Abstract
Objective
To assess the effects of direct moxibustion on 24-hour ambulatory blood pressure (ABP) and clinical symptoms of traditional Chinese medicine (TCM) in elderly patients with essential hypertension, and to explore the antihypertensive effect and influencing factors of moxibustion.
Methods
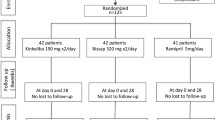
A total of 101 elderly hypertension patients who met the inclusion criteria were randomly assigned to a direct moxibustion I group (n=33), a direct moxibustion II group (n=34), and a control group (n=34). The treatment of calcium antagonist (CCB) or angiotensin II receptor antagonist (ARB) was adopted in the control group. The treatment of direct moxibustion I plus the same medicine as the control group were adopted in the direct moxibustion I group, five cones per acupoint and three times per week, for 5 weeks in total. The treatment of direct moxibustion II plus the same medicine as the control group were adopted in the direct moxibustion II group, five cones per acupoint and three times per week, for 5 weeks in total. The changes of 24-hour ABP and clinical symptoms of TCM after treatment were compared in the three groups.
Results
The mean 24-hour ambulatory systolic blood pressure (mean 24 h ASBP), night ASBP, percentage of mean 24-hour ambulatory diastolic blood pressure (mean 24 h ADBP)>90 mmHg, and percentage of day ADBP>90 mmHg in the control group were elevated after treatment (P<0.05). The percentage of night ADBP>80 mmHg in the direct moxibustion I group was reduced by treatment (P<0.01). There were no significant differences in the other outcome measures of 24 h ABP, such as day ASBP, percentage of mean 24 h ASBP>140 mmHg, percentage of day ASBP>140 mmHg, percentage of night ASBP>120 mmHg, mean 24 h ADBP, day ADBP, night ADBP, 24 h ambulatory pulse pressure (APP), after treatment in all groups (P>0.05). The degree of improvement of the clinical symptoms of TCM showed significant differences among the three groups of patients (P<0.01). The total effective rate in the direct moxibustion I group was 73.3%, which was superior to those in the direct moxibustion II group and control group (13.3% and 10.0%, respectively).
Conclusion
The direct moxibustion has benign regulative effect on blood pressure of elderly patients with essential hypertension, and improves their clinical symptoms. The direct moxibustion method I (burning the next moxa cone after the previous one had totally burnt out) was superior to method II (burning the next moxa cone when the previous one had not totally burnt out ) in lowering blood pressure and improving symptoms of elderly patients with essential hypertension.
摘要
目的
观察直接灸对老年原发性高血压患者24 小时动态血压、中医临床症状的影响, 探讨中医灸法的降压作用与影响因素。
方法
将符合纳入标准的101 例老年高血压患者随机分入直接灸I 组(33 例)、直接灸II 组(34 例)和对照组(34 例)。对照组采用钙拮抗剂(calcium antagonist, CCB)或血管紧张素II 受体拮抗剂(angiotensin IIreceptor antagonist, ARB)治疗, 连续5 星期。直接灸I 组采用直接灸I 配合药物治疗, 每穴5 壮, 每星期3 次, 5 星期为1 疗程。直接灸II 组采用直接灸II 配合药物治疗, 每穴5 壮, 每星期3 次, 5 星期为1 疗程。观察治疗前后3组患者中医临床症状的变化, 检测24 小时动态血压(ambulatory blood pressure, ABP)
结果
