Abstract
Genetic and acquired motor-neuron-disorders (MNDs) may undergo acute deterioration resulting in various emergency situations. This literature review aims at summarising and discussing current knowledge about emergencies in MNDs. Emergencies that have been reported in MND patients include: respiratory, bulbar, cardiac, septic, epileptic, psychiatric, pain-related, and traumatic emergencies. Emergencies due to respiratory insufficiency have the strongest impact on morbidity and mortality in MNDs. To optimise the management of emergencies in MNDs, it is recommended to discuss these topics with the patient prior to their occurrence. After informed consent, patients may indicate their decision by signing an advance directive as to how such emergencies should be managed in case they arise. Generally, treatment of emergencies in MNDs is not at variance from treatment of similar emergencies due to other causes, but some peculiarities need to be pointed out. It is concluded that patients with MNDs may experience various emergencies during the disease course. Management of these conditions should be discussed with the patient prior to their appearance. Management of these emergencies follows general guidelines, which widely vary between countries, and depend on the availability of a patient’s advance directive.
Similar content being viewed by others
Introduction
Motor neuron disorders (MNDs), also known as anterior horn cell disorders, are a heterogeneous group of neuromuscular disorders (NMDs) due to impaired functioning of the second motor neuron [1]. In some of the MNDs the central nervous system may be additionally affected. MNDs may have a genetic cause or may be acquired. Genetic MNDs include familial amyotrophic lateral sclerosis (fALS), spinal muscular atrophies (SMAs), bulbospinal muscular atrophy Kennedy (BSMA), the adrenoleucodystrophies (ALDs), hereditary spastic paraplegias (HSPs), mitochondrial disorders (MIDs), hexosaminidase-deficiency type A (Sandhoff disease, GM2 gangliosidosis), and Brown–Vialetto–Van Laere syndrome (BVLS), a congenital motor neuron disease with pontobulbar palsy, sensorineural hearing loss, and respiratory insufficiency. The acquired MNDs include sporadic ALS (sALS), aluminium-. lead- and mercury-intoxication, syringomyelia, myelopathy, myelitis, Hirayama’s disease, and poliomyelitis. Genetic and acquired MNDs may undergo acute deterioration resulting in various emergency situations. This review aims at summarising and discussing current knowledge about emergencies in MNDs.
Materials and methods
Data for this review were identified by searches of MEDLINE, Current Contents, EMBASE, Web of Science, Web of Knowledge, LILACS, SCOPUS, and Google Scholar for references of relevant articles. Search terms used for these databases were “motor neuron disease,”“spinal muscular atrophy,” “neuronopathy,” “anterior horn cell disease,” “lead intoxication,” “adrenoleucodystrophy,” “Kennedy disease,” “Sandhoff disease,” “hereditary spastic paraplegia,” “Brown–Vialetto–Van Laere syndrome,” and “mitochondrial disorder,” which were combined with “emergency,” “respiratory insufficiency,” “Takotsubo syndrome,” “sepsis,” “infection,” “psychosis,” “epilepsy,” “seizure,” “pain,” and “trauma.” Results of the search were screened for potentially relevant studies by application of inclusion and exclusion criteria for the full texts of the relevant studies. Included were randomized controlled trials (RCTs), observational studies with controls, case series, and case reports. Reviews, editorials, and letters were not included. Only original articles about humans, in English, French, Spanish, or German and published between 1966 and 2016 were included. Reference lists of retrieved studies were checked for reports of additional studies.
Results
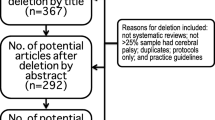
By searching the literature according to the criteria mentioned above, the number of hits achieved was 2993. By filtering these results through exclusion of articles on non-human subjects, of review articles, letters, and of editorials, and exclusion of articles in an inappropriate language, the number was reduced to 274 hits. After studying the abstracts, 125 were selected for detailed studying, but only 85 were accessible as full papers, and thus included in the list of references. Emergencies that have been reported in patients with MND include: respiratory, bulbar, cardiac, septic, epileptic, psychiatric, pain-related, and traumatic emergencies.
Respiratory emergency
Pathogenesis and presentation
Respiratory insufficiency is the most frequent cause of morbidity and mortality in MNDs [2, 3]. Particularly in ALS, SMA, ALD, BSMA, and BVLS, the respiratory muscles will be affected with progression of the disease resulting in respiratory insufficiency, infection, or respiratory failure [4, 5]. Rarely, respiratory dysfunction has been reported in HSP [6]. Affected muscles may be the diaphragm, the intercostal muscles, the scalene muscles, sternocleidomastoid, serratus anterior, pectoralis major, pectoralis minor, trapezius, latissimus dorsi, erector spinae, iliocostalis lumborum, quadratus lumborum, serratus posterior superior, serratus posterior inferior, transversum thoracis, levatores costarum, and subclavius muscles [7]. Respiratory insufficiency may be diagnosed clinically or by instrumental investigations. Instrumental investigations to detect clinically manifest or subclinical respiratory insufficiency include pulmonary function testing, bedside spirometry, nocturnal oxygenation monitoring, and blood gas analysis. Blood gas analysis may reveal partial or global respiratory insufficiency [decreased pO2, increased pCO2, or both, decreased maximal inspiratory pressure (MIP)]. With pulmonary function testing, the forced vital capacity (FVC), the MIP, or the maximal expiratory pressure (MEP) can be measured. Respiratory insufficiency is characterised by reduced FVC, increased MIP, and decreased MEP [8]. Partial or permanent hypoxygenation (O2 desaturation) may be measured online temporarily or permanently. Function of the diaphragm may be monitored by measuring the compound muscle action potential amplitude after supramaximal stimulation of the phrenic nerve [9]. An X-ray study of the lung may show unilateral or bilateral high riding of the diaphragm.
