Abstract
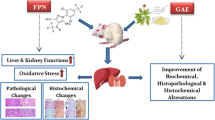
Zearalenone (ZEN) is a mycotoxin that contaminates crops worldwide and whose toxic adverse effects are well documented. This study aims to evaluate the protective effect of gallic acid (GA) against biochemical, oxidative, inflammatory, and pathological changes in ZEN treated rats’ hepatorenal system. Wistar rats (n = 50; 150 ± 30 g) were randomly grouped into five cohorts (= 10) specifically: Control (rat chow); ZEN alone (100 µg/kg; per os), GA alone (40 mg/kg; per os), ZEN + GA1 (100 µg/kg + 20 mg/kg per os) and ZEN + GA2 (100 µg/kg + 40 mg/kg per os) and the study was for 28 successive days. Upon terminal sacrifice, biomarkers of hepatorenal function and oxidative stress were analyzed. An assessment of cytokine levels (IL-1β, IL-10) and histopathology of the liver and kidneys was also performed. Relative to the control, serum levels of urea, creatinine, and hepatic transaminases increased significantly (p < 0.05) in the ZEN alone group and reduced in groups co-treated with GA. ZEN treatment further resulted in decreases in the rat’s antioxidant status. The increase in the reactive oxygen and nitrogen species (RONS) and lipid peroxidation (LPO) levels caused by ZEN exposure was reduced by GA in a dose-dependent manner (p < 0.05). Furthermore, ZEN-mediated increase in nitric oxide (NO), xanthine oxidase (XO), IL-1β, and myeloperoxidase (MPO) levels and suppression of IL-10 levels were reversed in the liver and kidney of GA co-treated rats. The extent of ZEN-mediated hepatorenal lesions was reduced in rats co-treated with GA. Our findings suggest that GA effectively abated biochemical, oxido-inflammatory and histological alteration caused by ZEN exposure, limiting ZEN toxicity and cellular damage in rats’ hepatic and renal tissues.
Similar content being viewed by others
Introduction
Zearalenone (ZEN) or the F-2 or RAL (resorcylic acid lactone) is a mycotoxin primarily produced by the fungus Fusarium graminearum (Zhang et al. 2016; Zinedine et al. 2007). ZEN contaminates agricultural products worldwide (Darwish et al. 2014; Wang et al. 2020). Its exposure results in harmful effects on humans and animals’ health (Aiko and Mehta 2015; Bennett and Klich 2003; Binder et al. 2017). ZEN is commonly found in the moderate climate zone, and exhibits high stability during storage and does not degrade when exposed to high temperature (Appell et al. 2017; Bai et al. 2018).
Studies have shown that exposure to ZEN is hepatotoxic (Bai et al. 2018), alters immune and hematologic function (Ben Salem et al. 2015; Wang et al. 2018b) and is systemically toxic (Rai et al. 2019). Thus elimination of ZEN from contaminated produce is of great importance (Wang et al. 2018c), as ZEN can be absorbed into the body, metabolised via hydroxylation to form either toxic α- and β-Zearalenol (α- and β-ZEL) (Olsen et al. 1987; Rai et al. 2019) in the liver (Malekinejad et al. 2006), and the gastrointestinal tract (Biehl et al. 1993). α-ZEL happens to be the more toxic of the two metabolites. (Brodehl et al. 2014) After absorption, ZEN is highly distributed in the liver (Rai et al. 2020). It also gets distributed to the kidney, intestine, fatty tissues, reproductive organs like the uterus, testes, and ovaries (Jiang et al. 2012; Koraichi et al. 2012). Plants and fungi can also metabolize ZEN by attaching polar residues like glucose and sulphates to mask the mycotoxin (Berthiller et al. 2013; Binder et al. 2017). Primarily, ZEN and its metabolites are glucuronidated in the liver and intestine of humans and animals at the sterically unobstructed phenolic 14-hydroxy group to form ZEN-16-GlcA (Pfeiffer et al. 2010). Glucuronic acid conjugation of α-ZEL mediates its final metabolic fate and excretion (Videmann et al. 2008). Recent studies revealed that α- and β-Zearalenol mediate their toxicities in the liver, kidney and other cells of the body by upregulating the activities of the glucose-regulated protein (GRP78) and, Growth arrest and DNA-damage induced protein (GADD34), resulting in endoplasmic reticulum stress (ERS)(Ben Salem et al. 2016). The induction of ERS is characterized by increased reactive oxygen species (ROS) generation (Marin et al. 2013), inflammatory responses (Jia et al. 2014), lipid peroxidation (Ben Salem et al. 2016; Wang et al. 2019), thereby decreasing endogenous antioxidant activities.
Considering the adverse impacts that ZEN and other mycotoxins have on human and livestock well-being, it is of immense public health significance to create plausible stratagems for neutralizing mycotoxins (Kowalska et al. 2016). Although the most effective method is prevention, it is relatively impractical to avoid mycotoxin contamination of crops.
Several strategies have been devised to reduce human and livestock exposure to ZEN. Among these strategies is microbial degradation of ZEN in situ (Wang et al. 2018c). Adding Bacillus velezensis A2 as an additive could effectively remove ZEN in feed and protect mice against ZEN toxic damage from the contaminated diet (Wang et al. 2018a) and wheat treatment with manganese to protect Zearalenone infection and its derivatives (Gzyl-Malcher et al. 2019). Supplementation with the carotenoid Crocin has been demonstrated to help mitigate ZEN-induced oxidative stress in the liver and kidney (Ben Salem et al. 2015) of mice. Furthermore, in vitro studies revealed that Kefir protect against ZEN toxicity and oxidative damage in cultured HCT-116 cell line (El Golli-Bennour et al. 2019) and opuntia ficus-indica protected Balb/C mice against oxidative damage induced by Zearalenone (Zourgui et al. 2008). Polyphenolic compounds, which can confer beneficial effects, and serve as chemoprotective pharmacological agents in preventing ZEN toxicity, have been investigated in in vitro and systemically. Gallic acid (GA, 3,4,5-trihydroxybenzoic acid) is a polyphenolic compound naturally present in some herbal formulation used in phytomedicine; with various biological properties which aid its ability to protect tissues and organs against the injuries induced by toxic compounds(Constant 1997; Mansouri et al. 2013; Owumi et al. 2020a). GA is readily absorbed in the gastrointestinal tract compared to several other polyphenolic acids, although its bioavailability is limited due to rapid metabolism and high elimination rate (Shahrzad et al. 2001). GA has been documented to exhibit antioxidant and anticancer activities (Badhani et al. 2015), substantial anti-inflammatory property (Banerjee et al. 2015), and a beneficial modulator of the immune system fending off microbial infection (Choubey et al. 2018). GA is recognized as safe by the Food and Drug Administration and has been used as an antioxidant in food, cosmetics, and pharmaceuticals (Shahrzad et al. 2001). GA has been reported to elicit protective effects against other mycotoxins – aflatoxin B1- which induces hepatorenal damage and oxido-inflammatory in rats’ stress (Owumi et al. 2020b). However, the shortage of data validating the protective effects of GA against ZEN-induced toxicity in relevant animal models necessitated this study.
