Abstract
Purpose
The aim of this study was to extract predictive factors of prolonged air leak (PAL) including air flow data as objective parameter by digital drainage system (DDS).
Methods
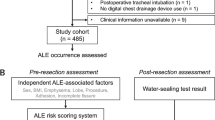
The 372 patients who underwent lung resection and had continuous log data of air flow by DDS were reviewed. PAL was defined as the air leak which was exceeding 20 ml/min and lasting 5 days or more. The 69 patients (18.5%) showed air leak and were divided into PAL group (n = 21) and non-PAL group (n = 48). The average flow per hour was calculated at 0, 12, and 24 postoperative hours (POH) and the residual ratio of flow at 12, 24, and 36 POH to that at the time after surgery was analyzed with clinical factors. Area under the receiver-operating characteristic curve (ROC-AUC) was calculated to determine optimal cut-off value of PAL predictors.
Results
ROC-AUC for flow at 36 POH was 0.88. Sensitivity and specificity were 0.91 and 0.73 when cut-off value was set at 20 mL/min at 36 POH. ROC-AUC for residual ratio at 36 POH was 0.82. Sensitivity and specificity were 0.81 and 0.79 when cut-off value of residual ratio was set at 0.20.
Conclusions
The air flow and the residual ratio measured by DDS will be useful predictors of postoperative PAL after lung resection.



Similar content being viewed by others
References
Cerfolio RJ, Bass CS, Pask AH, Katholi CR. Predictors and treatment of persistent air leaks. Ann Thorac Surg. 2002;73:1727–30. (discussion 30–1).
Brunelli A, Varela G, Refai M, Jimenez MF, Pompili C, Sabbatini A, et al. A scoring system to predict the risk of prolonged air leak after lobectomy. Ann Thorac Surg. 2010;90:204–9.
Orsini B, Baste JM, Gossot D, Berthet JP, Assouad J, Dahan M, et al. Index of prolonged air leak score validation in case of video-assisted thoracoscopic surgery anatomical lung resection: Results of a nationwide study based on the French national thoracic database, epithor. Eur J Cardiothorac Surg. 2015;48:608–11.
Attaar A, Winger DG, Luketich JD, Schuchert MJ, Sarkaria IS, Christie NA, et al. A clinical prediction model for prolonged air leak after pulmonary resection. J Thorac Cardiovasc Surg. 2016. https://doi.org/10.1016/j.jtcvs.2016.10.003.
Varela G, Jimenez MF, Novoa NM, Aranda JL. Postoperative chest tube management: Measuring air leak using an electronic device decreases variability in the clinical practice. Eur J Cardiothorac Surg. 2009;35:28–31.
Bertolaccini L, Rizzardi G, Filice MJ, Terzi A. ‘Six sigma approach’—an objective strategy in digital assessment of postoperative air leaks: a prospective randomised study. Eur J Cardiothorac Surg. 2011;39:e128-32.
Petrella F, Rizzo S, Radice D, Borri A, Galetta D, Gasparri R, et al. Predicting prolonged air leak after standard pulmonary lobectomy: computed tomography assessment and risk factors stratification. Surgeon. 2011;9:72–7.
Pompili C, Brunelli A, Salati M, Refai M, Sabbatini A. Impact of the learning curve in the use of a novel electronic chest drainage system after pulmonary lobectomy: A case-matched analysis on the duration of chest tube usage. Interact Cardiovasc Thorac Surg. 2011;13:490–3. (discussion 93).
Brunelli A, Salati M, Pompili C, Refai M, Sabbatini A. Regulated tailored suction vs regulated seal: a prospective randomized trial on air leak duration. Eur J Cardiothorac Surg. 2013;43:899–904.
Miller DL, Helms GA, Mayfield WR. Digital drainage system reduces hospitalization after video-assisted thoracoscopic surgery lung resection. Ann Thorac Surg. 2016;102:955–61.
Shoji F, Takamori S, Akamine T, Toyokawa G, Morodomi Y, Okamoto T, et al. Clinical evaluation and outcomes of digital chest drainage after lung resection. Ann Thorac Cardiovasc Surg 2016;22:354–58. (advpub).
Attaar A, Winger DG, Luketich JD, Schuchert MJ, Sarkaria IS, Christie NA, et al. A clinical prediction model for prolonged air leak after pulmonary resection. J Thorac Cardiovasc Surg. 2017;153:690–99 e2.
Rivera C, Bernard A, Falcoz PE, Thomas P, Schmidt A, Benard S, et al. Characterization and prediction of prolonged air leak after pulmonary resection: a nationwide study setting up the index of prolonged air leak. Ann Thorac Surg. 2011;92:1062–8. (discussion 68).
Brunelli A, Cassivi SD, Salati M, Fibla J, Pompili C, Halgren LA, et al. Digital measurements of air leak flow and intrapleural pressures in the immediate postoperative period predict risk of prolonged air leak after pulmonary lobectomy. Eur J Cardiothorac Surg. 2011;39:584–8.
Bille A, Borasio P, Gisabella M, Errico L, Lausi P, Lisi E, et al. Air leaks following pulmonary resection for malignancy: risk factors, qualitative and quantitative analysis. Interact Cardiovasc Thorac Surg. 2011;13:11–5.
Takamochi K, Imashimizu K, Fukui M, Maeyashiki T, Suzuki M, Ueda T, et al. Utility of objective chest tube management after pulmonary resection using a digital drainage system. Ann Thorac Surg. 2017;104:275–83.
Pompili C, Detterbeck F, Papagiannopoulos K, Sihoe A, Vachlas K, Maxfield MW, et al. Multicenter international randomized comparison of objective and subjective outcomes between electronic and traditional chest drainage systems. Ann Thorac Surg. 2014;98:490–6. (discussion 96–7).
Ciccone AM, Meyers BF, Guthrie TJ, Davis GE, Yusen RD, Lefrak SS, et al. Long-term outcome of bilateral lung volume reduction in 250 consecutive patients with emphysema. J Thorac Cardiovasc Surg. 2003;125:513–25.
Funding
This research received no specific grant from any funding agency in the public, commercial or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest to declare.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Goto, M., Aokage, K., Sekihara, K. et al. Prediction of prolonged air leak after lung resection using continuous log data of flow by digital drainage system. Gen Thorac Cardiovasc Surg 67, 684–689 (2019). https://doi.org/10.1007/s11748-019-01073-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11748-019-01073-y