Management
In the emergency department
If respiratory insufficiency occurs acutely without knowing the neurological diagnosis, MND patients usually undergo emergency intubation and consecutive mechanical ventilation. Due to the increased risk of vomiting, regurgitation, and aspiration in such a situation, the anesthetic management may be facilitated by application of rapid sequence induction (RSI), the cornerstone of emergency airway management. In case of acute respiratory and availability of a patient’s will, management is determined by what has been written as the patient’s desires. In case the patient refuses intubation, heated, humidified oxygen via a high-flow nasal cannula is an alternative option [10].
Prior to the emergency department
In most cases, respiratory insufficiency develops slowly over a long time. This is why MND patients should undergo repeated assessments of respiratory functions. The follow-up investigations can be facilitated by application of ambulatory spirometry [11]. In case respiratory insufficiency develops, physical therapy, application of oxygen, and non-invasive positive pressure ventilation (NIPPV) may alleviate the patient’s dyspnea. Airway management in MND patients under NIPPV may be supported by use of a humidification or saline nebulizer, by techniques such as breath stacking, by mechanically assisted coughing (MAC), or by use of mechanical insufflation-exsufflation. Opioid analgesics (morphine salts, diamorphine) may be utilised to reduce the cough reflex, control pain, and relieve dyspnoea. Oxygen therapy should be used with caution to avoid hypercapnia. Physiotherapy may be helpful to clear secretions. If these measures are no longer sufficient to provide decent oxygenation, it has to be decided if mechanical ventilation should be applied or not. Mechanical ventilation may take place in an institution or at home (home tracheotomy mechanical ventilation) [12]. Unique for the management of emergencies in patients with MNDs is that these patients are increasingly confronted with the various emergency situations long before they occur, and more and more frequently patients determine after informed consent in advance by signing an advance directive (AD) concerning type and intensity of treatment they want to receive in case it becomes necessary. However, living will and advance care planning (ACP) may be different in various countries, and should be carried out according to national or international guidelines. In a recent Italian study of relatives working as caregivers of artificially ventilated ALS patients, the mean survival time after tracheotomy is 30 months, 85% of the patients did not want to be tracheotomised, but were forced by their relatives to do so, the quality of life for patients and relatives massively deteriorated after tracheostomy, 4–6 months prior to decease, deterioration of the situation was recognized by the patients and relatives, communication between the two became worse as well, decubital ulcers, local infections, and septic conditions developed, the use of catheters became necessary, and that sedating and analgesic medications were more frequently applied than before tracheotomy [13]. Respiratory insufficiency in Brown–Vialetto–Van Laere syndrome, which is due to mutations in the riboflavin transporter, favourably responds to administration of riboflavin [14].
Bulbar emergency
Pathogenesis and presentation
Another emergency in patients with MND may arise if bulbar muscles become affected and insufficient. Bulbar problems may occur in case of choking caused by mucus build-up, problems swallowing food, water or saliva, or in case of exsiccosis. This may lead to impaired swallowing, impaired closure of the epiglottis, and impaired innervation of the larynx. As a consequence, nutrition, fluid intake, and speech become inadequate, leading to bulbar speech, dysphagia, aspiration, pneumonia, cachexia, and exsiccosis. Bulbar emergencies particularly arise in patients with ALS, SMA, and BSMA. Bulbar involvement has been also reported in ALD [15], HSP [16], BVLS [17] and Sandhoff disease [18].
Management
In the emergency department
In case of acute bulbar dysfunction and choking, oral suction, endotracheal suction, or in case of severe aspiration, intubation and artificial ventilation may be necessary. Though bulbar dysfunction may be triggered by infection or drugs, it is usually not reversible and requires an appropriate long-term management.
Prior to the emergency department
To avoid emergencies caused by impaired bulbar functions, it is recommended to timely implant a percutaneous, endoscopic gastrosotomy (PEG). This may avoid exsiccosis and malnutrition. The PEG should be placed early enough since aggressive proactive nutritional management appears essential in patients with MND [19]. To avoid aspiration, however, it is essential to either regularly aspirate the patient, or to create an elective tracheotomy. The tracheal stoma needs be one that can be cuffed to effectively avoid any fluid from running into the tracheal system, or to improve the shock caused by coughing. Prior to a tracheotomy, devices can be applied that mechanically support coughing. Deglution can be improved by regular electrical stimulation of the pharynx, as has been demonstrated in patients with ischemic stroke [20]. Swallowing in patients with ALS can be improved by changes of posture or by the use of special swallowing techniques. Compensatory and restitutional swallowing therapeutic methods can help to ensure oral alimentation for as long as possible, and also help prevent food aspiration.
Cardiac emergency
Pathogenesis and presentation
The most well-known and increasingly recognised acute cardiac emergency in MNDs is the Takotsubo syndrome (TTS), also known as stress cardiomyopathy or broken-heart syndrome. TTS is characterised by an acute-onset, usually reversible deterioration of left ventricular function triggered by physical or psychological stress. Psychological stress can be endogenous or exogenous. Three types of TTS are differentiated: the classical type where hypokinesia, dyskinesia, or akinesia affects the apical or apical and midventricular segments of the left ventricle; the inverted TTS where the basal or mid-ventricular segments are involved; and the global type where all segments of the left ventricle are affected [21]. Clinically, blood-chemically, and electrocardiographically TTS mimics myocardial infarction with the difference that echocardiography may show the Takotsubo morphology (akinetic/hypokinetic/dyskinetic segments together with hyperkinetic segments) and that coronary angiography is usually normal. In the majority of the cases, there is spontaneous or drug-supported complete remission of left ventricular dysfunction. Echocardiography becomes normal within 6 weeks after onset, and the electrocardiogram within 10 weeks after onset. In some cases, however, no remission can be achieved despite maximal treatment, with a fatal outcome. TTS is a condition that can recur. In MNDs, TTS is most frequently triggered by stress due to respiratory insufficiency [22]. Dyspnea from TTS has to be delineated from dyspnoea from muscular respiratory insufficiency, but in some cases, dyspnoea may be due to both. So far, TTS has been reported in 6 patients with ALS, but in none of the other MNDs [22–27]. Other cardiomyopathies are rare in MNDs, but dysrhythmias have been repeatedly reported. In a single patient with SMA dilatated cardiomyopathy has been found [28]. In single patients with Sandhoff disease, hypertrophic cardiomyopathy has been described [29]. In a recent case report, a patient carrying an LMNA mutation presented with a MND phenotype including dysrhythmias [30]. Autonomic involvement in ALS may be associated with atrio-ventricular (AV)-block III [31]. Malignant ventricular dysrhythmias have been occasionally reported in patients with SMA [32]. Other patients with SMA and right bundle branch block and intermittent AV-block III have been reported [33]. In the terminal stages of ALS, patients may have reduced sympathetic activity, giving rise to prolongation of the QT-interval, increased QTc dispersion, and sudden cardiac death [34]. In BSMA patients, Brugada-type ECGs have been reported [35].