Herein, we report in vivo findings on ZEN and GA’s effects on hepatorenal function in albino Wistar rats. We observed that GA ameliorated ZEN-induced hepatorenal dysfunction by decreasing oxidative stress, lipid peroxidation and inflammation in rats. Furthermore, GA protected against histopathological changes in the liver and kidney of rats exposed to ZEN for 28 consecutive days. To our knowledge, there is no reported study in the literature describing the protective in vivo effects of GA on ZEN-induced hepatorenal toxicity and oxidative damage, inflammatory responses and induction of apoptosis. This study is of significance, giving GA and gallate esters everyday use as antioxidants in cosmetics, food, and pharmaceutical industries (Monteiro et al. 2017; Ow and Stupans 2003).
Materials and methods
Chemicals
Zearalenone (≥ 99 %) and gallic acid were purchased from AKSci Scientific (San Mateo, CA, USA) and Sigma-Aldrich Chemical Company (St. Louis, Mo), respectively. 1-chloro-2,4-dinitrobenzene (CDNB), thiobarbituric acid (TBA), hydrogen peroxide (H2O2), 5’, 5’-dithiobis-2-nitrobenzoic acid (DTNB), epinephrine and glutathione (GSH) were procured from Sigma Aldrich Chemical Co. (MO, USA). Interleukin-1β (IL-1β), interleukin-10 (IL-10) and tumour necrosis factor-alpha (TNF-α), Enzyme-Linked Immunosorbent Assay (ELISA) kits were purchased from E-labscience Biotechnology (Beijing, China). Other chemicals used for these experiments were pure analytical grade and purchased from British Drug Houses (Poole, Dorset, U.K.).
Animal model and care for experimental animals
Adult Wistar rat (sex: male; ages: 10 weeks old; weight: 150 ± 30 g; n = 50) were procured from the Primate Colony Animal House Facility, College of Medicine, University of Ibadan and housed in polycarbonate cages in a well-ventilated animal house with free access to standard rat pellets (Ladokun™ Feeds, Ibadan, Nigeria) and water. Rats were allowed to adapt (one week) to their new environment preceding experimentation for a photoperiod of 12-hr light: 12-hr dark cycle and adequately cared for as specified by ‘Guide for the Care and Use of Laboratory Animals published by the National Institute of Health. All experiment was performed following the approved procedures by the University of Ibadan Ethical Committee and the guidelines of the United States National Academy of Sciences.
Experimental protocol
Experimental rats were assigned randomly to five groups consisting of ten rats each post acclimatization. They were dosed per os (p.o.) either with ZEN:100 µg/kg or GA: 20 and 40 mg/kg body weight and in combination in co-treated groups as required for four consecutive weeks as:
-
Control: treated with corn oil alone (2 ml/kg; p.o.).
-
Zearalenone (ZEN) alone: treated with ZEN (100 µg /kg; p.o).
-
Gallic Acid (GA) alone: treated with GA (40 mg/kg; p.o).
-
Zearalenone + GA1: treated with ZEN + GA (100 µg /kg + 20 mg/kg; p.o).
-
Zearalenone + GA2: treated with ZEN + GA (100 µg /kg + 40 mg/kg; p. o).
The doses of ZEN (100 µg/kg) (Cressey and Thomson 2006; Shin et al. 2009) and GA (20 and 40 mg/kg) (Garud and Kulkarni 2018; Owumi et al. 2020b) bodyweights used for this study were based on earlier published reviews. On day 29, after the last treatment, terminal body weights of experimental animals were recorded before exsanguination via the retro-orbital venous plexus to collect blood samples into pre-labelled plain tubes. Subsequently, rats were sacrificed by dislocation of the cervical vertebrae light ether anaesthesia. Serum was obtained by centrifugation (4000 g; 10 min; 40 C) of blood allowed to clot at room temperature. Subsequently, serum samples were preserved at -20 °C pending routine analysis of hepato-renal function biomarkers.
Evaluation of biomarkers of hepato-renal function
Serum levels of biomarkers of hepato-renal function such as aspartate aminotransferase (AST), alanine aminotransferase (ALT), alkaline phosphatase (ALP), lactate dehydrogenase (LDH), urea and creatinine were determined using commercial kits (Randox™ Laboratories Limited, Crumlin, U.K.).
Preparation of tissue homogenates and evaluation of biomarkers of hepato-renal antioxidant status and lipid peroxidation
Homogenization of the rat liver and kidney samples were performed in Tris–HCl buffer (50 mM; pH 7.4), the tissue homogenates were centrifuged (10,000 g; 15 min; 4 °C) to obtain the supernatants utilized in examining for the biomarkers of apoptosis, inflammation, and oxidative stress. Hepato-renal protein concentration was determined according to Lowry’s method (Lowry et al. 1951). Superoxide dismutase (SOD) activity was evaluated using the method described by Misra and Fridovich (Misra and Fridovich 1972), while catalase (CAT) enzyme activity was assessed by Claiborne’s technique (Clairborne 1995; Owumi et al. 2019b). Glutathione-S-transferase (GST) and glutathione peroxidase (GPx) enzyme activities were evaluated using Habig’s (Habig et al. 1974; Owumi et al. 2019b) and Rotruck’s (Owumi et al. 2020a; Rotruck et al. 1973) protocols, respectively. Furthermore, Glutathione (GSH) and Lipid peroxidation – by measuring malondialdehyde (MDA)- levels were assayed for, using the methods of Ellman (Ellman 1959) and Okhawa (Ohkawa et al. 1979), respectively.
Evaluation of reactive oxygen and nitrogen species (RONS) level
RONS generated in the hepatic and renal tissues was estimated with an established protocol that depends on RONS-dependent oxidation of 2’,7’-dichlorodihydrofluorescin diacetate (DCFH-DA) to 2’,7’-dichlorofluorescin (DCF) (Owumi and Dim 2019; Perez-Severiano et al. 2004). Quickly, the reaction mixture {sample + potassium phosphate buffer (0.1 M; pH 7.4) + DI water + DCFH-DA} was prepared with minimal exposure to air. Fluorescence emission of DCF arising from DCFHDA oxidation was evaluated for 10 min at an emission and excitation wavelengths of 525 and 488nm. The readings were obtained with M384 SpectraMax™ Multi-modal plate reader (Molecular Devices, San Jose, CA, USA). The proportion of DCF formation was expressed as a percentage fold over the control group.
Estimation of inflammatory biomarkers
In the hepato-renal samples, Nitric oxide (NO) levels were determined by the methods of Green (Green et al. 1982). The reaction mixture containing equal volume (sample + Griess reagent) was incubated for 15 min, and absorbance readings recorded at 540 nm. NO levels were extrapolated from a generated standard curve and expressed as Units/mg protein. Myeloperoxidase (MPO) activity was assayed following the previously described method by Granell (Granell et al. 2003; Owumi et al. 2020c).
