Abstract
Purpose
Survivors of multiple primary cancers make up a sizable proportion of all cancer survivors, yet little is known about the health of this population. We examined the prevalence of medical conditions and physical function deficits among multiple primary survivors compared with single primary survivors and individuals without a cancer history.
Methods
Participants were enrolled in the Cancer Prevention Study (CPS)-II Nutrition Cohort in 1992/1993. Prevalent medical conditions (diabetes, heart conditions, cerebrovascular conditions, emphysema/chronic bronchitis, osteoporosis, osteoarthritis), physical function limitations, use of a cane or walker, balance difficulties, and falls within the past year were assessed on a follow-up survey completed in 2011. We estimated age- and sex-adjusted prevalence ratios (PRs), comparing multiple primary survivors (N = 1003) to single primary survivors (N = 12,849) and participants without cancer (N = 63,578).
Results
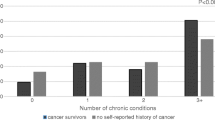
The prevalence of medical conditions did not differ substantially between multiple primary survivors and either comparison group. However, multiple primary survivors were more likely to report severe limitations in physical function than the single primary (PR = 1.48 (95% CI, 1.28–1.71)) and no-cancer (PR = 1.64 (95% CI, 1.42–1.88)) groups. Using a cane or walker and balance difficulties were also significantly more common among multiple primary survivors.
Conclusions
Despite a similar prevalence of comorbid medical conditions, severe functional limitations were significantly more common among multiple primary survivors than single primary survivors or individuals without cancer.
Implications for Cancer Survivors
Assessment of functional status and treatment of physical deficits may be an especially critical component of care for older patients with a history of multiple cancer diagnoses.
Similar content being viewed by others
References
American Cancer Society. Cancer treatment & survivorship facts & figures 2019–2021. Atlanta: American Cancer Society; 2019.
Travis LB. The epidemiology of second primary cancers. Cancer Epidemiol Biomark Prev. 2006;15(11):2020–6. https://doi.org/10.1158/1055-9965.Epi-06-0414.
Working Group Report. International rules for multiple primary cancers (ICD-0 third edition). Eur J Cancer Prev. 2005;14(4):307–8.
Travis LB, Demark Wahnefried W, Allan JM, Wood ME, Ng AK. Aetiology, genetics and prevention of secondary neoplasms in adult cancer survivors. Nat Rev Clin Oncol. 2013;10(5):289–301. https://doi.org/10.1038/nrclinonc.2013.41.
Mariotto AB, Rowland JH, Ries LA, Scoppa S, Feuer EJ. Multiple cancer prevalence: a growing challenge in long-term survivorship. Cancer Epidemiol Biomark Prev. 2007;16(3):566–71. https://doi.org/10.1158/1055-9965.Epi-06-0782.
Andrykowski MA. Physical and mental health status of survivors of multiple cancer diagnoses: findings from the National Health Interview Survey. Cancer. 2012;118(14):3645–53. https://doi.org/10.1002/cncr.26678.
Burris JL, Andrykowski MA. Physical and mental health status and health behaviors of survivors of multiple cancers: a national, population-based study. Ann Behav Med. 2011;42(3):304–12. https://doi.org/10.1007/s12160-011-9290-0.
Belcher SM, Hausmann EA, Cohen SM, Donovan HS, Schlenk EA. Examining the relationship between multiple primary cancers and psychological distress: a review of current literature. Psychooncology. 2017;26(12):2030–9. https://doi.org/10.1002/pon.4299.
Belcher SM, Low CA, Posluszny DM, Schear R, Kramer RE, Donovan HS. Psychological distress, health behaviors, and benefit finding in survivors of multiple primary cancers: results from the 2010 Livestrong Survey. Oncol Nurs Forum. 2017;44(6):703–11. https://doi.org/10.1188/17.Onf.703-711.
Gotay CC, Ransom S, Pagano IS. Quality of life in survivors of multiple primary cancers compared with cancer survivor controls. Cancer. 2007;110(9):2101–9. https://doi.org/10.1002/cncr.23005.
Thong MS, Mols F, Verhoeven RH, Liu L, Andrykowski MA, Roukema JA, et al. Multiple primary cancer survivors have poorer health status and well-being than single primary cancer survivors: a study from the population-based PROFILES registry. Psychooncology. 2013;22(8):1834–42. https://doi.org/10.1002/pon.3227.