Management
In the emergency department
Since TTS mimics myocardial infarction, the emergency physician needs to initially exclude myocardial infarction. The clinical presentation suggests TTS, echocardiography is the next diagnostic step. If echocardiography confirms TTS, coronary heart disease needs to be excluded by coronary angiography. There is no consensus whether each type of TTS requires drug or invasive treatment. Consensus, however, exists that the global type of TTS requires therapy. In case the treating physician decides for a treatment, drugs used for heart failure therapy are recommended. Adrenergic substances should be avoided since they might enhance systolic dysfunction. Patients with acute dysrhythmias may require antidysrhythmic medication, implantation of a pacemaker, or an implantable cardioverter defibrillator (ICD) [31]. In case of severe ventricular dysrhythmias, cardio-pulmonary resuscitation (CPR) may be necessary.
Prior to the emergency department
To avoid the development of TTS, all measures must be taken to avoid triggering factors of TTS. These include anxiety management, avoidance of pain, and extensive education about the diagnosis and prognosis with consecutive psychological support.
Septic emergency
Pathogenesis and presentation
Patients with MND carry an increased risk of infections because of immobility, respiratory insufficiency, or the frequent need to carry out invasive measures. In case focal infections are not sufficiently treated with antibiotics, are treated too late, are not treated at all, or in case the causative agents are resistant to the applied antibiotics, bacteriemia or septicaemia may ensue. Particularly, patients with ALS are prone to develop septic conditions [36]. More rarely, sepsis develops in patients with spinal muscular atrophy [37]. Sepsis in patients with MND may originate from respiratory infections, decubitus, sinusitis due to nasal tubes, tracheotomy, skin lesions from the ventilator mask, PEG, urinary catheter, phlebitis, or from thrombosis due to immobility.
Management
In the emergency department
If sepsis is complicated by respiratory insufficiency or cardiac compromise, including septic shock, intensive care measures will be necessary. In case of septic shock in a MND patient without a patient’s ability to give permission, all measures according to established guidelines [38] should be taken to attempt achieving complete recovery.
Prior to the emergency department
Managing an infection prior to septic shock can be challenging, particularly in the early stages of the condition. This is because early manifestations may be non-specific. Blood chemical investigations such as decreased thrombocyte count, elevated procalcitonin, elevated lactate, or elevated interleukin (IL)-6 may support the diagnosis [39]. Most important is to identify the focus of the sepsis, to identify the causative agent, and to treat according to the antibiogram. The choice of antibiotic treatment must consider if a patient additionally suffers from myasthenia, epilepsy, liver insufficiency, renal insufficiency, or allergy to antibiotics. Generally, aminoglycosides should be avoided for the treatment of sepsis. Unique for the treatment of severe infections in MND patients under mechanical ventilation is, that the management can be determined already before the occurrence of such a situation in form of a patient’s written wishes.
Epileptic emergency
Pathogenesis and presentation
Among the MNDs with central nervous system involvement, such as ALS, SMA, ALD, MID, HSP, or Sandhoff disease, emergencies may arise due to affection of the brain. The classical emergency due to central nervous system involvement is the seizure. In neonates, seizures may even be the initial manifestation of ALD [40]. Seizures may also occur in adults with ALD or female carriers of the disease [41]. Rarely, seizures have been described in patients with BVLS [42]. Myoclonus epilepsy has been described in patients with SMA [43, 44], and also in patients with Sandhoff disease [45]. Occasionally, seizures can be a phenotypic feature also of HSP [46].
Management
In the emergency department
If a NMD patient has a single generalised seizure, a series of seizures, or status epilepticus, treatment according to the currently valid guidelines of the International League Against Epilepsy (ILAE) should be applied [47].
Prior to the emergency department
To prevent emergencies from seizures in MND patients, optimal seizure control should be pursued. Treatment of seizures and epilepsy in MNDs is the same as in non-MND patients. Generally, seizures in MND patients respond favorably to standard antiepileptic drugs (AEDs) [41]. If seizures occur in patients with MNDs due to a MID, however, care has to be taken not to apply AEDs with a mitochondrion-toxic potential, such as valproic acid, carbamazepine, phenytoin, or barbiturates, or to give them only if other antiepileptic drugs are ineffective.
Psychiatric emergencies
Pathogenesis and presentation
Another type of cerebral emergency in patients with MNDs is the acute confusional state, which may be associated with dementia, as in ALS [48–50], BSMA [51], Sandhoff disease [52, 53], HSP [54], MID, or ALD [55, 56] (Table 1). Psychiatric emergencies, including psychosis, may particularly occur in MNDs due to a MID. Among MIDs, confusional states and psychosis have been particularly reported in patients with MELAS syndrome, LHON [57], and adult Leigh-syndrome [58].
Management
In the emergency department
If a MND patient presents with a confusional state, delirium, severe depression, or an acute psychosis, the patient should undergo cerebral imaging and possibly electroencephalography (EEG), and if not explanatory, should be referred to the psychiatrist. If a psychiatrist is not immediately available, standard sedative, antidepressive, or antipsychotic medication should be applied according to published recommendations [59]. Psychiatric emergencies in MID patients require treatment according to current recommendations [60], and cautious application of mitochondrion-toxic drugs, including neuroleptics.
