Abstract
We recently showed that a hypocaloric carbohydrate restricted diet (CRD) had two striking effects: (1) a reduction in plasma saturated fatty acids (SFA) despite higher intake than a low fat diet, and (2) a decrease in inflammation despite a significant increase in arachidonic acid (ARA). Here we extend these findings in 8 weight stable men who were fed two 6-week CRD (12%en carbohydrate) varying in quality of fat. One CRD emphasized SFA (CRD-SFA, 86 g/d SFA) and the other, unsaturated fat (CRD-UFA, 47 g SFA/d). All foods were provided to subjects. Both CRD decreased serum triacylglycerol (TAG) and insulin, and increased LDL-C particle size. The CRD-UFA significantly decreased plasma TAG SFA (27.48 ± 2.89 mol%) compared to baseline (31.06 ± 4.26 mol%). Plasma TAG SFA, however, remained unchanged in the CRD-SFA (33.14 ± 3.49 mol%) despite a doubling in SFA intake. Both CRD significantly reduced plasma palmitoleic acid (16:1n-7) indicating decreased de novo lipogenesis. CRD-SFA significantly increased plasma phospholipid ARA content, while CRD-UFA significantly increased EPA and DHA. Urine 8-iso PGF2α, a free radical-catalyzed product of ARA, was significantly lower than baseline following CRD-UFA (−32%). There was a significant inverse correlation between changes in urine 8-iso PGF2α and PL ARA on both CRD (r = −0.82 CRD-SFA; r = −0.62 CRD-UFA). These findings are consistent with the concept that dietary saturated fat is efficiently metabolized in the presence of low carbohydrate, and that a CRD results in better preservation of plasma ARA.
Similar content being viewed by others
Introduction
The rationale for using carbohydrate-restricted diets (CRD) in an experimental setting is that dietary carbohydrate is the major stimulus of the glucose-insulin axis which, in turn has profound effects on several metabolic processes. The shift away from an anabolic state leads to an increase in fat oxidation thereby altering lipoprotein metabolism and cardio-metabolic profile [1]. Low carbohydrate diets consistently decrease fasting and postprandial plasma triacylglycerol (TAG), increase HDL-cholesterol (HDL-C), lower plasma insulin, and improve insulin sensitivity [2]. While LDL-cholesterol (LDL-C) responses are more variable, there is a consistent shift from small to larger particles [3]. These responses to carbohydrate restriction have been shown to occur in isocaloric experiments [4–6] indicating that the effects are not solely due to weight loss.
In our previous study of overweight men and women consuming a hypocaloric CRD, one of the most striking responses was a significantly greater reduction in plasma SFA levels in response to a CRD compared to a low fat diet, despite a threefold greater presence of dietary SFA in the carbohydrate-reduced diet [7]. Control of lipid metabolism, particularly SFA availability, is of current interest because of a recent meta-analysis showing that dietary SFA is not a risk factor for cardiovascular disease [8] and the indication that replacement by carbohydrate, in particular, may increase risk [9]. The extent to which plasma SFA reflects dietary saturated fat consumption is not clear-cut and is significantly affected by the presence of carbohydrate [3, 7]. Cassady et al. [10], for example, found that plasma palmitic and stearic acids did not depend on the saturated fat content of two different CRD. Two other studies reported lower plasma levels of SFA in response to diets that contained two to threefold greater intake of SFA but were lower in carbohydrate than standard intakes [11, 12].
The other remarkable finding in our previous investigation was a significant decrease in inflammatory markers despite a marked increase in plasma arachidonic acid (ARA) [7]. The metabolic intermediates in the production of ARA were decreased suggesting that synthesis was not increased. We proposed rather that the increase was due to better preservation of ARA. This idea was supported indirectly by the observation of significant reductions in several inflammatory cytokines that were also inversely correlated with changes in ARA. The ratio of n-6 to n-3 highly unsaturated fatty acids in phospholipids (PL) has received significant attention due to their conversion to eicosanoids of different biologic effects. The n-6 ARA (20:4n-6) more readily promotes inflammation when converted enzymatically or non-enzymatically to pro-inflammatory eicosanoids and F2-isoprostanes [13, 14], whereas an increase in membrane eicosapentaenoic acid (EPA; 20:5n-3), an n-3 PUFA has anti-inflammatory effects and decreases risk of cardiovascular disease [15, 16]. Increasing ARA in membranes, however, does not inevitably lead to greater inflammation and may in fact have the opposite effect [15, 17]. The proinflammatory effects of ARA are due to metabolites produced subsequent to its release from membranes rather than the proportion of the intact fatty acid. Enzymatic metabolism of free ARA results in production of eicosanoids, and free radical-induced peroxidation of ARA results in the formation of isoprostanes. Measurement of isoprostanes is considered an accurate marker of oxidative stress, but it also represents a unique non-enzymatic degradation product of ARA [18].
Here, we extend the findings of our previous study by assessing plasma fatty acid composition responses in men who participated in two 6-week weight maintenance CRD feeding periods varying only in fatty acid composition. One CRD was designed to be high in SFA (emphasizing dairy fat and eggs), and the other was designed to be lower in saturated fat and consequently higher in unsaturated fat from both polyunsaturated (PUFA) and monounsaturated (MUFA) fatty acids (emphasizing fish, nuts, omega-3 enriched eggs, and olive oil). The objectives were to: (1) establish whether the disconnect between dietary and plasma SFA levels persists under isocaloric conditions, (2) determine if a weight stable CRD increases plasma ARA and the association with inflammatory markers and isoprostanes, and (3) determine whether an increase in dietary EPA and docosahexaenoic acid (DHA; 22:6n-3) on a CRD mitigates the increase in plasma ARA and its association with inflammatory markers and isoprostanes.
