Abstract
Background
The spectrum of ground glass opacity (GGO) is a diagnostic and clinical management quandary. The role of computed tomographic scans in detecting malignant GGO has inter-observer variability. Pure GGO have been traditionally thought to be predominantly benign in nature and has long volume doubling times. This study was undertaken to correlate the findings of radiology and histology of ground glass opacities at our institute.
Methods
This study is a retrospective observational study of patients who underwent lung resection surgery for radiology proven ground glass opacities between January 2010 and December 2018. A total of 115 patients were included in the study based on inclusion and exclusion criteria and were analysed.
Results
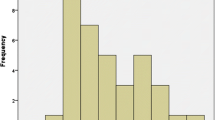
The patients were divided into two groups; pure GGO (n = 50), mixed GGO (n = 65). The pathological tumour size was ≤ 2 cm in 51% of the patients and 27 patients had the size between 2.1 and 3.0 cm. The predominant histopathologic feature was lepidic predominance in 54 patients followed by 24 patients with acinar predominance. Among patients with radiological tumour size of ≤ 2 cm, pure GGO was present in 48% of the patients. Among patients with pure GGO, 96% of the patients had no solid component. 44 patients had only single CT scan before proceeding to surgery. All these patients had mixed GGO.
Conclusion
Our study concludes pure GGOs, though lacking solid component have a high propensity to be malignant. The role of repeated CT surveillance in this context without offering curative surgery may be questionable.
Similar content being viewed by others
References
Migliore M, Fornito M, Palazzolo M, et al. Ground glass opacities management in the lung cancer screening era. Ann Transl Med 2018; https://doi.org/10.21037/atm.2017.07.28
Chen D, Dai C, Kadeer X, et al. New horizons in surgical treatment of ground-glass nodules of the lung: experience and controversies. Ther Clin Risk Manag. 2018;14:203–11. https://doi.org/10.2147/TCRM.S152127.
Lee C-T. What do we know about ground-glass opacity nodules in the lung? Transl Lung Cancer Res. 2015;4:656–9. https://doi.org/10.3978/j.issn.2218-6751.2015.04.05.
Travis WD, Brambilla E, Noguchi M, et al. International association for the study of lung cancer/american thoracic society/european respiratory society international multidisciplinary classification of lung adenocarcinoma. J Thorac Oncol. 2011;6:244–85. https://doi.org/10.1097/JTO.0b013e318206a221.
Hasegawa M, Sone S, Takashima S, et al. Growth rate of small lung cancers detected on mass CT screening. Br J Radiol. 2000;73:1252–9. https://doi.org/10.1259/bjr.73.876.11205667.
Huang C, Wang C, Wang Y, et al. The prognostic significance of pure ground glass opacities in lung cancer computed tomographic images. J Cancer. 2019;10:6888–95. https://doi.org/10.7150/jca.33132.
Suzuki K, Koike T, Asakawa T, et al. A prospective radiological study of thin-section computed tomography to predict pathological noninvasiveness in peripheral clinical IA lung cancer (Japan Clinical Oncology Group 0201). J Thorac Oncol. 2011;6:751–6. https://doi.org/10.1097/JTO.0b013e31821038ab.
Son JY, Lee HY, Lee KS, et al. Quantitative CT analysis of pulmonary ground-glass opacity nodules for the distinction of invasive adenocarcinoma from pre-invasive or minimally invasive adenocarcinoma. PLoS ONE. 2014. https://doi.org/10.1371/journal.pone.0104066.
Lim H-J, Ahn S, Lee KS, et al. Persistent pure ground-glass opacity lung nodules ≥ 10 mm in diameter at CT scan: histopathologic comparisons and prognostic implications. Chest. 2013;144:1291–9. https://doi.org/10.1378/chest.12-2987.
Mimae T, Miyata Y, Tsutani Y, et al. What are the radiologic findings predictive of indolent lung adenocarcinoma? Jpn J Clin Oncol. 2015;45:367–72. https://doi.org/10.1093/jjco/hyv005.