Prior to the emergency department
In case of evolving psychiatric abnormalities in patients with a MND, not only psychiatric treatment needs to be initiated, but also neurologic work-up including imaging and EEG not to miss a deterioration of the MND or the occurrence of co-pathologies. Depression, anxiety, psychotic symptoms, drive failure, or excitation state, need to be adequately treated and drugs, which could promote such conditions, need to be discontinued.
Pain
Pathogenesis and presentation
Pain is a frequent manifestation of MNDs. It may occur as a chronic condition, or may arise suddenly, even as an emergency. Pain in MNDs may have different causes. Acute pain in MNDs is most frequently due to muscle cramps. In a study of 41 patients with ALS, 95% develop muscle cramps during the disease course [61]. These muscle cramps occur either spontaneously, particularly in the distal limbs [62], or they are induced by voluntary or involuntary contractions. Frequency of muscle cramps in ALS varies considerably from month to month, but generally frequency and intensity decline during the first year after onset [61]. Muscle cramps more frequently occur in patients with limb-onset ALS, or those >60 years of age, than among those with bulbar-onset ALS and age <60 years [61]. In addition to ALS, cramps have been reported in patients with BSMA [63] and Sandhoff disease [64]. However, pain in ALS may also be non-specific. In a study of 46 ALS patients, 78% of the patients complained about non-specific pain [62]. Pain in ALS results in a significant disturbance of the activities of daily living, in a reduction of the quality of life, and to depression [62]. Pain may also result from severe spasticity as in ALD [65]. Non-specific pain additionally occurs in SMA [66] and HSP [67],
Management
In the emergency department
A MND patient with acute pain needs to be thoroughly investigated for the cause of pain, and after identification of the cause, needs to receive analgesics according to the guidelines from pain societies [68]. According to a recent Cochrane-review [69], there is currently no compound available that can be recommended for the treatment of muscle cramps in MNDs. However, magnesium, chinin, respectively gabapentin should be tried, but chinin has been taken off the market in several countries because of cardiac or hematological side effects.
Prior to the emergency department
Pain due to cramps or neuropathy, spasticity, arthralgia, or myalgia have to be taken seriously by treating physicians and adequately treated. Prophylactic measures are mandatory in NMD patients to prevent the development acute or chronic pain.
Trauma
Pathogenesis and presentation
Ambulatory ALS patients have a risk of falls and traumatic injuries. The risk of falls results on the one hand from progressive muscle weakness and resultant gait disturbance [70], and on the other hand from impaired processing of vestibular input [71]. In a recent study of 34 ambulatory ALS patients with normal results on vestibulatory testing, 37% showed a decreased ability to adequately process the vestibular input [71]. In case ALS is associated with dementia, falls may result from confusional states. Falls may also be due to involvement of the autonomic nervous system. Another potential cause of falls in ambulatory MND patients may be impaired sensory functions with or without sensory ataxia. An emergency may arise in case of a fall and injury, such as head trauma or bone fractures. Head trauma may not only acutely deteriorate ALD [72], but may even trigger the development of ALD [73]. Falls in BSMA or ALD may lead to hip fractures [74, 75]. Fractures have also been reported in patients with SMA although they may often go undetected [76]. The frequency of fractures is particularly high in ALS [77].
Management
In the emergency department
In case of a severe trauma, MND patients need to be referred to trauma surgery. Unique for MND patients undergoing general anesthesia is that, particularly in MID patients, deterioration of the general condition may occur after surgery.
Prior to the emergency department
To prevent fractures in the context of falls, it has been recently proposed to treat these patients with the etidronat bisphosphonate [78].
Discussion
This review shows that patients with hereditary or acquired MNDs may experience various emergencies in case of respiratory muscle weakness, bulbar muscle weakness, cardiac compromise, infectious disease, epilepsy, psychiatric abnormalities, pain, or trauma. The most important of the emergencies are acute respiratory insufficiency and epilepsy since they have the strongest impact on morbidity and mortality of MND patients.
Management of emergencies in MNDs is not at variance from management in patients with other diagnoses, and follows current national or international guidelines. However, management of emergencies in patients with MNDs strongly depends on whether the neurological diagnosis is already known and established, or not, when the patient arrives in the emergency department, and whether there is an AD available or not (Fig. 1). In case the underlying diagnosis is not yet established, emergencies in NMD patients should be managed according to the most recent and updated national or international guidelines. In case the diagnosis MND is established, management of emergencies depends on whether or not an AD is available. In case no AD is available, but the diagnosis MND is known, treating physicians have to decide if an emergency is managed according to currently valid guidelines, by less intensive measures, or palliative, which can result in an ethical dilemma [79]. In case there is no AD available, and the patient is not decisionally capacitated, therapy has to be applied according to the disposal of the procurator, if available (Fig. 1). If no advocate representative is available, the treating physician decides which therapeutic management is applied. For example, in case of acute respiratory failure and absence of an AD, treating physicians need to decide whether the patient is going to be intubated and mechanically ventilated. In case of a bulbar emergency, treating physicians need to decide whether a patient should receive a nasogastral tube, a central intravenous line, a PEG, or a tracheostomy. In case of infections, treating physicians need to decide if antibiotics are applied, which antibiotics are given, and how often in case of recurrent infections. Seizures should be treated in any case, and an AD should not contain the prohibition of treating seizures.
In case an AD is available, treating physicians need to handle the emergency according to the commitment in the AD. In this case, management of emergencies strongly depends on how detailed the AD is drafted, and which eventualities have been considered at the time of the agreement. Concerning the content of an AD, it is recommended that potential emergencies are explained to and discussed with the patient prior their occurrence, and that the patient gives informed consent how such possible emergencies should be managed when they arise (Fig. 1) [80]. Current practice in Switzerland and France tends to discourage the use mechanical ventilation in MNDs due to fear of a “locked-in syndrome”, the huge burden put on caregivers, and unmasking cognitive decline in MNDs with dementia [81]. In Norway, an autonomous patient has the right to refuse life-prolonging treatment, but if the patient is not defined as dying, health personnel are obliged to start life-saving treatment in an emergency situation even against the patient’s will [82].
