Abstract
Objective
The current study assessed the knowledge of the medical students regarding the nature of radiation, associated risks, and protective measures.
Method
A cross-sectional study was conducted among international students enrolled in different medical colleges/universities in Xian, PR China. A self-developed and self-reported questionnaire was used for the current study. The descriptive statistics was carried out to summarize the finding of the study. Chi-square and Fisher exact tests were conducted to assess the association of the demographics with knowledge level.
Results
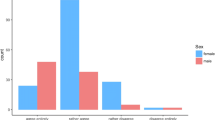
A total of 796 students responded among 980. Most of the participants fell in the age range of 20–25 years (42.6%), being male (67.1%) and having bachelor’s education (56.7%). Participants with previous experience was 58.7%. The age group of 20–25 years (p < 0.001), being male (p < 0.001), having bachelor education (p < 0.001), and previous experience (p = 0.009) was significantly associated with moderate to good knowledge. The overall knowledge about the nature of radiation (96%) and associated risk (82%) was good, but regarding protection, 59% of the participants showed good knowledge.
Conclusion
Most of the participants showed satisfactory result. However, the knowledge regarding protection measures was poor in almost half of the population.


Similar content being viewed by others
Data availability
The data can be requested from the corresponding author on valid request.
References
Mattoon JS (2006) Digital radiography. Vet Comp Orthop Traumatol 19:123–132
Roberts GD, Graham JP (2001) Computed radiography. Vet Clin North Am Equine Pract 17:47–61. https://doi.org/10.1016/s0749-0739(17)30074-3
Bansal T, Beese R (2019) Interpreting a chest X-ray. Br J Hosp Med (Lond) 80:C75–C79. https://doi.org/10.12968/hmed.2019.80.5.C75
Abalo KD, Rage E, Leuraud K et al (2021) Early life ionizing radiation exposure and cancer risks: systematic review and meta-analysis. Pediatr Radiol 51:45–56. https://doi.org/10.1007/s00247-020-04803-0
Rühm W, Laurier D, Wakeford R (2022) Cancer risk following low doses of ionising radiation - current epidemiological evidence and implications for radiological protection. Mutat Res Genet Toxicol Environ Mutagen 873:503436. https://doi.org/10.1016/j.mrgentox.2021.503436
Mazzei-Abba A, Folly CL, Kreis C et al (2021) External background ionizing radiation and childhood cancer: update of a nationwide cohort analysis. J Environ Radioact 238–239:106734. https://doi.org/10.1016/j.jenvrad.2021.106734
Busby C (2022) Ionizing radiation and cancer: the failure of the risk model. Cancer Treat Res Commun 31:100565. https://doi.org/10.1016/j.ctarc.2022.100565
Martin SE, Begun EM, Samir E et al (2019) Incidence and morbidity of radiation-induced hemorrhagic cystitis in prostate cancer. Urology 131:190–195. https://doi.org/10.1016/j.urology.2019.05.034
Miglioretti DL, Lange J, van den Broek JJ et al (2016) Radiation-induced breast cancer incidence and mortality from digital mammography screening: a modeling study. Ann Intern Med 164:205–214. https://doi.org/10.7326/m15-1241
Dong Y, Ridge JA, Ebersole B et al (2019) Incidence and outcomes of radiation-induced late cranial neuropathy in 10-year survivors of head and neck cancer. Oral Oncol 95:59–64. https://doi.org/10.1016/j.oraloncology.2019.05.014
Brown N, Jones L (2013) Knowledge of medical imaging radiation dose and risk among doctors. J Med Imaging Radiat Oncol 57:8–14. https://doi.org/10.1111/j.1754-9485.2012.02469.x
Aldhamy H, Maniatopoulos G, McCune VL et al (2023) Knowledge, attitude and practice of infection prevention and control precautions among laboratory staff: a mixed-methods systematic review. Antimicrob Resist Infect Control 12:57. https://doi.org/10.1186/s13756-023-01257-5
Woodhouse KD, Tremont K, Vachani A et al (2017) A review of shared decision-making and patient decision aids in radiation oncology. J Cancer Educ 32:238–245. https://doi.org/10.1007/s13187-017-1169-8
Hassan QA, Hussein AS, Fadhil AA et al (2022) Assessment of awareness and knowledge among medical students regarding radiation exposure from common diagnostic imaging procedures: radiation exposure awareness among medical students. AL-Kindy Coll Med J 18:118–122. https://doi.org/10.47723/kcmj.v18i2.792
