Abstract
Background
The prevalence of chronic kidney disease (CKD) among Japanese morbidly obese patients undergoing bariatric surgery and the impact of bariatric surgery on their renal function has not previously been investigated.
Objectives
The aims were to assess the prevalence of CKD patients who underwent bariatric surgery in our institution and to elucidate the impact of bariatric surgery on their kidney function as measured by the estimated glomerular filtration rate by Cystatin-C (eGFRcys).
Setting
The setting of the study was in a single private hospital.
Methods
Two hundred fifty-four consecutive Japanese patients who underwent bariatric surgery were retrospectively analyzed to elucidate the prevalence of CKD. The eGFRcys was calculated to assess the change in the kidney function for 1 year after surgery.
Results
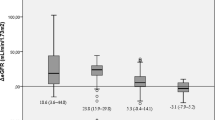
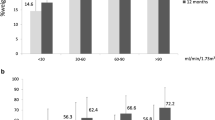
The preoperative prevalence of CKD was as follows: G1, 45.3%; G2, 47.2%; G3, 6.5%; and G4, 0.9%. The eGFRcys values before and after surgery were compared; the G1 and G2 patients showed significantly improved eGFRcys values after surgery (G1 101 [94–108] vs 114 [103–127]; G2 79 [74–84] vs 97 [87–104] ml/min/1.73 m2; p < 0.01) with significant weight loss (G1 38.1 ± 6.2 vs 26.5 ± 3.4; G2 38.5 ± 6.9 vs 26.7 ± 3.6 kg/m2; p < 0.01). Although the renal function of G3 patients was not improved after surgery (44 [42–47] vs 45 [43–63] ml/min/1.73 m2; p = 0.08), successful weight loss was achieved (36.1 ± 6.3 vs 26.6 ± 3.6 kg/m2; p < 0.01). In multivariate analysis, postoperative eGFRcys correlated negatively with proteinuria (p < 0.01), age (p < 0.01), and body mass index (p < 0.01) and positively with persistence of antihypertensive drugs.
Conclusion
Bariatric surgery resulted in the significant improvement in the eGFRcys values of Japanese patients with morbid obesity, particularly those with pre-CKD (eGFRcys ≥ 60 ml/min/1.73 m2), while the eGFRcys values of CKD patients (< 60 ml/min/1.73 m2) were not ameliorated by surgery.
Similar content being viewed by others
References
Imai E, Horio M, Watanabe T, et al. Prevalence of chronic kidney disease in the Japanese general population. Clin Exp Nephrol. 2009;13(6):621–30. doi:10.1007/s10157-009-0199-x.
Ogden CL, Carroll MD, Kit BK, et al. Prevalence of obesity in the United States, 2009-2010. NCHS Data Brief. 2012;82:1–8. http://www.ncbi.nlm.nih.gov/pubmed/22617494. Accessed May 25, 2016
Yoshiike N, Matsumura Y, Zaman MM, et al. Descriptive epidemiology of body mass index in Japanese adults in a representative sample from the National Nutrition Survey 1990-1994. Int J Obes Relat Metab Disord. 1998;22(7):684–7. http://www.ncbi.nlm.nih.gov/pubmed/9705030. Accessed May 25, 2016
Hsu C, McCulloch CE, Iribarren C, et al. Body mass index and risk for end-stage renal disease. Ann Intern Med. 2006;144(1):21–8. http://www.ncbi.nlm.nih.gov/pubmed/16389251. Accessed November 15, 2016
Ix JH, Sharma K. Mechanisms linking obesity, chronic kidney disease, and fatty liver disease: the roles of fetuin-A, adiponectin, and AMPK. J Am Soc Nephrol. 2010;21(3):406–12. doi:10.1681/ASN.2009080820.
Navaneethan SD, Yehnert H. Bariatric surgery and progression of chronic kidney disease. Surg Obes Relat Dis. 2009;5(6):662–5. doi:10.1016/j.soard.2009.01.006.
Mirajkar N, Bellary S, Ahmed M, et al. The impact of bariatric surgery on estimated glomerular filtration rate in patients with type 2 diabetes: a retrospective cohort study. Surg Obes Relat Dis. 2016; doi:10.1016/j.soard.2016.02.024.
Coupaye M, Flamant M, Sami O, et al. Determinants of evolution of glomerular filtration rate after bariatric surgery: a 1-year observational study. Obes Surg. 2017;27(1):126–33. doi:10.1007/s11695-016-2260-7.
Levey AS, Stevens LA, Schmid CH, et al. A new equation to estimate glomerular filtration rate. Ann Intern Med. 2009;150(9):604–12. http://www.ncbi.nlm.nih.gov/pubmed/19414839. Accessed May 26, 2016
Friedman AN, Moe S, Fadel WF, et al. Predicting the glomerular filtration rate in bariatric surgery patients. Am J Nephrol. 2014;39(1):8–15. doi:10.1159/000357231.