Experimental Procedures
Study Participants
Eight men, aged 38–58 years old, with BMI of 25–35 kg/m2 participated in this controlled dietary intervention. Medical history, family history, and dietary intake from a 3 day diet record were collected at baseline. Exclusion criteria were abnormal glucose levels, hypercholesterolemia, a diagnosis of Type I or II diabetes, liver or other metabolic or endocrine dysfunction, hypertension, or use of cholesterol or diabetic medications. Subjects were also excluded if they were taking any supplements known to affect serum lipoprotein levels (i.e. fish oil, niacin, psyllium fiber) or inflammation (i.e. aspirin). Subjects were not excluded if they were already following a CRD, but were excluded if they were trying to lose weight or had a body mass that changed ±3 kg in the last 3 months. Subjects were asked to maintain their same activity level during the experimental period (verified by activity records) and sedentary individuals were not allowed to start a new exercise program in order to account for possible confounding effects on the dependant variables.
Study Design and Dietary Intervention
In a randomized, cross-over, controlled design, an isocaloric carbohydrate restricted high saturated fat diet (CRD-SFA) was compared to a CRD higher in unsaturated fat (CRD-UFA). Each dietary feeding period was 6 weeks in duration, based on previous research showing that the fatty acid composition of plasma PL stabilizes within 4–6 weeks of dietary change [19] and blood lipids stabilize within 6 weeks of a CRD [20]. Three weeks prior to starting each of the 6 week dietary feeding periods, all subjects were counseled to consume a run-in free-living weight-maintaining CRD (~10%en from carbohydrate, 65%en from fat, and 25%en from protein), using standardized procedures from our research laboratory. The purpose of this run-in period was to: aide in determining an appropriate energy level to maintain body weight; standardize subject’s physiologic state before each diet; and initiate metabolic adaptations to carbohydrate restriction. Urinary ketones were monitored throughout the entire CRD run-in period and intervention using reagent strips (Bayer Corporation, Elkart, IN) to ensure compliance and to assure the presence of nutritional ketosis. After the run-in period, subjects were randomized to one of two dietary arms as described above. Following the 6 week feeding period, subjects returned to their individual baseline diet for 4 weeks. Once washed out, they returned to the same run-in CRD for another 3 weeks, and then crossed over to the next 6 week controlled CRD feeding arm.
Dietary energy for each subject was prescribed to maintain body weight, estimated using the Harris-Benedict equation and multiplied by an activity factor from 1.2 to 1.55 depending on individual activity level. This was averaged with their caloric intake during their baseline dietary intake and run-in CRD period. Composition of the experimental diets was developed using nutrient analysis software consisting of normal foods that differed only in the relative amount of saturated and unsaturated fatty acids, but were matched for food type, energy, total fat, dietary fiber, trans fat, and cholesterol (Food Processor 7.71, ESHA Research, Salem, OR). Validation of the daily nutrient composition was confirmed by chemical analysis (Covance Inc, Princeton, NJ). Table 1 shows the average nutrient intake for 3 days of the 7-day rotational menu via chemical analysis. A daily multi-vitamin and mineral supplement at levels ≥100% of the RDA was also given to subjects and consumed throughout the entire intervention to ensure adequate micronutrient status.
In each 6-week feeding period, all food and beverages were provided for subjects in a 7-day rotational menu, and no other foods or beverages were allowed, unless they were calorie-free or very-low-calorie (i.e., tea, water, diet soda). Predominant foods in the CRD-SFA were high-fat dairy (cream, butter, cheese, and low-carbohydrate milk), eggs, meat, poultry, and white fish, and a few low omega-3 nuts and seeds (such as almonds). In the CRD-UFA, predominant foods were liquid omega-3 PUFA eggs (Egg Creations, Burnbrae Farms Ltd, ON, Canada. Containing EPA, DPA and DHA), hard shell omega-3 eggs (high in ALA and DHA), salmon, sardines, meat, poultry, olive oil, canola oil, low-fat low-carbohydrate dairy, walnuts, and seeds. Subjects picked up prepared, packaged food every Monday, Wednesday and Friday. All take-out food containers were returned unwashed and inspected to ensure that all food and fat had been consumed.
Anthropometrics
Body weight was measured weekly in the morning before food consumption and maintained within ±2 kg during the dietary intervention. Adjustments in caloric intake were made to maintain body weight within these parameters. Body composition was measured by dual-energy X-ray absorptiometry (Prodigy, Lunar Corporation, Madison, WI) at baseline, and at the start and end of each diet feeding intervention. Analyses were performed by the same blinded technician.
Blood Collection and Analysis
Blood samples were obtained at baseline, pre-dietary intervention and post-dietary intervention for both feeding periods. The sample was obtained from an arm vein after subjects rested quietly for 10 min in the supine position. Whole blood was collected into tubes with no preservative or EDTA and centrifuged at 1,500×g for 15 min and 4 °C, and promptly aliquoted into separate storage tubes which were stored at −75 °C until analyzed. A portion of serum (~3 ml) was immediately sent to a certified medical laboratory (Quest Diagnostics, Wallingford, CT) for determination of total cholesterol (TC), HDL-C, TAG, and calculated LDL-C concentrations using automated enzymatic procedures (Olympus America Inc., Melville, NY).