与治疗前比较, 对照组治疗后24 小时平均收缩压 (mean 24-hour ambulatory systolic blood pressure, mean 24 h ASBP)、夜间ASBP、24小时平均舒张压(mean 24-hour ambulatory diastolic blood pressure, mean 24 h ADBP)>90 mmHg 百分比与白昼ADBP>90 mmHg 百分比上升均有统计学差异(均P<0.05)。与治疗前比较, 直接灸I 组治疗后夜间ADBP>80 mmHg百分比明显降低 (P<0.01); 其余24 小时动态血压观察指标[日间ASBP、mean 24 h ASBP>140 mmHg 百分比、日间ASBP>140 mmHg 百分比、夜间 ASBP>120 mmHg 百分比、24 h mean ADBP、日间ADBP、夜间 ADBP 及24 小时动态脉压(ambulatory pulse pressure, APP)], 各组治疗前后比较均无统计学差异(P>0.05)。直接灸I 组总有效率为73.3%, 直接灸II 组总有效率为13.3%, 对照组总有效率为10.0%, 3 组患者中医临床症状改善情况有统计学差异(P<0.01)。
结论
直接灸对老年原发性高血压患者的血压具有良性调节作用, 能够改善患者的临床症状。直接灸方法I (艾炷燃尽后再续灸下1 壮)对老年原发性高血压患者血压和症状的改善作用优于直接灸方法II(不待艾炷燃尽就迅速熄灭艾炷, 续灸下1 壮)。
Similar content being viewed by others
References
Revision Committee for Clinical Practice Guidelines for the Management of Hypertension in the Community. Clinical practice guidelines for the management of hypertension in the community (2014 revised edition) Linchuang Huicui, 2015, 30(7): 725–744.
Wang J, Zhang L, Wang F, Liu L, Wang H. China National Survey of Chronic Kidney Disease Working Group. Prevalence, awareness, treatment, and control of hypertension in China: results from a national survey. Am J Hypertens, 2014, 27(11): 1355–1361.
Tomasik T, Gryglewska B, Windak A, Grodzicki T. Hypertension in the elderly: how to treat patients in 2013? The essential recommendations of the Polish guidelines. Pol Arch Med Wewn, 2013, 123(7-8): 409–416.
Gao Y, Chen G, Tian H, Lin L, Lu J, Weng J, Jia W, Ji L, Xiao J, Zhou Z, Ran X, Ren Y, Chen T, Yang W. China National Diabetes and Metabolic Disorders Study Group. Prevalence of hypertension in China: a cross-sectional study. PLoS One, 2013, 8(6): e65938.
Whitworth JA. World Health Organization, International Society of Hypertension Writing Group. 2003 World Health Organization (WHO)/International Society of Hypertension (ISH) statement on management of hypertension. J Hypertens, 2003, 21(11): 1983–1992.
Chobanian AV, Bakris GL, Black HR, Cushman WC, Green LA, Izzo JL Jr, Jones DW, Materson BJ, Oparil S, Wright JT Jr, Roccella EJ. National Heart, Lung, and Blood Institute Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure. National High Blood Pressure Education Program Coordinating Committee. The seventh report of the joint national committee on prevention, detection, evaluation, and treatment of high blood pressure: the JNC 7 report. JAMA, 2003, 89(19): 2560–2572.
Ministry of Health of the People’s Republic of China. Guiding Principles for Clinical Study of New Chinese Medicines. Beijing: China Medical Science Press, 2002: 76–77.
Wu HG, Liu HR, Ma XP, Shi Y. Moxibustion. Shanghai: Shanghai Science and Technology Publishing House, 2016: 59.
Wang LL. The clinical characteristics and suitable diseases of grain-sized moxibustion. Shanghai Zhenjiu Zazhi, 2013, 32(11): 889–891.
Zhou P, Wang LL, Zhang JB. Cheng Dan-an’s contribution to direct moxibustion with moxa cone in Chinese Acupuncture and Moxibustion. Zhongguo Zhen Jiu, 2014, 34(4): 409–412.
Yang CS, Zhang JB. Moxibustion characteristics of Dan’an Cheng and his experience of clinical applications. Jiangsu Zhongyiyao, 2016, 48(1): 5–8.
Han XJ. Chinese medical diagnosis and treatment project of hypertension (first draft). Zhonghua Zhongyiyao Zazhi, 2008, 23(7): 611–613.
