Abstract
Background
There has been a significant increase in the volume of urological patients on daily anticoagulation therapy requiring invasive elective urological procedures.
Aims
We sought to assess whether urologists are familiar with appropriate perioperative management strategies in this patient cohort.
Methods
Urologists completed a questionnaire on their current management strategy for warfarin during the perioperative period in patients undergoing elective urological surgery. Eleven urological procedures graded as minor, endoscopic and major were assessed in the study. In addition, respondents were also asked whether they administered bridging therapy with heparin when warfarin was discontinued perioperatively.
Results
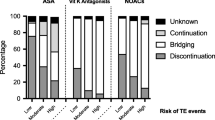
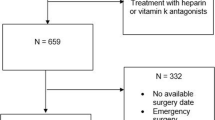
The response rate was 52.5% (210/400). Procedure grade did not influence the duration warfarin was discontinued preoperatively with respondents discontinuing the agent 4.71 ± 1.52 days (range 2–10 days) prior to minor procedures, 4.74 ± 1.43 days (range 2–10 days) prior to endoscopic procedures and 4.88 ± 1.34 days (range 2–10 days) prior to major procedures (p > 0.05). Postoperatively, procedure grade significantly affected the day to recommencement with respondents recommencing warfarin 2.41 ± 2.31 days (range 1–14 days) after minor procedures, 3.07 ± 3.52 days (range 1–28 days) after endoscopic procedures and 4.38 ± 3.53 days (range 1–14 days) after major procedures (p < 0.0001). In total, 60 ± 0.52% of the respondents who discontinued warfarin routinely administered bridging therapy with heparin perioperatively.
Conclusions
Our study demonstrates variations in perioperative management practices for patients on chronic anticoagulation therapy undergoing urological procedures. Urologists should familiarise themselves with standardised guidelines if this patient subgroup are to receive optimal perioperative management.
Similar content being viewed by others
References
Hirsh J, Fuster V, Ansell J et al (2003) American Heart Association/American College of Cardiology Foundation guide to warfarin therapy. Circulation 107:1692–1711
Kefer JC, Desai MM, Fergany A et al (2008) Outcomes of partial nephrectomy in patients on chronic oral anticoagulant therapy. J Urol 180:2370–2374 Discussion 2734
Kearon C, Hirsh J (1997) Management of anticoagulation before and after elective surgery. N Engl J Med 336:1506–1511
Larson BJ, Zumberg MS, Kitchens CS (2005) A feasibility study of continuing dose-reduced warfarin for invasive procedures in patients with high thromboembolic risk. Chest 127:922–927
Fang MC, Singer DE (2004) Anticoagulation for atrial fibrillation. Cardiol Clin 22:47–62
Douketis JD, Berger PB, Dunn AS et al (2008) The perioperative management of antithrombotic therapy: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines (8th edition). Chest 133:299S–339S
Halachmi S, Katz Y, Meretyk S et al (2008) Perioperative morbidity and mortality in 80 years and older undergoing elective urology surgery––a prospective study. Aging Male 11:162–166
Daniels PR (2005) Therapy insight: management of urology patients taking long-term warfarin anticoagulation therapy. Nat Clin Pract Urol 2:343–350
Palareti G, Legnani C (1996) Warfarin withdrawal Pharmacokinetic–pharmacodynamic considerations. Clin Pharmacokinet 30:300–313
White RH, McKittrick T, Hutchinson R et al (1995) Temporary discontinuation of warfarin therapy: changes in the international normalized ratio. Ann Intern Med 122:40–42
Spyropoulos AC, Turpie AG, Dunn AS et al (2006) Clinical outcomes with unfractionated heparin or low-molecular-weight heparin as bridging therapy in patients on long-term oral anticoagulants: the REGIMEN registry. J Thromb Haemost 4:1246–1252
Spyropoulos AC, Frost FJ, Hurley JS et al (2004) Costs and clinical outcomes associated with low-molecular-weight heparin vs unfractionated heparin for perioperative bridging in patients receiving long-term oral anticoagulant therapy. Chest 125:1642–1650
Hirsh J, Raschke R (2004) Heparin and low-molecular-weight heparin: the seventh ACCP conference on antithrombotic and thrombolytic Therapy. Chest 126:188S–203S
Kovacs MJ, Kearon C, Rodger M et al (2004) Single-arm study of bridging therapy with low-molecular-weight heparin for patients at risk of arterial embolism who require temporary interruption of warfarin. Circulation 110:1658–1663
Douketis JD, Johnson JA, Turpie AG (2004) Low-molecular-weight heparin as bridging anticoagulation during interruption of warfarin: assessment of a standardized periprocedural anticoagulation regimen. Arch Intern Med 164:1319–1326
Dotan ZA, Mor Y, Leibovitch I et al (2002) The efficacy and safety of perioperative low molecular weight heparin substitution in patients on chronic oral anticoagulant therapy undergoing transurethral prostatectomy for bladder outlet obstruction. J Urol 168:610–613 discussion 614
Dunn AS, Spyropoulos AC, Turpie AG (2007) Bridging therapy in patients on long-term oral anticoagulants who require surgery: the Prospective Peri-operative Enoxaparin Cohort Trial (PROSPECT). J Thromb Haemost 5:2211–2218
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Davis, N.F., Fanning, D.M., McGuire, B.B. et al. Perioperative management of chronic anticoagulation therapy in urological patients: a cross-sectional survey of practice. Ir J Med Sci 180, 823–828 (2011). https://doi.org/10.1007/s11845-011-0738-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11845-011-0738-9