Abstract
Introduction
The effect of local anesthetic applications to trocar sites on postoperative pain control has been studied many times, and different results have been obtained. We planned a controlled study evaluating the effect of bupivacaine administration and other contributing factors on postoperative pain following sleeve gastrectomy.
Material and Methods
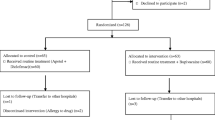
Patients who underwent laparoscopic sleeve gastrectomy were included in the study. Patients were randomized into two groups according to local application as either a local or non-local group. Also, the patients were grouped separately from local group allocation according to time to first passage of flatus (< 12 h, ≥ 12 h) and duration of surgery (> 50 min, ≤ 50 min). A visual analogue scale (VAS) was performed at 4, 8, 12, 24, and 48 h postoperatively. Opioid analgesics (pethidine HCl) were administered if the patient’s VAS score was greater than 5. Demographic characteristics, such as age, gender, height, weight, body mass index (BMI), and operative time, were recorded. Demographic characteristics and VAS scores were compared between groups.
Results
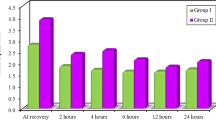
A total of 168 patients were included in the study. Of these, 84 patients were included in both of the local and non-local groups. The demographic characteristics between groups were similar. There was no significant difference between groups in terms of VAS scores (p > 0.05). In the analysis according to the time to first passage of flatus, the 48th-hour VAS scores were lower in the early flatus group (p = 0.036). According to the duration of surgery, first flatus was detected earlier, and VAS scores at the 8th and 12th hours were less in the short operation group (p < 0.001, p = 0.005, p = 0.031, respectively).
Discussion
Although we did not show any effect of local administration of bupivacaine in LSG on pain, we concluded that other factors like duration of surgery and first flatus time have an impact on this issue.

Similar content being viewed by others
References
Torres-Landa S, Kannan U, Guajardo I, Pickett-Blakely OE, Dempsey DT, Williams NN, Dumon KR. The surgical management of obesity. Minerva Chir. 2017 Dec 14. doi: https://doi.org/10.23736/S0026-4733.17.07588-5. [Epub ahead of print]
Badaoui R, Chentoufi YA, Hchikat A, et al. Outpatient laparoscopic sleeve gastrectomy: first 100 cases. Journal of Clinical Anesthesia. 2016;34:85–90.
El Sherif FA, Othman AH, Abd El-Rahman AM, et al. Effect of adding intrathecal morphine to a multimodal analgesic regimen for postoperative pain management after laparoscopic bariatric surgery: a prospective, double-blind, randomized controlled trial. Br J Pain. 2016;10(4):209–16. https://doi.org/10.1177/2049463716668904.
Sherwinter DA, Ghaznavi AM, Spinner D, et al. Continuous infusion of intraperitoneal bupivacaine after laparoscopic surgery: a randomized controlled trial. Obes Surg. 2008;18:1581–6. https://doi.org/10.1007/s11695-008-9628-2.
Tam T, Harkins G, Wegrzyniak L, et al. Infiltration of bupivacaine local anesthetic to trocar insertion sites after laparoscopy: a randomized, double-blind, stratified, and controlled trial. J Minim Invasive Gynecol. 2014;21(6):1015–21. https://doi.org/10.1016/j.jmig.2014.04.013. Epub 2014 May 2
Einarsson JI, Sun J, Orav J, et al. Local analgesia in laparoscopy: a randomized trial. Obstet Gynecol. 2004;104(6):1335–9.
Kim JE, Shim SH, Dong M, et al. Port site infiltration of local anesthetic after laparoendoscopic single site surgery for benign adnexal disease. Obstet Gynecol Sci. 2017;60(5):455–61. https://doi.org/10.5468/ogs.2017.60.5.455. Epub 2017 Sep 18
El Hachem L, Small E, Chung P, Moshier EL, Friedman K, Fenske SS, Gretz HF 3rd. Randomized controlled double-blind trial of transversus abdominis plane block versus trocar site infiltration in gynecologic laparoscopy. Am J Obstet Gynecol. 2015 212(2):182.e1–9. doi: https://doi.org/10.1016/j.ajog.2014.07.049.
