Abstract
Objective
Bariatric surgery leads to more rapid and greater weight loss (WL) compared to medical weight loss (MWL), but the differences in body composition (BC) changes for these modalities remain unclear. Due to the known health risks associated with central adiposity, we compared the changes in regional distribution of fat mass (FM) and lean mass (LM) after surgical versus MWL.
Methods
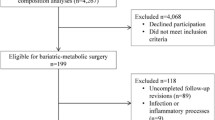
In this 1:1:1 randomized trial among 15 persons with type 2 diabetes and body mass index (BMI) 30–39.9 kg/m2, we compared changes in BC, by dual-energy X-ray absorptiometry and abdominal computerized tomography, at time of 10%WL or 9 months after intervention (whichever came first). Participants underwent MWL, adjustable gastric banding (AGB), or Roux-en-Y gastric bypass (RYGB). Non-parametric tests evaluated BC differences (FM, LM, and visceral adipose tissue [VAT]) within and across all three arms and between pair-wise comparisons.
Results
Twelve female participants (75% African American) completed the study. Patient age, BMI, and baseline anthropometric characteristics were similar across study arms. AGB lost more LM (MWL − 5.2%, AGB − 10.3%, p = 0.021) and VAT (MWL + 10.9%, AGB − 28.0%, p = 0.049) than MWL. RYGB tended to lose more VAT (MWL +10.9%, RYGB − 20.2%, p = 0.077) than MWL. AGB tended to lose more LM than RYGB (AGB − 12.38%, RYGB − 7.29%, p = 0.15).
Conclusions
At similar WL, AGB lost more LM and VAT than MWL; RYGB similarly lost more VAT. Given the metabolic benefits of reducing VAT and retaining LM, larger studies should confirm the changes in BC after surgical versus medical WL.
Clinical Trial Registration
NCTDK089557 – ClinicalTrials.gov
Similar content being viewed by others
References
Jensen MD. Role of body fat distribution and the metabolic complications of obesity. J Clin Endocrinol Metab. 2008;93(11 Suppl 1):S57–63.
Webster JD, Hesp R, Garrow JS. The composition of excess weight in obese women estimated by body density, total body water and total body potassium. Hum Nutr Clin Nutr. 1984;38(4):299–306.
Marks BL, Rippe JM. The importance of fat free mass maintenance in weight loss programmes. Sports Med. 1996;22(5):273–81.
Knowler WC, Barrett-Connor E, Fowler SE, et al. Reduction in the incidence of type 2 diabetes with lifestyle intervention or metformin. N Engl J Med. 2002;346(6):393–403.
Unick JL, Beavers D, Jakicic JM, et al. Effectiveness of lifestyle interventions for individuals with severe obesity and type 2 diabetes: results from the look AHEAD trial. Diabetes Care. 2011;34(10):2152–7.
Yeh HC, Clark JM, Emmons KE, et al. Independent but coordinated trials: insights from the practice-based opportunities for weight reduction trials collaborative research group. Clin Trials. 2010;7(4):322–32.
Mechanick JI, Youdim A, Jones DB, et al. Clinical practice guidelines for the perioperative nutritional, metabolic, and nonsurgical support of the bariatric surgery patient—2013 update: cosponsored by American Association of Clinical Endocrinologists, the Obesity Society, and American Society for Metabolic & bariatric surgery. Obesity (Silver Spring). 2013;21(Suppl 1):S1–27.
Dixon JB, Strauss BJ, Laurie C, et al. Changes in body composition with weight loss: obese subjects randomized to surgical and medical programs. Obesity (Silver Spring). 2007;15(5):1187–98.
Schneider J, Peterli R, Gass M, et al. Laparoscopic sleeve gastrectomy and roux-en-Y gastric bypass lead to equal changes in body composition and energy metabolism 17 months postoperatively: a prospective randomized trial. Surg Obes Relat Dis. 2016;12(3):563–70.
Pownall HJ, Bray GA, Wagenknecht LE, et al. Changes in body composition over 8 years in a randomized trial of a lifestyle intervention: the look AHEAD study. Obesity (Silver Spring). 2015;23(3):565–72.
Haywood CJ, Prendergast LA, Purcell K, et al. Very low calorie diets for weight loss in obese older adults—a randomized trial. J Gerontol A Biol Sci Med Sci. 2017;73(1):59–65.
Moize V, Andreu A, Rodriguez L, et al. Protein intake and lean tissue mass retention following bariatric surgery. Clin Nutr. 2013;32(4):550–5.
Coupaye M, Bouillot JL, Coussieu C, et al. One-year changes in energy expenditure and serum leptin following adjustable gastric banding in obese women. Obes Surg. 2005;15(6):827–33.
Carey DGPG, Raymond RL, Skau KB. Body composition and metabolic changes following bariatric surgery: effects on fat mass, lean mass, and basal metabolic rate. Obes Surg. 2006;16:469–77.
Sergi G, Lupoli L, Busetto L, et al. Changes in fluid compartments and body composition in obese women after weight loss induced by gastric banding. Ann Nutr Metab. 2003;47(3–4):152–7.
Kiyama T, Mizutani T, Okuda T, et al. Postoperative changes in body composition after gastrectomy. J Gastrointest Surg. 2005;9(3):313–9.
