Abstract
Introduction
Endoscopic sleeve gastroplasty (ESG) is a novel weight loss procedure that reduces the size of the stomach using an endoscopic suturing device. There are severe adverse events that have been reported following ESG (Brethauer et al. Surg Obes Relat Dis. 6:689–94, 2010; Abu Dayyeh et al. Gastrointest Endosc. 78:530–5, 2013; Nava et al. Endoscopy. 47:449–52, 2015; Nava et al. Endosc Int Open. 4(2):E222–7, 2016). However, complications like gastric perforation following ESG have not been reported. This video presents a case with gastric perforation following ESG and its surgical treatment.
Methods
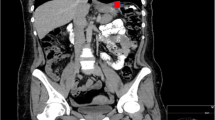
A 44-year-old female patient with an initial body mass index (BMI) of 38 kg/m2 underwent an ESG. Her comorbidities include gastroesophageal reflux disease (GERD) and polycystic ovary syndrome (PCOS). On postoperative day six, the patient presented with lower abdominal pain. The patient refused to get an esophagogastroduodenoscopy (EGD) or laparoscopy done. An upper gastrointestinal series (UGI) was performed, and a large ileus was noted with no evidence of leak or free air. On postoperative day seven, a computed tomography (CAT) scan showed a large amount of free air and fluid throughout the abdomen and pelvis. The patient was taken to the operating room (OR) for an exploratory laparoscopy.
Results
Upon entering the abdomen, a large amount of pus and free fluid was noted. This was irrigated free from the abdominal cavity until it came back clear. We noted six sutures that went intraluminally to extraluminally and entered the anterior abdominal wall. These sutures were taken down until we found the perforation. A GIA stapler was placed over the perforation, and the defect was closed. The staple line was then imbricated. Once done with the imbrication, we spent a significant amount of time laparoscopically irrigating the abdomen with 12 L of fluid. In total, three drains were placed to assist with draining the abdomen.
Conclusion
ESG is a feasible endobariatric option, but complications like gastric perforation can occur. For such complication, immediate surgical treatment is indicated.
Similar content being viewed by others
References
Brethauer SA, Chand B, Schauer PR, et al. Transoral gastric volume reduction for weight management: technique and feasibility in 18 patients. Surg Obes Relat Dis. 2010;6:689–94.
Abu Dayyeh BK, Rajan E, Gostout CJ. Endoscopic sleeve gastroplasty: a potential endoscopic alternative to surgical sleeve gastrectomy for treatment of obesity. Gastrointest Endosc. 2013;78:530–5.
Nava G, Galvão M, Castaño B, et al. Endoscopic sleeve gastroplasty for the treatment of obesity. Endoscopy. 2015;47:449–52.
Nava L, Galvao M, Castaño B, et al. Endoscopic sleeve gastroplasty with 1-year follow-up: factors predictive of success. Endosc Int Open. 2016;4(2):E222–7.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Author 2, the corresponding author of this report is part of the speaker bureau for Medtronic and has been awarded a research grant by Medtronic for the study of Duodenal Switch.
All other authors have no conflicts of interests to declare.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic Supplementary Material
(MP4 336,519 kb)
Rights and permissions
About this article
Cite this article
Surve, A., Cottam, D., Medlin, W. et al. A Video Case Report of Gastric Perforation Following Endoscopic Sleeve Gastroplasty and its Surgical Treatment. OBES SURG 29, 3410–3411 (2019). https://doi.org/10.1007/s11695-019-03992-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-019-03992-4