Glucose and insulin concentrations were analyzed in serum in duplicate (YSI 2300 STAT, Yellow Springs, OH, CV 0.5%) and radioimmunoassay (Diagnostic Systems Laboratory, Webster, TX, CV 4.3%), respectively, and used to calculate an index of insulin resistance [HOMA-IR; calculated as Glucose (mmol/l) Insulin (μIU/ml/22.5)]. The 75th percentile cut-off value for insulin resistance in non-diabetic individuals has been determined to correspond to a value of 2.29 [17]. Lipoprotein particle size of LDL-C was determined in serum using non-gradient polyacrylamide gel electrophoresis (Lipoprint LDL System, Quantimetrix Co., Redondo Beach, CA) as previously described [21]. Serum total ketone bodies were determined by a cyclic enzymatic method that measures both acetoacetate (AcAc) and 3-hydroxybutyrate (3-HB) (Wako Chemicals USA Inc, Richmond, VA). Absorbance was read at a wavelength of 404 nm on a microplate reader (Versa Max Molecular Devices Corp. Sunnyvale, CA, USA) and analyzed with associated SoftMax Pro software (CV 4.2%). Serum IL-6, IL-8, MCP-1, TNF-α, and leptin were measured using xMAP® technology on a Luminex® IS 200 system with antibodies to these analytes from LINCO Research (St. Charles, MO). Assays were completed in duplicate according to manufacturer’s instructions (IL-6 CV 12.7%, IL-8 CV 10.4%, MCP-1 CV 7.3%, TNF-α CV 9.7%, Leptin CV 10.2%). High Sensitivity C-reactive protein (hs-CRP) was determined in serum on an IMMULITE Automated Analyzer using the commercially available immulite chemiluminescent enzyme immunometric assay (Immulite®, Diagnostic Products Corp., Los Angeles, CA, USA).
A 24-h urine collection was performed at baseline and post-dietary intervention. A 10-ml aliquot of urine was stored at −75 °C for subsequent analysis of F2-Isoprostane (8-iso PGF2α) concentrations. All samples were analyzed in triplicate using column extraction followed by an ACETM Competitive Enzyme Immunoassay with 8-Isoprostane enzyme-linked immunosorbent assay (EIA) kit (Cayman Chemicals, Ann Arbor, MI). Briefly, 2 ml frozen thawed urine was purified through an 8-Isoprostane Affinity Column (Caymen Chemicals), washed with column buffer and ultra pure water, and eluted with ethanol:water (95:5). Elution was dried with nitrogen; the volume of the dried sample was brought to 2 ml with enzyme immunoassay buffer in a 1:10 dilution. Absorbance was read at 420 nm and data was analyzed with a log-logit curve fit (CV 5.7%). The results were expressed relative to creatinine concentrations determined using Jaffe’s colorimetric method (Cayman Chemicals) read at an absorbance of 490 nm (CV 3.2%).
Fatty Acid Composition
Plasma was shipped on dry ice to Lipid Technologies LLC (Austin, MN) and analyzed for plasma fatty acid composition in circulating PL, TAG and CE using capillary gas chromatography as previously described [7]. Lipids were extracted according to the method of Bligh/Dyer whereby mixtures of plasma, methanol, chloroform and water were prepared such that lipid is recovered in a chloroform layer. The resulting lipid extracts were maintained under an atmosphere of nitrogen following extraction and kept frozen prior to additional processing. Immediately prior to lipid class separation, lipid samples were dried under a gentle stream of nitrogen, rediluted in 50 μl of chloroform and prepared for lipid class separation. Lipid classes were separated on commercial silica gel G plates (AnalTech, Newark, DE). The chromatographic plates were developed in a solvent system consisting of distilled petroleum ether (b.p.30–60 °C): diethyl ether: acetic acid (80:20:1, by vol). Following development, the silica gel plates were sprayed with a methanolic solution containing 0.5% 2,7-dichlorofluorescein which was then used to visualize lipid classes under ultraviolet light. Desired corresponding lipid bands were then scraped into Teflon-lined screw cap tubes. The samples were then transesterified with boron trifluoride (10%) in excess methanol (Supelco, Bellefonte, PA) in an 80 °C water bath for 90 min. Resulting fatty acid methyl esters were extracted with water and petroleum ether and stored frozen until gas chromatographic analysis was performed.
Lipid class fatty acid methyl ester composition was determined by capillary gas chromatography. Methyl ester samples were blown to dryness under nitrogen and resuspended in hexane. Resulting fatty acid methyl esters were separated and quantified with a Shimadzu capillary gas chromatograph (GC17) utilizing a 30 m Restek free fatty acid phase (FFAP) coating and EZChrom software. The instrument temperature was programmed from 190 to 240° at 7 °C/min with a final hold of 10 min, separating and measuring fatty acid methyl esters ranging from 12:0 to 24:1. The detector temperature was 250 °C. Helium carrier gas was used at a flow rate of 1.4 ml/min. and a split ratio of 1:25. Chromatographic data was collected and processed with EZChrom software (Scientific Products, CA). Fatty acids were identified by comparison to authentic fatty acid standards and quantitated with peak area and internal standard. Individual peaks, representing as little as 0.05% of the fatty acid methyl esters, were distinguished. Fatty acid data are expressed in relative (mol%) and absolute (nmol/ml) terms.
Statistics
ANOVA with repeated measures was used to evaluate changes from baseline across diets. Data that was not normally distributed was log transformed. Significant main effects were further analyzed using a Tukey post hoc test. Differences between values following CRD-SFA and CRD-UFA were evaluated using paired student’s t test. The alpha level for significance was <0.05.
Results
Dietary Intake
Nutrient intake estimated at baseline from dietary records showed a lower than expected energy, 2,072 kcal/d compared to 2,513 kcal/d for the feeding periods. This was likely due to under-reporting at baseline (Table 1) [22] although it has been argued that the demands of gluconeogenesis and other processes require more energy for weight maintenance [23]. Habitual carbohydrate intake was also lower than the average American diet at 32%en reflecting two subjects who were habitually consuming a lower-carbohydrate diet. Both CRD were well tolerated and compliance was excellent as assessed by verbal feedback and inspection of returned food containers throughout the intervention. There was no consistent preference for one diet treatment over the other by subjects. Briefly, the main difference between the two low carbohydrate diets was in the relative amount of SFA, MUFA, PUFA (CRD-SFA = 31, 21, and 5%; CRD-UFA = 17, 25, and 15%). Although the CRD-UFA contained higher amounts of both n-6 and n-3 PUFA, the ratio of n-6/n-3 PUFA was lower in the CRD-UFA. Other nutrients, including cholesterol, were matched with the exception of (naturally occurring) trans fatty acids which were inherently higher on the CRD-SFA diet due to the higher intake of high-fat dairy. Compared to baseline, the CRD-SFA diet provided more than twice as much dietary SFA (86 vs. 40 g) while in the CRD-UFA, intake of SFA was 47 grams. Compared to baseline, the CRD-UFA provided more total PUFA (41 vs. 16 g), n-3 PUFA (3%en vs. 0.7%en), and n-6 PUFA (11%en vs. 7%en). Cholesterol intake in both diets was about twofold higher than baseline intake.
