Abstract
Objectives
This systematic review and meta-analysis aimed to evaluate the efficacy of exercise training in patients with nonalcoholic fatty liver disease (NAFLD).
Methods
We searched PubMed, Cochrane Library, Web of Science, and Embase for relevant research from January 2001 to December 2021. The efficacy of exercise training was analyzed.
Results
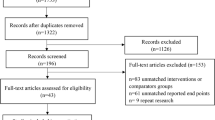
A total of 21 articles, involving 1733 patients, were included. Exercise training, including resistance training, aerobic exercise training, and high-intensity training, showed the efficacy in reducing weight (MD = 3.46, 95% CI [1.94, 4.98]), BMI (MD = 0.89, 95% CI [0.17, 1.61]), and ALT (MD = 6.66, 95% CI [3.27, 10.04]) and AST (MD = 3.14, 95% CI [0.35, 5.93]) levels in patients with NAFLD. When the exercise training lasted for ≥ 20 weeks, the total cholesterol (TC) (MD = 0.13, 95% CI [0.04, 0.22]), triglyceride (TG) (MD = 0.29, 95% CI [0.12, 0.47]), and blood glucose (GLU) (MD = − 0.18, 95% CI [0.10, 0.26]) levels significantly reduced. Compared with the exercise training group, the exercise training combined with probiotics group showed more efficiency in reducing the ALT, AST, TG, and TC levels. However, the exercise training combined with a hypoglycemic agent group showed no obvious efficiency compared with the exercise training group.
Conclusion
Exercise training can improve NAFLD. The improvement was more obvious when exercise was performed for ≥ 20 weeks. Probiotics may enhance the efficiency of exercise training.






Similar content being viewed by others
References
Kessoku T, Imajo K, Kobayashi T et al (2020) Lubiprostone in patients with non-alcoholic fatty liver disease: a randomised, double-blind, placebo-controlled, phase 2a trial. The lancet Gastroenterology & hepatology 5(11):996–1007. https://doi.org/10.1016/s2468-1253(20)30216-8
Cai J, Zhang XJ, Ji YX et al (2020) Nonalcoholic fatty liver disease pandemic fuels the upsurge in cardiovascular diseases. Circ Res 126(5):679–704. https://doi.org/10.1161/CIRCRESAHA.119.316337
Hariri M, Gholami A, Mirhafez SR et al (2020) A pilot study of the effect of curcumin on epigenetic changes and DNA damage among patients with non-alcoholic fatty liver disease: a randomized, double-blind, placebo-controlled, clinical trial. Complement Ther Med. https://doi.org/10.1016/j.ctim.2020.102447
Yao J, Meng M, Yang S et al (2018) Effect of aerobic and resistance exercise on liver enzyme and blood lipids in Chinese patients with nonalcoholic fatty liver disease: a randomized controlled trial. Int J Clin Exp Med 11(5):4867–4874
Wong VW, Wong GL, Chan RS et al (2018) Beneficial effects of lifestyle intervention in non-obese patients with non-alcoholic fatty liver disease. J Hepatol 69(6):1349–1356. https://doi.org/10.1016/j.jhep.2018.08.011
Takahashi A, Abe K, Fujita M et al (2020) Simple resistance exercise decreases cytokeratin 18 and fibroblast growth factor 21 levels in patients with nonalcoholic fatty liver disease: a retrospective clinical study. Medicine (Baltimore) 99(22):e20399. https://doi.org/10.1097/md.0000000000020399
Sáez-Lara MJ, Robles-Sanchez C, Ruiz-Ojeda FJ et al (2016) Effects of probiotics and synbiotics on obesity, insulin resistance syndrome, type 2 diabetes and non-alcoholic fatty liver disease: a review of human clinical trials. Int J Mol Sci 17(6). https://doi.org/10.3390/ijms17060928
