Abstract
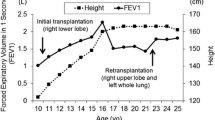
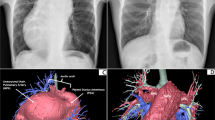
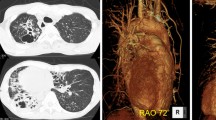
Pediatric pulmonary hypertension after surgery for congenital heart disease is a significant complication. We present a case of living-donor lung transplantation for a 12-year-old girl with pulmonary hypertension after surgical repair of transposition of great arteries. Despite repairing the transposition of great arteries, her growth was severely restricted because of progressive pulmonary hypertension; thus, lung transplantation was discussed. Standard bilateral lobar transplantation seemed unfeasible due to oversized grafts, so we performed a single lobar transplantation. Unexpectedly, she developed complications and died 3 months postoperatively despite another emergent lobar transplantation. We discussed the challenges and potential solutions regarding lobar size mismatching.


Similar content being viewed by others
References
Shiina Y, Toyoda T, Kawasoe Y, Tateno S. Prevalence of adult patients with congenital heart disease in Japan. Int J Cardiol. 2011;146:13–6.
Rafael A-G, Carmen L-G, Maria S-D, Ruiz J, Gonzalez I, Cubero J, et al. Pulmonary hypertension and congenital heart disease: an insight from the REHAP National Registry. Int J Cardiol. 2015;184:717–23.
Cordina R, Celermajer D. Late-onset pulmonary arterial hypertension after a successful atrial or arterial switch procedure for transposition of the great arteries. Pediatr Cardiol. 2010;31:238–41.
Date H, Aoyama A, Hijiya K, Motoyama H, Handa T, Kinoshita H, et al. Outcomes of various transplant procedures (single, sparing, inverted) in living-donor lobar lung transplantation. J Thorac Cardiovasc Surg. 2017;153:479–86.
Zijlstra WMH, Elmasry O, Pepplinkhuizen S, Ivy DD, Bonnet D, Luijendijk P, et al. Pulmonary arterial hypertension in children after neonatal arterial switch operation. Heart. 2017;103:1244–9.
Watanabe T, Adachi O, Suzuki Y, Notsuda H, Niikawa H, Matsuda Y, et al. Lung transplant for pulmonary arterial hypertension after arterial switch operation. Ann Thorac Surg. 2015;100:e133-4.
Toyooka S, Kusano KF, Goto K, Masaomi Y, Oto T, Sano Y, et al. Right but not left ventricular function recovers early after living-donor lobar lung transplantation in patients with pulmonary arterial hypertension. J Thorac Cardiovasc Surg. 2009;138:222–6.
Aguilar PR, Bemiss BC, Witt C, Byers DE, Kreisel D, Puri V, et al. Impact of delayed chest closure on surgical site infection after lung transplantation. Ann Thorac Surg. 2017;104:1208–14.
Weill D, Benden C, Corris PA, Dark JH, Davis RD, Keshavjee S, et al. A consensus document for the selection of lung transplant candidates: 2014—an update from the Pulmonary Transplantation Council of the International Society for Heart and Lung Transplantation. J Hear Lung Transpl. 2015;34:1–15.
Miyoshi K, Oto T, Okazaki M, Yamane M, Toyooka S, Goto K, et al. Extracorporeal membrane oxygenation bridging to living-donor lobar lung transplantation. Ann Thorac Surg. 2009;88:e56-7.
Shimada A, Terada J, Tsushima K, Tateishi Y, Abe R, Oda S, et al. Veno-venous extracorporeal membrane oxygenation bridged living-donor lung transplantation for rapid progressive respiratory failure with pleuroparenchymal fibroelastosis after allogeneic hematopoietic stem cell transplantation. Respir Investig. 2018;56:258–62.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Yoshinaga, D., Baba, S., Hirata, T. et al. Living-donor lung transplantation after surgical repair of transposition of the great arteries. Gen Thorac Cardiovasc Surg 67, 640–643 (2019). https://doi.org/10.1007/s11748-018-1006-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11748-018-1006-y