Abstract
Purpose
This study explored the pattern of complementary or alternative medicine (CAM) use among Chinese survivors of childhood cancer and identified potential drug-CAM interactions and factors predicting CAM use.
Methods
This cross-sectional study recruited 393 survivors of childhood cancer (male, 57.8%; mean age, 17.7 [SD = 7.3] years; mean years post-treatment, 8.8 [SD = 5.0]) from a public hospital in Hong Kong. Participants reported CAM and over-the-counter medications that they used in the past year. Prescription drug data were extracted from pharmacy dispensing records. Potential interactions between concurrent CAM and chronic medications were identified from well-established CAM-drug/herb-drug interaction databases. A multivariate logistic regression was performed to analyze associations of socio-demographic and clinical factors with CAM use.
Results
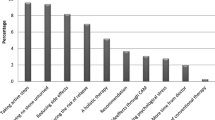
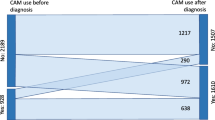
Half (n = 205/393, 52.2%) of the participants reported the use of CAM. The most popular CAMs were traditional Chinese medicine (n = 127/205, 62.0%) and natural products (n = 114/205, 55.3%). Among the 69 survivors (33.7%) concurrently using CAM and chronic medications, one-third (n = 21/69, 30.4%) were at risk of drug-CAM interactions that are of moderate significance. Adult survivors were more likely to use CAM than pediatric survivors (odds ratio [OR], 2.35; 95% confidence interval [CI], 1.31–4.41). Brain tumor survivors were more likely than other solid tumor survivors to use non-oral therapies (OR, 2.70; 95% CI, 1.01–7.72).
Conclusions
The prevalence of CAM use among Chinese survivors of childhood cancer was high. A minority of survivors had a risk of clinically significant CAM-drug interactions. Future studies should focus on survivors’ behavior and motivations for CAM use.
Implications for Cancer Survivors
As the concurrent use of CAM and chronic medications might result in interactions, healthcare providers should proactively identify such interactions and develop referral pathways to promote evidence-based integrative therapies for survivors.


Similar content being viewed by others
Availability of data and materials
Not applicable
Code availability
Not applicable
References
Miller KD, Nogueira L, Mariotto AB, Rowland JH, Yabroff KR, Alfano CM, et al. Cancer treatment and survivorship statistics, 2019. CA Cancer J Clin. 2019;69(5):363–85.
Allemani C, Matsuda T, Di Carlo V, Harewood R, Matz M, Nikšić M, et al. Global surveillance of trends in cancer survival 2000–14 (CONCORD-3): analysis of individual records for 37 513 025 patients diagnosed with one of 18 cancers from 322 population-based registries in 71 countries. Lancet. 2018;391(10125):1023–75.
Oeffinger KC, Mertens AC, Sklar CA, Kawashima T, Hudson MM, Meadows AT, et al. Chronic health conditions in adult survivors of childhood cancer. N Engl J Med. 2006;355(15):1572–82.
Complementary, alternative, or integrative health: what’s in a name? NCCIH. 2011. https://nccih.nih.gov/health/integrative-health. Accessed on 8 Dec 2020.
Kelly KM. Integrative therapies for children with hematological malignancies. Hematology Am Soc Hematol Educ Program. 2009;2009(1):307–12.
Miller PE, Vasey JJ, Short PF, Hartman TJ. Dietary supplement use in adult cancer survivors. Oncol Nurs Forum. 2009;36(1):61–8.
Song S, Youn J, Lee YJ, Kang M, Hyun T, Song Y, et al. Dietary supplement use among cancer survivors and the general population: a nation-wide cross-sectional study. BMC Cancer. 2017;17(1):891.
John GM, Hershman DL, Falci L, Shi Z, Tsai W, Greenlee H. Complementary and alternative medicine use among US cancer survivors. J Cancer Surviv. 2016;10(5):850–64.
Rock CL, Newman VA, Neuhouser ML, Major J, Barnett MJ. Antioxidant supplement use in cancer survivors and the general population. J Nutr. 2004;134(11):3194S–5S.
Diorio C, Lam CG, Ladas EJ, Njuguna F, Afungchwi GM, Taromina K, et al. Global use of traditional and complementary medicine in childhood cancer: a systematic review. J Glob Oncol. 2017;3(6):791–800.