Patnaik JL, Byers T, Diguiseppi C, Denberg TD, Dabelea D. The influence of comorbidities on overall survival among older women diagnosed with breast cancer. J Natl Cancer Inst. 2011;103(14):1101–11. https://doi.org/10.1093/jnci/djr188.
Sarfati D, Koczwara B, Jackson C. The impact of comorbidity on cancer and its treatment. CA Cancer J Clin. 2016;66(4):337–50. https://doi.org/10.3322/caac.21342.
Sogaard M, Thomsen RW, Bossen KS, Sorensen HT, Norgaard M. The impact of comorbidity on cancer survival: a review. Clin Epidemiol. 2013;5(Suppl 1):3–29. https://doi.org/10.2147/clep.S47150.
Williams GR, Dunham L, Chang Y, Deal AM, Pergolotti M, Lund JL, et al. Geriatric assessment predicts hospitalization frequency and long-term care use in older adult cancer survivors. J Oncol Pract. 2019;15(5):e399–409. https://doi.org/10.1200/jop.18.00368.
Pergolotti M, Deal AM, Williams GR, Bryant AL, Bensen JT, Muss HB, et al. Activities, function, and health-related quality of life (HRQOL) of older adults with cancer. J Geriatr Oncol. 2017;8(4):249–54. https://doi.org/10.1016/j.jgo.2017.02.009.
Calle EE, Rodriguez C, Jacobs EJ, Almon ML, Chao A, McCullough ML, et al. The American Cancer Society Cancer Prevention Study II Nutrition Cohort: rationale, study design, and baseline characteristics. Cancer. 2002;94(2):500–11. https://doi.org/10.1002/cncr.10197.
Hays RD, Bjorner JB, Revicki DA, Spritzer KL, Cella D. Development of physical and mental health summary scores from the patient-reported outcomes measurement information system (PROMIS) global items. Qual Life Res. 2009;18(7):873–80. https://doi.org/10.1007/s11136-009-9496-9.
Zou G. A modified Poisson regression approach to prospective studies with binary data. Am J Epidemiol. 2004;159(7):702–6. https://doi.org/10.1093/aje/kwh090.
Donin N, Filson C, Drakaki A, Tan HJ, Castillo A, Kwan L, et al. Risk of second primary malignancies among cancer survivors in the United States, 1992 through 2008. Cancer. 2016;122(19):3075–86. https://doi.org/10.1002/cncr.30164.
Pergolotti M, Deal AM, Lavery J, Reeve BB, Muss HB. The prevalence of potentially modifiable functional deficits and the subsequent use of occupational and physical therapy by older adults with cancer. J Geriatr Oncol. 2015;6(3):194–201. https://doi.org/10.1016/j.jgo.2015.01.004.
La Vecchia C, Giordano SH, Hortobagyi GN, Chabner B. Overweight, obesity, diabetes, and risk of breast cancer: interlocking pieces of the puzzle. Oncologist. 2011;16(6):726–9. https://doi.org/10.1634/theoncologist.2011-0050.
Wildiers H, Heeren P, Puts M, Topinkova E, Janssen-Heijnen ML, Extermann M, et al. International Society of Geriatric Oncology consensus on geriatric assessment in older patients with cancer. J Clin Oncol. 2014;32(24):2595–603. https://doi.org/10.1200/jco.2013.54.8347.
Economou D, Hurria A, Grant M. Integrating a cancer-specific geriatric assessment into survivorship care. Clin J Oncol Nurs. 2012;16(3):E78–85. https://doi.org/10.1188/12.Cjon.E78-e83.
Campbell PT, Deka A, Jacobs EJ, Newton CC, Hildebrand JS, McCullough ML, et al. Prospective study reveals associations between colorectal cancer and type 2 diabetes mellitus or insulin use in men. Gastroenterology. 2010;139(4):1138–46. https://doi.org/10.1053/j.gastro.2010.06.072.
Funding
The American Cancer Society, Inc. supports the maintenance and follow-up of the Cancer Prevention Studies.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interests.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the Emory University Institutional Review Board and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. This article does not contain any studies with animals performed by any of the authors.
Informed consent
All participants provided written informed consent.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOCX 22 kb) (DOCX 22 kb)
Rights and permissions
About this article
Cite this article
Anderson, C., Gapstur, S.M., Leach, C.R. et al. Medical conditions and physical function deficits among multiple primary cancer survivors. J Cancer Surviv 14, 518–526 (2020). https://doi.org/10.1007/s11764-020-00872-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11764-020-00872-0