Ramalho R, Guimaraes C, Gil C, et al. Morbid obesity and inflammation: a prospective study after adjustable gastric banding surgery. Obes Surg. 2009;19(7):915–20.
Ito MK, Goncalves VSS, Faria S, et al. Effect of protein intake on the protein status and lean mass of post-bariatric surgery patients: a systematic review. Obes Surg. 2017;27(2):502–12.
Aron-Wisnewsky J, Verger EO, Bounaix C, et al. Nutritional and protein deficiencies in the short term following both gastric bypass and gastric banding. PLoS One. 2016;11(2):e0149588.
Schollenberger AE, Karschin J, Meile T, et al. Impact of protein supplementation after bariatric surgery: a randomized controlled double-blind pilot study. Nutrition. 2016;32(2):186–92.
Olbers T, Bjorkman S, Lindroos A, et al. Body composition, dietary intake, and energy expenditure after laparoscopic roux-en-Y gastric bypass and laparoscopic vertical banded gastroplasty: a randomized clinical trial. Ann Surg. 2006;244(5):715–22.
Davidson LE, Yu W, Goodpaster BH, et al. Fat-free mass and skeletal muscle mass five years after bariatric surgery. Obesity (Silver Spring). 2018;26(7):1130–6.
Isom KA. Standardizing the evolution of the postoperative bariatric diet. Diabetes Spectrum. 2012;25(4):222–8.
Kim B, Tsujimoto T, So R, et al. Changes in lower extremity muscle mass and muscle strength after weight loss in obese men: a prospective study. Obes Res Clin Pract. 2015;9(4):365–73.
Siervo M, Faber P, Lara J, et al. Imposed rate and extent of weight loss in obese men and adaptive changes in resting and total energy expenditure. Metabolism. 2015;64(8):896–904.
Weiss R, Appelbaum L, Schweiger C, et al. Short-term dynamics and metabolic impact of abdominal fat depots after bariatric surgery. Diabetes Care. 2009;32(10):1910–5.
Carroll JF, Franks SF, Smith AB, et al. Visceral adipose tissue loss and insulin resistance 6 months after laparoscopic gastric banding surgery: a preliminary study. Obes Surg. 2009;19(1):47–55.
Heath ML, Kow L, Slavotinek JP, et al. Abdominal adiposity and liver fat content 3 and 12 months after gastric banding surgery. Metabolism. 2009;58(6):753–8.
Phillips ML, Lewis MC, Chew V, et al. The early effects of weight loss surgery on regional adiposity. Obes Surg. 2005;15(10):1449–55.
Bluher S, Raschpichler M, Hirsch W, et al. A case report and review of the literature of laparoscopic sleeve gastrectomy in morbidly obese adolescents: beyond metabolic surgery and visceral fat reduction. Metabolism. 2013;62(6):761–7.
Courcoulas AP, Christian NJ, Belle SH, et al. Weight change and health outcomes at 3 years after bariatric surgery among individuals with severe obesity. JAMA. 2013;310(22):2416–25.
Sanguankeo A, Lazo M, Upala S, et al. Effects of visceral adipose tissue reduction on CVD risk factors independent of weight loss: the look AHEAD study. Endocr Res. 2017;42(2):86–95.
Kissler HJ, Settmacher U. Bariatric surgery to treat obesity. Semin Nephrol. 2013;33(1):75–89.
Koo BKMK, Kim HJ, et al. Changes of abdominal thigh adipose tissue and skeletal muscle attenuation in response to energy restriction or exercise in overweight type 2 diabetes. Obesity. 2008;16:S228–S28.
Dagan SS, Goldenshluger A, Globus I, et al. Nutritional recommendations for adult bariatric surgery patients: clinical practice. Adv Nutr. 2017;8(2):382–294.
Acknowledgements
The authors would like to thank the patients and staff at the Johns Hopkins Center for Bariatric Surgery and the Institute for Clinical and Translational Research staff, without whom this research would not be possible. The study protocol is available upon request (submit request to jclark1@jhmi.edu) beginning at the time of publication and ending 36 months after publication. We are unable to share the individual participant data from this study.
Funding Sources
JMC and NMM were supported by Grant Number 1R01DK089557 (PI: J Clark, NIH, NIDDK). CJL was supported by Grant Number 5KL2TR001077-02 as part of the Institute for Clinical and Translational Research Grant from the NIH/NCAT and career development award from the NIH/NIDDK (K23DK107921). This study was also supported by the Translational Research Enhancement Core of the Hopkins Digestive Diseases Basic Research Development Center (P30, DK089502-01 NIDDK/NIH) and by the Johns Hopkins Institute for Clinical and Translational Research (ICTR) which is funded in part by Grant Number UL1 TR001079 from the National Center for Advancing Translational Sciences (NCATS) a component of the National Institutes of Health (NIH), and NIH Roadmap for Medical Research.
Author information
Authors and Affiliations
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed Consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Varma, S., Lee, C.J., Brown, T.T. et al. Comparative Effects of Medical Versus Surgical Weight Loss on Body Composition: a Pilot Randomized Trial. OBES SURG 29, 2503–2510 (2019). https://doi.org/10.1007/s11695-019-03879-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-019-03879-4