Abstract
Purpose
Our study aimed to examine whether receipt of follow-up care plans is associated with greater guideline-concordant CRC screening stratified by breast, prostate, and lung cancer survivors.
Methods
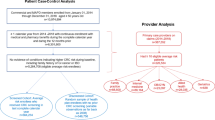
We used data from years 2016, 2018, and 2020 of the Behavioral Risk Factor Surveillance System on 3339 eligible treatment-utilizing cancer survivors with complete treatment. We performed descriptive statistics and multivariable logistic regression to examine the mentioned association.
Results
We observed that 83.9% of breast and 88.2% of prostate cancer survivors with follow-care plans received CRC screening (p-value < 0.001). The lowest CRC screening use was observed among lung cancer (70.8%). In multivariable analysis, receipt of follow-up care plans was strongly associated with greater odds of receiving CRC screening in breast (OR, 2.67; 95% CI: 1.71–4.16) and prostate (OR, 3.81; 95% CI: 2.30–6.31) cancer survivors. Regardless of provider type, 84 to 88% reduced likelihood of receipt of CRC screening when they received follow-up care plans among lung cancer survivors. Among those without follow-up care plans, breast (OR, 0.29; 95% CI: 0.09–0.92) and lung (OR, 0.05; 95% CI: 0.01–0.25) cancer survivors who received care from general practices were less likely to receive CRC screening compared to those who received care from non-general practices.
Conclusions
Receipt of follow-up care plans was associated with greater CRC screening use in breast and prostate cancers. Lung cancer survivors demonstrated lower screening use despite receipt of follow-up care plans.
Implication for Cancer Survivors
Patient and provider communication regarding CRC screening recommendation should be included in their follow-up care plans.

Similar content being viewed by others
Data availability
The datasets generated during the current study are available in the Center for Disease Control, and Prevention repository, https://www.cdc.gov/brfss/.
References
Centers for Disease Control and Prevention (CDC). An Update on Cancer Deaths in the United States. Atlanta, GA: US Department of Health and Human Services, Centers for Disease Control and Prevention, Division of Cancer Prevention and Control; 2022.
American Cancer Society (ACS). Cancer Facts & Figures 2022. Atlanta: American Cancer Society; 2022.
Siegel RL, Miller KD, Fuchs HE, Jemal A. Cancer statistics, 2022. CA Cancer J Clin. 2022;72(1):7–33.
Brenner H, Chen C. The colorectal cancer epidemic: challenges and opportunities for primary, secondary and tertiary prevention. Br J Cancer. 2018;119(7):785–92.
American Cancer Society (ACS). Cancer Treatment & Survivorship Facts & Figures 2022–2024. Atlanta: American Cancer Society;2022.
Secondary Primary Cancers. Available from: https://dceg.cancer.gov/research/what-we-study/second-cancers. Accessed May 31, 2022.
Desautels D, Czaykowski P, Nugent Z, Demers AA, Mahmud SM, Singh H. Risk of colorectal cancer after the diagnosis of prostate cancer: A population-based study. Cancer. 2016;122(8):1254–60.
Baxter NN, Tepper JE, Durham SB, Rothenberger DA, Virnig BA. Increased risk of rectal cancer after prostate radiation: a population-based study. Gastroenterology. 2005;128(4):819–24.
Davis EJ, Beebe-Dimmer JL, Yee CL, Cooney KA. Risk of second primary tumors in men diagnosed with prostate cancer: a population-based cohort study. Cancer. 2014;120(17):2735–41.
Donin N, Filson C, Drakaki A, et al. Risk of Second Primary Malignancies Among Cancer Survivors in the United States, 1992 Through 2008. Cancer. 2016;122(19):3075–86.
Travis LB. Therapy-associated solid tumors. Acta Oncol. 2002;41(4):323–33.
Travis LB, Rabkin CS, Brown LM, et al. Cancer survivorship - Genetic susceptibility and second primary cancers: Research strategies and recommendations. Jnci-J the National Cancer Institute. 2006;98(1):15–25.
Schoen RE, Weissfeld JL, Kuller LH. Are Women with Breast, Endometrial, or Ovarian-Cancer at Increased Risk for Colorectal-Cancer. Am J Gastroenterol. 1994;89(6):835–42.
