Abstract
Background
GERD and Achalasia are two known complications after sleeve gastrectomy. Treatment towards each of these complications varies and requires a tailored approach.
Methods
We present a 55-year-old female with class II obesity and a previous history of sleeve gastrectomy who developed significant gastroesophageal reflux disease refractory to medical management. After a covid infection in fall of 2020, she began to report new symptoms of dysphagia that progressed from solids to liquids. She underwent extensive workup including upper endoscopy, upper GI barium swallow, manometry, pH impedence, and EndoFlip leading to a diagnosis of Achalasia type II as well as a paraesophageal hernia.
Results
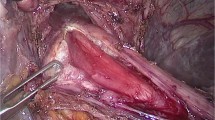
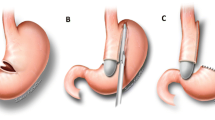
Given these findings, she underwent a combined paraesophageal hernia repair with conversion of sleeve gastrectomy to Roux-en-Y gastric diversion and an intra-operative peroral endoscopic myotomy. Intraoperatively, she was noted to have significant lower abdominal adhesions leading to performing the Roux-en-Y reconstruction through a supramesocolic defect in a retrocolic fashion.
Conclusions
While the development of heartburn and achalasia after sleeve gastrectomy is rare, it requires interventions dedicated towards each etiology. This case demonstrates treatment of both these symptoms is feasible in a single operation.
Similar content being viewed by others
References
Alalwan AA, Friedman J, Park H, Segal R, Brumback BA, Hartzema AG. US national trends in bariatric surgery: a decade of study. Surgery. 2021;170(1):13–7. https://doi.org/10.1016/j.surg.2021.02.002.
Yeung KTD, Penney N, Ashrafian L, Darzi A, Ashrafian H. Does sleeve gastrectomy expose the distal esophagus to severe reflux?: A systematic review and meta-analysis. Ann. Surg. 2020;271:257–65. https://doi.org/10.1097/SLA.0000000000003275.
Crafts TD, Lyo V, Rajdev P, Wood SG. Treatment of achalasia in the bariatric surgery population: a systematic review and single-institution experience. Surg. Endosc. 2021;35(9):5203–16. https://doi.org/10.1007/s00464-020-08015-3.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics Approval and Consent to Participate
This article does not contain any studies with human participants or animals performed by any of the authors. Informed Consent does not apply.
Competing Interests
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Key points
• Gastroesophageal reflux disease (GERD) and achalasia are known complications after sleeve gastrectomy (SG) and require different therapeutic interventions
• Myotomy for achalasia cannot be followed by fundoplication in the post-SG patient, and alternative interventions to reduce risk of GERD are needed
• Conversion to Roux-en-Y Gastric bypass (RYGB) is an accepted operative choice for patients with GERD and history of SG
Supplementary Information
Below is the link to the electronic supplementary material.
Supplementary file1 (MP4 384 MB)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Slack, D., Colavita, P. & Nimeri, A. Laparoscopic Paraesophageal Hernia (PEH) Repair, Roux-en-Y Gastric Bypass, and Per Oral Endoscopic Myotomy (POEM) in a Patient with Achalasia After Sleeve Gastrectomy. OBES SURG 33, 1955–1956 (2023). https://doi.org/10.1007/s11695-023-06623-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-023-06623-1