Abstract
Background
Many factors, including preoperative weight, may determine final weight loss after bariatric surgery; however, their proportional contribution is unclear. To such end, we evaluated weight loss patterns among obese adolescents.
Methods
We evaluated 57 adolescents who underwent laparoscopic sleeve gastrectomy from 2011 to 2017. Data collection included demographics, anthropometrics, and comorbidities and was done over a 3-year follow-up period. Statistical analysis was performed using Student’s t test and repeated measures ANOVA.
Results
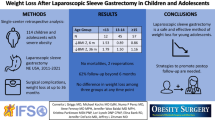
In the morbidly obese (MO) group, 82% were female, while 52% were male in the super obese (SMO) group (P < 0.0059). While 13/34 patients in the obese group achieved > 60% percent excess body weight loss (%EBWL), only 3/23 super obese patients achieved > 60% EBWL (P = 0.0695). %EBWL at 1-year follow-up significantly differed between the obese and super obese groups, 61.7 ± 14.6% and 47.7 ± 14.9% respectively (P = 0.035). The average BMI in the obese group was 29.8 at 1 year and 41.3 in the super obese group. There was a significant difference in the rate of excess weight loss (%EBWL/month) between the two groups (P < 0.01). There was good comorbidity resolution (about 70%) in both groups after surgery.
Conclusion
Comorbidity resolution after sleeve gastrectomy is excellent in the adolescent population irrespective of initial BMI. Consideration should be given to earlier bariatric intervention in SMO adolescents to facilitate return to near normal BMI. Focus on education of referral sources, such as community pediatricians and family practitioners to facilitate early bariatric evaluation should be considered. Weight loss in postsurgical SMO patients should be carefully monitored and adjunctive interventions should be considered.


Similar content being viewed by others
References
Hales CM, Carroll MD, Fryar CD, et al. Prevalence of obesity among adults and youth: United States, 2015–2016. US Department of Health and Human Services, Centers for Disease Control and Prevention, National Center for Health Statistics; 2017.
Hsia DS, Fallon SC, Brandt ML. Adolescent bariatric surgery. Arch Pediatr Adolesc Med. 2012;166(8):757–66.
Treadwell JR, Sun F, Schoelles K. Systematic review and meta-analysis of bariatric surgery for pediatric obesity. Ann Surg. 2008;248(5):763–76.
Black JA, White B, Viner RM, et al. Bariatric surgery for obese children and adolescents: a systematic review and meta-analysis. Obes Rev. 2013;14(8):634–44.
Arafat M, Norain A, Burjonrappa SC. Characterizing bariatric surgery utilization and complication rates in the adolescent population. J Pediatr Surg. 2019;54(2):288–92.
Inge TH, Jenkins TM, Zeller M, et al. Baseline BMI is a strong predictor of nadir BMI after adolescent gastric bypass. J Pediatr. 2010;156(1):103–8.
Jaworska N, MacQueen G. Adolescence as a unique developmental period. J Psychiatry Neurosci. 2015 Sep;40(5):291–3.
Sawyer S, Azzopardi PS, Wickremarathne D, et al. (2018). The age of adolescence. Lancet Child Adolesc Health. 2018;2(3):157–228.
Serrano OK, Zhang Y, Kintzer E, et al. Outcomes of bariatric surgery in the young: a single-institution experience caring for patients under 21 years old. Surg Endosc. 2016;30(11):5015–22.
Freedman DS, Butte NF, Taveras EM, et al. BMI z-scores are a poor indicator of adiposity among 2- to 19-year-olds with very high BMIs, NHANES 1999-2000 to 2013-2014. Obesity (Silver Spring). 2017;25(4):739–46.
Poirier P, Cornier MA, Mazzone T, et al. Bariatric surgery and cardiovascular risk factors: a scientific statement from the American Heart Association. Circulation. 2011;123(15):1683–701.
Lee JM, Villamor E. Tackling childhood overweight and obesity: thresholds and beyond. JAMA Pediatr. 2013;167(1):87–8.
Holterman AX, Holterman M, Browne A, et al. Patterns of surgical weight loss and resolution of metabolic abnormalities in superobese bariatric adolescents. J Pediatr Surg. 2012;47(9):1633–9.
Nguyen NT, Goldman C, Rosenquist CJ, et al. Laparoscopic versus open gastric bypass: a randomized study of outcomes, quality of life, and costs. Ann Surg. 2001;234(3):279–91.
McBride CL, Petersen A, Sudan D, et al. Short bowel syndrome following bariatric surgical procedures. Am J Surg. 2006;192(6):828–32.
Ukleja A. Dumping syndrome: pathophysiology and treatment. Nutr Clin Pract. 2005;20(5):517–25.
Upala S, Jaruvongvanich V, Sanguankeo A. Risk of nephrolithiasis, hyperoxaluria, and calcium oxalate supersaturation increased after Roux-en-Y gastric bypass surgery: a systematic review and meta-analysis. Surg Obes Relat Dis. 2016;12(8):1513–21.
Stenard F, Iannelli A. Laparoscopic sleeve gastrectomy and gastroesophageal reflux. World J Gastroenterol. 2015;21(36):10348–57.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Disclosures
None.
Statement of Informed Consent
This was a retrospective study and IRB approval with HIPPA compliance was obtained from the institution for the study.
Statement of Human and Animal Rights/Ethical Approval
This was a retrospective study and no human or animal was harmed in the study.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Level of Evidence: Level III
Rights and permissions
About this article
Cite this article
Norain, A., Arafat, M. & Burjonrappa, S. Trending Weight Loss Patterns in Obese and Super Obese Adolescents: Does Laparoscopic Sleeve Gastrectomy Provide Equivalent Outcomes in both Groups?. OBES SURG 29, 2511–2516 (2019). https://doi.org/10.1007/s11695-019-03867-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-019-03867-8