Body Weight and Composition
Body fat percentage and body mass of subjects after the two experimental diets were not significantly different from baseline. A small, but significant (P < 0.05) decrease in body mass (difference: 0.94 ± 0.13 kg) occurred following the CRD-UFA diet compared to the CRD-SFA diet (Table 2).
Blood Markers
Blood lipid, metabolic, and inflammatory markers are presented in Table 2. Serum ketones were moderately elevated as a result of carbohydrate restriction. Fasting plasma TC and LDL-C were variable but were higher on average following CRD-SFA compared to CRD-UFA. The increase in HDL-C following CRD-SFA (14%) and CRD-UFA (8%) from baseline resulted in no significant change in the TC/HDL or LDL/HDL ratios.
Consistent with numerous studies on CRD even in the absence of weight loss, a dramatic decrease in plasma TAG was seen. TAG fell from baseline by 39% after the CRD-SFA and by 34% on the CRD-UFA. There was also a decrease in TAG/HDL ratio for both the CRD-SFA (−39%) and CRD-UFA (−43%). LDL mean and peak particle size following the two diets were both significantly higher than baseline.
Blood glucose, insulin, and HOMA-IR were not significantly different from baseline or between diets. Using 2.29 as the cut-off point to define insulin resistance [21], two subjects were insulin resistant (HOMA-IR = 3.06 and 5.53) at baseline. HOMA-IR values were <2.29 for both subjects after the CRD-UFA and for one of the insulin resistant subjects after the CRD-SFA.
There were no significant differences in any of the serum inflammatory markers (hs-CRP, IL-6, IL-8, TNF-α, MCP-1, leptin) between the two interventions. Compared to baseline levels of urinary 8-iso PGF2α (629 ± 262 pg/Creatinine mg), concentrations were reduced by 17% after the CRD-SFA (524 ± 146 pg/Creatinine mg; P = 0.253) and by 32% after the CRD-UFA (425 ± 61 pg/Creatinine mg; P = 0.018). After the CRD-UFA, all 8 subjects had lower urine 8-iso PGF2α than baseline and 7 out of 8 had lower concentrations compared to the CRD-SFA.
Plasma Saturated and Monounsaturated Fatty Acids
The major changes in plasma SFA and MUFA were in the plasma TAG fraction. The mol% of total SFA in TAG was significantly lower following CRD-UFA compared to CRD-SFA (Table 3). At the same time, the effect was less than might be expected given the nearly two-fold difference in dietary saturated fat suggesting that the reduction in carbohydrate was the major determinant; there was, in fact, no difference in total SFA in TAG between baseline and CRD-SFA. The lower total SFA after the CRD-UFA was mainly attributed to a decrease in 16:0, the predominant SFA in plasma TAG although, again, the magnitude of the effect was small. Compared to baseline, 16:1n-7 mol% in plasma TAG was significantly lower following both CRD, but not different between CRD. A comprehensive list of fatty acids from TAG, PL and CE fractions is provided in Table 3.
Plasma Polyunsaturated Fatty Acids
The major changes in plasma PUFA were in the PL fraction. There were distinct differences between the CRD in plasma PL long chain n-6 and n-3 PUFA (Table 3). Compared to baseline, all subjects had an increase in 20:4n-6 after the CRD-SFA, and those values were higher than 20:4n-6 after the CRD-UFA in all but one subject. Interestingly, despite an increase in 20:4n-6 in response to the CRD-SFA the immediate precursor 20:3n-6 was not increased and was in fact lower than baseline. Total n-3 PUFA was significantly higher following the CRD-UFA than baseline and CRD-SFA values primarily due to greater increases in 20:5n-3 (EPA) and 22:6n-3 (DHA). The PL n-6/n-3 ratio (calculated as the sum of all n-6 PUFA divided by the sum of all n-3 PUFA), was significantly lower following CRD-UFA than CRD-SFA and baseline. Compared to baseline, the ARA/EPA ratio was significantly increased after the CRD-SFA whereas it was decreased after the CRD-UFA. Compared to baseline the ARA/EPA ratio was decreased after the CRD-UFA in all subjects, and it was higher during the CRD-SFA than the CRD-UFA in all subjects.
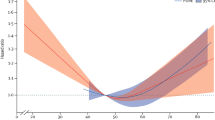
Intuitively, one might presume an increase in PL ARA would result in a corresponding increase in 8-iso PGF2α, yet we observed the opposite. There was a significant inverse correlation between changes in urine 8-iso PGF2α and PL ARA on both low carbohydrate diets (r = −0.82 CRD-SFA, P = 0.007; r = −0.62 CRD-UFA, P = 0.05) indicating that those subjects who showed greater increases in plasma ARA had greater reductions in 8-iso PGF2α.
