Abstract
Background
Long-term failure after Roux-en-Y gastric bypass (RYGB) is well known and occurs in 10–15% of patients according to the literature. Causes are multifactorial and dilatation of the gastro-jejunal anastomosis (GJA) is only one of these. A transoral outlet reduction (TORe) with endoscopic sutures to reinstall more restriction could be a valid and safe alternative to reduce regained weight after failed gastric bypass surgery. The objective of this article is to describe our single-center experience and discuss the adverse events of the technique.
Objectives
To describe our single-center case series and adverse events after TORe for weight regain after RYGB.
Methods
We report a case series of 20 patients referred due to weight regain after RYGB with a dilated GJA. TORe was performed using an endoscopic full-thickness suture device (Apollo OverStitch®) to reduce the diameter of the GJA and the volume of the gastric reservoir. Prospectively collected data on technical feasibility, safety and efficacy are described with a median follow-up of 22 (6–38) months.
Results
Mean BMI was 44.5 kg/m2 at the time of RYGB. Postoperative nadir BMI was 27,7 kg/m2. The average time to TORe was 12.1 years after initial RYGB. Patients regained a mean 45.9% of excess body weight loss (EWL) before TORe and had a mean preprocedural BMI of 35.3 kg/m2. The aim was to reduce the aperture of the GJA to 5 mm which was done with a mean of 1.7 sutures and 3.5 stitches. The mean absolute weight loss was 13 kg and BMI reduction was 3.9 kg/m2 after 6 months. After a median follow-up of 22 months, a BMI of 31.4 kg/m2 was observed. Dumping symptoms resolved in four of our patients 6 weeks after TORe. Procedural adverse events were nausea and vomiting, sore throat, mild transient abdominal pain, diarrhea and constipation. All of them were treated conservatively. Due to a lack of weight loss, a suture failure was assumed in two of our patients. We describe one case of postprocedural mediastinitis, presumably due to a distal esophageal perforation, treated with a laparoscopic drainage without clinical evidence for perforation.
Conclusions
Endoscopic TORe by narrowing the dilated GJA appears to be an efficient and safe minimal invasive option to tackle weight regain after RYGB and should be more used in clinical practice.
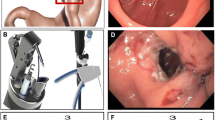
Graphical Abstract





Similar content being viewed by others
Abbreviations
- RYGB:
-
Roux-en-Y gastric bypass
- TORe:
-
Transoral outlet reduction
- GJA:
-
Gastrojejunal anastomosis
- AE:
-
Adverse event
- APMC:
-
Argon plasma mucosal coagulation
- %EBWL:
-
Percent excess body weight loss
- TWL:
-
Total weight loss
References
Buchwald H, Oien DM. Metabolic/bariatric surgery worldwide 2011. Obes Surg. 2013;23(4):427–36. https://doi.org/10.1007/s11695-012-0864-0.
Arterburn DE, Olsen MK, Smith VA, et al. Association between bariatric surgery and long-term survival. JAMA - J Am Med Assoc. 2015;313(1):62–70. https://doi.org/10.1001/jama.2014.16968.
Welbourn R, Hollyman M, Kinsman R, et al. Bariatric surgery worldwide: baseline demographic description and one-year outcomes from the Fourth IFSO Global Registry Report 2018. Obes Surg. 2019;29(3):782–95. https://doi.org/10.1007/s11695-018-3593-1.
Angrisani L, Santonicola A, Iovino P, et al. Bariatric surgery worldwide 2013. Obes Surg. 2015;25(10):1822–32. https://doi.org/10.1007/s11695-015-1657-z.
Adams TD, Davidson LE, Litwin SE, et al. Weight and metabolic outcomes 12 years after gastric bypass. N Engl J Med. 2017;377(12):1143–55. https://doi.org/10.1056/nejmoa1700459.
Sjöström L, Narbro K, Sjöström CD, et al. Effects of bariatric surgery on mortality in Swedish obese subjects. N Engl J Med. 2007;357(8):741–52. https://doi.org/10.1056/nejmoa066254.
Nicoletti CF, de Oliveira BAP, de Pinhel MAS, et al. Influence of excess weight loss and weight regain on biochemical indicators during a 4-year follow-up after Roux-en-Y gastric bypass. Obes Surg. 2015;25(2):279–84. https://doi.org/10.1007/s11695-014-1349-0.
Changela K. Peroral endoscopic reduction of dilated gastrojejunal anastomosis after bariatric surgery: techniques and efficacy. World J Gastrointest Endosc. 2016;8(4):239. https://doi.org/10.4253/wjge.v8.i4.239.
Callahan ZM, Su B, Kuchta K, et al. Five-year results of endoscopic gastrojejunostomy revision (transoral outlet reduction) for weight gain after gastric bypass. Surg Endosc. 2020;34(5):2164–71. https://doi.org/10.1007/s00464-019-07003-6.
Kumar N, Thompson CC. Transoral outlet reduction for weight regain after gastric bypass: long-term follow-up. Gastrointest Endosc. 2016;83(4):776–9. https://doi.org/10.1016/j.gie.2015.08.039.
Conaty EA, Novak S, Avitia R, et al. Endoscopic gastrojejunal revision (transoral outlet reduction) for persistent hypoglycemia after gastric bypass. Obes Surg. 2019;29(11):3773–5. https://doi.org/10.1007/s11695-019-04113-x.
Kumar N. Weight loss endoscopy: development, applications, and current status. World J Gastroenterol. 2016;22(31):7069–79. https://doi.org/10.3748/wjg.v22.i31.7069.
Jaruvongvanich V, Vantanasiri K, Laoveeravat P, et al. Endoscopic full-thickness suturing plus argon plasma mucosal coagulation versus argon plasma mucosal coagulation alone for weight regain after gastric bypass: a systematic review and meta-analysis. Gastrointest Endosc. 2020;92(6):1164-1175.e6. https://doi.org/10.1016/j.gie.2020.07.013.
Relly R, Mati S, Cohen Aviv N, et al. Endoscopic trans-oral outlet reduction after bariatric surgery is safe and effective for dumping syndrome. Surg Endosc. 1234;35:6846–6852. https://doi.org/10.1007/s00464-020-08190-3.
Jirapinyo P, Kumar N, AlSamman MA, et al. Five-year outcomes of transoral outlet reduction for the treatment of weight regain after Roux-en-Y gastric bypass. Gastrointest Endosc. 2020;91(5):1067–73. https://doi.org/10.1016/j.gie.2019.11.044.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Key points
• Dilation of the gastrojejunal anastomosis is a possible mechanism of weight regain
• Reducing the anastomosis leads to weight loss
• Mean loss of 13 kg after TORe procedure
• Resolution of dumping symptoms after TORe
Supplementary Information
Below is the link to the electronic supplementary material.
Supplementary file1 (MP4 132344 KB)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Vansteenbrugge, L., Strypstein, S., Biglari, M. et al. Transoral Outlet Reduction to Tackle Weight Regain After Roux-en-Y Gastric Bypass: a Single Center Initial Experience. OBES SURG 33, 1646–1651 (2023). https://doi.org/10.1007/s11695-023-06580-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-023-06580-9