Furthermore, hepatic and renal concentrations of IL-10 and IL-1β were evaluated using ELISA Kits from E-labscience (Beijing, China) following the manufacturer’s protocol. All readings were obtained with M384 SpectraMax™ Multi-modal plate reader (Molecular Devices, San Jose, CA, USA).
Histopathological examination of liver and kidney
Liver and kidney samples that were earlier fixed in phosphate-buffered formalin (10 %; for three days) were randomly selected for histological analysis. The samples were embedded in paraffin following sequential dehydration processes. Subsequently, microtome sliced tissue Secs. (4–5 μm) were fixed on charged microscopic glass slides before hematoxylin and eosin (H & E) staining (Bancroft and Gamble 2008; Owumi et al. 2019a). Histopathologic examination of hepatic and renal tissue was conducted with the aid of a light microscope (Leica DM 500, Germany), pathological abnormalities were scored by a pathologist blinded to experimental slides. Images were captured using a digital camera (Leica ICC50 E, Germany) attached to the microscope.
Statistical analysis
Experimental data were expressed as mean ±S. D, n = 10 per group. The values obtained were analyzed using one-way ANOVA followed by Dunnett’s multiple comparisons tests, performed using GraphPad Prism version 8.3.0 for Mac, GraphPad Software, San Diego, California USA, www.graphpad.com; Statistically significant values were set at p < 0.05.
Results
GA caused a reduction in terminal body weight and relieved hepatic and renal toxicity in ZEN treated rats
The bodyweight of rat treated with ZEN alone increased by 7.33 % compared to the untreated control. ZEN + GA1 and ZEN + GA2 co-treated groups also differed by 4.89 and 3.30 %, respectively, compared to the ZEN alone treated group Table 1. A 4.54 % increase in the body weights of rats treated with GA alone relative to the untreated control was also observed. ZEN alone treated exhibited almost no treatment-related body and relative organ weight gains. The effect of GA on ZEN-induced hepatorenal toxicity was evaluated by creatinine and urea and hepatic transaminases (ALT, AST, ALP and GGT) level in the serum. Figure 1 describes GA’s influence on biomarkers of hepatic and renal toxicity in ZEN-treated rats. Exposure to ZEN (100 µg/kg) increased significantly (p < 0.05) biomarkers of hepatic and renal injury in rat serum compared to the control rats. The AST, ALT, ALP, and GGT increased by 135.4 %, 222.1 %, 110.9 %, and 111.1 %, respectively, compared to the control group. In rats co-treated with GA (20 and 40 mg/kg) and ZEN, GA reduced ZEN-mediated increases in creatinine and urea levels, in addition to ALT, AST, ALP and GGT activities in rat serum compared to ZEN alone treated rats Fig. 1. Treatment with GA (40 mg/kg) alone caused almost no treatment-related changes in hepatorenal biomarkers of toxicity. Treatment with GA alone at 40 mg/kg for 28 successive days caused almost no treatment-related effect on these biomarkers.
Effect of gallic acid (GA) on hepatorenal functional enzymes in Zearalenone (ZEN)-treated rats. Zearalenone (ZEN: 100 µg/Kg); GA1: 20 mg/kg; GA2: 40 mg/kg. Data are shown as mean ± S.D; (n = 10) per group. Significance markers indicate groups compared to one another (p < 0.05). * to ****: indicates the level of significance. AST: aspartate aminotransferase; ALT: alanine aminotransferase; GGT: gamma-glutamyl transferase; ALP: alanine aminotransferase; Creatinine and Urea
GA treatment restored ZEN-induced reduction in hepatic and renal antioxidant enzymes activities, GSH, and total thiol levels in rats
The influence of GA on the oxidative stress indices in ZEN-treated rats was evaluated and the results presented in Figs. 2 and 3. Results showed a decrease (p < 0.05) in the activities of SOD CAT and total thiols (TSH) in the liver of ZEN treated rats by 90.18 %, 71.37 and 45.01 %, respectively and in the kidney by 94.2 %, 29.7 %, and 29 % respectively compared to the control Fig. 2. There was also a decrease (p < 0.05) in the activities of GST, GPx, and GSH in the liver of ZEN alone treated rats by 83.78 %, 47.25 %, and 48.65 %, respectively, and in the kidney of ZEN alone treated rats by 54.4 %, 32.69 %, and 56.4 % respectively when compared to the control groups Fig. 3. Co-treatment with GA at 20 and 40 mg/kg decreased (p < 0.05) the reduction in the activities of these antioxidant enzymes (SOD, CAT, GST and GPx) and significantly restored their hepatic and renal activities similar to control levels in ZEN + GA2 (40 mg/kg) -treated rats. Treatment with GA alone significantly increased hepatorenal GSH and TSH level relative to both control cohorts - untreated controls and ZEN alone.
Effect of gallic acid (GA) on SOD, CAT activities, and TSH levels in the liver and kidney of rats treated with Zearalenone (ZEN: 100 µg/Kg); GA1: 20 mg/kg; GA2: 40 mg/kg. Data are shown as mean ± S.D; (n = 10) per group. Significance markers indicate groups compared to one another (p < 0.05). * to ****: indicates the level of significance. SOD: superoxide dismutase; CAT: catalase, and TSH: total thiol group
Effect of gallic acid (GA) on GST, GPx activities, and GSH levels in the liver and kidney of rats treated with Zearalenone (ZEN: 100 µg/Kg); GA1: 20 mg/kg; GA2: 40 mg/kg. Data are shown as mean ± S.D.; (n = 10) per group. Significance markers indicate groups compared to one another (p < 0.05). * to ****: indicates the level of significance. GST: glutathione-S-transferase; GPx: glutathione peroxidase, and GSH: glutathione
GA attenuates ZEN-induced hepatorenal RONS generation, xanthine oxidase (XO) activity and induction of lipid peroxidation (LPO) in rats
The effect of GA on RONS generation, xanthine oxidase (XO) activity and subsequent lipid peroxidation (LP) in experimental rats were evaluated, and the results are presented in Fig. 4. Treatment with ZEN alone evidently increased (p < 0.05) RONS levels in the liver (40.79 %), kidney (56.2 %) relative to the untreated control group. Also, LPO levels in the kidney and liver of ZEN alone treated rats were also increased (p < 0.05) by 125.6 and 50 %, respectively, compared to untreated control. Co-treatment with GA protected against renal and hepatic lipid peroxidative damage evidenced by decreases (p < 0.05) in RONS and LPO levels relative to rats treated with ZEN alone. Reduction in RONS levels in groups co-treated with ZEN + GA1 and ZEN + GA2 was 23.14 and 34.43 %, respectively, compared to the ZEN alone group in the liver and 22.4 and 34.6 % respectively compared to ZEN alone group in the kidney. LPO levels in groups co-treated with ZEN + GA1 and ZEN + GA2 were reduced (p < 0.05) by 20.37 and 42.59 % in the liver, 24.4 and 65.6 % in the kidney relative to ZEN alone treated rats. Furthermore, XO activity was decreased (p < 0.05) in the liver and kidney of ZEN + GA treated rats dose-dependently by GA1: 16.5 and 22.8 %; and GA2: 55.7 and 42.3 %, respectively. ZEN alone treated rats exhibited high levels of XO activity in the liver (169.44 %) and Kidney (105.1 %) Fig. 4.