Fenske WK, Dubb S, Bueter M, et al. Effect of bariatric surgery-induced weight loss on renal and systemic inflammation and blood pressure: a 12-month prospective study. Surg Obes Relat Dis. 2013;9(4):559–68. doi:10.1016/j.soard.2012.03.009.
Nehus EJ, Khoury JC, Inge TH, et al. Kidney outcomes three years after bariatric surgery in severely obese adolescents. Kidney Int. 2016; doi:10.1016/j.kint.2016.09.031.
Lee W-J, Wang W. Bariatric surgery: Asia-Pacific perspective. Obes Surg. 2005;15(6):751–7. doi:10.1381/0960892054222614.
Horio M, Imai E, Yasuda Y, et al. Collaborators developing the Japanese equation for estimated GFR. GFR estimation using standardized serum cystatin C in Japan. Am J Kidney Dis. 2013;61(2):197–203. doi:10.1053/j.ajkd.2012.07.007.
Matsuo S, Imai E, Horio M, et al. Revised equations for estimated GFR from serum creatinine in Japan. Am J Kidney Dis. 2009;53(6):982–92. doi:10.1053/j.ajkd.2008.12.034.
Levey AS, Becker C, Inker LA. Glomerular filtration rate and albuminuria for detection and staging of acute and chronic kidney disease in adults: a systematic review. JAMA. 2015;313(8):837–46. doi:10.1001/jama.2015.0602.
Seki Y, Kasama K, Hashimoto K. Long-term outcome of laparoscopic sleeve gastrectomy in morbidly obese Japanese patients. Obes Surg. 2016;26(1):138–45. doi:10.1007/s11695-015-1728-1.
Seki Y, Kasama K, Umezawa A, et al. Laparoscopic sleeve gastrectomy with duodenojejunal bypass for type 2 diabetes mellitus. Obes Surg. 2016; doi:10.1007/s11695-016-2057-8.
Hashimoto K, Seki Y, Kasama K. Laparoscopic intragastric surgery and laparoscopic roux-y gastric bypass were performed simultaneously on a morbidly obese patient with a gastric submucosal tumor: a report of a case and review. Obes Surg. 2015;25(3):564–7. doi:10.1007/s11695-014-1550-1.
Akbari A, Clase CM, Acott P, et al. Canadian Society of Nephrology commentary on the KDIGO clinical practice guideline for CKD evaluation and management. Am J Kidney Dis. 2015;65(2):177–205. doi:10.1053/j.ajkd.2014.10.013.
Matsuzawa Y, Funahashi T, Nakamura T. The concept of metabolic syndrome: contribution of visceral fat accumulation and its molecular mechanism. J Atheroscler Thromb. 2011;18(8):629–39. http://www.ncbi.nlm.nih.gov/pubmed/21737960. Accessed May 25, 2016
Abou-Mrad RM, Abu-Alfa AK, Ziyadeh FN. Effects of weight reduction regimens and bariatric surgery on chronic kidney disease in obese patients. AJP Ren Physiol. 2013;305(5):F613–7. doi:10.1152/ajprenal.00173.2013.
Friedman AN, Ogden LG, Foster GD, et al. Comparative effects of low-carbohydrate high-protein versus low-fat diets on the kidney. Clin J Am Soc Nephrol. 2012;7(7):1103–11. doi:10.2215/CJN.11741111.
Chang AR, Chen Y, Still C, et al. Bariatric surgery is associated with improvement in kidney outcomes. Kidney Int. 2016;90(1):164–71. doi:10.1016/j.kint.2016.02.039.
Li K, Zou J, Ye Z, et al. Effects of bariatric surgery on renal function in obese patients: a systematic review and meta analysis. Joles JA, ed. PLoS One. 2016;11(10):e0163907. doi:10.1371/journal.pone.0163907.
Ito R, Yamakage H, Kotani K, et al. Comparison of cystatin C- and creatinine-based estimated glomerular filtration rate to predict coronary heart disease risk in Japanese patients with obesity and diabetes. Endocr J. 2015;62(2):201–7. doi:10.1507/endocrj.EJ14-0352.
Rubino F, Nathan DM, Eckel RH, et al. Metabolic surgery in the treatment algorithm for type 2 diabetes: a joint statement by international diabetes organizations. Diabetes Care. 2016;39(6):861–77. doi:10.2337/dc16-0236.
Acknowledgements
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interests.
Informed Consent
Informed consent was obtained from all individual participants included in the study.
Human and Animal Rights
Our present study has been approved by the appropriate Institutional review board, which is set up in our hospital.
Rights and permissions
About this article
Cite this article
Wakamatsu, K., Seki, Y., Kasama, K. et al. Prevalence of Chronic Kidney Disease in Morbidly Obese Japanese and the Impact of Bariatric Surgery on Disease Progression. OBES SURG 28, 489–496 (2018). https://doi.org/10.1007/s11695-017-2863-7
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-017-2863-7