Abstract
Purpose
Obesity is associated with increased cardiovascular risk. Bariatric surgery (BS) improves the clinical and metabolic profile. Retinal caliber changes could precede cardiovascular events. Different studies have shown an improvement in retinal caliber after BS. The aim of this study was to examine retinal caliber and other cardiovascular target organ damage before and after BS.
Materials and Methods
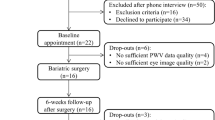
Monocentric, prospective cohort study at the Montpellier University Hospital. Biologic features, vessel stiffness, echocardiograph variables, and retinal caliber at baseline and 6 and 12 months were assessed in consecutive patients with class 2 or 3 obesity undergoing BS. A mixed linear model adjusted for age and sex was used.
Results
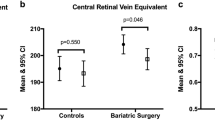
We included 88 patients (75 women). The mean (SD) age was 43 years (11) and mean (SD) baseline weight 117 (21) Kg. Mean changes in the first year after BS were − 5.1 µm in central retinal vein equivalent (CRVE) (p < 0.0001), + 0.02 in arteriole-to-venule ratio (AVR) (p < 0.0001), − 1.4 mmol/L in glycemia (p < 0.0001), − 1.0 mg/L in natural logarithm of C-reactive protein (p < 0.0001), and − 54.0 g in left ventricular mass (p = 0.0005). We observed no significant improvement in arterial stiffness markers. Predictors of improvement in CRVE were high baseline weight (p = 0.030), male sex (p = 0.025), and no diabetes history (p Dynamic links between variations
= 0.047).
Conclusion
The retinal microvascular phenotype improved during the first year after bariatric surgery, with decreased CRVE and increased AVR. Factors associated with retinal microvascular plasticity were male sex, high baseline weight, and absence of diabetes. Longitudinal assessment of retinal vascular calibers may offer new insights into the pathophysiology of subclinical vascular processes.
Graphical abstract



Similar content being viewed by others
References
Calle EE, Thun MJ, Petrelli JM, et al. Body-mass index and mortality in a prospective cohort of U.S. adults. N Engl J Med. 1999;341(15):1097–105.
Must A, Spadano J, Coakley EH, et al. The disease burden associated with overweight and obesity. JAMA. 1999;282(16):1523–9.
Safar ME, Struijker-Boudier HAJ. New goals in hypertension management: target-organ protection beyond blood pressure lowering. Drugs. 2003;63 Spec No 1:45–7.
Adams TD, Gress RE, Smith SC, et al. Long-term mortality after gastric bypass surgery. N Engl J Med. 2007;357(8):753–61.
McGeechan K. Meta-analysis: retinal vessel caliber and risk for coronary heart disease. Ann Intern Med. 2009;151(6):404.
Wang JJ, Liew G, Klein R, et al. Retinal vessel diameter and cardiovascular mortality: pooled data analysis from two older populations. Eur Heart J. 2007;28(16):1984–92.
Boillot A, Zoungas S, Mitchell P, et al. Obesity and the microvasculature: a systematic review and meta-analysis. PLOS ONE 2013 févr;8(2):e52708
Bachmayer C, Lammert A, Hasenberg T, et al. Healthy obese and post bariatric patients - metabolic and vascular patterns. Exp Clin Endocrinol Diabetes. 2013;121(8):483–7.
Lammert A, Hasenberg T, Kräupner C, et al. Improved arteriole-to-venule ratio of retinal vessels resulting from bariatric surgery. Obesity. 2012;20(11):2262–7.
Viljanen A, Soinio M, Cheung CY, et al. Effects of bariatric surgery on retinal microvascular architecture in obese patients. Int J Obes. 2019;43(9):1675–80.
Agarwal A, Saini A, Mahajan S, et al. Effect of weight loss on the retinochoroidal structural alterations among patients with exogenous obesity. PLoS ONE. 2020;15(7):e0235926.