Effect of gallic acid (GA) on RONS, LPO levels, and XO activities in the liver and kidney of rats treated with Zearalenone (ZEN: 100 µg/Kg); GA1: 20 mg/kg; GA2: 40 mg/kg. Data are shown as mean ± S.D.; (n = 10) per group. Significance markers indicate groups compared to one another (p < 0.05). * to ****: indicates the level of significance. RONS: reactive oxygen and nitrogen species; LPO: lipid peroxidation, and XO: xanthine oxidase
GA suppresses ZEN mediated increase in biomarkers of inflammation in rats
The influence of GA on the biomarkers of inflammation was assessed in ZEN-treated rats’ liver and kidney. Figures 5 and 6 depict the impact of GA on biomarkers of inflammation, administration of ZEN alone increased (p < 0.05) the hepatic and renal MPO activity, and levels of NO, and IL-1β, and suppressed IL-10 levels relative to the untreated control group. In the liver, NO level and MPO activity in ZEN alone treated rats increased by 81.28 and 182.4 %, respectively, compared to the untreated control Fig. 5. NO and MPO in the kidney also increased by 80 and 93.2 % compared to the untreated control. In ZEN alone, treated rats level of IL-1β increased in the liver (361.5 %) and kidney (81.9 %), while IL-10 levels decreased in the liver (55 %) and kidney (68.57 %) relative to untreated control Fig. 6. Co-treatment with GA alleviated ZEN-mediated increases in the preceding biomarkers of inflammation. Group co-treated with ZEN + GA2 dose-dependently decreased (p < 0.05) IL-1β level and increased IL-10 levels relative to group co-treated with ZEN + GA1. The levels of IL-1β and IL-10 in the liver and kidneys of rats treated with GA only did not differ (p < 0.05) compared to the untreated control rats.
Effect of gallic acid (GA) on NO level, and MPO activity in the liver and kidney of rats treated with Zearalenone (ZEN: 100 µg/Kg); GA1: 20 mg/kg; GA2: 40 mg/kg. Data are shown as mean ± S.D.; (n = 10) per group. Significance markers indicate groups compared to one another (p < 0.05). * to ****: indicates the level of significance. NO: nitric oxide; MPO: myeloperoxidase
Effect of gallic acid (GA) on IL-1β, and IL-10 levels in the liver and kidney of rats treated with Zearalenone (ZEN: 100 µg/Kg); GA1: 20 mg/kg; GA2: 40 mg/kg. Data are shown as mean ± S.D.; (n = 10) per group. Significance markers indicate groups compared to one another (p < 0.05). * to ****: indicates the level of significance—IL-1β: Interleukin-1beta, and IL-10: Interleukin-10
GA reversed ZEN-induced hepatorenal lesions in exposed rats
The representative photomicrographs depicting GA’s influence on ZEN-induced histological damage in the liver and kidney of experimental rats are shown in Figs. 7 and 8. The kidney and liver of control and rats treated with GA alone appeared normal with typical, well-preserved histological architecture. Administration of ZEN alone caused disseminated congestion, infiltration of inflammatory cells and glomerular dystrophy with disaggregated podocytes, whereas the liver showed significant congestion and focal periportal infiltration by inflammatory cells. However, rats treated with GA1 and GA2 combined with ZEN presented typical liver and kidney histological features and were similar to control.
Representative photomicrographs of the liver from control, ZEN only, GA only, co-exposure groups. Control and gallic acid (GA) only-treated groups showed typical hepatic architecture. Zearalenone (ZEN) only-treated rats showed marked disseminated portal fibrosis and congestion (black arrow), infiltration by inflammatory cells (red arrow) and necrosis (green arrow). ZEN + GA1 and ZEN + GA2 appeared comparable to the control. H and E stained, Magnification: x400
Representative photomicrographs of the kidney section from control, ZEN only, GA only, co-exposure groups. Control and gallic acid (GA) only-treated groups showed typical kidney architecture. Zearalenone (ZEN) only-treated rats showed severe disseminated tubular necrosis (black arrow), infiltration by inflammatory cells (red arrow) and disseminated segmental glomerular necrosis (green arrow). The kidney of rats treated with ZEN and GA appeared comparable to the control. H and E stained, Magnification: x400
Discussion
ZEN is a mycotoxin that contaminates feedstuff and crops worldwide, resulting in toxic effects on human and animal health (Aiko and Mehta 2015; Bennett and Klich 2003; Binder et al. 2017; Darwish et al. 2014; Wang et al. 2020) exposed to such contaminated product. Here we investigated the protective role of GA against ZEN-induced oxidative, inflammatory and pathological changes in rats. After exposure to ZEN for 28-days, rats showed an attenuated gain in body weight relative to the untreated control (p < 0.05) (Table 1). This reduction in weight gain may be attributed to loss of appetite (Joslyn and Glick 1969; Roberts et al. 2007), decreased nutrient digestibility, or reduced growth (Wang et al. 2012). Co-treatment with GA reversed ZEN-induced reduction in weight gain dose-dependently. This result is indicative of a beneficial role of GA in enhancing digestibility (Banerjee et al. 2005). However, the peculiar drop in body weight gain, especially in rats co-treated with ZEN + GA1, can perhaps be attributed to GA’s ability to cause a reduction in body weight (Totani et al. 2011). Previously reported data indicates that GA decreased bodyweight when GA was administered intraperitoneally to experimental rats (Roberts et al. 2007). Thus, the mechanism by which GA reduces food intake involves more than taste aversion or gastrointestinal factors. The reason could also be related to ZEN metabolites’ fate and kinetics, which was administered to the animals and competitive binding to the metabolic site.
Increases in hepatic transaminases in serum indicate hepatobiliary system dysfunction (Kaplan 1993; Ramaiah 2007) and subsequent seeping of hepatic specific transaminases -AST, GGT, ALT ALP- into circulation that are easily quantified as biomarkers of hepatobiliary-toxicity. ZEN treatment resulted in increases (p < 0.05) of hepatic transaminases -AST, ALT, and ALP- activities when compared to the control, a reflection of the hepatotoxicity of ZEN as previously reported (Gao et al. 2018; Zhou et al. 2015). GA co-treatment ameliorated the damage induced by ZEN by decreasing (p < 0.05) serum hepatic transaminases in the GA co-treated groups dose-dependently.
The kidneys are key players in the excretion of waste products and toxins such as urea and creatinine generated from the degradation of proteins and waste produced from muscle breakdowns (Katari et al. 2017; Rubenstein et al. 2012). Urea and creatinine clearance reflect kidney function, and increases in serum urea and creatinine levels indicate a dysfunctional kidney (Bidani and Churchill 1989). ZEN treatment caused significantly high serum creatinine and urea levels in experimental rats; these increases could suggest impaired renal function/renal damage, dehydration, and protein catabolism (Hejazy and Koohi 2017) caused by ZEN exposure. GA dose-dependently reduced serum urea and creatinine levels, further underscoring GA’s ability to protect against ZEN toxicity.
