Abstract
Background
Minimization of opiate use is an important focus in the setting of the severe national opioid crisis. This study evaluated the role of liposomal bupivacaine (LB) in decreasing postoperative opioid use before and after implementation of a bariatric enhanced recovery after surgery (ERAS) program.
Methods
We performed an IRB-approved, prospective, double-blind, randomized controlled trial of LB versus plain bupivacaine (PB) in patients undergoing elective, minimally invasive, weight loss surgery at a comprehensive metabolic and bariatric surgery program from November 2017 to December 2019. Primary outcomes were postoperative morphine milligram equivalents per day (MME/day) and average subjective inpatient pain level. Secondary outcomes were length of hospital stay (LOS) and adverse events (AEs).
Results
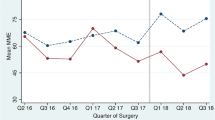
Of the 100 patients enrolled, 78 were randomly assigned to LB (42) or PB (36). Thirty-four received the ERAS protocol, and 44 did not. The mean MME/day use did not differ significantly by the bupivacaine group [median, IQR PB: 20.3 (40.95); LB: 33.0 (42.9); p = .314], but it did differ by the ERAS group [median, IQR no ERAS 33.2 (47.1), ERAS 24.0 (34.0); p = .049]. Length of stay, inpatient pain score, and AEs did not differ significantly by either the bupivacaine or the ERAS group.
Conclusions
In our study, liposomal bupivacaine did not significantly decrease postoperative opioid use either before implementation of ERAS or as part of an enhanced recovery after surgery program for minimally invasive bariatric surgery procedures.
Graphical Abstract


Similar content being viewed by others
Data Availability
Data is available upon request for the methods and materials related to this project.
References
Wilson N, Kariisa M, Seth P, et al. Drug and opioid-involved overdose deaths — United States, 2017–2018. MMWR Morb Mortal Wkly Rep. 2020;69(11):290–7. https://doi.org/10.15585/mmwr.mm6911a4.
Wick EC, Grant MC, Wu CL. Postoperative multimodal analgesia pain management with nonopioid analgesics and techniques: a review. JAMA Surg. 2017;152(7):691–7. https://doi.org/10.1001/jamasurg.2017.0898.
Bray MS, Appel AL, Kallies KJ, et al. Implementation of an enhanced recovery after surgery program for colorectal surgery at a community teaching hospital. Wis Med J. 2017;116(1):22–6.
King AB, Spann MD, Jablonski P, et al. An enhanced recovery program for bariatric surgical patients significantly reduces perioperative opioid consumption and postoperative nausea. Surg Obes Relat Dis. 2018;14(6):849–56. https://doi.org/10.1016/j.soard.2018.02.010.
Thorell A, MacCormick AD, Awad S, et al. Guidelines for perioperative care in bariatric surgery: Enhanced Recovery After Surgery (ERAS) society recommendations. World J Surg. 2016;40(9):2065–83. https://doi.org/10.1007/s00268-016-3492-3.
Moncada R, Martinaitis L, Landecho M, et al. Does preincisional infiltration with bupivacaine reduce postoperative pain in laparoscopic bariatric surgery? Obes Surg. 2016;26(2):282–8. https://doi.org/10.1007/s11695-015-1761-0.
Bamgbade OA, Oluwole O, Khaw RR. Perioperative analgesia for fast-track laparoscopic bariatric surgery. Obes Surg. 2017;27(7):1828–34. https://doi.org/10.1007/s11695-017-2562-4.
Dumlu EG, Tokaç M, Öcal H, et al. Local bupivacaine for postoperative pain management in thyroidectomized patients: a prospective and controlled clinical study. Turkish J Surg. 2016;32(3):173–7. https://doi.org/10.5152/UCD.2015.3138.
Cohen SM, Vogel JD, Marcet JE, et al. Liposome bupivacaine for improvement in economic outcomes and opioid burden in GI surgery: IMPROVE study pooled analysis. J Pain Res. 2014;7:359–66. https://doi.org/10.2147/JPR.S63764.
Highlights of Prescribing Information: Exparel (bupivicaine liposome injectable suspension); 2021. Revised: 3/2022. https://www.exparel.com/hcp/prescribing-information.pdf.
