Abstract
Acute coronary syndromes (ACS) represent an enormous disease burden, especially in the Western world, where they are one of the largest causes of mortality and morbidity. Patients suffering an acute coronary event are at very high risk of further coronary events, and although improvements in medical therapy over the past two decades have significantly reduced the risk, it remains high. 3-Hydroxy-3-methylglutaryl coenzyme A reductase inhibitors (statins) are now fully established in the primary and secondary prevention of stable coronary heart disease, and recently a substantial body of evidence has proven their efficacy in ACS. This paper examines the evidence for statin use in ACS.
Similar content being viewed by others
References and Recommended Reading
Rosamond W, Flegal K, Friday G, et al.: Heart disease and stroke statistics-2007 update: a report from the American Heart Association Statistics Committee and Stroke Statistics Subcommittee. Circulation 2007, 115:e69–e171.
Hospital Episode Statistics 2004–2005. Available at http://www.hesonlinenhsuk2006. Accessed October 10, 2007.
Naghavi M, Libby P, Falk E, et al.: From vulnerable plaque to vulnerable patient: a call for new definitions and risk assessment strategies: Part II. Circulation 2003, 108:1772–1778.
Naghavi M, Libby P, Falk E, et al.: From vulnerable plaque to vulnerable patient: a call for new definitions and risk assessment strategies: Part I. Circulation 2003, 108:1664–1672.
Wallentin L, Lagerqvist B, Husted S, et al.: Outcome at 1 year after an invasive compared with a non-invasive strategy in unstable coronary-artery disease: the FRISC II invasive randomised trial. FRISC II Investigators. Fast Revascularisation during Instability in Coronary artery disease. Lancet 2000, 356:9–16.
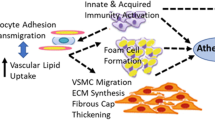
Libby P, Theroux P: Pathophysiology of coronary artery disease. Circulation 2005, 111:3481–3488.
Gordon T, Castelli WP, Hjortland MC, et al.: Predicting coronary heart disease in middle-aged and older persons. The Framington study. JAMA 1977, 238:497–499.
Baigent C, Keech A, Kearney PM, et al.: Efficacy and safety of cholesterol-lowering treatment: prospective meta-analysis of data from 90,056 participants in 14 randomised trials of statins. Lancet 2005, 366:1267–1278.
Randomised trial of cholesterol lowering in 4444 patients with coronary heart disease: the Scandinavian Simvastatin Survival Study (4S). Lancet 1994, 344:1383–1389.
Prevention of cardiovascular events and death with pravastatin in patients with coronary heart disease and a broad range of initial cholesterol levels. The Long-Term Intervention with Pravastatin in Ischaemic Disease (LIPID) Study Group. N Engl J Med 1998, 339:1349–1357.
Influence of pravastatin and plasma lipids on clinical events in the West of Scotland Coronary Prevention Study (WOSCOPS). Circulation 1998, 97:1440–1445.
Collins R, Peto R, Armitage J: The MRC/BHF Heart Protection Study: preliminary results. Int J Clin Pract 2002, 56:53–56.
Sacks FM, Pfeffer MA, Moye LA, et al.: The effect of pravastatin on coronary events after myocardial infarction in patients with average cholesterol levels. Cholesterol and Recurrent Events Trial investigators. N Engl J Med 1996, 335:1001–1009.
Sever PS, Dahlof B, Poulter NR, et al.: Prevention of coronary and stroke events with atorvastatin in hypertensive patients who have average or lower-than-average cholesterol concentrations, in the Anglo-Scandinavian Cardiac Outcomes Trial-Lipid Lowering Arm (ASCOT-LLA): a multicentre randomised controlled trial. Lancet 2003, 361:1149–1158.
Buchwald H, Varco RL, Boen JR, et al.: Effective lipid modification by partial ileal bypass reduced long-term coronary heart disease mortality and morbidity: five-year posttrial follow-up report from the POSCH. Program on the Surgical Control of the Hyperlipidemias. Arch Intern Med 1998, 158:1253–1261.