Zhang RZ, Chen ZX, Hu SY, Zheng YJ, Zhou ML. Clinical investigation of the composition of TCM syndromes in 3 578 hypertension patients. Zhongyiyao Linchuang Zazhi, 2007, 19(4): 360–364.
Wang LY, Li Y, Li N, Ding Y, Shi NN, Han XJ. Study on TCM syndrome distribution of 1 508 cases of hypertension patients with clinical epidemiology. Zhonghua Zhongyiyao Zazhi, 2010, 5(12): 1960–1963.
Zhu YB, Wang Q, Deng QW, Cai J, Song XH, Yan X. Relationships between constitutional types of traditional Chinese medicine and hypertension. CJIM, 2010, 8(1): 40–45.
Zhong JB. Research on TCM names, etiology, pathogenesis, and differentiation of essential hypertension by the experience of TCM physicians. Shijie Zhongxiyi Jiehe Zazhi, 2009, 4(12): 843–846.
Peng LH, Feng LM, Chen ZF, Cai W, Yang CY, Zhang J, Xie M, Yang D. Effects of moxibustion on blood pressure, NO, ET, SOD and MDA in patients with hypertension. Zhongguo Zhen Jiu, 2004, 24(3): 157–159.
Wang X, Wu HL, Li XQ. Antihypertensive effect of acupuncture at Taichong (LR 3) on ambulatory blood pressure. Xin Zhongyi, 2007, 39(11): 21–22.
Luo WJ, Jiang YG, Liu J, Wu HL, Wang X. Clinical efficacy of treating patients with hypertension and anxiety states by acupuncture. Zhongyi Linchuang Yanjiu, 2012, 4(12): 44–45.
Yang DH. Effect of electroacupuncture at Quchí (LI 11) and Taichong (LR 3) on blood pressure variability in young patients with hypertension. World J Acupunct Moxibustion, 2011, 21(1): 8–12.
Wu QM, Feng GX, Tang XF. Effects of acupuncture at Siguan points plus warming acupuncture-moxibustion at Baihui (GV 20) on plasma ET and NO in patients with essential hypertension. Zhongguo Zhen Jiu, 2004, 24(1): 53–55.
He CG, Long HH, Cai SC, Fei AH, Xu TF, Zhu CF, Qin XF, Wang L. Discussion on the influence factors of moxibustion therapy. Zhongyi Xuebao, 2015, 30(9): 1373–1376.
Wu HG, Ma XP, Zhou CL, Bao CH, Dou CZ. Research situation and the strategic thinking of moxibustion. Shijie Zhongyiyao, 2013, 8(8): 845–851.
Wang XJ, Wang LL, Zhang JB. Quantity regulation in grain moxibustion. Shanghai Zhenjiu Zazhi, 2013, 32(6): 426–429.
Hu ZH, Wang Y, Wang SS, Wu Z, Jin XX, Xu JH, Zhang JJ, Bai ZJ, Lu Q. Dose-response study on partitioned moxibustion in intervening insulin resistance. Shanghai Zhenjiu Zazhi. 2016, 35(2): 146–148.
Kou ST, Wu HG, Liu HR, Chen YL, Liu LG, Chen YF, Chen HP, Wang SY, Hua XG, Zhou EH. Research of moxibustion quantity and significance. Zhonghua Zhongyiyao Xuekan, 2008, 26(5): 935–937.
Author information
Authors and Affiliations
Corresponding authors
Rights and permissions
About this article
Cite this article
Lee, Eh., Zhou, Cl., Zhao, Tp. et al. Effect of direct moxibustion on blood pressure and clinical symptoms in elderly patients with essential hypertension. J. Acupunct. Tuina. Sci. 14, 73–81 (2016). https://doi.org/10.1007/s11726-016-0904-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11726-016-0904-8
Keywords
- Moxibustion Therapy
- Direct Moxibustion
- Moxa Cone Moxibustion
- Hypertension, Essential
- Blood Pressure Monitoring, Ambulatory
- Aged