Adequate management of emergencies in MND patients additionally includes that drugs that may deteriorate the acute situation are discontinued. As an example, baclofen which is given for spasticity in ALS patients, and may deteriorate muscle weakness, needs to be immediately discontinued in case of respiratory failure [83]. Also drugs that are used for behavioural disturbances must be discontinued since they may deteriorate dysarthria, dysphagia, and muscle weakness in ALS patients [83]. MIDs may mimic MNDs [84], and treatment of MIDs mimicking MNDs is at variance from treatment of MNDs due to other causes [84, 85]. Overall, however, emergencies in MNDs are treated according to guidelines that are not specific for MNDs. There is a need to generate such specific guidelines in the future.
Limitations of the review are that caregiver breakdown, social emergencies, laryngospasm, or blockage in the feeding tube are not addressed due to space limitations.
Conclusions
Patients with MNDs may experience respiratory, bulbar, cardiac, infectious, epileptic, psychiatric, pain-related, and traumatic emergencies during the disease course. Currently, management of emergencies in MNDs is not at variance from management of the same emergencies in other patients, and follows current national or international guidelines. Due to some peculiarities of MNDs, however, there is a need to generate guidelines that are specific for emergencies in MNDs. These should include that management of emergencies in MNDs is discussed with the patient prior to the occurrence of any emergency, and that informed consent and an AD be obtained from the patient concerning the initiation of invasive measures in case such emergencies arise.
Abbreviations
- ACP:
-
Advance care planning
- AD:
-
Advance directive
- AEDs:
-
Antiepileptic drugs
- ALD:
-
Adrenoleucodystrophy
- ALS:
-
Amyotrophic lateral sclerosis
- AV-block:
-
Atrio-ventricular block
- BSMA:
-
Bulbospinal muscular atrophy Kennedy
- BVLS:
-
Brown–Vialetto–Van Laere syndrome
- CPR:
-
Cardio-pulmonary resuscitation
- EEG:
-
Electroencephalography
- fALS:
-
Familial amyotrophic lateral sclerosis
- FVC:
-
Forced vital capacity
- HSPs:
-
Hereditary spastic paraplegias
- ICD:
-
Implantable cardioverter defibrillator
- ILAE:
-
International League Against Epilepsy
- MAC:
-
Mechanically assisted coughing
- MEP:
-
Maximal expiratory pressure
- MIDs:
-
Mitochondrial disorders
- MIP:
-
Maximal inspiratory pressure
- MND:
-
Motor neuron disease
- NIPPV:
-
Non-invasive positive pressure ventilation
- NMDs:
-
Neuromuscular disorders
- PEG:
-
Percutaneous, endoscopic gastrostomy
- RSI:
-
Rapid sequence induction
- sALS:
-
Sporadic amyotrophic lateral sclerosis
- SMA:
-
Spinal muscular atrophy
- TTS:
-
Takotsubo syndrome
References
Morris J (2015) Amyotrophic lateral sclerosis (ALS) and related motor neuron diseases: an overview. Neurodiagn J 55:180–194
Damak H, Décosterd D (2015) Acute respiratory failure in neuromuscular disease. Rev Med Suisse 11:1809–1814
Macpherson CE, Bassile CC (2016) Pulmonary physical therapy techniques to enhance survival in amyotrophic lateral sclerosis: a systematic review. J Neurol Phys Ther 40:165–175
Xiong H, Zhang YH, Qin J, Xiao JX, Shi CY, Zhou SM, Wu XR (2003) Clinical characteristics of X-linked adrenoleukodystrophy. Zhonghua Er Ke Za Zhi 41:203–207
Chahin N, Klein C, Mandrekar J, Sorenson E (2008) Natural history of spinal-bulbar muscular atrophy. Neurology 70:1967–1971
McDermott CJ, Burness CE, Kirby J, Cox LE, Rao DG, Hewamadduma C, Sharrack B, Hadjivassiliou M, Chinnery PF, Dalton A, Shaw PJ, UK and Irish HSP Consortium (2006) Clinical features of hereditary spastic paraplegia due to spastin mutation. Neurology 67:45–51
Kendall F, McCreary E, Provance P, Rodgers M, Romai W (2005) Muscles testing and function with posture and pain, 5th edn. Lippincott Williams & Wilkins, Philadelphia
Orsini M, Lopes AJ, Menezes SL, Oliveira AB, Freitas MR, Nascimento OJ, Guimarães FS (2015) Current issues in the respiratory care of patients with amyotrophic lateral sclerosis. Arq Neuropsiquiatr 73:873–876
Jenkins JA, Sakamuri S, Katz JS, Forshew DA, Guion L, Moore D, Miller RG (2016) Phrenic nerve conduction studies as a biomarker of respiratory insufficiency in amyotrophic lateral sclerosis. Amyotroph Lateral Scler Frontotemporal Degener 17:213–220
Díaz-Lobato S, Folgado MA, Chapa A, Mayoralas Alises S (2013) Efficacy of high-flow oxygen by nasal cannula with active humidification in a patient with acute respiratory failure of neuromuscular origin. Respir Care 58:e164–e167
Couratier P, Vincent F, Torny F, Lacoste M, Melloni B, Lemaire F, Antonini MT (2005) Spirometer-dependence of vital capacity in ALS: validation of a portable device in 52 patients. Amyotroph Lateral Scler Other Motor Neuron Disord 6:239–245
Sancho J, Servera E, Díaz JL, Bañuls P, Marín J (2011) Home tracheotomy mechanical ventilation in patients with amyotrophic lateral sclerosis: causes, complications and 1-year survival. Thorax 66:948–952