Buchwald H, Varco RL, Matts JP, et al.: Effect of partial ileal bypass surgery on mortality and morbidity from coronary heart disease in patients with hypercholesterolemia. Report of the Program on the Surgical Control of the Hyperlipidemias (POSCH). N Engl J Med 1990, 323:946–955.
Falk E, Shah PK, Fuster V: Coronary plaque disruption. Circulation 1995, 92:657–671.
Chan WL, Pejnovic N, Hamilton H, et al.: Atherosclerotic abdominal aortic aneurysm and the interaction between autologous human plaque-derived vascular smooth muscle cells, type 1 NKT, and helper T cells. Circ Res 2005, 96:675–683.
Toutouzas K, Drakopoulou M, Mitropoulos J, et al.: Elevated plaque temperature in non-culprit de novo atheromatous lesions of patients with acute coronary syndromes. J Am Coll Cardiol 2006, 47:301–306.
Blake GJ, Ridker PM: C-reactive protein and other inflammatory risk markers in acute coronary syndromes. J Am Coll Cardiol 2003, 41(4 Suppl 4):37S–42S.
Davignon J, Ganz P: Role of endothelial dysfunction in atherosclerosis. Circulation 2004, 109(23 Suppl 1):III27–III32.
Watanabe N, Ikeda U: Matrix metalloproteinases and atherosclerosis. Curr Atheroscler Rep 2004, 6:112–120.
Haramaki N, Ikeda H, Takenaka K, et al.: Fluvastatin alters platelet aggregability in patients with hypercholesterolemia: possible improvement of intraplatelet redox imbalance via HMG-CoA reductase. Arterioscler Thromb Vasc Biol 2007, 27:1471–1477.
Sanguigni V, Pignatelli P, Lenti L, et al.: Short-term treatment with atorvastatin reduces platelet CD40 ligand and thrombin generation in hypercholesterolemic patients. Circulation 2005, 111:412–419.
Mitsios JV, Papathanasiou AI, Elisaf M, et al.: The inhibitory potency of clopidogrel on ADP-induced platelet activation is not attenuated when it is co-administered with atorvastatin (20 mg/day) for 5 weeks in patients with acute coronary syndromes. Platelets 2005, 16:287–292.
Kwak B, Mulhaupt F, Myit S, Mach F: Statins as a newly recognized type of immunomodulator. Nat Med 2000, 6:1399–1402.
Schonbeck U, Libby P: Inflammation, immunity, and HMG-CoA reductase inhibitors: statins as antiinflammatory agents? Circulation 2004, 109(21 Suppl 1):II18–II26.
Ray KK, Cannon CP: The potential relevance of the multiple lipid-independent (pleiotropic) effects of statins in the management of acute coronary syndromes. J Am Coll Cardiol 2005, 46:1425–1433.
Ray KK, Morrow DA, Shui A, et al.: Relation between soluble intercellular adhesion molecule-1, statin therapy, and long-term risk of clinical cardiovascular events in patients with previous acute coronary syndrome (from PROVE IT-TIMI 22). Am J Cardiol 2006, 98:861–865.
Kinlay S, Schwartz GG, Olsson AG, Rifai N, et al.: High-dose atorvastatin enhances the decline in inflammatory markers in patients with acute coronary syndromes in the MIRACL study. Circulation 2003, 108:1560–1566.
Link A, Ayadhi T, Bohm M, Nickenig G: Rapid immunomodulation by rosuvastatin in patients with acute coronary syndrome. Eur Heart J 2006, 27:2945–2955.
Ridker PM, Cannon CP, Morrow D, et al.: C-reactive protein levels and outcomes after statin therapy. N Engl J Med 2005, 352:20–28.
Beckman JA, Creager MA: The nonlipid effects of statins on endothelial function. Trends Cardiovasc Med 2006, 16:156–162.
Dilaveris P, Giannopoulos G, Riga M, et al.: Beneficial effects of statins on endothelial dysfunction and vascular stiffness. Curr Vasc Pharmacol 2007, 5:227–237.
Fichtlscherer S, Schmidt-Lucke C, Bojunga S, et al.: Differential effects of short-term lipid lowering with ezetimibe and statins on endothelial function in patients with CAD: clinical evidence for ‘pleiotropic’ functions of statin therapy. Eur Heart J 2006, 27:1182–1190.
