Abstract
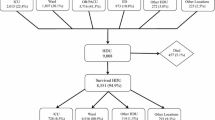
High-Dependency care Units (HDUs) have been introduced worldwide as intermediate wards between Intensive Care Units (ICUs) and general wards. Performing a comparative assessment of the quality of care in HDU is challenging because there are no uniform standards and heterogeneity among centers is wide. The Fenice network promoted a prospective cohort study to assess the quality of care provided by HDUs in Italy. This work aims at describing the structural characteristics and admitted patients of Italian HDUs. All Italian HDUs affiliated to emergency departments were eligible to participate in the study. Participating centers reported detailed structural information and prospectively collected data on all admitted adult patients. Patients’ data are presented overall and analyzed to evaluate the heterogeneity across the participating centers. A total of 12 HDUs participated in the study and enrolled 3670 patients. Patients were aged 68 years on average, had multiple comorbidities and were on major chronic therapies. Several admitted patients had at least one organ failure (39%). Mortality in HDU was 8.4%, raising to 16.6% in hospital. While most patients were transferred to general wards, a small proportion required ICU transfer (3.9%) and a large group was discharged directly home from the HDU (31%). The expertise of HDUs in managing complex and fragile patients is supported by both the available equipment and the characteristics of admitted patients. The limited proportion of patients transferred to ICUs supports the hypothesis of preventing of ICU admissions. The heterogeneity of HDU admissions requires further research to define meaningful patients’ outcomes to be used by quality-of-care assessment programs.

Similar content being viewed by others
Data availability
The data that support the findings of this study are not openly available due to reasons of sensitivity.
References
Ridley SA (1998) Intermediate care possibilities, requirements and solutions. Anaesthesia 53(7):654–664
Caramello V, Catalano A, Macciotta A, Dansero L, Sacerdote C, Costa G et al (2022) Improvements throughout the Three Waves of COVID-19 Pandemic: Results from 4 Million Inhabitants of North-West Italy. J Clin Med 11(15):4304
Plate JDJ, Leenen LPH, Houwert M, Hietbrink F (2017) Utilisation of Intermediate Care Units: A Systematic Review. Crit Care Res Pract 2017:8038460
Boots R, Lipman J (2002) High dependency units: issues to consider in their planning. Anaesth Intensive Care 30(3):348–354
Bertolini G, Confalonieri M, Rossi C, Rossi G, Simini B, Gorini M et al (2005) Costs of the COPD Differences between intensive care unit and respiratory intermediate care unit. Respir Med 99(7):894–900
Nasraway SA, Cohen IL, Dennis RC, Howenstein MA, Nikas DK, Warren J et al (1998) Guidelines on admission and discharge for adult intermediate care units American College of Critical Care Medicine of the Society of Critical Care Medicine. Crit Care Med 26(3):607–610
Cibinel GA, Bacciottini N, Carpinteri G, et al. (2020) Le unità di Terapia Subintensiva nella rete ospedaliera italiana [Internet]. Available from: https://www.simeu.it/w/download/get/0/2020_05_21_SIMEU_Policy_Statement_TSI.pdf/download/articoli/famiglie/302 Accesssed 21 May 2020
Waydhas C, Herting E, Kluge S, Markewitz A, Marx G, Muhl E et al (2018) Intermediate care units: Recommendations on facilities and structure. Med Klin Intensivmed Notfmed 113(1):33–44
Plate JDJ, Peelen LM, Leenen LPH, Houwert RM, Hietbrink F (2018) A Proposal for an intermediate care unit-quality measurement framework. Crit Care Res Pract 2018:4560718
Mario Negri Institute for Pharmacological Research (2024) Evaluation and Improvement of the Health-care Quality in Semi-intensive Care Units. Mario Negri Institute for Pharmacological Research, Rome
Istituto Mario Negri (2021) Fenice—Un nuovo network del laboratorio di epidemiologia clinica. Istituto Mario Negri, Milano