Shneerson C, Taskila T, Gale N, Greenfield S, Chen Y. The effect of complementary and alternative medicine on the quality of life of cancer survivors: a systematic review and meta-analyses. Complement Ther Med. 2013;21(4):417–29.
Mertens AC, Sencer S, Myers CD, Recklitis C, Kadan-Lottick N, Whitton J, et al. Complementary and alternative therapy use in adult survivors of childhood cancer: a report from the Childhood Cancer Survivor Study. Pediatr Blood Cancer. 2008;50(1):90–7.
Ndao DH, Ladas EJ, Bao Y, Cheng B, Nees SN, Levine JM, et al. Use of complementary and alternative medicine among children, adolescent, and young adult cancer survivors: a survey study. J Pediatr Hematol Oncol. 2013;35(4):281–8.
Poon LHJ, Yu C, Peng L, Ewig CL, Zhang H, Li C, et al. Clinical ascertainment of health outcomes in Asian survivors of childhood cancer: a systematic review. J Cancer Surviv. 2019;13(3):374–96.
McCune JS, Hatfield AJ, Blackburn AAR, Leith PO, Livingston RB, Ellis GK. Potential of chemotherapy-herb interactions in adult cancer patients. Support Care Cancer. 2004;12(6):454–62.
Smitherman AB, Mohabir D, Wilkins TM, Blatt J, Nichols HB, Dusetzina SB. Early post-therapy prescription drug usage among childhood and adolescent cancer survivors. J Pediatr. 2018;195:161–8.
Chan EW, Lau WC, Leung WK, Mok MT, He Y, Tong TS, et al. Prevention of dabigatran-related gastrointestinal bleeding with gastroprotective agents: a population-based study. Gastroenterology. 2015;149(3):586–95.
Wong MC, Jiang JY, Tang J, Lam A, Fung H, Mercer SW. Health services research in the public healthcare system in Hong Kong: an analysis of over 1 million antihypertensive prescriptions between 2004–2007 as an example of the potential and pitfalls of using routinely collected electronic patient data. BMC Health Serv Res. 2008;8(1):138.
World Health Organization. ATC/DDD classification (final).(ATC/DDD classification)(anatomical therapeutic chemical (ATC) classifications and defined daily doses). WHO Drug Information. 2011;25(1):43.
Lexi-drugs online. Hudson (OH): Lexicomp, Inc.; 2020. http://online.lexi.com. Last accessed on 10 Dec 2020. Subscription required to view.
Natural Medicines. Somerville (MA): Therapeutic Research Center; 2020. https://naturalmedicines.therapeuticresearch.com. Last accessed on 10 Dec 2020. Subscription required to view.
About Herbs, Botanicals & Other Products. Memorial Sloan-Kettering Cancer Center; 2020. https://www.mskcc.org/cancer-care/treatments/symptom-management/integrative-medicine/herbs. Last accessed on 10 Dec 2020.
Baxter K, Preston CL, editors. Stockley's drug interactions. London: Pharmaceutical Press; 2020. https://www.medicinescomplete.com/mc/stockley/current/. Last accessed on 10 Dec 2020.
Williamson E, Driver S, Baxter K, Claire LP, editors. Stockley's herbal medicines interactions. London: Pharmaceutical Press; 2020. https://www.medicinescomplete.com/mc/stockley/current/. Last accessed on 10 Dec 2020.
The drug–herb interaction information. Taiwan: Taiwan’s Ministry of Health and Welfare; 2011. Available from https://dhi.cmu.edu.tw/query/. Last accessed on 10 Dec 2020.
Cassileth BR, Lucarelli CD. Herb-drug interactions in oncology. PMPH-USA; 2003.
A to Z List of Cancer Types. National Cancer Institute. https://www.cancer.gov/types. Accessed on 8 Dec 2020.
Patients' socioeconomic status and their evaluations of primary care in Hong Kong. BMC Health Serv Res. 2013;13(1):487.
Wong CSM, Chan WC, Lam LCW, Law WY, Tang WY, Wong TY, et al. Living environment and psychological distress in the general population of Hong Kong. Procedia Environ Sci. 2016;36:78–81.
Census and statistics department Hong Kong special administrative region. Thematic household survey report—report No. 26. Census and Statistics Department, Hong Kong Special Administrative Region. 2005.
