Abstract
Background
The aim of this study was to investigate the effects of bivalirudin on endothelial cell proliferation and neointimal hyperplasia in a rabbit carotid artery model.
Methods
“New Zealand rabbits (n = 12)” weighing 2–3 kg were randomly divided into two groups. Arteriotomy was performed to the rabbit carotid artery and closed with continuous suture technique. Group B (n = 6) as a control group received 150 U/kg heparin sodium; however, group A (n = 6) was given 0.75 mg/kg bivalirudin i.v. bolus and infusion 1.75 mg/kg/hour (B01AE06-Bivalirudin 250 mg) during perioperation period. At the end of the 28th day, the carotid artery segment was excised and evaluated histologically.
Results
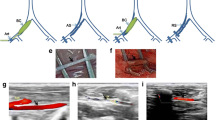
All histological and immune staining analyzes were performed by two blind researchers in the treatment of rabbits. In the control group rabbit carotid artery sections, tunica intima was observed to thicken. In the bivalirudin group, intimal hyperplasia was less observed compared to the control group. No significant difference was observed between groups in tunica media thickness. Lumen diameter and lumen area were found to be wider in the experimental group. P value was found to be less than 0.05.
Conclusion
Our study demonstrates that bivalirudin significantly affects and prevents neointimal hyperplasia and endothelial cell proliferation.






Similar content being viewed by others
References
Chen X, Ren S, Ma MG, Sudharshan D, Lin L, Mengzhou X, et al. Hirulog-like peptide reduces restenosis and expression of tissue factor and transforming growth factor-beta in carotid artery of atherosclerotic rabbits. Atherosclerosis. 2003;169(1):31–40.
Akkaya G, Bilen C, Gencpinar T, Akokay P, Uğurlu B. Effects of rivaroxaban on intimal hyperplasia and smooth muscle cell proliferation at the carotid artery anastomosis site in rabbits. Anatol J Cardiol. 2017;18(4):261–5.
Anand S, Kim M, Kamran C, Samin KS, Annapoorna SK, Fareed J, et al. Comparison of platelet function and morphology in patients undergoing percutaneous coronary ıntervention receiving bivalirudin versus unfractionated heparin versus clopidogrel pretreatment and bivalirudin. Am J Cardiol. 2007;100(3):417–24.
Stone GW, McLaurin BT, Cox DA, Bertrand ME, Lincoff AM, Moses JW, et al. Bivalirudin for patients with acute coronary syndromes. N Engl J Med. 2006;355(21):2203–16.
Weitz J, Bates M. Acute coronary syndromes: A focus on thrombin. J Invasive Cardiol. 2002;14(Suppl B):2B–7B.
Hasija S, Talwar S, Makhija N, Sandeep C, Poonam M, Ujjwal KC, et al. Randomized controlled trial of heparin versus bivalirudin anticoagulation in acyanotic children undergoing open heart surgery. J Cardiothorac Vasc Anesth. 2018;32(6):2633–40.
Shore-Lesserson L, Baker RA, Ferraris V, Greilich PE, Fitzgerald D, Roman P, et al. STS/SCA/AmSECT clinical practice guidelines: anticoagulation during cardiopulmonary bypass. J Extra Corpor Technol. 2018;50(1):5–18.
Yau JW, Stafford AR, Liao P, Robin R, Weitz J. Mechanism of catheter thrombosis: comparison of the antithrombotic activities of fondaparinux, enoxaparin, and heparin in vitro and in vivo. Blood. 2011;118(25):6667–74.
Füreder L, Böhmig GA, Schaefer AK, Steinlechner B. Extracorporeal immunoadsorption in heparin- and protamine-induced thrombocytopaenia prior to cardiac surgery. Eur J Cardiothorac Surg. 2019;56(1):206–7.
Warkentin TE. Heparin-induced thrombocytopenia in critically ill patients. Semin Thromb Hemost. 2015;41:49–60.
Dunning J, Versteegh M, Fabbri A, Pavie A, Kolh P, Lockowandt U, et al. Guideline on antiplatelet and anticoagulation management in cardiac surgery. Eur J Cardiothorac Surg. 2008;34:73–92.
Wang JH, Cao FL, Huang YL. Inhibitory effect of irbesartan on restenosis after balloon angioplasty and mechanism thereof: experiment with rabbits. Zhonghua Yi Xue Za Zhi. 2006;86(34):2395–8.
Lauth M, Cattaruzza M, Hecker M. ACE inhibitor and AT1 antagonist blockade of deformation-induced gene expression in the rabbit jugular vein through B2 receptor activation. Arterioscler Thromb Vasc Biol. 2001;21(1):61–6.
Ghigliotti G, Mereto E, Eisenberg PR, Martelli A, Orsi P, Sini D, et al. N-acetyl-cysteine reduces neointimal thickening and procoagulant activity after balloon-induced injury in abdominal aortae of New Zealand white rabbits. Thromb Haemost. 2001;85(4):724–9.
Chang CC, Chichareon P, Modolo R, Takahashi K, Kogame N, Tomaniak M, et al. Association between post-percutaneous coronary intervention bivalirudin infusion and net adverse clinical events: a post hoc analysis of the GLOBAL LEADERS study. Eur Heart J Cardiovasc Pharmacother. 2019. https://doi.org/10.1093/ehjcvp/pvz051.
Funding
The authors received no financial support for the research or authorship of this article.
Author information
Authors and Affiliations
Contributions
Concept—PA and TG; design—TG and BK; supervision—SB, BK, PA, and MB; resource—CB; materials—TG; data collection and/or processing—TG and CE; analysis—CE and CB; literature search—TG, MB, and CB; writing—TG and BK; critical review—CB; other—PA. All authors approved the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Gencpinar, T., Bayrak, S., Bilen, C. et al. Effect of bivalirudin on neointimal hyperplasia and endothelial proliferation in rabbit. Gen Thorac Cardiovasc Surg 69, 425–433 (2021). https://doi.org/10.1007/s11748-020-01454-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11748-020-01454-8