Molina JAD, Seow E, Heng BH, Chong WF, Ho B (2014) Outcomes of direct and indirect medical intensive care unit admissions from the emergency department of an acute care hospital: a retrospective cohort study. BMJ Open 4(11):e005553
Prin M, Harrison D, Rowan K, Wunsch H (2015) Epidemiology of admissions to 11 stand-alone high-dependency care units in the UK. Intensive Care Med 41(11):1903–1910
Confalonieri M, Trevisan R, Demsar M, Lattuada L, Longo C, Cifaldi R et al (2015) Opening of a respiratory intermediate care unit in a general hospital: impact on mortality and other outcomes. Respiration 90(3):235–242
Wright CJ, Allan R (2017) Progressing care in the medical high dependency unit: unit configurations, staffing, standards, and daily routine. Acute Med 16(1):16–20
Amiruddin N, Prescott GJ, Coventry DA, Jansen JO (2018) Evaluating service development in critical care: The impact of establishing a medical high dependency unit on intensive care unit workload, case mix, and mortality. J Intensive Care Soc 19(3):226–235
Wong DJN, Popham S, Wilson AM, Barneto LM, Lindsay HA, Farmer L et al (2019) Postoperative critical care and high-acuity care provision in the United Kingdom, Australia, and New Zealand. Br J Anaesth 122(4):460–469
Confalonieri M, Kodric M, Garuti G (2001) Respiratory intermediate (high dependency) unit care in Europe: models of service provision. Monaldi Arch Chest Dis 56(3):248–253
Garfield M, Jeffrey R, Ridley S (2000) An assessment of the staffing level required for a high-dependency unit. Anaesthesia 55(2):137–143
Chen F, Liu L, Wang Y, Liu Y, Fan L, Chi J (2022) Delirium prevalence in geriatric emergency department patients: a systematic review and meta-analysis. Am J Emerg Med 59:121–128
Krewulak KD, Stelfox HT, Leigh JP, Ely EW, Fiest KM (2018) Incidence and prevalence of delirium subtypes in an adult ICU: a systematic review and meta-analysis. Crit Care Med 46(12):2029–2035
Yang FM, Marcantonio ER, Inouye SK, Kiely DK, Rudolph JL, Fearing MA et al (2009) Phenomenological subtypes of delirium in older persons: patterns, prevalence, and prognosis. Psychosomatics 50(3):248–254
Torres OH, Francia E, Longobardi V, Gich I, Benito S, Ruiz D (2006) Short- and long-term outcomes of older patients in intermediate care units. Intensive Care Med 32(7):1052–1059
Morland M, Haagensen R, Dahl FA, Berdal JE (2018) Epidemiology and prognoses in a medical intermediate care unit. Tidsskr Nor Laegeforen 138:8
Acknowledgements
The start of the Fenice HDU project was partially supported by an unconditioned grant from the Italian Society of Emergency Medicine (SIMEU).
Funding
Italian Society of Emergency Medicine (SIMEU), Unconditioned grant.
Author information
Authors and Affiliations
Contributions
The authors substantially contributed to the paper as follows: conception and design (GP, FS, MC, GC, VC, CR, FA, AB, RB, MC, EC, PC, GIG, PN, LP, PPP, SP, AR, GN, GB), analysis (FS, CR, GN) and interpretation (all authors) of data, drafting the article (GP, FS, MC, GC, VC, GN, GB) or critical revision (all authors). All authors approved the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interests
None of the authors has any conflict of interest in relation to this work.
Ethical Approval
The study was approved by the ethics committee of the Fondazione IRCCS Istituto Neurologico “Carlo Besta” and by the institutional review boards of all participating centers.
Informed consent
Informed consent was obtained from patients or legal representatives.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Porta, G., Signorini, F., Converso, M. et al. The Fenice project to evaluate and improve the quality of healthcare in high-dependency care units: results after the first year. Intern Emerg Med (2024). https://doi.org/10.1007/s11739-024-03640-5
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11739-024-03640-5