Alper I, Ulukaya S, Yüksel G, et al. Laparoscopic cholecystectomy pain: effects of the combination of incisional and intraperitoneal levobupivacaine before or after surgery. Agri. 2014;26(3):107–12. https://doi.org/10.5505/agri.2014.42650.
Cantore F, Boni L, Di Giuseppe M, et al. Pre-incision local infiltration with levobupivacaine reduces pain and analgesic consumption after laparoscopic cholecystectomy: a new device for day-case procedure. Int J Surg. 2008;6(Suppl 1):S89–92. https://doi.org/10.1016/j.ijsu.2008.12.033. Epub 2008 Dec 24
Hartwig M, Allvin R, Bäckström R, et al. Factors associated with increased experience of postoperative pain after laparoscopic gastric bypass surgery. Obes Surg. 2017 Jul;27(7):1854–8. https://doi.org/10.1007/s11695-017-2570-4.
Xu SQ, Li YH, Wang SB, et al. Effects of intravenous lidocaine, dexmedetomidine and their combination on postoperative pain and bowel function recovery after abdominal hysterectomy. Minerva Anestesiol. 2017;83(7):685–94. https://doi.org/10.23736/S0375-9393.16.11472-5.
Basak F, Hasbahceci M, Sisik A, et al. Glisson’s capsule cauterisation is associated with increased postoperative pain after laparoscopic cholecystectomy: a prospective case-control study. Ann R Coll Surg Engl. 2017;99(6):485–9. https://doi.org/10.1308/rcsann.2017.0068.
Cohen AR, Smith AN, Henriksen BS. Postoperative opioid requirements following Roux-en-Y gastric bypass in patients receiving continuous bupivacaine through a pump system: a retrospective review. Hosp Pharm. 2013;48(6):479–83. https://doi.org/10.1310/hpj4806-47.
Ruiz-Tovar J, Gonzalez J, Garcia A, et al. Intraperitoneal ropivacaine irrigation in patients undergoing bariatric surgery: a prospective randomized clinical trial. Obes Surg. 2016;26(11):2616–21. https://doi.org/10.1007/s11695-016-2142-z.
Ruiz-Tovar J, Muñoz JL, Gonzalez J, et al. Postoperative pain after laparoscopic sleeve gastrectomy: comparison of three analgesic schemes (isolated intravenous analgesia, epidural analgesia associated with intravenous analgesia and port-sites infiltration with bupivacaine associated with intravenous analgesia). Surg Endosc. 2017;31(1):231–6. https://doi.org/10.1007/s00464-016-4961-3.
Bamgbade OA, Oluwole O, Khaw RR. Perioperative analgesia for fast-track laparoscopic bariatric surgery. Obes Surg. 2017;27(7):1828–34. https://doi.org/10.1007/s11695-017-2562-4.
Moncada R, Martinaitis L, Landecho M, et al. Does pre-incisional infiltration with bupivacaine reduce postoperative pain in laparoscopic bariatric surgery? Obes Surg. 2016;26(2):282–8. https://doi.org/10.1007/s11695-015-1761-0.
Torensma B, Oudejans L, van Velzen M, et al. Pain sensitivity and pain scoring in patients with morbid obesity. Surg Obes Relat Dis. 2017;13(5):788–95. https://doi.org/10.1016/j.soard.2017.01.015.
Cho JS, Kim HI, Lee KY, et al. Comparison of the effects of patient-controlled epidural and intravenous analgesia on postoperative bowel function after laparoscopic gastrectomy: a prospective randomized study. Surg Endosc. 2017;31(11):4688–96. https://doi.org/10.1007/s00464-017-5537-6.
Conde SM, del Agua IA, Moreno AB, et al. Postoperative pain after conventional laparoscopic versus single port sleeve gastrectomy: a prospective, randomised, controlled clinical trial. Surg Obes Relat Dis. 2017;13(4):608–13. https://doi.org/10.1016/j.soard.2016.11.012.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Ethical Approval
Ethics committee approval was obtained for this study.
Informed Consent
Informed consent was obtained from the patients.
Rights and permissions
About this article
Cite this article
Sisik, A., Erdem, H. Effect of Trocar Site Bupivacaine Administration, Time of First Passage of Flatus, and Duration of the Surgery on Postoperative Pain After Sleeve Gastrectomy: a Case Control Study. OBES SURG 29, 444–450 (2019). https://doi.org/10.1007/s11695-018-3529-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-018-3529-9