Lavine JE, Schwimmer JB, Van Natta ML et al (2011) Effect of vitamin E or metformin for treatment of nonalcoholic fatty liver disease in children and adolescents: the TONIC randomized controlled trial. JAMA 305(16):1659–1668. https://doi.org/10.1001/jama.2011.520
Moher D, Shamseer L, Clarke M et al (2015) Preferred reporting items for systematic review and meta-analysis protocols (PRISMA-P) 2015 statement. Syst Rev. https://doi.org/10.1186/2046-4053-4-1
Cai GS, Su H, Zhang J (2020) Protective effect of probiotics in patients with non-alcoholic fatty liver disease. Medicine (Baltimore) 99(32):e21464. https://doi.org/10.1097/md.0000000000021464
Khoo J, Hsiang JC, Taneja R et al (2019) Randomized trial comparing effects of weight loss by liraglutide with lifestyle modification in non-alcoholic fatty liver disease. Liver Int 39(5):941–949. https://doi.org/10.1111/liv.14065
Duseja A, Acharya SK, Mehta M et al (2019) High potency multistrain probiotic improves liver histology in non-alcoholic fatty liver disease (NAFLD): a randomised, double-blind, proof of concept study. BMJ open gastroenterology 6(1). https://doi.org/10.1136/bmjgast-2019-000315
Banitalebi E, Faramarzi M, Nasiri S et al (2019) Effects of different exercise modalities on novel hepatic steatosis indices in overweight women with type 2 diabetes. Clin Mol Hepatol 25(3):294–304. https://doi.org/10.3350/cmh.2018.0086
Abdelbasset WK, Tantawy SA, Kamel DM et al (2019) A randomized controlled trial on the effectiveness of 8-week high-intensity interval exercise on intrahepatic triglycerides, visceral lipids, and health-related quality of life in diabetic obese patients with nonalcoholic fatty liver disease. Medicine (Baltimore) 98(12):e14918. https://doi.org/10.1097/md.0000000000014918
Bakhshimoghaddam F, Shateri K, Sina M et al (2018) Daily consumption of synbiotic yogurt decreases liver steatosis in patients with nonalcoholic fatty liver disease: a randomized controlled clinical trial. J Nutr 148(8):1276–1284. https://doi.org/10.1093/jn/nxy088
Zhang HJ, Pan LL, Ma ZM et al (2017) Long-term effect of exercise on improving fatty liver and cardiovascular risk factors in obese adults: a 1-year follow-up study. Diabetes Obes Metab 19(2):284–289. https://doi.org/10.1111/dom.12809
Takahashi A, Imaizumi H, Hayashi M et al (2017) Simple resistance exercise for 24 weeks decreases alanine aminotransferase levels in patients with non-alcoholic fatty liver disease. Sports medicine international open 1(1):E2-e7. https://doi.org/10.1055/s-0042-117875
Rezende RE, Duarte SM, Stefano JT et al (2016) Randomized clinical trial: benefits of aerobic physical activity for 24 weeks in postmenopausal women with nonalcoholic fatty liver disease. Menopause (New York, NY) 23(8):876–883. https://doi.org/10.1097/gme.0000000000000647
Takahashi A, Abe K, Usami K et al (2015) Simple Resistance Exercise helps Patients with Non-alcoholic Fatty Liver Disease. International journal of sports medicine 36(10): 848-852. https://doi.org/10.1055/s-0035-1549853
Shamsoddini A, Sobhani V, Ghamar Chehreh ME et al (2015) Effect of aerobic and resistance exercise training on liver enzymes and hepatic fat in iranian men with nonalcoholic fatty liver disease. Hepat Mon 15(10):e31434. https://doi.org/10.5812/hepatmon.31434
Hallsworth K, Thoma C, Hollingsworth KG et al (2015) Modified high-intensity interval training reduces liver fat and improves cardiac function in non-alcoholic fatty liver disease: a randomized controlled trial. Clinical science (London, England : 1979) 129(12): 1097–1105. https://doi.org/10.1042/cs20150308