ZEN has been reported to increase oxidative stress (Wang et al. 2012), supporting our current finding, where ZEN treatment resulted in increased generation of RONS, depleting GSH / total thiol (TSH) levels and upregulated endogenous antioxidant enzyme (GPx, GST, SOD, CAT) activities primarily involved in mitigating oxidative stress in the experimental animal. GA’s antioxidative and –inflammatory activities (Badhani et al. 2015; Banerjee et al. 2015; Choubey et al. 2018; Usha et al. 2014), without manifesting toxicity or any adverse clinical indications, have been well demonstrated in the literature. GA enhanced antioxidant levels by increasing GSH and TSH levels in the liver and kidney of treated rats. TSH status, especially thiol (-SH) groups present on protein, are considered significant plasma antioxidants in vivo, and most of them are present in albumin (Prakash et al. 2004). These -SHs are the major reducing groups present in the body fluids (Monod et al. 1965). Oxidative damage is mainly caused by the generation of many RONS and free radicals. RONS generated in the tissues can stimulate oxidative tissue damage due to the inability to detoxify these toxic radicals. Exposure to ZEN alone caused an increase in RONS levels in the liver and kidney tissues, and such exposure is implicated in LPO formation. As expected, we also observed an increase in LPO levels in the liver and kidneys of ZEN treated rats, indicated by the significant rise in Malondialdehyde (MDA) content compared to the control (Ben Salah-Abbes et al. 2009; Zourgui et al. 2008). GA co-treatment significantly reduced RONS and LPO levels in rats’ liver and kidney, attributable to GA’s reported free radical scavenging ability (Choubey et al. 2018).
XO is a valuable marker for the assessment of liver function (Battelli et al. 2001). We observed that XO activities increased in liver and kidney of ZEN treated rats while co-treatment with GA showed a dose-dependent decrease in XO activity compared to ZEN alone. NO is a signalling molecule involved in the onset of inflammation (Sharma et al. 2006), and it is a marker of inflammation. NO toxicity is attributable to its ability to act in conjunction with superoxide anion and disrupt the structure of macromolecules such as proteins, thus inhibiting their function (Carr et al. 2000), triggering an inflammatory response. Increased NO levels in the liver and kidney of rats treated alone with ZEN indicate an inflammatory response. GA resisted the enhanced production of NO exemplified by decreases in NO levels in the co-treated groups, in agreement with earlier reports of GA’s anti-inflammatory properties (Choubey et al. 2018).
MPO is a hemoprotein expressed in neutrophils and monocytes (Valko et al. 2006). An increase in MPO activity is associated with leukocyte infiltration, a significant inflammatory response player (Badhani et al. 2015; Usha et al. 2014). We observed that ZEN treatment significantly increased MPO activity in liver and kidney rats. In contrast, GA co-treatment reversed this observed increase in MPO activity, indicative of inhibition of leukocytes infiltration. IL-1β is a known pro-inflammatory cytokine involved in the mediation of inflammatory response (Valko et al. 2006).
Conversely, IL-10 is an anti-inflammatory cytokine capable of enhancing antibody production and β-cell survival (Gutierrez-Murgas et al. 2016; Steen et al. 2020). ZEN treated rats showed a significant increase in IL-1β in liver and kidney tissues than the control group. Co-treatment with GA caused a concomitant decrease in IL-1β and increased IL-10 (p < 0.05) levels in test rats’ liver and kidney compared to the controls. Other parameters evaluated were the histopathological changes in the test rats’ hepatorenal system. While control rats presented with typical histoarchitecture of the liver and kidney, ZEN treatment resulted in moderate to marked disseminated periportal infiltration by inflammatory cells and focal congestion, in line with previous findings reported Jia et al. (2014). Co-treatment with GA alleviated histological damages induced by ZEN alone with moderate disseminated congestion and mild infiltration by inflammatory cells.
On the other hand, the kidney of rats treated with ZEN alone shows a focal area of congestion and mild disseminated glomerular congestion/hypercellularity. These were reserved by GA co-treatment, where the kidney appears to be similar to the control rat kidney—taken together, dosing rats adversely altered all parameters measured with ZEN alone. They were mitigated in the presence of GA, indicating that GA can serve as an antidote to diminish ZEN-mediated toxic biochemical alteration and oxido-inflammatory responses, as shown in our proposed mechanism of GA action Fig. 9. Collectively, GA could serve as a protective biomolecule against ZEN inadvertently present in the food supply.
Structures of naturally occurring Zearalenone (ZEN), illustrating the metabolic pathways involved in ZEN metabolism by 3α and 3β -hydroxysteroid dehydrogenase (HSDs) and cytochrome P450 s(CYP450s)-mediated activation of ZEN. We focused on the formation and fates of α and β-Zearalenol that result in the cyto-, hepato- and genotoxicity of ZEN. The plausible mechanism(s) of GA-mediated phytochemical based prevention of ZEN-induced injury in rats’ liver and kidney. Note that uridylyl-glucuronic transferase (UGT) is known to detoxify α and β-Zearalenol further, here was used as a model to illustrate the consequence of induction of Phase II drug-metabolizing enzymes by GA. Red arrow indicates upregulation, black arrow indicates downregulation, and blue T-arrow indicates suppression
Conclusions
The free radical scavenging activity of GA as a result of its polyphenolic content makes GA not only valuable for the food industry, especially in baked foods where it helps prevent rancidity, but also in cosmetics pharmaceutical industries. The present study showed GA’s ability to reverse oxidative, inflammatory and pathological damages induced by ZEN in the liver and kidney of male Wistar rats due to its antioxidative, anti-inflammatory capacity. These results suggest that GA can protect the hepatorenal system of rats exposed to ZEN from damages by enhancing antioxidant activities, decreasing hepatorenal toxicity, and reducing some inflammatory biomarkers levels and activities in the liver and kidney of rats in the co-treated groups. Due to the beneficial and pivotal role played by GA in mitigating hepatorenal alterations induced by ZEN in rats, GA could be considered as an additive in the rat diet to prevent damages caused by accidental exposure to ZEN, as well as other probable mycotoxins exposure.