Brynskov T, Laugesen CS, Floyd AK, et al. Thickening of inner retinal layers in the parafovea after bariatric surgery in patients with type 2 diabetes. Acta Ophthalmol. 2016;94(7):668–74.
Streese L, Königstein K, Goricki L, et al. Short- and long-term effects of bariatric surgery on vascular phenotype. Obes Surg. 2019;29(4):1301–8.
Daien V, Carriere I, Kawasaki R, et al. Retinal vascular caliber is associated with cardiovascular biomarkers of oxidative stress and inflammation: the POLA study. PLoS ONE. 2013;8(7):e71089.
Illán-Gómez F, Gonzálvez-Ortega M, Orea-Soler I, et al. Obesity and inflammation: change in adiponectin, C-reactive protein, tumour necrosis factor-alpha and interleukin-6 after bariatric surgery. Obes Surg. 2012;22(6):950–5.
Tapp RJ, Owen CG, Barman SA, et al. Retinal vascular tortuosity and diameter associations with adiposity and components of body composition. Obesity (Silver Spring). 2020;28(9):1750–60.
Nienov OH, Machado FD, Dias LS, et al. Effect of bariatric surgery on high-density lipoprotein (HDL) cholesterol in non-diabetic patients with severe obesity. Obes Surg. 2020;30(1):154–60.
Cunha FM, Oliveira J, Preto J, et al. The effect of bariatric surgery type on lipid profile: an age, sex, body mass index and excess weight loss matched study. Obes Surg. 2016;26(5):1041–7.
Buchwald H, Estok R, Fahrbach K, et al. Weight and type 2 diabetes after bariatric surgery: systematic review and meta-analysis. Am J Med. 2009;122(3):248-256.e5.
Seghieri M, Vitolo E, Giannini L, et al. Determinants of glomerular filtration rate following bariatric surgery in individuals with severe, otherwise uncomplicated, obesity: an observational, prospective study. Acta Diabetol. 2017;54(6):593–8.
Fesler P, Mimran A. Estimation of glomerular filtration rate: what are the pitfalls? Curr Hypertens Rep. 2011;13(2):116–21.
Giudici A, Palombo C, Kozakova M, et al. Weight loss after bariatric surgery significantly improves carotid and cardiac function in apparently healthy people with morbid obesity. Obes Surg. 2020;30(10):3776–83.
Wang FM, Yang C, Tanaka H, et al. Increase in arterial stiffness measures after bariatric surgery. Atherosclerosis. 2021;320:19–23.
Rider OJ, Francis JM, Ali MK, et al. Beneficial cardiovascular effects of bariatric surgical and dietary weight loss in obesity. J Am Coll Cardiol. 2009;54(8):718–26.
Owan T, Avelar E, Morley K, et al. Favorable changes in cardiac geometry and function following gastric bypass surgery: 2-year follow-up in the Utah obesity study. J Am Coll Cardiol. 2011;57(6):732–9.
Funding
The university scholarship “année recherche” from Montpellier University. The sponsors or funding organization had no role in the design or conduct of this research.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed Consent
Informed consent was obtained from all individual participants included in the study.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Key points
• The retinal microvascular phenotype improved during the first year after bariatric surgery, with decreased central retinal vein equivalent (− 5.1 µm, p < 0.0001), and increased arteriole-to-venule ratio (+ 0.02, p < 0.0001).
• Factors associated with retinal microvascular plasticity were male sex, high baseline weight, and absence of diabetes.
• Longitudinal assessment of retinal vascular calibers may offer new insights into the pathophysiology of subclinical vascular processes.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Appendices
Appendix
Table 5
Appendix 2
Figure
Rights and permissions
About this article
Cite this article
Debourdeau, E., Gardes, G., Nocca, D. et al. Longitudinal Effect of Bariatric Surgery on Retinal Microcirculation and Target Organ Damage: the BASTOD Study. OBES SURG 32, 1–10 (2022). https://doi.org/10.1007/s11695-022-06064-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-022-06064-2