Pugh CJ, Spring VS, Kemp GJ et al (2014) Exercise training reverses endothelial dysfunction in nonalcoholic fatty liver disease. Am J Physiol Heart Circ Physiol 307(9):H1298-1306. https://doi.org/10.1152/ajpheart.00306.2014
Pugh CJ, Cuthbertson DJ, Sprung VS et al (2013) Exercise training improves cutaneous microvascular function in nonalcoholic fatty liver disease. Am J Physiol Endocrinol Metab 305(1):E50-58. https://doi.org/10.1152/ajpendo.00055.2013
Al-Jiffri O, Al-Sharif FM, Abd El-Kader SM et al (2013) Weight reduction improves markers of hepatic function and insulin resistance in type-2 diabetic patients with non-alcoholic fatty liver. Afr Health Sci 13(3):667–672. https://doi.org/10.4314/ahs.v13i3.21
Sullivan S, Kirk EP, Mittendorfer B et al (2012) Randomized trial of exercise effect on intrahepatic triglyceride content and lipid kinetics in nonalcoholic fatty liver disease. Hepatology 55(6):1738–1745. https://doi.org/10.1002/hep.25548
Bozzetto L, Prinster A, Annuzzi G et al (2012) Liver fat is reduced by an isoenergetic MUFA diet in a controlled randomized study in type 2 diabetic patients. Diabetes Care 35(7):1429–1435. https://doi.org/10.2337/dc12-0033
Chen S-M, Liu C-Y, Li S-R et al (2008) Effects of therapeutic lifestyle program on ultrasound-diagnosed nonalcoholic fatty liver disease. J Chin Med Assoc 71(11):551–558. https://doi.org/10.1016/s1726-4901(08)70168-0
Jia GY, Han T, Gao L et al (2018) Effect of aerobic exercise and resistance exercise in improving non-alcoholic fatty liver disease: a randomized controlled trial. Zhonghua gan zang bing za zhi [Chinese journal of hepatology] 26(1):34–41. https://doi.org/10.3760/cma.j.issn.1007-3418.2018.01.009
Whitsett M, VanWagner LB (2015) Physical activity as a treatment of non-alcoholic fatty liver disease: a systematic review. World J Hepatol 7(16):2041–2052. https://doi.org/10.4254/wjh.v7.i16.2041
Lule KO, Akarsu E, Sayiner ZA et al (2022) The effects of metformin, pioglitazone, exenatide and exercise on fatty liver in obese diabetic rats: the role of IRS-1 and SOCS-3 molecules. Inflammopharmacology. https://doi.org/10.1007/s10787-021-00916-6
Yu Y, Yu L, Cheng N et al (2021) Exercise alleviates the apolipoprotein A5-toll-like receptor 4 axis impairment in mice with high-fat diet-induced non-alcoholic steatohepatitis. Front Physiol. https://doi.org/10.3389/fphys.2021.783341
Charatcharoenwitthaya P, Kuljiratitikal K, Aksornchanya O et al (2021) Moderate-intensity aerobic vs resistance exercise and dietary modification in patients with nonalcoholic fatty liver disease: a randomized clinical trial. Clinical and translational gastroenterology 12(3): e00316. https://doi.org/10.14309/ctg.0000000000000316
Iwanaga S, Hashida R, Takano Y et al (2020) Hybrid training system improves insulin resistance in patients with nonalcoholic fatty liver disease: a randomized controlled pilot study. Tohoku J Exp Med 252(1):23–32. https://doi.org/10.1620/tjem.252.23
Gomes Anunciação P, Doederlein Polito M (2011) A review on post-exercise hypotension in hypertensive individuals. Arq Bras Cardiol 96(5):e100-109
Boutcher YN, Boutcher SH (2017) Exercise intensity and hypertension: what’s new? J Hum Hypertens 31(3):157–164. https://doi.org/10.1038/jhh.2016.62
Kelley GA, Kelley KS (2008) Efficacy of aerobic exercise on coronary heart disease risk factors. Prev Cardiol 11(2):71–75. https://doi.org/10.1111/j.1751-7141.2008.08037.x