Bours MJ, Beijer S, Winkels RM, Van Duijnhoven FJ, Mols F, Breedveld-Peters JJ, et al. Dietary changes and dietary supplement use, and underlying motives for these habits reported by colorectal cancer survivors of the Patient Reported Outcomes Following Initial Treatment and Long-Term Evaluation of Survivorship (PROFILES) registry. Br J Nutr. 2015;114(2):286–96.
Pang KW. The making of Chinese medicine in Hong Kong. Social Transformations in Chinese Societies. 2018;14(1):17–28.
Hoffman MC, Mulrooney DA, Steinberger J, Lee J, Baker KS, Ness KK. Deficits in physical function among young childhood cancer survivors. J Clin Oncol. 2013;31(22):2799–805.
Viscuse PV, Price K, Millstine D, Bhagra A, Bauer B, Ruddy KJ. Integrative medicine in cancer survivors. Curr Opin Oncol. 2017;29(4):235–42.
Eslami M, Badkoubeh RS, Mousavi M, Radmehr H, Salehi M, Tavakoli N, et al. Oral ascorbic acid in combination with beta-blockers is more effective than beta-blockers alone in the prevention of atrial fibrillation after coronary artery bypass grafting. Tex Heart Inst J. 2007;34(3):268–74.
Sohl SJ, Borowski LA, Kent EE, Smith AW, Oakley-Girvan I, Rothman RL, et al. Cancer survivors' disclosure of complementary health approaches to physicians: the role of patient-centered communication. Cancer. 2015;121(6):900–7.
Mao JJ, Palmer CS, Healy KE, Desai K, Amsterdam J. Complementary and alternative medicine use among cancer survivors: a population-based study. J Cancer Surviv. 2011;5(1):8–17.
Sibinga EM, Ottolini MC, Duggan AK, Wilson MH. Parent-pediatrician communication about complementary and alternative medicine use for children. Clin Pediatr (Phila). 2004;43(4):367–73.
Lemay J, Amin A, Pacaud D. Complementary and alternative medicine use in children and adolescents with type 1 diabetes. Paediatr Child Health. 2011;16(8):468–72.
Adams D, Dagenais S, Clifford T, Baydala L, King WJ, Hervas-Malo M, et al. Complementary and alternative medicine use by pediatric specialty outpatients. Pediatrics. 2013;131(2):225–32.
Gottschling S, Meyer S, Längler A, Scharifi G, Ebinger F, Gronwald B. Differences in use of complementary and alternative medicine between children and adolescents with cancer in Germany: a population based survey. Pediatr Blood Cancer. 2014;61(3):488–92.
Gagnon EM, Recklitis CJ. Parents' decision-making preferences in pediatric oncology: The relationship to health care involvement and complementary therapy use. Psychooncology. 2003;12(5):442–52.
Schneider C, Schneider D. The practice of autonomy: patients, doctors, and medical decisions. Oxford: Oxford University Press on Demand; 1998.
Haupt R, Essiaf S, Dellacasa C, Ronckers CM, Caruso S, Sugden E, et al. The ‘Survivorship Passport’ for childhood cancer survivors. Eur J Cancer. 2018;102:69–81.
Poplack DG, Fordis M, Landier W, Bhatia S, Hudson MM, Horowitz ME. Childhood cancer survivor care: development of the Passport for Care. Nat Rev Clin Oncol. 2014;11(12):740–50.
Funding
The research was supported by grant number 03170047 from the Food and Health Bureau Hong Kong (Health and Medical Research Fund Research Fellowship). The funder had no role in study design, data collection/analysis/interpretation or manuscript preparation.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection, and analysis were performed by CS Lam, YM Cheng, and HS Li. The first draft of the manuscript was written by CS Lam, and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Ethics approval
This study was approved by the Joint Chinese University of Hong Kong–New Territories East Cluster Clinical Research Ethics Committee (Ref. No. 2018.427).
Consent to participate
Informed consent was obtained from all the individual participants included in the study.
Consent for publication
Not applicable
Conflicts of interest
The authors have no conflicts of interest to declare that are relevant to the content of this article.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
ESM 1
(DOCX 44 kb).
Rights and permissions
About this article
Cite this article
Lam, C.S., Cheng, Y.M., Li, H.S. et al. Use of complementary or alternative medicine and potential interactions with chronic medications among Chinese survivors of childhood cancer. J Cancer Surviv 16, 568–581 (2022). https://doi.org/10.1007/s11764-021-01051-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11764-021-01051-5