Demirtaş M, Turan A, Akpunar S et al (2023) Knowledge level of medical students about ionising radiation used for diagnostic purpose in radiology: a survey study. Radiat Prot Dosimetry 199:1232–1238. https://doi.org/10.1093/rpd/ncad164
Ell T (2022) Improving the entry-to-practice education of radiographers. In: Almeida RPP (ed) Handbook of Research on Improving Allied Health Professions Education: Advancing Clinical Training and Interdisciplinary Translational Research. IGI Global, Hershey, PA, USA, pp 124–137. https://doi.org/10.4018/978-1-7998-9578-7.ch008
Cohen JA (2019) Knowledge of radiation legislation and guidelines amongst foundation doctors is inadequate for safe practice in the current era of radiology. Clin Radiol 74:418–420. https://doi.org/10.1016/j.crad.2019.01.020
O’Sullivan J, O’Connor OJ, O’Regan K et al (2010) An assessment of medical students’ awareness of radiation exposures associated with diagnostic imaging investigations. Insights Imaging 1:86–92. https://doi.org/10.1007/s13244-010-0009-8
Faggioni L, Paolicchi F, Bastiani L et al (2017) Awareness of radiation protection and dose levels of imaging procedures among medical students, radiography students, and radiology residents at an academic hospital: results of a comprehensive survey. Eur J Radiol 86:135–142. https://doi.org/10.1016/j.ejrad.2016.10.033
Maharjan S, Parajuli K, Sah S, Poudel U (2020) Knowledge of radiation protection among radiology professionals and students: a medical college-based study. Eur J Radiol Open 7:100287. https://doi.org/10.1016/j.ejro.2020.100287
Ottolenghi A, Trott KR, Smyth V (2019) Education and training to support radiation protection research in Europe: the DoReMi experience. Int J Radiat Biol 95:90–96. https://doi.org/10.1080/09553002.2018.1454616
Rainford L, Tcacenco A, Potocnik J et al (2023) Student perceptions of the use of three-dimensional (3-D) virtual reality (VR) simulation in the delivery of radiation protection training for radiography and medical students. Radiography (Lond) 29:777–785. https://doi.org/10.1016/j.radi.2023.05.009
Todua F, Nadareishvili D, Ormotsadze G, Sanikidze T (2016) Basic radiation protection education and training for medical professionals; Georgian experience and future perspective. Radiat Prot Dosimetry 169:422–424. https://doi.org/10.1093/rpd/ncv528
Belyi DA, Khomenko VI, Bebeshko VG (2009) Emergency preparedness of Research Center for Radiation Medicine and its hospital to admit and treat the patients with signs of acute radiation sickness. Radiat Prot Dosimetry 134:159–163. https://doi.org/10.1093/rpd/ncp077
Ploussi A, Efstathopoulos EP, Brountzos E (2021) The importance of radiation protection education and training for medical professionals of all specialties. Cardiovasc Intervent Radiol 44:829–834. https://doi.org/10.1007/s00270-020-02744-7
Fischetti C, Bhatter P, Frisch E et al (2022) The evolving importance of artificial intelligence and radiology in medical trainee education. Acad Radiol 29(Suppl 5):S70-s75. https://doi.org/10.1016/j.acra.2021.03.023
Zwaan L, Kok EM, van der Gijp A (2017) Radiology education: a radiology curriculum for all medical students? Diagnosis 4:185–189. https://doi.org/10.1515/dx-2017-0009
Wong K, Gallant F, Szumacher E (2021) Perceptions of Canadian radiation oncologists, radiation physicists, radiation therapists and radiation trainees about the impact of artificial intelligence in radiation oncology - national survey. J Med Imaging Radiat Sci 52:44–48. https://doi.org/10.1016/j.jmir.2020.11.013
Funding
None.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection, and analysis were performed by Pardis Bahadori, Ana P. Molina-Recalde, and Abdullah Alruwaili. The first draft of the manuscript was written by Ahmed Alanazy, Wondimagegn Tibebu Tilahun, and Gulsanga Ayub, and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Bahadori, P., Molina-Recalde, A.P., Saleh Alruwaili, A. et al. Assessment of medical students’ knowledge regarding radiation associated risk and its protection: finding from a cross-sectional study. Ir J Med Sci 193, 1515–1519 (2024). https://doi.org/10.1007/s11845-023-03583-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11845-023-03583-4