References
Aiko V, Mehta A (2015) Occurrence, detection and detoxification of mycotoxins. J Biosci 40:943–954. https://doi.org/10.1007/s12038-015-9569-6
Appell M, Wang LC, Bosma WB (2017) Analysis of the photophysical properties of zearalenone using density functional theory. J Lumines 188:551–557
Badhani B, Sharma N, Kakkar R (2015) Gallic acid: a versatile antioxidant with promising therapeutic and industrial applications. RSC Adv 5:27540–27557. https://doi.org/10.1039/c5ra01911g
Bai X, Sun C, Xu J, Liu D, Han Y, Wu S, Luo X (2018) Detoxification of zearalenone from corn oil by adsorption of functionalized GO systems. Appl Surf Sci 430:198–207. https://doi.org/10.1016/j.apsusc.2017.06.055
Bancroft JD, Gamble M (2008) Theory and practise of histological techniques, 6th edn. Churchill Livingstone Elsevier, Philadelphia
Banerjee R, Mukherjee G, Patra KC (2005) Microbial transformation of tannin-rich substrate to gallic acid through co-culture method. Bioresour Technol 96:949–953. https://doi.org/10.1016/j.biortech.2004.08.004
Banerjee N, Kim H, Krenek K, Talcott ST, Mertens-Talcott SU (2015) Mango polyphenolics suppressed tumor growth in breast cancer xenografts in mice: role of the PI3K/AKT pathway and associated microRNAs. Nutr Res 35:744–751. https://doi.org/10.1016/j.nutres.2015.06.002
Battelli MG, Musiani S, Valgimigli M, Gramantieri L, Tomassoni F, Bolondi L, Stirpe F (2001) Serum xanthine oxidase in human liver disease. Am J Gastroenterol 96:1194–1199. https://doi.org/10.1111/j.1572-0241.2001.03700.x
Ben Salah-Abbes J, Abbes S, Abdel-Wahhab MA, Oueslati R (2009) Raphanus sativus extract protects against Zearalenone induced reproductive toxicity, oxidative stress and mutagenic alterations in male Balb/c mice. Toxicon 53:525–533. https://doi.org/10.1016/j.toxicon.2009.01.013
Ben Salem I, Boussabbeh M, Helali S, Abid-Essefi S, Bacha H (2015) Protective effect of Crocin against zearalenone-induced oxidative stress in liver and kidney of Balb/c mice . Environ Sci Pollut Res Int 22:19069–19076. https://doi.org/10.1007/s11356-015-5086-2
Ben Salem I, Boussabbeh M, Prola A, Guilbert A, Bacha H, Lemaire C, Abid-Essefi S (2016) Crocin protects human embryonic kidney cells (HEK293) from alpha- and beta-Zearalenol-induced ER stress and apoptosis . Environ Sci Pollut Res Int 23:15504–15514. https://doi.org/10.1007/s11356-016-6741-y
Bennett JW, Klich M (2003) Mycotoxins. Clin Microbiol Rev 16:497–516. https://doi.org/10.1128/cmr.16.3.497-516.2003
Berthiller F et al (2013) Masked mycotoxins: a review . Mol Nutr Food Res 57:165–186. https://doi.org/10.1002/mnfr.201100764
Bidani A, Churchill PC (1989) Acute renal failure. Dis Mon 35:63–132. https://doi.org/10.1016/0011-5029(89)90017-5
Biehl ML, Prelusky DB, Koritz GD, Hartin KE, Buck WB, Trenholm HL (1993) Biliary excretion and enterohepatic cycling of zearalenone in immature pigs. Toxicol Appl Pharmacol 121:152–159. https://doi.org/10.1006/taap.1993.1140
Binder SB, Schwartz-Zimmermann HE, Varga E, Bichl G, Michlmayr H, Adam G, Berthiller F (2017) Metabolism of zearalenone and its major modified forms in pigs. Toxins (Basel) 9. https://doi.org/10.3390/toxins9020056
Brodehl A, Moller A, Kunte HJ, Koch M, Maul R (2014) Biotransformation of the mycotoxin zearalenone by fungi of the genera Rhizopus and Aspergillus FEMS. Microbiol Lett 359:124–130. https://doi.org/10.1111/1574-6968.12586
Carr AC, McCall MR, Frei B (2000) Oxidation of LDL by myeloperoxidase and reactive nitrogen species: reaction pathways and antioxidant protection Arterioscler. Thromb Vasc Biol 20:1716–1723. https://doi.org/10.1161/01.atv.20.7.1716
Choubey S, Goyal S, Varughese LR, Kumar V, Sharma AK, Beniwal V (2018) Probing gallic acid for its broad spectrum applications. Mini Rev Med Chem 18:1283–1293. https://doi.org/10.2174/1389557518666180330114010
Clairborne A (1995) Catalase activity. Handbook of Methods for Oxygen Radical Research. CRC Press, Boca Raton
Constant J (1997) Alcohol, ischemic heart disease, and the French paradox. Clin Cardiol 20:420–424. https://doi.org/10.1002/clc.4960200504
Cressey P, Thomson B (2006) Risk profile: Mycotoxins in the New Zealand food supply, in The New Zealand Mycotoxin Surveillance Program 06-14 Report Series, R. Vannoort, Editor. 2014, Institute of Environmental Sciences & Research Limited: Christchurch, p 177
Darwish WS, Ikenaka Y, Nakayama SM, Ishizuka M (2014) An overview on mycotoxin contamination of foods in Africa. J Vet Med Sci 76:789–797. https://doi.org/10.1292/jvms.13-0563
El Golli-Bennour E, Timoumi R, Koroit M, Bacha H, Abid-Essefi S (2019) Protective effects of kefir against zearalenone toxicity mediated by oxidative stress in cultured HCT-116cells. Toxicon 157:25–34. https://doi.org/10.1016/j.toxicon.2018.11.296
Ellman GL (1959) Tissue sulfhydryl groups. Arch Biochem Biophys 82:70–77. https://doi.org/10.1016/0003-9861(59)90090-6
Gao X et al (2018) Dietary silymarin supplementation alleviates zearalenone-induced hepatotoxicity and reproductive toxicity in rats. J Nutr 148:1209–1216. https://doi.org/10.1093/jn/nxy114
Garud MS, Kulkarni YA (2018) Gallic acid attenuates type I diabetic nephropathy in rats. Chem Biol Interact 282:69–76. https://doi.org/10.1016/j.cbi.2018.01.010
Granell S et al (2003) Heparin mobilizes xanthine oxidase and induces lung inflammation in acute pancreatitis. Crit Care Med 31:525–530. https://doi.org/10.1097/01.CCM.0000049948.64660.06
Green LC, Wagner DA, Glogowski J, Skipper PL, Wishnok JS, Tannenbaum SR (1982) Analysis of nitrate, nitrite, and [15 N]nitrate in biological fluids. Anal Biochem 126:131–138. https://doi.org/10.1016/0003-2697(82)90118-x
Gutierrez-Murgas YM, Skar G, Ramirez D, Beaver M, Snowden JN (2016) IL-10 plays an important role in the control of inflammation but not in the bacterial burden in S. epidermidis CNS catheter infection. J Neuroinflammation 13:271. https://doi.org/10.1186/s12974-016-0741-1
Gzyl-Malcher B, Rudolphi-Skorska E, Sieprawska A, Filek M (2019) Manganese protects wheat from the mycotoxin zearalenone and its derivatives. Sci Rep 9:14214. https://doi.org/10.1038/s41598-019-50664-5
