Abstract
Purpose
Improvements in colorectal cancer (CRC) prevention, early detection, and treatment have resulted in substantial gains in survival. However, the health-related quality of life (HRQoL) of CRC survivors often depends on access to supportive care, which differs by survivors’ socioeconomic characteristics. The purpose of this study was to investigate the relationship between socioeconomic characteristics and HRQoL in a diverse group of CRC survivors.
Methods
We conducted a population-based, cross-sectional study to examine the association between socioeconomic factors (household income, health literacy, and insurance status) and HRQoL domains of pain interference, fatigue, physical function, sleep disturbance, anxiety, and depression. PROMIS® Short Forms v.2.0 were used to assess domains of HRQoL. Linear regression modeling was used to estimate the coefficient representing the average HRQoL domain score and its 95% confidence interval (CI).
Results
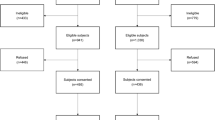
Three hundred one CRC survivors participated in the survey. Low-income (≤ $30,000) CRC survivors had, on average, a 4.70-point (95% CI 1.10–8.28) higher pain interference score, a 7.02-point (95% CI 3.27–10.77) higher fatigue score, a 5.13-point (95% CI − 8.56 to − 1.71) lower physical function score, and a 4.44-point (95% 1.40–7.49) higher depression score than CRC survivors with an income ≥ $70,000. Survivors with Medicaid insurance reported significantly greater pain interference and worse physical function than privately insured survivors. Survivors with low health literacy reported significantly greater pain interference compared with survivors with high health literacy.
Conclusions
Substantial socioeconomic disparities in HRQoL were observed in this diverse population of CRC survivors.
Implications for Cancer Survivors
Designing supportive care interventions to improve HRQoL among low-income and Medicaid-insured CRC survivors is critical for eliminating disparities in CRC outcomes.
Similar content being viewed by others
References
Bluethmann SM, Mariotto AB, Rowland JH. Anticipating the “Silver Tsunami”: prevalence trajectories and comorbidity burden among older cancer survivors in the United States. Cancer Epidemiol Biomark Prev. 2016;25(7):1029–36. https://doi.org/10.1158/1055-9965.EPI-16-0133.
SEER Cancer Statistics Review (CSR) 1975-2014 [database on the Internet]. National Cancer Institute. 2018. Available from: https://seer.cancer.gov/csr/1975_2014/. Accessed: April 11, 2018.
Mols F, Schoormans D, de Hingh I, Oerlemans S, Husson O. Symptoms of anxiety and depression among colorectal cancer survivors from the population-based, longitudinal PROFILES Registry: prevalence, predictors, and impact on quality of life. Cancer. 2018;124:2621–8. https://doi.org/10.1002/cncr.31369.
Russell L, Gough K, Drosdowsky A, Schofield P, Aranda S, Butow PN, et al. Psychological distress, quality of life, symptoms and unmet needs of colorectal cancer survivors near the end of treatment. J Cancer Surviv. 2015;9(3):462–70. https://doi.org/10.1007/s11764-014-0422-y.
Weaver KE, Forsythe LP, Reeve BB, Alfano CM, Rodriguez JL, Sabatino SA, et al. Mental and physical health-related quality of life among U.S. cancer survivors: population estimates from the 2010 National Health Interview Survey. Cancer Epidemiol Biomark Prev. 2012;21(11):2108–17. https://doi.org/10.1158/1055-9965.EPI-12-0740.
Yabroff KR, Lawrence WF, Clauser S, Davis WW, Brown ML. Burden of illness in cancer survivors: findings from a population-based national sample. J Natl Cancer Inst. 2004;96(17):1322–30. https://doi.org/10.1093/jnci/djh255.
Ness KK, Wall MM, Oakes JM, Robison LL, Gurney JG. Physical performance limitations and participation restrictions among cancer survivors: a population-based study. Ann Epidemiol. 2006;16(3):197–205. https://doi.org/10.1016/j.annepidem.2005.01.009.
Andrykowski MA, Aarts MJ, van de Poll-Franse LV, Mols F, Slooter GD, Thong MS. Low socioeconomic status and mental health outcomes in colorectal cancer survivors: disadvantage? advantage?... or both? Psychooncology. 2013;22(11):2462–9. https://doi.org/10.1002/pon.3309.