Discussion
Dietary saturated fat has been the focus of nutritional recommendations since the 1970 study of Ancel Keys [24]. Current recommendations are as low as 7% [25] although the subject has always generated some controversy. The biologic effect of dietary SFA is presumed to rest with its effect on plasma SFA and other lipid fractions but a number of reports in the literature suggest that this needs to be experimentally established [7, 11, 12]. In the current study, we used a controlled-feeding design to examine responses in plasma fatty acids, lipoproteins, isoprostanes and inflammatory markers in men who switched from their habitual diet to a CRD either high in SFA (CRD-SFA) or unsaturated fat (CRD-UFA) including eggs with long chain n-3 PUFA. The primary findings were that: (1) there is limited effect of dietary SFA on plasma SFA in the context of a weight maintenance low carbohydrate diet, (2) a weight maintenance CRD high in SFA (representing the typical nutrient composition of CRD we have studied in our many previous investigations) resulted in a significant increase in plasma ARA without an accompanying increase in inflammation or oxidative stress, (3) a weight maintenance CRD higher in unsaturated fat (CRD-UFA) including EPA and DHA (CRD-UFA) prevented the increase in plasma ARA while increasing plasma EPA and DHA content and significantly decreasing urine 8-iso PGF2α, a degradation breakdown product of ARA, and, (4) the changes in plasma ARA and urine 8-iso PGF2α were inversely correlated on both CRD independent of fat composition supporting and strengthening our hypothesis of less catabolism of ARA (i.e., better preservation of ARA) on a CRD.
Saturated Fat
The most striking finding was the lack of association between dietary SFA intake and plasma SFA concentrations. Compared to baseline, a doubling of saturated fat intake on the CRD-SFA did not increase plasma SFA in any of the lipid fractions, and when saturated fat was only moderately increased on the CRD-UFA, the proportion of SFA in plasma TAG was reduced from 31.06% to 27.48 mol%. Since plasma TAG was also reduced, the total SFA concentration in plasma TAG was decreased by 47% after the CRD-UFA, similar to the 57% decrease we observed in overweight men and women after 12 week of a hypocaloric CRD [7]. These results can best be explained by the metabolic adaptations induced by carbohydrate restriction [1], notably less stimulation of insulin. Lower insulin levels result in increased lipolysis and fatty acid oxidation while simultaneously decreasing activity of key enzymes in de novo lipogenesis. From a mechanistic standpoint, restriction in dietary carbohydrate is the dominant dietary manipulation that accelerates fat mobilization and oxidation [26]. The lipid fraction most responsive to carbohydrate restriction was TAG. Higher incorporation of SFA into VLDL TAG is correlated with insulin resistance and adiposity [27], probably reflecting accelerated hepatic de novo lipogenesis. Plasma TAG transports the greatest amount of fatty acids that are actively involved in energy exchange. Therefore a decrease in plasma SFA, from reduced hepatic fatty acid synthesis or increased beta-oxidation, may attenuate atherogenic cell-signaling even in the presence of higher dietary SFA. The limited change in SFA in PL may be due to lower turnover in this fraction (the sn-1 position almost always carries a SFA), or to the short duration of this study. Previous studies have shown that increased plasma PL and CE SFA levels predict development of cardiovascular disease (CVD) [28, 29].
The presence of palmitoleic acid (16:1n-7) is an indicator of de novo fatty acid synthesis [30] since the compound is limited in the diet. Both isocaloric CRD feeding periods in this study significantly decreased TAG 16:1n-7, suggesting that similar reductions in our previous experiments using a hypocaloric CRD [3, 7], were a consequence of carbohydrate restriction rather than calorie reduction or weight loss. Lower 16:1n-7 also provides an explanation for the lack of association between dietary and plasma SFA since the 16:0 species is the primary product of fatty acid synthesis. Parallel reduction in 16:0 and 16:1n-7 suggests that stearoyl-CoA desaturase-1 (SCD-1), the enzyme responsible for desaturating 16:0, was not down-regulated independent of lipogenesis, since, in that case, the proportion of 16:0 would be expected to rise. Increased plasma levels of SFA and 16:1n-7 have been reported in obese adolescents [31] and adults with MetSyn [32] and higher 16:1n-7 is associated with increased abdominal obesity, lipogenesis, and hypertriglyceridemia [33, 34].
Highly Unsaturated Fatty Acids
The increase in PL ARA in weight stable men after the CRD-SFA (order of 2 units expressed as mol%) is similar to the previously reported effect in overweight men on a hypocaloric diet [7] indicating that the latter was not due to weight loss. Replacing SFA with unsaturated fat including n-3 PUFA prevented the increase in plasma ARA, and also resulted in a marked increase in plasma EPA and DHA, likely a result of higher dietary intake on the CRD-UFA (1.5 g vs. 0.4 g/day). Previous studies have shown close association between dietary EPA and DHA and plasma EPA and DHA [35]. Increased plasma ARA following CRD-SFA may have resulted from less competition from n-3 PUFA for preferential acyl incorporation into the sn-2 position of phospholipids [36]. Dietary intakes of ARA were high in both CRD-UFA and CRD-SFA. Competition among n-3 and n-6 PUFA at the level of desaturation and chain elongation steps of fatty acid biosynthesis may also be important.
An increase in phospholipid ARA mol% and PL ARA/EPA ratio is commonly viewed as contributing to a pro-inflammatory and pro-oxidative state. These effects following CRD-SFA, however, were not accompanied by elevation of any of the inflammatory markers or 8-iso PGF2α. Along these lines, a meta-analysis of 14 case–control and prospective cohort studies found that increased ARA in plasma PL or triglycerides was not associated with coronary events [37], while a recent case-controlled study of acute coronary syndrome (ACS) found a U-shaped relationship between odds ratio for ACS and erythrocyte ARA content [38]. Ferrucci L et al. [15] demonstrated and inverse relation between plasma ARA and pro-inflammatory markers, in agreement with the current study. A CRD that resulted in an increased ARA/EPA ratio also decreased C-reactive protein (CRP) [17]. A number of other studies have failed to link increased ARA in plasma lipids with deleterious outcomes [39–43]. The lack of association between plasma PL ARA and plasma PL ARA/EPA ratio and inflammation following CRD-SFA supports the idea that ARA in plasma membranes is not pro-inflammatory, especially in the context of low dietary carbohydrate. In fact, there was a trend (P < 0.08) for an anti-inflammatory effect on the adipocytokine leptin. Although leptin is not a classic cytokine, several immune cells (including polymorphonuclear leukocytes, monocytes, macrophages and lymphocytes) have leptin receptors and their activity can be modulated by leptin. Leptin has also been shown to stimulate production of ROS by activated monocytes in vitro [44]. Previous CRD investigations indicate significant reductions in response to a low carbohydrate diet even when normalizing for changes in body or fat mass [3].