Boutcher SH (2011) High-intensity intermittent exercise and fat loss. Journal of obesity. https://doi.org/10.1155/2011/868305
Trapp EG, Chisholm DJ, Freund J et al (2005) (2008) The effects of high-intensity intermittent exercise training on fat loss and fasting insulin levels of young women. Int J Obes 32(4):684–691. https://doi.org/10.1038/sj.ijo.0803781
Hashida R, Kawaguchi T, Bekki M et al (2017) Aerobic vs. resistance exercise in non-alcoholic fatty liver disease: a systematic review. J Hepatol 66(1): 142–152. https://doi.org/10.1016/j.jhep.2016.08.023
Wang Y, Li N, Yang JJ et al (2020) Probiotics and fructo-oligosaccharide intervention modulate the microbiota-gut brain axis to improve autism spectrum reducing also the hyper-serotonergic state and the dopamine metabolism disorder. Pharmacol Res. https://doi.org/10.1016/j.phrs.2020.104784
Liu M, Ding J, Zhang H et al (2020) Lactobacillus casei LH23 modulates the immune response and ameliorates DSS-induced colitis via suppressing JNK/p-38 signal pathways and enhancing histone H3K9 acetylation. Food Funct. https://doi.org/10.1039/d0fo00546k
Jang HR, Park HJ, Kang D et al (2019) A protective mechanism of probiotic Lactobacillus against hepatic steatosis via reducing host intestinal fatty acid absorption. Exp Mol Med 51(8):1–14. https://doi.org/10.1038/s12276-019-0293-4
Scorletti E, Afolabi PR, Miles EA et al (2020) Synbiotics alter fecal microbiomes, but not liver fat or fibrosis, in a randomized trial of patients with nonalcoholic fatty liver disease. Gastroenterology 158(6):1597-1610.e1597. https://doi.org/10.1053/j.gastro.2020.01.031
Loomba R, Ling L, Dinh DM et al (2021) The commensal microbe veillonella as a marker for response to an FGF19 analog in NASH. Hepatology 73(1):126–143. https://doi.org/10.1002/hep.31523
Eguchi Y, Kitajima Y, Hyogo H et al (2015) Pilot study of liraglutide effects in non-alcoholic steatohepatitis and non-alcoholic fatty liver disease with glucose intolerance in Japanese patients (LEAN-J). Hepatol Res 45(3):269–278. https://doi.org/10.1111/hepr.12351
Armstrong MJ, Hull D, Guo K et al (2016) Glucagon-like peptide 1 decreases lipotoxicity in non-alcoholic steatohepatitis. J Hepatol 64(2):399–408. https://doi.org/10.1016/j.jhep.2015.08.038
Bhat A, Sebastiani G, Bhat M (2015) Systematic review: preventive and therapeutic applications of metformin in liver disease. World J Hepatol 7(12):1652–1659. https://doi.org/10.4254/wjh.v7.i12.1652
Funding
This article was supported by Qingdao Science and Technology Benefit People Demonstration and Guidance Project (21–43-02–0016). Qingdao Science and Technology Benefit People Demonstration and Guidance Project,21–43-02–0016.
Author information
Authors and Affiliations
Contributions
X.Y and Y.W conduct preliminary search, extract information, calculate information, and write the paper. J.L revises the paper. W.H designs the experiment. J.D approves the final version.
Corresponding author
Ethics declarations
Ethics approval
Not applicable.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Yu, X., Wang, Y., Lai, J. et al. Comparative efficacy of exercise training processes in improving nonalcoholic fatty liver disease: a systematic review and meta-analysis. Ir J Med Sci 192, 131–142 (2023). https://doi.org/10.1007/s11845-022-02988-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11845-022-02988-x