Hosokawa S, Hiasa Y, Tomokane T, et al.: The effects of atorvastatin on coronary endothelial function in patients with recent myocardial infarction. Clin Cardiol 2006, 29:357–362.
Furman C, Copin C, Kandoussi M, et al.: Rosuvastatin reduces MMP-7 secretion by human monocyte-derived macrophages: potential relevance to atherosclerotic plaque stability. Atherosclerosis 2004, 174:93–98.
Luan Z, Chase AJ, Newby AC: Statins inhibit secretion of metalloproteinases-1,-2,-3, and-9 from vascular smooth muscle cells and macrophages. Arterioscler Thromb Vasc Biol 2003, 23:769–775.
Spencer FA, Allegrone J, Goldberg RJ, et al.: Association of statin therapy with outcomes of acute coronary syndromes: the GRACE study. Ann Intern Med 2004, 140:857–866.
Fonarow GC, Wright RS, Spencer FA, et al.: Effect of statin use within the first 24 hours of admission for acute myocardial infarction on early morbidity and mortality. Am J Cardiol 2005, 96:611–616.
Liem AH, van Boven AJ, Veeger NJ, et al.: Effect of fluvastatin on ischaemia following acute myocardial infarction: a randomized trial. Eur Heart J 2002, 23:1931–1937.
Thompson PL, Meredith I, Amerena J, et al.: Effect of pravastatin compared with placebo initiated within 24 hours of onset of acute myocardial infarction or unstable angina: the Pravastatin in Acute Coronary Treatment (PACT) trial. Am Heart J 2004, 148:e2.
de Lemos JA, Blazing MA, Wiviott SD, et al.: Early intensive vs a delayed conservative simvastatin strategy in patients with acute coronary syndromes: phase Z of the A to Z trial. JAMA 2004, 292:1307–1316.
Schwartz GG, Olsson AG, Ezekowitz MD, et al.: Effects of atorvastatin on early recurrent ischemic events in acute coronary syndromes: the MIRACL study: a randomized controlled trial. JAMA 2001, 285:1711–1718.
Olsson AG, Schwartz GG, Szarek M, et al.: High-density lipoprotein, but not low-density lipoprotein cholesterol levels influence short-term prognosis after acute coronary syndrome: results from the MIRACL trial. Eur Heart J 2005, 26:890–896.
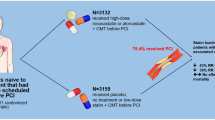
Cannon CP, Braunwald E, McCabe CH, et al.: Intensive versus moderate lipid lowering with statins after acute coronary syndromes. N Engl J Med 2004, 350:1495–1504.
Ray KK, Cannon CP, McCabe CH, et al.: Early and late benefits of high-dose atorvastatin in patients with acute coronary syndromes: results from the PROVE IT-TIMI 22 trial. J Am Coll Cardiol 2005, 46:1405–1410
Wiviott SD, de Lemos JA, Cannon CP, et al.: A tale of two trials: a comparison of the post-acute coronary syndrome lipid-lowering trials A to Z and PROVE IT-TIMI 22. Circulation 2006, 113:1406–1414.
Ridker PM, Morrow DA, Rose LM, et al.: Relative efficacy of atorvastatin 80 mg and pravastatin 40 mg in achieving the dual goals of low-density lipoprotein cholesterol <70 mg/dl and C-reactive protein <2 mg/l: an analysis of the PROVE-IT TIMI-22 trial. J Am Coll Cardiol 2005, 45:1644–1648.
Ray KK, Cannon CP, Cairns R, et al.: Relationship between uncontrolled risk factors and C-reactive protein levels in patients receiving standard or intensive statin therapy for acute coronary syndromes in the PROVE IT-TIMI 22 trial. J Am Coll Cardiol 2005, 46:1417–1424.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Liew, T.V., Ray, K.K. Intensive statin therapy in acute coronary syndromes. Curr Atheroscler Rep 10, 158–163 (2008). https://doi.org/10.1007/s11883-008-0023-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11883-008-0023-1