Robertson TC, Hall K, Bear S, et al. Transversus abdominis block utilizing liposomal bupivacaine as a non-opioid analgesic for postoperative pain management. Surg Endosc. 2019;33(8):2657–62. https://doi.org/10.1007/s00464-018-6543-z.
Bhakta A, Glotzer O, Ata A, et al. Analgesic efficacy of laparoscopic-guided transverse abdominis plane block using liposomal bupivacaine in bariatric surgery. Am J Surg. 2018;215(4):643–6. https://doi.org/10.1016/j.amjsurg.2017.09.006.
Knudson RA, Dunlavy PW, Franko J, et al. Effectiveness of liposomal bupivacaine in colorectal surgery: a pragmatic nonsponsored prospective randomized double blinded trial in a community hospital. Dis Colon Rectum. 2016;59(9):862–9. https://doi.org/10.1097/DCR.0000000000000648.
Nadeau MH, Saraswat A, Vasko A, et al. Bupivacaine versus liposomal bupivacaine for postoperative pain control after augmentation mammaplasty: a prospective, randomized, double-blind trial. Aesthetic Surg J. 2016;36(2):NP47–52. https://doi.org/10.1093/asj/sjv149.
Knight RB, Walker PW, Keegan KA, et al. A randomized controlled trial for pain control in laparoscopic urologic surgery: 0.25% bupivacaine versus long-acting liposomal bupivacaine. J Endourol. 2015;29(9):1019–24. https://doi.org/10.1089/end.2014.0769.
Parascandola SA, Ibañez J, Keir G, et al. Liposomal bupivacaine versus bupivacaine/epinephrine after video-assisted thoracoscopic wedge resection. Interact Cardiovasc Thorac Surg. 2017;24(6):925–30. https://doi.org/10.1093/icvts/ivx044.
Redan J, Wells T, Reeder S, et al. Reducing opioid adverse events: a safe way to improve outcomes. Surg Technol Int. 2016;28:101–9.
Vyas KS, Rajendran S, Morrison SD, et al. Systematic review of liposomal bupivacaine (Exparel) for postoperative analgesia. Plast Reconstr Surg. 2016;138(4):748e-e756. https://doi.org/10.1097/PRS.0000000000002547.
Smith TW, Wang X, Singer MA, et al. Enhanced recovery after surgery: a clinical review of implementation across multiple surgical subspecialties. Am J Surg. 2020;219(3):530–4. https://doi.org/10.1016/j.amjsurg.2019.11.009.
McCann ME. Effective, cost-effective, or (just) costly? Anesthesiol. 2021;134(2):139–42. https://doi.org/10.1097/ALN.0000000000003658.
Hussain N, Brull R, Sheehy B, et al. Perineural liposomal bupivacaine is not superior to nonliposomal bupivacaine for peripheral nerve block analgesia. Anesthesiol. 2021;134(2):147–64. https://doi.org/10.14097/ALN.0000000000003651.
Cook KF, Kallen MA, Buckenmaier C, et al. Evaluation of the validity and response burden of patient self-report measures of the pain assessment screening tool and outcomes registry (Pastor). Mil Med. 2017;182(7):e1851–61. https://doi.org/10.7205/MILMED-D-16-00285.
Hodges JL, Lehmann EL. Estimates of location based on rank tests. Ann Math Stat. 1963;34(598):611.
IBM Corp. Released 2021. IBM SPSS Statistics for Windows, Version 28.0. Armonk, NY: IBM Corp.
NCSS/PASS 2016 Statistical Software (2016). NCSS, LLC.
Microsoft Corporation. (2021). Microsoft Excel. Retrieved from https://office.microsoft.com/excel.
Trotta M, Ferrari C, D’Alessandro G, et al. Enhanced recovery after bariatric surgery (ERABS) in a high-volume bariatric center. Surg Obes Relat Dis. 2019;15(10):1785–92. https://doi.org/10.1016/j.soard.2019.06.038.
Nagliati C, Contin R, Pennisi D. Considering ERAS protocols as a part of multimodal analgesia in bariatric surgery. J Clean Prod. 2020;16(12):2132–3. https://doi.org/10.1016/j.soard.2020.05.011.