Kato T, Suzuki K, Muto Y, et al. Multiple primary malignancies involving primary sporadic colorectal cancer in Japan: incidence of gastric cancer with colorectal cancer patients may be higher than previously recognized. World Journal of Surgical Oncology. Feb 7 2015;13.
Dash C, Lu JC, Parikh V, et al. Disparities in colorectal cancer screening among breast and prostate cancer survivors. Cancer Med. 2021;10(4):1448–56.
Hewitt ME GP, American Society of Clinical Oncology, Institute of Medicine (U.S.), EBSCO Publishing (Firm), National Academies Press (U.S.),, al. e. From cancer patient to cancer survivor: lost in transition. Washington, D.C: National Academies Press; 2006.
American Society of Clinical Oncology (ASCO). ASCO Cancer Treatment and Survivorship Care Plans. https://www.cancer.net/survivorship/follow-care-after-cancer-treatment/asco-cancer-treatment-and-survivorship-care-plans. Accessed June 24, 2022.
Shay LA, Schmidt S, Dioun SI, Grimes A, Embry L. Receipt of a survivorship care plan and self-reported health behaviors among cancer survivors. J Cancer Surviv. 2019;13(2):180–6.
Centers for Disease Control and Prevention (CDC). Use of Colorectal Cancer Screening Tests. 2021; https://www.cdc.gov/cancer/colorectal/statistics/use-screening-tests-BRFSS.htm. Accessed July 13, 2022, 2022.
Laiyemo AO, Adebogun AO, Doubeni CA, et al. Influence of provider discussion and specific recommendation on colorectal cancer screening uptake among US. adults. Prev Med. 2014;67:1–5.
White PM, Itzkowitz SH. Barriers Driving Racial Disparities in Colorectal Cancer Screening in African Americans. Curr Gastroenterol Rep. 2020;22(8):41.
Harper DM, Tariq M, Alhawli A, Syed N, Patel M, Resnicow K. Cancer risk perception and physician communication behaviors on cervical cancer and colorectal cancer screening. Elife. 2021;10.
Adegboyega A, Aleshire M, Wiggins AT, Palmer K, Hatcher J. A Motivational Interviewing Intervention to Promote CRC Screening: A Pilot Study. Cancer Nurs. 2022;45(1):E229-e237.
Carcaise-Edinboro P, Bradley CJ. Influence of patient-provider communication on colorectal cancer screening. Med Care. 2008;46(7):738–45.
Katz ML, Young GS, Zimmermann BJ, Tatum CM, Paskett ED. Assessing Colorectal Cancer Screening Barriers by Two Methods. J Cancer Educ. 2018;33(3):536–43.
Ford ME, Sterba KR, Armeson K, Malek AM, Knight KD, Zapka J. Factors Influencing Adherence to Recommended Colorectal Cancer Surveillance: Experiences and Behaviors of Colorectal Cancer Survivors. J Cancer Educ. 2019;34(5):938–49.
Young JM, Durcinoska I, DeLoyde K, Solomon MJ. Patterns of follow up and survivorship care for people with colorectal cancer in new South Wales, Australia: a population-based survey. BMC Cancer. 2018;18(1):339.
Centers for Disease Control and Prevention (CDC). Behavioral Risk Factor Surveillance System Survey Data. Atlanta, Georgia: U.S. Department of Health and Human Services, Centers for Disease Control and Prevention, 2020.
Wolf AMD, Fontham ETH, Church TR, et al. Colorectal cancer screening for average-risk adults: 2018 guideline update from the American Cancer Society. CA Cancer J Clin. 2018;68(4):250–81.
US Preventive Services Task Force. Screening for colorectal cancer: US preventive services task force recommendation statement. JAMA. 2021;325(19):1965–77.
Brennan ME, Gormally JF, Butow P, Boyle FM, Spillane AJ. Survivorship care plans in cancer: a systematic review of care plan outcomes. Br J Cancer. 2014;111(10):1899–908.
Jacobsen PB, DeRosa AP, Henderson TO, et al. Systematic Review of the Impact of Cancer Survivorship Care Plans on Health Outcomes and Health Care Delivery. J Clin Oncol. 2018;36(20):2088–100.
Kenzik KM, Kvale EA, Rocque GB, et al. Treatment Summaries and Follow-Up Care Instructions for Cancer Survivors: Improving Survivor Self-Efficacy and Health Care Utilization. Oncologist. 2016;21(7):817–24.