Veronese S, Valle A, Chiò A, Calvo A, Oliver D (2014) The last months of life of people with amyotrophic lateral sclerosis in mechanical invasive ventilation: a qualitative study. Amyotroph Lateral Scler Frontotemporal Degener 15:499–504
Foley AR, Menezes MP, Pandraud A, Gonzalez MA, Al-Odaib A, Abrams AJ et al (2014) Treatable childhood neuronopathy caused by mutations in riboflavin transporter RFVT2. Brain 137:44–56
Nagumo K, Shinotoh H, Arai K, Furumoto H, Hirayama K (1995) Frontal type adrenoleukodystrophy: the progress of the white matter lesion—a neuroradiological and pathological study. Rinsho Shinkeigaku 35:983–990
Matsufuji M, Osaka H, Gotoh L, Shimbo H, Takashima S, Inoue K (2013) Partial PLP1 deletion causing X-linked dominant spastic paraplegia type 2. Pediatr Neurol 49:477–481
Dakhil FO, Bensreiti SM, Zew MH (2010) Pontobulbar palsy and sensorineural deafness (Brown–Vialetto–Van Laere syndrome): the first case from Libya. Amyotroph Lateral Scler 11:397–398
Maegawa GH, Stockley T, Tropak M, Banwell B, Blaser S, Kok F, Giugliani R, Mahuran D, Clarke JT (2006) The natural history of juvenile or subacute GM2 gangliosidosis: 21 new cases and literature review of 134 previously reported. Pediatrics 118:e1550–e1562
Mitsumoto H, Davidson M, Moore D, Gad N, Brandis M, Ringel S, Rosenfeld J, Shefner JM, Strong MJ, Sufit R, Anderson FA, ALS CARE Study Group (2003) Percutaneous endoscopic gastrostomy (PEG) in patients with ALS and bulbar dysfunction. Amyotroph Lateral Scler Other Motor Neuron Disord 4:177–185
Bath PM, Scutt P, Love J, Clavé P, Cohen D, Dziewas R, Iversen HK, Ledl C, Ragab S, Soda H, Warusevitane A, Woisard V, Hamdy S, Swallowing Treatment Using Pharyngeal Electrical Stimulation (STEPS) Trial Investigators (2016) Pharyngeal electrical stimulation for treatment of dysphagia in subacute stroke: a randomized controlled trial. Stroke 47:1562–1570
Finsterer J, Wahbi K (2014) CNS disease triggering Takotsubo stress cardiomyopathy. Int J Cardiol 177:322–329
Peters S (2014) Takotsubo cardiomyopathy in respiratory stress syndrome in amyotrophic lateral sclerosis. Int J Cardiol 177:187
Suzuki Y, Oishi M, Kanno A, Ogawa K, Fujisawa M, Kamei S (2013) Amyotrophic lateral sclerosis accompanying elevated catecholamines occurring as a complication of takotsubo cardiomyopathy. Geriatr Gerontol Int 13:240–241
Massari FM, Tonella T, Tarsia P, Kirani S, Blasi F, Magrini F (2011) Tako-tsubo syndrome in a young man with amyotrophic lateral sclerosis. A case report. G Ital Cardiol (Rome) 12:388–391
Matsuyama Y, Sasagasako N, Koike A, Matsuura M, Koga T, Kawajiri M, Ohyagi Y, Iwaki T, Kira J (2008) An autopsy case of amyotrophic lateral sclerosis with ampulla cardiomyopathy. Rinsho Shinkeigaku 48:249–254
Mitani M, Funakawa I, Jinnai K (2005) Transient left ventricular apical ballooning, “Takotsubo” cardiomyopathy, in an amyotrophic lateral sclerosis patient on long-term respiratory support. Rinsho Shinkeigaku 45:740–743
Takayama N, Iwase Y, Ohtsu S, Sakio H (2004) “Takotsubo” cardiomyopathy developed in the postoperative period in a patient with amyotrophic lateral sclerosis. Masui 53:403–406
Elkohen M, Vaksmann G, Elkohen MR, Francart C, Foucher C, Rey C (1996) Cardiac involvement in Kugelberg-Welander disease. A prospective study of 8 cases. Arch Mal Coeur Vaiss 89:611–617
Villamizar-Schiller IT, Pabón LA, Hufnagel SB, Serrano NC, Karl G, Jefferies JL, Hopkin RJ, Prada CE (2015) Neurological and cardiac responses after treatment with miglustat and a ketogenic diet in a patient with Sandhoff disease. Eur J Med Genet 58:180–183
Iwahara N, Hisahara S, Hayashi T, Kawamata J, Shimohama S (2015) A novel lamin A/C gene mutation causing spinal muscular atrophy phenotype with cardiac involvement: report of one case. BMC Neurol 15:13. doi:10.1186/s12883-015-0269-5
Shemisa K, Kaelber D, Parikh SA, Mackall JA (2014) Autonomic etiology of heart block in amyotrophic lateral sclerosis: a case report. J Med Case Rep 8:224. doi:10.1186/1752-1947-8-224
Roos M, Sarkozy A, Chierchia GB, De Wilde P, Schmedding E, Brugada P (2009) Malignant ventricular arrhythmia in a case of adult onset of spinal muscular atrophy (Kugelberg–Welander disease). J Cardiovasc Electrophysiol 20:342–344
Takahashi N, Shimada T, Ishibashi Y, Sugamori T, Hirano Y, Oyake N, Murakami Y (2006) Cardiac involvement in Kugelberg–Welander disease: a case report and review. Am J Med Sci 332:354–356
Asai H, Hirano M, Udaka F, Shimada K, Oda M, Kubori T, Nishinaka K, Tsujimura T, Izumi Y, Konishi N, Matsumoto S, Kameyama M, Ueno S (2007) Sympathetic disturbances increase risk of sudden cardiac arrest in sporadic ALS. J Neurol Sci 254:78–83
Araki A, Katsuno M, Suzuki K, Banno H, Suga N, Hashizume A, Mano T, Hijikata Y, Nakatsuji H, Watanabe H, Yamamoto M, Makiyama T, Ohno S, Fukuyama M, Morimoto S, Horie M, Sobue G (2014) Brugada syndrome in spinal and bulbar muscular atrophy. Neurology 82:1813–1821
