exercise on Peak Oxygen Consumption, VE/VCO2 Slope, and Health-Related Quality of Life in Patients with Heart Failure with Preserved Left Ventricular Ejection Fraction: a Systematic Review and Meta-Analysis. Curr Atheroscler Rep 21, 45 (2019). https://doi.org/10.1007/s11883-019-0806-6
Published:
DOI: https://doi.org/10.1007/s11883-019-0806-6