Stein KD, Syrjala KL, Andrykowski MA. Physical and psychological long-term and late effects of cancer. Cancer. 2008;112(11 Suppl):2577–92. https://doi.org/10.1002/cncr.23448.
Ohlsson-Nevo E, Karlsson J, Nilsson U. Effects of a psycho-educational programme on health-related quality of life in patients treated for colorectal and anal cancer: a feasibility trial. Eur J Oncol Nurs. 2016;21:181–8. https://doi.org/10.1016/j.ejon.2015.10.002.
Young J, Harrison J, Solomon M, Butow P, Dennis R, Robson D, et al. Development and feasibility assessment of telephone-delivered supportive care to improve outcomes for patients with colorectal cancer: pilot study of the CONNECT intervention. Support Care Cancer. 2010;18(4):461–70. https://doi.org/10.1007/s00520-009-0689-0.
NCI Dictionary of Cancer Terms. Published online at https://www.cancer.gov/publications/dictionaries/cancer-terms/2018. NCI dictionary of cancer terms. Accessed 15 Feb 2018
Ramsey SD, Andersen MR, Etzioni R, Moinpour C, Peacock S, Potosky A, et al. Quality of life in survivors of colorectal carcinoma. Cancer. 2000;88(6):1294–303.
Moreno PI, Ramirez AG, San Miguel-Majors SL, Fox RS, Castillo L, Gallion KJ, et al. Satisfaction with cancer care, self-efficacy, and health-related quality of life in Latino cancer survivors. Cancer. 2018;124(8):1770–9. https://doi.org/10.1002/cncr.31263.
Singh GK, Jemal A. Socioeconomic and racial/ethnic disparities in cancer mortality, incidence, and survival in the United States, 1950-2014: over six decades of changing patterns and widening inequalities. J Environ Public Health. 2017;2017:2819372. https://doi.org/10.1155/2017/2819372.
McDougall JA, Banegas MP, Wiggins CL, Chiu VK, Rajput A, Kinney AY. Rural disparities in treatment-related financial hardship and adherence to surveillance colonoscopy in diverse colorectal cancer survivors. Cancer Epidemiol Biomark Prev. 2018;27:1275–82. https://doi.org/10.1158/1055-9965.EPI-17-1083.
Hart LG, Larson EH, Lishner DM. Rural definitions for health policy and research. Am J Public Health. 2005;95(7):1149–55. https://doi.org/10.2105/AJPH.2004.042432.
Chew LD, Griffin JM, Partin MR, Noorbaloochi S, Grill JP, Snyder A, et al. Validation of screening questions for limited health literacy in a large VA outpatient population. J Gen Intern Med. 2008;23(5):561–6. https://doi.org/10.1007/s11606-008-0520-5.
Chew LD, Bradley KA, Boyko EJ. Brief questions to identify patients with inadequate health literacy. Fam Med. 2004;36(8):588–94.
SEER Program coding and staging manual 2018, (2018).
Health Measures: Transforming How Health is Measured. In: Intro to PROMIS®. Published online at http://www.healthmeasures.net/explore-measurement-systems/promis/intro-to-promis. 2018. http://www.healthmeasures.net/explore-measurement-systems/promis/intro-to-promis. Accessed April 19, 2018; 2018.
University of California Los Angeles Institute for Digital Research and Education. Regression with Stata chapter 2 – regression diagnostics. UCLA, Published online at https://stats.idre.ucla.edu/stata/webbooks/reg/chapter2/stata-webbooksregressionwith-statachapter-2-regression-diagnostics/. 2017. Accessed April 20, 2018; 2018.
Hudson MM, Mertens AC, Yasui Y, Hobbie W, Chen H, Gurney JG, et al. Health status of adult long-term survivors of childhood cancer: a report from the Childhood Cancer Survivor Study. JAMA. 2003;290(12):1583–92. https://doi.org/10.1001/jama.290.12.1583.
Chen CX, Kroenke K, Stump TE, Kean J, Carpenter JS, Krebs EE, et al. Estimating minimally important differences for the PROMIS pain interference scales: results from 3 randomized clinical trials. Pain. 2018;159(4):775–82. https://doi.org/10.1097/j.pain.0000000000001121.