The isoprostane 8-iso PGF2α is a free radical-catalyzed product of ARA measured as a general indicator of oxidative stress [18]. We found no change in 8-iso PGF2α after the CRD-SFA despite a significant increase in plasma ARA. Similarly, a significant decrease in 8-iso PGF2α was observed after the CRD-UFA where there was no change in plasma ARA. The inverse correlation between changes in plasma PL ARA and 8-iso PGF2α indicates better preservation of ARA in response to a CRD. The fat sources in this diet, olive oil and lipid from fish and liquid omega-3 eggs, may have contributed to lower urinary 8-iso PGF2α following CRD-UFA. Urinary excretion has been shown to be reduced by extra virgin olive oil [45], moderate fish oil supplementation (3.6 g/d n-3 PUFA), [46] and one daily fish meal (providing 3 g n-3 PUFA) reduced urinary F2-isoprostane levels in dyslipidemic non-insulin-dependent diabetic patients [47].
Insulin Resistance Syndrome
Saturated fatty acids are often implicated in the worsening of insulin resistance [48], but the effect is contingent upon the presence of ample carbohydrate. Carbohydrate restriction in the presence of high saturated fat leads to improvement in insulin sensitivity despite increased lipolytic rates and release of fatty acids into the circulation [49]. In the current study, the two subjects who had insulin resistance at baseline improved after restricting carbohydrate. The TAG/HDL-C ratio is strongly correlated with insulin resistance and levels >3.5 are indicative of increased CVD risk [50]. All subjects showed TAG/HDL-C values less than this value after the CRD consistent with the HOMA-IR results. Carbohydrate restrictions thus improved insulin sensitivity independent of dietary fatty acid composition. Many factors can influence serum cholesterol responses to saturated fat [51] including genetic variations [52] and the current study showed high variability in LDL-C. Independent of LDL-C concentration, however, individuals with a predominance of small LDL particles (pattern B) have >threefold risk of CVD [53]. In the current study, the variable LDL response was accompanied by uniform increase in LDL particle size.
Dietary Recommendations
The current findings further challenge the broad recommendation to restrict saturated fat especially since those calories are likely to be replaced with carbohydrate. The many factors that contribute to the relation of fat intake and fatty acid composition have been reviewed [54], and our results emphasize the substantial impact of a low carbohydrate intake in regulating the connection between dietary and plasma SFA. A higher saturated fat intake can be efficiently metabolized in the presence of low carbohydrate and lead to consistent improvements in markers of CVD risk. Whereas studies of benefits of carbohydrate restriction are rarely cited in the literature, responses of even a single meal high in saturated fat are taken as convincing evidence even if done in the presence of high carbohydrate. Ultimately, however, long term studies show that replacement of saturated fat with carbohydrate is at best neutral [55, 56]. Persistence of recommendations in the face of continued failure of large trials to show an effect of saturated fat remains one of the strange anomalies in current medical science.
Substitution of a portion of the SFA within a CRD with UFA including a combination of both MUFA and n-6 and n-3 PUFA had a profound effect on plasma fatty acid composition, reduced oxidative stress, but did not alter the positive effects on features of metabolic syndrome (e.g., insulin, TAG, LDL particle size). As low carbohydrate diets become more widely prescribed and used, it will be important to determine the range of dietary fatty acids most conducive to improving long-term health. Our results point to a suitable diet that had an emphasis on low carbohydrate foods with fat sources emphasizing MUFA and n-3 PUFA (e.g., omega-3 eggs, avocado, salmon, sardines, meat, poultry, olive oil, canola oil, nuts and seeds) although there was little if any detriment in a higher saturated fat approach.
Abbreviations
- ALA:
-
α-Linoleic acid
- ARA:
-
Arachidonic acid
- BMI:
-
Body mass index
- CRD:
-
Carbohydrate restricted diet
- CVD:
-
Cardiovascular disease
- CE:
-
Cholesteryl ester
- D6D:
-
Delta-6-desaturase
- DHA:
-
Docosahexaenoic acid
- EPA:
-
Eicosapentaenoic acid
- FM:
-
Fat mass
- hs-CRP:
-
High sensitivity C-reactive protein
- HOMA-IR:
-
Homeostasis model assessment insulin resistance index
- IL:
-
Interleukin
- LA:
-
Linoleic acid
- MCP-1:
-
Monocyte chemotactic protein-1
- MUFA:
-
Monounsaturated fatty acids
- MI:
-
Myocardial infarction
- NA:
-
Not available
- %en:
-
Percent total energy
- PUFA:
-
Polyunsaturated fatty acids
- TAG:
-
Triacylglycerol
- PL:
-
Phospholipid
- ROS:
-
Reactive oxygen species
- RDA:
-
Recommended daily allowance
- SFA:
-
Saturated fatty acids
- TNF-α:
-
Tumor necrosis factor-α
References
Volek JS, Fernandez ML, Feinman RD, Phinney SD (2008) Dietary carbohydrate restriction induces a unique metabolic state positively affecting atherogenic dyslipidemia, fatty acid partitioning, and metabolic syndrome. Prog Lipid Res 47:307–318
Volek JS, Feinman RD (2005) Carbohydrate restriction improves the features of metabolic syndrome. Metabolic syndrome may be defined by the response to carbohydrate restriction. Nutr Metab (Lond) 2:31