Wallner L, Slezak JM, Quinn VP, et al. Quality of Preventive Care Before and After Prostate Cancer Diagnosis. J of Mens Health. 2015;11(5):14–21.
Islam KMM, Jiang XQ, Anggondowati T, Lin G, Ganti AK. Comorbidity and Survival in Lung Cancer Patients. Cancer Epidem Biomar. 2015;24(7):1079–85.
Blanch-Hartigan D, Chawla N, Beckjord EI, et al. Cancer survivors’ receipt of treatment summaries and implications for patient-centered communication and quality of care. Patient Educ Couns. 2015;98(10):1274–9.
Rajapakse P. An Update on Survivorship Issues in Lung Cancer Patients. World J Oncol. 2021;12(2–3):45–9.
Salz T, Oeffinger KC, McCabe MS, Layne TM, Bach PB. Survivorship care plans in research and practice. CA Cancer J Clin. 2012;62(2):101–17.
Skolarus TA, Wolf AMD, Erb NL, et al. American Cancer Society Prostate Cancer Survivorship Care Guidelines. Ca-a Cancer J Clinicians. 2014;64(4):226–49.
Resnick MJ, Lacchetti C, Penson DF. Prostate Cancer Survivorship Care Guidelines: American Society of Clinical Oncology Practice Guideline Endorsement. J Oncol Practice. 2015;11(3):E445–9.
Pozo CLP, Morgan MAA, Gray JE. Survivorship Issues for Patients With Lung Cancer. Cancer Control. 2014;21(1):40–50.
Attai DJ, Katz MS, Streja E, et al. Patient preferences and comfort for cancer survivorship models of care: results of an online survey. J Cancer Surviv. Feb 3 2022.
Tucholka JL, Jacobson N, Steffens NM, et al. Breast cancer survivor’s perspectives on the role different providers play in follow-up care. Support Care Cancer. 2018;26(6):2015–22.
Yang P, Cheville AL, Wampfler JA, et al. Quality of Life and Symptom Burden among Long-Term Lung Cancer Survivors. J Thorac Oncol. 2012;7(1):64–70.
Huang ZP, Cheng HL, Loh SY, Cheng KKF. Functional Status, Supportive Care Needs, and Health-Related Quality of Life in Advanced Lung Cancer Patients Aged 50 and Older. Asia Pac J Oncol Nurs. 2020;7(2):151–60.
Chan RJ, Crawford-Williams F, Crichton M, et al. Effectiveness and implementation of models of cancer survivorship care: an overview of systematic reviews. J Cancer Surviv. Nov 16 2021.
Parry C, Kent EE, Forsythe LP, Alfano CM, Rowland JH. Can’t see the forest for the care plan: a call to revisit the context of care planning. J Clin Oncol. 2013;31(21):2651–3.
Acknowledgements
Thanks to co-authors for their expertise and assistance throughout all aspects of this study and for their help in completing the manuscript.
Funding
This research was supported at least in part through the Georgia Cancer Center Paceline funding mechanism (principal investigator: Meng-Han Tsai). Malcolm S. Bevel was also supported partially by the Georgia Cancer Center Paceline funding mechanism. In addition, Justin X. Moore was supported by the National Institute on Minority Health and Health Disparities of the National Institutes of Health under Award Number K01MD015304. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception. Material preparation and data analysis were performed by Meng-Han Tsai and Malcolm S. Bevel. The first draft of the manuscript was written by Meng-Han Tsai and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethical approval
The respective health departments from each state grant Institutional Review Board (IRB) approval for the distribution and collection of data using the BRFSS. Data extracted for this study were publicly available and de-identified, and thus considered exempt from IRB review at Augusta University. This article does not include any studies with animals performed by any of the authors.
Consent to participate
Verbal informed consent was obtained from all individual participants included in the study as per the BRFSS process for data collection.
Consent for publication
This study does not include any individual person’s data in any form (including any individual details, images, or videos).
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Tsai, MH., Bevel, M.S., Andrzejak, S.E. et al. Receipt of follow-up care plans on colorectal cancer screening among breast, prostate, and lung cancer survivors. J Cancer Surviv 18, 781–790 (2024). https://doi.org/10.1007/s11764-022-01309-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11764-022-01309-6