Fang F, Chen H, Wirdefeldt K, Ronnevi LO, Al-Chalabi A, Peters TL, Kamel F, Ye W (2011) Infection of the central nervous system, sepsis and amyotrophic lateral sclerosis. PLoS One 6(12):e29749. doi:10.1371/journal.pone.0029749
Westendorp IC, Tiemessen MA, de Jong M, Soomers A, Wakelkamp IM, Boersma WG (2005) Moraxella catarrhalis sepsis in a patient with juvenile spinal muscle atrophy. Neth J Med 63:227–229
Rhodes A, Evans LE, Alhazzani W, Levy MM, Antonelli M, Ferrer R et al (2017) Surviving sepsis campaign: international guidelines for management of sepsis and septic shock: 2016. Intensive Care Med. doi:10.1007/s00134-017-4683-6
Fan SL, Miller NS, Lee J, Remick DG (2016) Diagnosing sepsis—the role of laboratory medicine. Clin Chim Acta 460:203–210
Chang YC, Huang CC, Huang SC, Hung FC (2008) Neonatal adrenoleukodystrophy presenting with seizure at birth: a case report and review of the literature. Pediatr Neurol 38:137–139
Brownstone E, Voigtländer T, Baumhackl U, Finsterer J (2013) Epilepsy in adult X-linked adrenoleucodystrophy due to the deletion c.1415-1416delAG in exon 5 of the ABCD1-gene. Gene 513:71–74
Sathasivam S (2008) Brown–Vialetto–Van Laere syndrome. Orphanet J Rare Dis 3:9. doi:10.1186/1750-1172-3-9
Rubboli G, Veggiotti P, Pini A, Berardinelli A, Cantalupo G, Bertini E, Tiziano FD, D’Amico A, Piazza E, Abiusi E, Fiori S, Pasini E, Darra F, Gobbi G, Michelucci R (2015) Spinal muscular atrophy associated with progressive myoclonic epilepsy: a rare condition caused by mutations in ASAH1. Epilepsia 56:692–698
Gan JJ, Garcia V, Tian J, Tagliati M, Parisi JE, Chung JM, Lewis R, Baloh R, Levade T, Pierson TM (2015) Acid ceramidase deficiency associated with spinal muscular atrophy with progressive myoclonic epilepsy. Neuromuscul Disord 25:959–963
Saouab R, Mahi M, Abilkacem R, Boumdin H, Chaouir S, Agader O, Amil T, Hanine A (2011) A case report of Sandhoff disease. Clin Neuroradiol 21:83–85
Lynch DS, Koutsis G, Tucci A, Panas M, Baklou M, Breza M, Karadima G, Houlden H (2016) Hereditary spastic paraplegia in Greece: characterisation of a previously unexplored population using next-generation sequencing. Eur J Hum Genet 24:857–863
Sauro KM, Wiebe S, Dunkley C, Janszky J, Kumlien E, Moshé S, Nakasato N, Pedley TA, Perucca E, Senties H, Thomas SV, Wang Y, Wilmshurst J, Jetté N (2016) The current state of epilepsy guidelines: a systematic review. Epilepsia 57:13–23
Goy ER, Carter J, Ganzini L (2008) Neurologic disease at the end of life: caregiver descriptions of Parkinson disease and amyotrophic lateral sclerosis. J Palliat Med 11:548–554
Luigetti M, Quaranta D, Conte A, Piccininni C, Lattante S, Romano A, Silvestri G, Zollino M, Sabatelli M (2013) Frontotemporal dementia, Parkinsonism and lower motor neuron involvement in a patient with C9ORF72 expansion. Amyotroph Lateral Scler Frontotemporal Degener 14:66–69
Konagaya M, Kato T, Sakai M, Kuru S, Matsuoka Y, Konagaya Y, Hashizume Y, Tabira T (2003) A clinical and pathological study of a Japanese case of Amyotrophic Lateral Sclerosis/Parkinsonism-dementia complex with family history. J Neurol 250:164–170
Kessler H, Prudlo J, Kraft S, Supprian T (2005) Dementia of frontal lobe type in Kennedy’s disease. Amyotroph Lateral Scler Other Motor Neuron Disord 6:250–253
Johnson WG, Cohen CS, Miranda AF, Waran SP, Chutorian AM (1980) Alpha-locus hexosaminidase genetic compound with juvenile gangliosidosis phenotype: clinical, genetic, and biochemical studies. Am J Hum Genet 32:508–518
Eirís J, Chabás A, Coll MJ, Castro-Gago M (1999) Late infantile and juvenile form of GM2-gangliosidosis variant B1. Rev Neurol 29:435–438
Fraidakis MJ, Brunetti M, Blackstone C, Filippi M, Chiò A (2016) Novel compound heterozygous spatacsin mutations in a greek kindred with hereditary spastic paraplegia SPG11 and dementia. Neurodegener Dis 16:373–381
Ramos-Ríos R, Berdullas J, Araúxo A, Santos-García D (2009) Schizophreniform psychosis at onset of adrenoleukodystrophy. CNS Spectr 14:711–712
Kopala LC, Tan S, Shea C, Orlik H, Vandorpe R, Honer WG (2000) Adrenoleukodystrophy associated with psychosis. Schizophr Res 45:263–265
Li JM, Rucker JC (2010) Irreversible optic neuropathy in wernicke encephalopathy and leber hereditary optic neuropathy. J Neuroophthalmol 30:49–53
Fassone E, Wedatilake Y, DeVile CJ, Chong WK, Carr LJ, Rahman S (2013) Treatable Leigh-like encephalopathy presenting in adolescence. BMJ Case Rep 2013:200838. doi:10.1136/bcr-2013-200838
Zdanowicz N, Mees L, Jacques D, Tordeurs D, Reynaert C (2014) Assessment and treatment of the risk of psychosis in adolescents—a review. Psychiatr Danub 26:115–121
Finsterer J, Bindu PS (2015) Therapeutic strategies for mitochondrial disorders. Pediatr Neurol 52:302–313
Caress JB, Ciarlone SL, Sullivan EA, Griffin LP, Cartwright MS (2016) Natural history of muscle cramps in amyotrophic lateral sclerosis. Muscle Nerve 53:513–517