Volek JS, Phinney SD, Forsythe CE et al (2009) Carbohydrate restriction has a more favorable impact on the metabolic syndrome than a low fat diet. Lipids 44:297–309
Krauss RM, Blanche PJ, Rawlings RS, Fernstrom HS, Williams PT (2006) Separate effects of reduced carbohydrate intake and weight loss on atherogenic dyslipidemia. Am J Clin Nutr 83:1025–1031
Sharman MJ, Kraemer WJ, Love DM et al (2002) A ketogenic diet favorably affects serum biomarkers for cardiovascular disease in normal-weight men. J Nutr 132:1879–1885
Volek JS, Sharman MJ, Gomez AL, Scheett TP, Kraemer WJ (2003) An isoenergetic very low carbohydrate diet improves serum HDL cholesterol and triacylglycerol concentrations, the total cholesterol to HDL cholesterol ratio and postprandial lipemic responses compared with a low fat diet in normal weight, normolipidemic women. J Nutr 133:2756–2761
Forsythe CE, Phinney SD, Fernandez ML et al (2008) Comparison of low fat and low carbohydrate diets on circulating fatty acid composition and markers of inflammation. Lipids 43:65–77
Siri-Tarino PW, Sun Q, Hu FB, Krauss RM (2010) Meta-analysis of prospective cohort studies evaluating the association of saturated fat with cardiovascular disease. Am J Clin Nutr 91(3):535–546
Siri-Tarino PW, Sun Q, Hu FB, Krauss RM (2010) Saturated fat, carbohydrate, and cardiovascular disease. Am J Clin Nutr 91(3):502–509
Cassady BA, Charboneau NL, Brys EE, Crouse KA, Beitz DC, Wilson T (2007) Effects of low carbohydrate diets high in red meats or poultry, fish and shellfish on plasma lipids and weight loss. Nutr Metab (Lond) 4:23
King IB, Lemaitre RN, Kestin M (2006) Effect of a low-fat diet on fatty acid composition in red cells, plasma phospholipids, and cholesterol esters: investigation of a biomarker of total fat intake. Am J Clin Nutr 83:227–236
Raatz SK, Bibus D, Thomas W, Kris-Etherton P (2001) Total fat intake modifies plasma fatty acid composition in humans. J Nutr 131:231–234
Hjelte LE, Nilsson A (2005) Arachidonic acid and ischemic heart disease. J Nutr 135:2271–2273
Lands B (2008) A critique of paradoxes in current advice on dietary lipids. Prog Lipid Res 47:77–106
Ferrucci L, Cherubini A, Bandinelli S, Bartali B, Corsi A, Lauretani F, Martin A, Andres-Lacueva C, Senin U, Guralnik JM (2006) Relationship of plasma polyunsaturated fatty acids to circulating inflammatory markers. J Clin Endocrinol Metab 91:439–446
von Schacky C, Harris WS (2007) Cardiovascular risk and the omega-3 index. J Cardiovasc Med (Hagerstown) 8(Suppl 1):S46–S49
Johnston CS, Tjonn SL, Swan PD, White A, Hutchins H, Sears B (2006) Ketogenic low-carbohydrate diets have no metabolic advantage over nonketogenic low-carbohydrate diets. Am J Clin Nutr 83:1055–1061
Morrow JD, Roberts LJ (1997) The isoprostanes: unique bioactive products of lipid peroxidation. Prog Lipid Res 36:1–21
Harris WS, Pottala JV, Sands SA, Jones PG (2007) Comparison of the effects of fish and fish-oil capsules on the n 3 fatty acid content of blood cells and plasma phospholipids. Am J Clin Nutr 86:1621–1625
Volek JS, Gomez AL, Kraemer WJ (2000) Fasting lipoprotein and postprandial triacylglycerol responses to a low-carbohydrate diet supplemented with n-3 fatty acids. J Am Coll Nutr 19:383–391
Radikova Z, Koska J, Huckova M et al (2006) Insulin sensitivity indices: a proposal of cut-off points for simple identification of insulin-resistant subjects. Exp Clin Endocrinol Diab 114:249–256
Hoidrup S, Andreasen AH, Osler M et al (2002) Assessment of habitual energy and macronutrient intake in adults: comparison of a seven day food record with a dietary history interview. Eur J Clin Nutr 56:105–113
Feinman RD, Fine EJ (2004) “A calorie is a calorie” violates the second law of thermodynamics. Nutr J 3(9)
Keys A (1970) Coronary heart disease in seven countries 41(Supp l):1–211
American Diabetes Association (2008) Nutrition recommendations and interventions for diabetes—2008. Diabetes Care 31(Suppl 1):S61–S78
Klein S, Wolfe RR (1992) Carbohydrate restriction regulates the adaptive response to fasting. Am J Physiol 262:E631–E636
Kotronen A, Velagapudi VR, Yetukuri L et al (2009) Serum saturated fatty acids containing triacylglycerols are better markers of insulin resistance than total serum triacylglycerol concentrations. Diabetologia 52:684–690
Miettinen TA, Naukkarinen V, Huttunen JK, Mattila S, Kumlin T (1982) Fatty-acid composition of serum lipids predicts myocardial infarction. Br Med J (Clin Res Ed) 285:993–996
Wang L, Folsom AR, Eckfeldt JH (2003) Plasma fatty acid composition and incidence of coronary heart disease in middle aged adults: the atherosclerosis risk in communities (ARIC) study. Nutr Metab Cardiovasc Dis 13:256–266
Aarsland A, Wolfe RR (1998) Hepatic secretion of VLDL fatty acids during stimulated lipogenesis in men. J Lipid Res 39:1280–1286
Klein-Platat C, Drai J, Oujaa M, Schlienger JL, Simon C (2005) Plasma fatty acid composition is associated with the metabolic syndrome and low-grade inflammation in overweight adolescents. Am J Clin Nutr 82:1178–1184
Warensjo E, Riserus U, Vessby B (2005) Fatty acid composition of serum lipids predicts the development of the metabolic syndrome in men. Diabetologia 48:1999–2005
Kunesova M, Hainer V, Tvrzicka E et al (2002) Assessment of dietary and genetic factors influencing serum and adipose fatty acid composition in obese female identical twins. Lipids 37:27–32