Habig WH, Pabst MJ, Jakoby WB (1974) Glutathione S-transferases. The first enzymatic step in mercapturic acid formation. J Biol Chem 249:7130–7139. https://doi.org/10.1016/S0021-9258(19)42083-8
Hejazy M, Koohi MK (2017) Effects of Nano-zinc on Biochemical Parameters in Cadmium-Exposed Rats . Biol Trace Elem Res 180:265–274. https://doi.org/10.1007/s12011-017-1008-0
Jia Z, Liu M, Qu Z, Zhang Y, Yin S, Shan A (2014) Toxic effects of zearalenone on oxidative stress, inflammatory cytokines, biochemical and pathological changes induced by this toxin in the kidney of pregnant rats. Environ Toxicol Pharmacol 37:580–591. https://doi.org/10.1016/j.etap.2014.01.010
Jiang SZ et al (2012) Effect on hepatonephric organs, serum metabolites and oxidative stress in post-weaning piglets fed purified zearalenone-contaminated diets with or without calibrin-Z. J Anim Physiol Anim Nutr (Berl) 96:1147–1156. https://doi.org/10.1111/j.1439-0396.2011.01233.x
Joslyn MA, Glick (1969) Comparative effects of gallotannic acid and related phenolics on the growth of rats. J Nutr 98:119–126. https://doi.org/10.1093/jn/98.1.119
Kaplan MM (1993) Laboratory tests, vol 1. Diseases of the liver, 7th edn. Lippincott, Philadelphia
Katari R et al (2017) Tissue engineering and regenerative medicine solutions for the abdominal organs. In: Thomaz-Soccol V, Pandey A, Resende RR (eds) Current developments in biotechnology and bioengineering. Elsevier, Amsterdam, pp 325–347. https://doi.org/10.1016/B978-0-444-63660-7.00013-9
Koraichi F, Videmann B, Mazallon M, Benahmed M, Prouillac C, Lecoeur S (2012) Zearalenone exposure modulates the expression of ABC transporters and nuclear receptors in pregnant rats and fetal liver. Toxicol Lett 211:246–256. https://doi.org/10.1016/j.toxlet.2012.04.001
Kowalska K, Habrowska-Gorczynska DE, Piastowska-Ciesielska AW (2016) Zearalenone as an endocrine disruptor in humans. Environ Toxicol Pharmacol 48:141–149. https://doi.org/10.1016/j.etap.2016.10.015
Lowry OH, Rosebrough NJ, Farr AL, Randall RJ (1951) Protein measurement with the Folin phenol reagent. J Biol Chem 193:265–275
Malekinejad H, Maas-Bakker R, Fink-Gremmels J (2006) Species differences in the hepatic biotransformation of zearalenone. Vet J 172:96–102. https://doi.org/10.1016/j.tvjl.2005.03.004
Mansouri MT, Naghizadeh B, Ghorbanzadeh B, Farbood Y, Sarkaki A, Bavarsad K (2013) Gallic acid prevents memory deficits and oxidative stress induced by intracerebroventricular injection of streptozotocin in rats. Pharmacol Biochem Behav 111:90–96. https://doi.org/10.1016/j.pbb.2013.09.002
Marin DE, Pistol GC, Neagoe IV, Calin L, Taranu I (2013) Effects of zearalenone on oxidative stress and inflammation in weanling piglets. Food Chem Toxicol 58:408–415. https://doi.org/10.1016/j.fct.2013.05.033
Misra HP, Fridovich I (1972) The role of superoxide anion in the autoxidation of epinephrine and a simple assay for superoxide dismutase. J Biol Chem 247:3170–3175
Monod J, Wyman J, Changeux J-P (1965) On the nature of allosteric transitions: A plausible model. J Mol Biol 12:88–118. https://doi.org/10.1016/s0022-2836(65)80285-6
Monteiro E et al (2017) Gallic acid-loaded gel formulation combats skin oxidative stress: Development, characterization and ex vivo biological assays. Polymers (Basel) 9. https://doi.org/10.3390/polym9090391
Ohkawa H, Ohishi N, Yagi K (1979) Assay for lipid peroxides in animal tissues by thiobarbituric acid reaction. Anal Biochem 95:351–358. https://doi.org/10.1016/0003-2697(79)90738-3
Olsen M, Pettersson H, Sandholm K, Visconti A, Kiessling KH (1987) Metabolism of zearalenone by sow intestinal mucosa in vitro. Food Chem Toxicol 25:681–683. https://doi.org/10.1016/0278-6915(87)90101-3
Ow YY, Stupans I (2003) Gallic acid and gallic acid derivatives: effects on drug metabolizing enzymes. Curr Drug Metab 4:241–248. https://doi.org/10.2174/1389200033489479
Owumi SE, Dim UJ (2019) Manganese suppresses oxidative stress, inflammation and caspase-3 activation in rats exposed to chlorpyrifos. Toxicol Rep 6:202–209. https://doi.org/10.1016/j.toxrep.2019.02.007
Owumi SE, Ajijola IJ, Agbeti OM (2019a) Hepatorenal protective effects of protocatechuic acid in rats administered with anticancer drug methotrexate. Hum Exp Toxicol 38:1254–1265. https://doi.org/10.1177/0960327119871095
Owumi SE, Dim UJ, Najophe ES (2019b) Diethylnitrosamine aggravates cadmium-induced hepatorenal oxidative damage in prepubertal rats. Toxicol Ind Health 35:537–547. https://doi.org/10.1177/0748233719863287
Owumi S, Najophe ES, Farombi EO, Oyelere AK (2020a) Gallic acid protects against Aflatoxin B1 -induced oxidative and inflammatory stress damage in rats kidneys and liver. J Food Biochem 44:e13316. https://doi.org/10.1111/jfbc.13316
Owumi SE, Najophe SE, Farombi OE, Oyelere AK (2020b) Gallic Acid protects against Aflatoxin B1-induced oxidative and inflammatory stress damage in rats kidneys and liver. J Food Biochem. https://doi.org/10.1111/jfbc.13316
Owumi SE, Olayiwola YO, Alao GE, Gbadegesin MA, Odunola OA (2020) Cadmium and nickel co-exposure exacerbates genotoxicity and not oxido-inflammatory stress in liver and kidney of rats: Protective role of omega-3 fatty acid. Environ Toxicol 35:231–241. https://doi.org/10.1002/tox.22860
Perez-Severiano F, Santamaria A, Pedraza-Chaverri J, Medina-Campos ON, Rios C, Segovia J (2004) Increased formation of reactive oxygen species, but no changes in glutathione peroxidase activity, in striata of mice transgenic for the Huntington’s disease mutation. Neurochem Res 29:729–733. https://doi.org/10.1023/b:nere.0000018843.83770.4b
Pfeiffer E, Hildebrand A, Mikula H, Metzler M (2010) Glucuronidation of zearalenone, zeranol and four metabolites in vitro: formation of glucuronides by various microsomes and human UDP-glucuronosyltransferase isoforms. Mol Nutr Food Res 54:1468–1476. https://doi.org/10.1002/mnfr.200900524
Prakash M, Upadhya S, Prabhu R (2004) Protein thiol oxidation and lipid peroxidation in patients with uraemia. Scand J Clin Lab Invest 64:599–604. https://doi.org/10.1080/00365510410002869