Hays RD, Spritzer KL, Fries JF, Krishnan E. Responsiveness and minimally important difference for the patient-reported outcomes measurement information system (PROMIS) 20-item physical functioning short form in a prospective observational study of rheumatoid arthritis. Ann Rheum Dis. 2015;74(1):104–7. https://doi.org/10.1136/annrheumdis-2013-204053.
Yost KJ, Eton DT, Garcia SF, Cella D. Minimally important differences were estimated for six Patient-Reported Outcomes Measurement Information System-Cancer scales in advanced-stage cancer patients. J Clin Epidemiol. 2011;64(5):507–16. https://doi.org/10.1016/j.jclinepi.2010.11.018.
Altice CK, Banegas MP, Tucker-Seeley RD, Yabroff KR. Financial hardships experienced by cancer survivors: a systematic review. J Natl Cancer Inst. 2017;109(2):djw205. https://doi.org/10.1093/jnci/djw205.
Zafar SY, Abernethy AP. Financial toxicity, part I: a new name for a growing problem. Oncology (Williston Park). 2013;27(2):80–1, 149.
Kent EE, Forsythe LP, Yabroff KR, Weaver KE, de Moor JS, Rodriguez JL, et al. Are survivors who report cancer-related financial problems more likely to forgo or delay medical care? Cancer. 2013;119(20):3710–7. https://doi.org/10.1002/cncr.28262.
Park J, Look KA. Relationship between objective financial burden and the health-related quality of life and mental health of patients with cancer. J Oncol Pract. 2018;14(2):e113–e21. https://doi.org/10.1200/JOP.2017.027136.
Miller DB, Cage JL, Nowacki AS, Jackson B, Modlin CS. Health literacy (HL) & health-related quality of life (HRQL) among minority men. J Natl Med Assoc. 2018;110(2):124–9. https://doi.org/10.1016/j.jnma.2017.10.001.
Schaffler J, Leung K, Tremblay S, Merdsoy L, Belzile E, Lambrou A, et al. The effectiveness of self-management interventions for individuals with low health literacy and/or low income: a descriptive systematic review. J Gen Intern Med. 2018;33(4):510–23. https://doi.org/10.1007/s11606-017-4265-x.
Niu X, Roche LM, Pawlish KS, Henry KA. Cancer survival disparities by health insurance status. Cancer Med. 2013;2(3):403–11. https://doi.org/10.1002/cam4.84.
Parikh AA, Robinson J, Zaydfudim VM, Penson D, Whiteside MA. The effect of health insurance status on the treatment and outcomes of patients with colorectal cancer. J Surg Oncol. 2014;110(3):227–32. https://doi.org/10.1002/jso.23627.
Robbins AS, Pavluck AL, Fedewa SA, Chen AY, Ward EM. Insurance status, comorbidity level, and survival among colorectal cancer patients age 18 to 64 years in the National Cancer Data Base from 2003 to 2005. J Clin Oncol. 2009;27(22):3627–33. https://doi.org/10.1200/JCO.2008.20.8025.
Ahmed S, Berzon RA, Revicki DA, Lenderking WR, Moinpour CM, Basch E, et al. The use of patient-reported outcomes (PRO) within comparative effectiveness research: implications for clinical practice and health care policy. Med Care. 2012;50(12):1060–70. https://doi.org/10.1097/MLR.0b013e318268aaff.
Calvert M, Kyte D, Mercieca-Bebber R, Slade A, Chan AW, King MT, et al. Guidelines for inclusion of patient-reported outcomes in clinical trial protocols: the SPIRIT-PRO extension. JAMA. 2018;319(5):483–94. https://doi.org/10.1001/jama.2017.21903.
Funding
The Surface Family Trust (A. Kinney) and internal start-up funding (A. Kinney and J. McDougall) from the University of New Mexico Comprehensive Cancer Center were used to support this project.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
McDougall, J.A., Blair, C.K., Wiggins, C.L. et al. Socioeconomic disparities in health-related quality of life among colorectal cancer survivors. J Cancer Surviv 13, 459–467 (2019). https://doi.org/10.1007/s11764-019-00767-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11764-019-00767-9