Paillard F, Catheline D, Duff FL et al (2008) Plasma palmitoleic acid, a product of stearoyl-coA desaturase activity, is an independent marker of triglyceridemia and abdominal adiposity. Nutr Metab Cardiovasc Dis 18:436–440
Vidgren HM, Agren JJ, Schwab U, Rissanen T, Hanninen O, Uusitupa MI (1997) Incorporation of n-3 fatty acids into plasma lipid fractions, and erythrocyte membranes and platelets during dietary supplementation with fish, fish oil, and docosahexaenoic acid-rich oil among healthy young men. Lipids 32:697–705
Lands WE, Libelt B, Morris A, Kramer NC, Prewitt TE, Bowen P, Schmeisser D, Davidson MH, Burns JH (1992) Maintenance of lower proportions of (n-6) eicosanoid precursors in phospholipids of human plasma in response to added dietary (n-3) fatty acids. Biochim Biophys Acta 1180:147–162
Harris WS, Poston WC, Haddock CK (2007) Tissue n-3 and n-6 fatty acids and risk for coronary heart disease events. Atherosclerosis 193:1–10
Block RC, Harris WS, Reid KJ, Spertus JA (2008) Omega-6 and trans fatty acids in blood cell membranes: a risk factor for acute coronary syndromes? Am Heart J 156:1117–1123
Nelson GJ, Schmidt PC, Bartolini G, Kelley DS, Phinney SD, Kyle D, Silbermann S, Schaefer EJ (1997) The effect of dietary arachidonic acid on plasma lipoprotein distributions, apoproteins, blood lipid levels, and tissue fatty acid composition in humans. Lipids 32:427–433
Nelson GJ, Schmidt PC, Bartolini G, Kelley DS, Kyle D (1997) The effect of dietary arachidonic acid on platelet function, platelet fatty acid composition, and blood coagulation in humans. Lipids 32:421–425
Kelley DS, Taylor PC, Nelson GJ, Schmidt PC, Mackey BE, Kyle D (1997) Effects of dietary arachidonic acid on human immune response. Lipids 32:449–456
Kelley DS, Taylor PC, Nelson GJ, Mackey BE (1998) Arachidonic acid supplementation enhances synthesis of eicosanoids without suppressing immune functions in young healthy men. Lipids 33:125–130
Calder PC (2007) Dietary arachidonic acid: harmful, harmless or helpful? Br J Nutr 98:451–453
Guzik TJ, Mangalat D, Korbut R (2006) Adipocytokines—novel link between inflammation and vascular function? J Physiol Pharmacol 57:505–528
Visioli F, Caruso D, Galli C, Viappiani S, Galli G, Sala A (2000) Olive oils rich in natural catecholic phenols decrease isoprostane excretion in humans. Biochem Biophys Res Commun 278:797–799
Nalsen C, Vessby B, Berglund L, Uusitupa M, Hermansen K, Riccardi G, Rivellese A, Storlien L, Erkkila A, Yla-Herttuala S, Tapsell L, Basu S (2006) Dietary (n-3) fatty acids reduce plasma F2-isoprostanes but not prostaglandin F2alpha in healthy humans. J Nutr 136:1222–1228
Mori TA, Dunstan DW, Burke V, Croft KD, Rivera JH, Beilin LJ, Puddey IB (1999) Effect of dietary fish and exercise training on urinary F2-isoprostane excretion in non-insulin-dependent diabetic patients. Metabolism 48:1402–1408
Vessby B, Unsitupa M, Hermansen K et al (2001) Substituting dietary saturated for monounsaturated fat impairs insulin sensitivity in healthy men and women: the KANWU study. Diabetologia 44:312–319
Kirk E, Reeds DN, Finck BN, Mayurranjan SM, Patterson BW, Klein S (2009) Dietary fat and carbohydrates differentially alter insulin sensitivity during caloric restriction. Gastroenterology 136:1552–1560
McLaughlin T, Reaven G, Abbasi F et al (2005) Is there a simple way to identify insulin-resistant individuals at increased risk of cardiovascular disease? Am J Cardiol 96:399–404
Wilke MS, Clandinin MT (2005) Influence of dietary saturated fatty acids on the regulation of plasma cholesterol concentration. Lipids 40:1207–1213
Mata P, Lopez-Miranda J, Pocovi M et al (1998) Human apolipoprotein A-I gene promoter mutation influences plasma low density lipoprotein cholesterol response to dietary fat saturation. Atherosclerosis 137:367–376
Austin MA, King MC, Vranizan KM, Krauss RM (1990) Atherogenic lipoprotein phenotype. A proposed genetic marker for coronary heart disease risk. Circulation 82:495–506
Lands WEM (1995) Long-term fat intake and biomarkers. Am J Clin Nutr 61:721S–725S
Howard BV, Van Horn L, Hsia J et al (2006) Low-fat dietary pattern and risk of cardiovascular disease: the women’s health initiative randomized controlled dietary modification trial. JAMA 295:655–666
Jakobsen MU, O’Reilly EJ, Heitmann BL et al (2009) Major types of dietary fat and risk of coronary heart disease: a pooled analysis of 11 cohort studies. Am J Clin Nutr 89:1425–1432
Acknowledgments
This work was supported by the American Egg Board-Egg Nutrition Center Dissertation Fellowship in Nutrition Award. The funding agency had no input to the design and conduct of the study, the interpretation of the data, or preparation and approval of manuscripts.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
This article is published under an open access license. Please check the 'Copyright Information' section either on this page or in the PDF for details of this license and what re-use is permitted. If your intended use exceeds what is permitted by the license or if you are unable to locate the licence and re-use information, please contact the Rights and Permissions team.
About this article
Cite this article
Forsythe, C.E., Phinney, S.D., Feinman, R.D. et al. Limited Effect of Dietary Saturated Fat on Plasma Saturated Fat in the Context of a Low Carbohydrate Diet. Lipids 45, 947–962 (2010). https://doi.org/10.1007/s11745-010-3467-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11745-010-3467-3