Hanisch F, Skudlarek A, Berndt J, Kornhuber ME (2015) Characteristics of pain in amyotrophic lateral sclerosis. Brain Behav 5(3):e00296. doi:10.1002/brb3.296
Finsterer J, Soraru G (2016) Onset manifestations of spinal and bulbar muscular atrophy (Kennedy’s disease). J Mol Neurosci 58:321–329
Thomas PK, Young E, King RH (1989) Sandhoff disease mimicking adult-onset bulbospinal neuronopathy. J Neurol Neurosurg Psychiatry 52:1103–1106
Chu ML, Sala DA, Weiner HL (2001) Intrathecal baclofen in X-linked adrenoleukodystrophy. Pediatr Neurol 24:156–158
Lager C, Kroksmark AK (2015) Pain in adolescents with spinal muscular atrophy and Duchenne and Becker muscular dystrophy. Eur J Paediatr Neurol 19:537–546
Servelhere KR, Faber I, Saute JA, Moscovich M, D’Abreu A, Jardim LB, Teive HA, Lopes-Cendes I, Franca MC Jr (2016) Non-motor symptoms in patients with hereditary spastic paraplegia caused by SPG4 mutations. Eur J Neurol 23:408–411
Erlenwein J (2016) Management of acute pain therapy: guidelines, recommendations and current practice in german hospitals. Anasthesiol Intensivmed Notfallmed Schmerzther 51:40–48
Baldinger R, Katzberg HD, Weber M (2012) Treatment for cramps in amyotrophic lateral sclerosis/motor neuron disease. Cochrane Database Syst Rev 4:CD004157. doi:10.1002/14651858.CD004157.pub2
Radovanović S, Milićev M, Perić S, Basta I, Kostić V, Stević Z (2014) Gait in amyotrophic lateral sclerosis: is gait pattern differently affected in spinal and bulbar onset of the disease during dual task walking? Amyotroph Lateral Scler Frontotemporal Degener 15:488–493
Sanjak M, Hirsch MA, Bravver EK, Bockenek WL, Norton HJ, Brooks BR (2014) Vestibular deficits leading to disequilibrium and falls in ambulatory amyotrophic lateral sclerosis. Arch Phys Med Rehabil 95:1933–1939
Bouquet F, Dehais C, Sanson M, Lubetzki C, Louapre C (2015) Dramatic worsening of adult-onset X-linked adrenoleukodystrophy after head trauma. Neurology 85:1991–1993
Raymond GV, Seidman R, Monteith TS, Kolodny E, Sathe S, Mahmood A, Powers JM (2010) Head trauma can initiate the onset of adreno-leukodystrophy. J Neurol Sci 290:70–74
Kumakura M, Hara K, Obara G, Sata T (2015) A case of general anesthesia in a patient with spinal and bulbar muscular atrophy. Masui 64:1277–1279
Kindopp AS, Ashbury T (1998) Anaesthetic management of an adult patient with X-linked adrenoleukodystrophy. Can J Anaesth 45:990–992
Vai S, Bianchi ML, Moroni I, Mastella C, Broggi F, Morandi L, Arnoldi MT, Bussolino C, Baranello G (2015) Bone Spinal Muscular Atrophy. Bone 79:116–120
Zhou J, Yi J, Bonewald L (2015) Muscle-bone crosstalk in amyotrophic lateral sclerosis. Curr Osteoporos Rep 13:274–279
Sato Y, Honda Y, Iwamoto J (2006) Etidronate for fracture prevention in amyotrophic lateral sclerosis: a randomized controlled trial. Bone 39:1080–1086
Oliver D (2004) Ventilation in motor neuron disease: difficult decisions in difficult circumstances. Amyotroph Lateral Scler Other Motor Neuron Disord 5:6–8
EFNS Task Force on Diagnosis and Management of Amyotrophic Lateral Sclerosis, Andersen PM, Abrahams S, Borasio GD, de Carvalho M, Chio A, Van Damme P, Hardiman O, Kollewe K, Morrison KE, Petri S, Pradat PF, Silani V, Tomik B, Wasner M, Weber M (2012) EFNS guidelines on the clinical management of amyotrophic lateral sclerosis (MALS)–revised report of an EFNS task force. Eur J Neurol 19:360–375
Heritier Barras AC, Adler D, Iancu Ferfoglia R, Ricou B, Gasche Y, Leuchter I, Hurst S, Escher M, Pollak P, Janssens JP, CeSLA Group (2013) Is tracheostomy still an option in amyotrophic lateral sclerosis? Reflections of a multidisciplinary work group. Swiss Med Wkly 143:w13830
Bahus MK, Steen PA, Førde R (2012) Law, ethics and clinical judgment in end-of-life decisions–how do Norwegian doctors think? Resuscitation 83:1369–1373
Ait-El-Mkadem S, Chaussenot A, Bannwarth S, Rouzier C, Paquis-Flucklinger V, CHCHD10-Related Disorders (2015) In: Pagon RA, Adam MP, Ardinger HH, Wallace SE, Amemiya A, Bean LJH, Bird TD, Fong CT, Mefford HC, Smith RJH, Stephens K (eds) GeneReviews® [Internet]. University of Washington, Seattle, 1993–2016. http://www.ncbi.nlm.nih.gov/books/NBK304142/. Accessed Sept 2016
Finsterer J (2002) Mitochondriopathy as a differential diagnosis of amyotrophic lateral sclerosis. Amyotroph Lateral Scler Other Motor Neuron Disord 3:219–224
Lee JS, Hwang JS, Ryu KH, Lee EH, Kim SH (2007) Mitochondrial respiratory complex I deficiency simulating spinal muscular atrophy. Pediatr Neurol 36:45–47
Acknowledgements
No funding was received.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All applicable international, national, and/or institutional guidelines for the care of patients were followed.
Statement of human and animal rights
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Finsterer, J., Stöllberger, C. Emergencies in motoneuron disease. Intern Emerg Med 12, 641–650 (2017). https://doi.org/10.1007/s11739-017-1644-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11739-017-1644-6