Rai A, Das M, Tripathi A (2019) Occurrence and toxicity of a fusarium mycotoxin, zearalenone. Crit Rev Food Sci Nutr:1–20 https://doi.org/10.1080/10408398.2019.1655388
Rai A, Das M, Tripathi A (2020) Occurrence and toxicity of a fusarium mycotoxin zearalenone. Crit Rev Food Sci Nutr 60:2710–2729. https://doi.org/10.1080/10408398.2019.1655388
Ramaiah SK (2007) A toxicologist guide to the diagnostic interpretation of hepatic biochemical parameters. Food Chem Toxicol 45:1551–1557. https://doi.org/10.1016/j.fct.2007.06.007
Roberts AT et al (2007) The safety and efficacy of a dietary herbal supplement and gallic acid for weight loss. J Med Food 10:184–188. https://doi.org/10.1089/jmf.2006.272
Rotruck JT, Pope AL, Ganther HE, Swanson AB, Hafeman DG, Hoekstra WG (1973) Selenium: biochemical role as a component of glutathione peroxidase. Science 179:588–590. https://doi.org/10.1126/science.179.4073.588
Rubenstein DA, Yin W, Frame MD (2012) Chap. 12 - flow through the kidney. In: Rubenstein DA, Yin W, Frame MD (eds) Biofluid Mechanics. Academic, Boston, pp 325–345. https://doi.org/10.1016/B978-0-12-381383-1.00012-6
Shahrzad S, Aoyagi K, Winter A, Koyama A, Bitsch I (2001) Pharmacokinetics of gallic acid and its relative bioavailability from tea in healthy humans. J Nutr 131:1207–1210. https://doi.org/10.1093/jn/131.4.1207
Sharma V, McNeill JH, Verma S (2006) Diabetic cardiomyopathy: Where are we 40 years later? Can J Cardiol 22:305–308. https://doi.org/10.1016/s0828-282x(06)70914-x
Shin BS et al (2009) Physiologically based pharmacokinetics of zearalenone. J Toxicol Environ Health A 72:1395–1405. https://doi.org/10.1080/15287390903212741
Steen EH, Wang X, Balaji S, Butte MJ, Bollyky PL, Keswani SG (2020) The role of the anti-inflammatory cytokine interleukin-10 in tissue fibrosis . Adv Wound Care (New Rochelle) 9:184–198. https://doi.org/10.1089/wound.2019.1032
Totani N, Tateishi S, Takimoto T, Maeda Y, Sasaki H (2011) Gallic acid glycerol ester promotes weight-loss in rats. J Oleo Sci 60:457–462. https://doi.org/10.5650/jos.60.457
Usha T, Middha SK, Bhattacharya M, Lokesh P, Goyal AK (2014) Rosmarinic acid, a new polyphenol from Baccaurea ramiflora Lour. Leaf: A probable compound for its anti-inflammatory activity . Antioxidants (Basel) 3:830–842. https://doi.org/10.3390/antiox3040830
Valko M, Rhodes CJ, Moncol J, Izakovic M, Mazur M (2006) Free radicals, metals and antioxidants in oxidative stress-induced cancer. Chem Biol Interact 160:1–40. https://doi.org/10.1016/j.cbi.2005.12.009
Videmann B, Mazallon M, Tep J, Lecoeur S (2008) Metabolism and transfer of the mycotoxin zearalenone in human intestinal Caco-2 cells. Food Chem Toxicol 46:3279–3286. https://doi.org/10.1016/j.fct.2008.07.011
Wang N et al (2018a) The protective role of Bacillus velezensis A2 on the biochemical and hepatic toxicity of zearalenone in mice. Toxins (Basel) 10. https://doi.org/10.3390/toxins10110449
Wang X et al (2018) Toxic effects of Zearalenone on intestinal microflora and intestinal mucosal immunity in mice. Food Agric Immunol 29:1002–1011. https://doi.org/10.1080/09540105.2018.1503233
Wang JP, Chi F, Kim IH (2012) Effects of montmorillonite clay on growth performance, nutrient digestibility, vulva size, faecal microflora, and oxidative stress in weaning gilts challenged with zearalenone. Anim Feed Sci Technol 178:158–166. https://doi.org/10.1016/j.anifeedsci.2012.09.004
Wang Y, Zhang J, Wang Y, Wang K, Wei H, Shen L (2018) Isolation and characterization of the Bacillus cereus BC7 strain, which is capable of zearalenone removal and intestinal flora modulation in mice. Toxicon 155:9–20. https://doi.org/10.1016/j.toxicon.2018.09.005
Wang N, Wu W, Pan J, Long M (2019) Detoxification strategies for zearalenone using microorganisms: a review. Microorganisms 7. https://doi.org/10.3390/microorganisms7070208
Wang M, Yang S, Cai J, Yan R, Meng L, Long M, Zhang Y (2020) Proteomic analysis using iTRAQ technology reveals the toxic effects of zearalenone on the leydig cells of rats. Food Chem Toxicol:111405. https://doi.org/10.1016/j.fct.2020.111405
Zhang H, Dong M, Yang Q, Apaliya MT, Li J, Zhang X (2016) Biodegradation of zearalenone by Saccharomyces cerevisiae: Possible involvement of ZEN responsive proteins of the yeast. J Proteomics 143:416–423. https://doi.org/10.1016/j.jprot.2016.04.017
Zhou C, Zhang Y, Yin S, Jia Z, Shan A (2015) Biochemical changes and oxidative stress induced by zearalenone in the liver of pregnant rats. Hum Exp Toxicol 34:65–73. https://doi.org/10.1177/0960327113504972
Zinedine A, Soriano JM, Molto JC, Manes J (2007) Review on the toxicity, occurrence, metabolism, detoxification, regulations and intake of zearalenone: an oestrogenic mycotoxin. Food Chem Toxicol 45:1–18. https://doi.org/10.1016/j.fct.2006.07.030
Zourgui L, Golli EE, Bouaziz C, Bacha H, Hassen W (2008) Cactus (Opuntia ficus-indica) cladodes prevent oxidative damage induced by the mycotoxin zearalenone in Balb/C mice. Food Chem Toxicol 46:1817–1824. https://doi.org/10.1016/j.fct.2008.01.023
Acknowledgements
This research was done without any specific grant from a funding agency in the public, commercial, or not-for-profit sector.
Author information
Authors and Affiliations
Contributions
All authors partook in the design, interpretation, and analysis of the study’s data. SEO and SON conceptualized the experiments; SN and TI: carried out the research and preliminary data analysis. SEO, SON, supervised the investigation, SEO, SON proof check data for error. The manuscript was written and revised by SEO, SON, SN and TI.
Corresponding author
Ethics declarations
Ethical standards
All experimentation results reported in this manuscript comply with all laws on using laboratory animals in Nigeria’s experimentation and according to global best practices.
Conflict of interest
The authors have no conflict of interest to declare.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Owumi, S.E., Najophe, S.E., Idowu, T.B. et al. Protective mechanisms of gallic acid on hepatorenal dysfunction of zearalenone treated rat. Biologia 76, 3123–3135 (2021). https://doi.org/10.1007/s11756-021-00828-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11756-021-00828-4