Detterbeck FC. More opaque than clear: reality is always cloaked in shades of gray. Oncology (Williston Park). 2016;30:275–6.
Aokage K, Saji H, Suzuki K, et al. A non-randomized confirmatory trial of segmentectomy for clinical T1N0 lung cancer with dominant ground glass opacity based on thin-section computed tomography (JCOG1211). Gen Thorac Cardiovasc Surg. 2017;65:267–72. https://doi.org/10.1007/s11748-016-0741-1.
Okada M, Koike T, Higashiyama M, et al. Radical sublobar resection for small-sized non-small cell lung cancer: a multicenter study. J Thorac Cardiovasc Surg. 2006;132:769–75. https://doi.org/10.1016/j.jtcvs.2006.02.063.
Rami-Porta R, Tsuboi M. Sublobar resection for lung cancer. Eur Respir J. 2009;33:426–35. https://doi.org/10.1183/09031936.00099808.
Zha J, Xie D, Xie H, et al. Recognition of “aggressive” behavior in “indolent” ground glass opacity and mixed density lesions. J Thorac Dis. 2016;8:1460–8. https://doi.org/10.21037/jtd.2016.05.33.
Jennings SG, Winer-Muram HT, Tarver RD, et al. Lung tumor growth: assessment with CT–comparison of diameter and cross-sectional area with volume measurements. Radiology. 2004;231:866–71. https://doi.org/10.1148/radiol.2313030715.
Kobayashi Y, Fukui T, Ito S, et al. How long should small lung lesions of ground-glass opacity be followed? J Thorac Oncol. 2013;8:309–14. https://doi.org/10.1097/JTO.0b013e31827e2435.
Yatabe Y, Borczuk AC, Powell CA. Do all lung adenocarcinomas follow a stepwise progression? Lung Cancer. 2011;74:7–11. https://doi.org/10.1016/j.lungcan.2011.05.021.
Kobayashi Y, Mitsudomi T, Sakao Y, et al. Genetic features of pulmonary adenocarcinoma presenting with ground-glass nodules: the differences between nodules with and without growth. Ann Oncol. 2015;26:156–61. https://doi.org/10.1093/annonc/mdu505.
Zhang Y, Fu F, Chen H. Management of ground-glass opacities in the lung cancer spectrum. Ann Thorac Surg. 2020;110:1796–804. https://doi.org/10.1016/j.athoracsur.2020.04.094.
Hasegawa M, Sakai F, Ishikawa R, et al. CT Features of epidermal growth factor receptor-mutated adenocarcinoma of the lung: comparison with nonmutated adenocarcinoma. J Thorac Oncol. 2016;11:819–26. https://doi.org/10.1016/j.jtho.2016.02.010.
Glynn C, Zakowski MF, Ginsberg MS. Are there imaging characteristics associated with epidermal growth factor receptor and KRAS mutations in patients with adenocarcinoma of the lung with bronchioloalveolar features? J Thorac Oncol. 2010;5:344–8. https://doi.org/10.1097/JTO.0b013e3181ce9a7a.
Rizzo S, Petrella F, Buscarino V, et al. CT Radiogenomic characterization of EGFR, K-RAS, and ALK mutations in non-small cell lung cancer. Eur Radiol. 2016;26:32–42. https://doi.org/10.1007/s00330-015-3814-0.
Hattori A, Suzuki K, Takamochi K, et al. Prognostic impact of a ground-glass opacity component in clinical stage IA non–small cell lung cancer. J Thorac Cardiovasc Surg. 2021;161:1469–80. https://doi.org/10.1016/j.jtcvs.2020.01.107.
Acknowledgements
The authors thank Eliazar Dimalapang for the statistical analysis.
Funding
Nil.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None to declare.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ram, D., Egan, H. & Ramanathan, T. Ground glass opacity: can we correlate radiological and histological features to plan clinical decision making?. Gen Thorac Cardiovasc Surg 70, 971–976 (2022). https://doi.org/10.1007/s11748-022-01826-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11748-022-01826-2