Małczak P, Pisarska M, Piotr M, et al. Enhanced recovery after bariatric surgery: systematic review and meta-analysis. Obes Surg. 2017;27(1):226–35. https://doi.org/10.1007/s11695-016-2438-z.
Schwartz AR. Reduction in opioid use and postoperative pain scores after elective laparotomy with implementation of enhanced recovery after surgery protocol on a gynecologic oncology service. Int J Gynecol Cancer. 2019;29(5):935–43. https://doi.org/10.1136/ijgc-2018-000131.
Ma P, Lloyd A, McGrath M, et al. Reduction of opioid use after implementation of enhanced recovery after bariatric surgery (ERABS). Surg Endosc. 2020;34(5):2184–90. https://doi.org/10.1007/s00464-019-07006-3.
Dunkman WJ, Manning MW. Enhanced recovery after surgery and multimodal strategies for analgesia. Surg Clin North Am. 2018;98(6):P1171–84. https://doi.org/10.1016/j.suc.2018.07.005.
Simpson JC, Bao X, Agarwala A. Pain management in enhanced recovery after surgery (ERAS) protocols. Clin Colon Rectal Surg. 2019;32(2):121–8. https://doi.org/10.1055/s-0038-1676477.
Baessler AM, Moor M, Conrad DJ, et al. Single-shot liposomal bupivacaine reduces postoperative narcotic use following outpatient rotator cuff repair: a prospective, double-blinded, randomized controlled trial. J Bone Joint Surg Am. 2020;102(22):1985–92. https://doi.org/10.2106/JBJS.20.00225.
Mattson CL, Tanz LJ, Quinn K, et al. Morbidity and mortality weekly report trends and geographic patterns in drug and synthetic opioid overdose deaths-United States, 2013-2019. Morb Mortal Wkly Rep. 2021;70(6):202-207. https://www.cdc.gov/nchs/data/nvsr/nvsr61/
Ljungqvist O, Scott M, Fearon KC. Enhanced recovery after surgery a review. JAMA Surg. 2017;152(3):292–8. https://doi.org/10.1001/jamasurg.2016.4952.
Acknowledgements
The authors would like to express our appreciation for the support of the inpatient Pharmacy Department and, particularly, the persistent support provided by Pharmacist Yuet H. Lam. All individuals in acknowledgements have given written permission to be named.
Author information
Authors and Affiliations
Contributions
All authors have contributed equally to this work.
Corresponding author
Ethics declarations
Ethical Approval
All procedures performed in this study that involved human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed Consent Statement
Informed consent was obtained from all individual participants included in this study.
Conflict of Interest
The authors declare no competing interests.
Disclaimer
The views expressed in this article reflect the results of research conducted by the authors and do not necessarily reflect the official policy or position of the Department of the Navy, Department of Defense, nor the United States Government.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Copyright Statement
Military services members are authors of this work that was prepared as part of official duties. Title 17 U.S.C 105 provides that “copyright protection under this title is not available for any work of the United States Government.” Title 17 U.S.C 230 101 defines a US Government work as work prepared by a military service member or employee of the US Government as part of that person’s official duties.
Recognition
• Poster presentation of early data during Obesity Week 2019.
• Poster presentation of complete data during ASMBS conference 2021.
• Podium presentation at the Navy Medicine Readiness & Training Command, San Diego regional Academic Research Competition 2021—Awarded: 1st place in Resident Category.
• Podium presentation at the US Navy-wide research competition 2021—Awarded: finalist.
Key Points
• The opioid crisis demands multimodal pain management of postoperative patients.
• Enhanced recovery after bariatric surgery protocols are widely adopted.
• Long-acting bupivacaine use in the setting of an ERAS has minimal benefit.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Becker, E., Hernandez, A., Greene, H. et al. Does Liposomal Bupivacaine Decrease Postoperative Opioid Use in Conjunction with an Enhanced Recovery After Bariatric Surgery Pathway? A Prospective, Double-blind, Randomized Controlled Trial. OBES SURG 33, 555–561 (2023). https://doi.org/10.1007/s11695-022-06417-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-022-06417-x