Abstract
Background
Prior studies have suggested less weight loss among African American compared to Caucasian patients; however, few studies have been able to simultaneously account for baseline differences in other demographic, clinical, or behavioral factors.
Methods
We interviewed patients at two weight loss surgery (WLS) centers and conducted chart reviews before and after WLS. We compared weight loss post-WLS by race/ethnicity and examined baseline demographic, clinical (BMI, comorbidities, quality of life), and behavioral (eating behavior, physical activity level, alcohol intake) factors that might explain observed racial differences in weight loss at 1 and 2 years after WLS.
Results
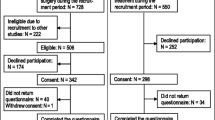
Of 537 participants who underwent either Roux-en-Y Gastric Bypass (54%) or gastric banding (46%), 85% completed 1-year follow-up and 73% completed 2-year follow-up. Patients lost a mean of 33.00% of initial weight at year 1 and 32.43% at year 2 after bypass and 16.07% and 17.56 % respectively after banding. After adjustment for other demographic characteristics and type of surgery, African Americans lost an absolute 5.93 ± 1.49% less weight than Caucasian patients after bypass (p < 0.001) and 4.72 ± 1.96% less weight after banding. Of the other demographic, clinical, behavioral factors considered, having diabetes and perceived difficulty making dietary changes at baseline were associated with less weight loss among gastric bypass patients whereas having a diagnosis of anxiety disorder was associated with less weight loss among gastric banding patients. The association between race and weight loss did not substantially attenuate with additional adjustment for these clinical and behavioral factors, however.
Conclusion
African American patients lost significantly less weight than Caucasian patients. Racial differences could not be explained by baseline demographic, clinical, or behavioral characteristics we examined.
Similar content being viewed by others

References
Sjostrom L, Lindroos AK, Peltonen M, et al. Lifestyle, diabetes, and cardiovascular risk factors 10 years after bariatric surgery. N Engl J Med. 2004;351(26):2683–93.
O'Brien PE, McPhail T, Chaston TB, et al. Systematic review of medium-term weight loss after bariatric operations. Obes Surg. 2006;16(8):1032–40.
Christou NV, Look D, Maclean LD. Weight gain after short- and long-limb gastric bypass in patients followed for longer than 10 years. Ann Surg. 2006;244(5):734–40.
Coleman KJ, Brookey J. Gender and racial/ethnic background predict weight loss after Roux-en-Y gastric bypass independent of health and lifestyle behaviors. Obes Surg. 2014;24(10):1729–36.
Admiraal WM, Celik F, Gerdes VE, et al. Ethnic differences in weight loss and diabetes remission after bariatric surgery: a meta-analysis. Diabetes Care. 2012;35(9):1951–8.
Courcoulas AP, O'Rourke RW, Dakin G, et al. Preoperative factors and 3-year weight gain change in the longitudinal assessment of bariatric surgery (LABS) consortium. Surg Obes Relat Dis. 2015;11(5):1109–18.
Ng JSR, Stone A, Ruano G, et al. Ethnic variation in weight loss, but not co-morbidity remission, after laparoscopic gastric banding and Roux-en-Y gastric bypass. Surg Obes Relat Dis. 2015;11(1):94–100.
Elli EF, Gonzalez-Heredia R, Patel N, et al. Bariatric surgery outcomes in ethnic minorities. Surgery. 2016;160(3):805–12.
Wee C, Davis R, Chiodi S, et al. Sex, race, and the adverse effects of social stigma vs. other quality of life factors among primary care patients with moderate to severe obesity. J Gen Intern Med. 2015;30(2):229–35.
White MA, O'Neil PM, Kolotkin RL, et al. Gender, race, and obesity-related quality of life at extreme levels of obesity. Obes Res. 2004;12(6):949–55.
Palmisano S, Silvestri M, Giuricin M, et al. Preoperative predictive factors of successful weight loss and glycaemic control 1 year after gastric bypass for morbid obesity. Obes Surg. 2015;25(11):2040–6.
Ortega E, Morinigo R, Flores L, et al. Predictive factors of excess body weight loss 1 year after laparoscopic bariatric surgery. Surg Endosc. 2012;26(6):1744–50.
Livhits M, Mercado C, Yermilov I, et al. Preoperative predictors of weight loss following bariatric surgery: systematic review. Obes Surg. 2012;22(1):70–89.
Forbush S, Nof L, Echternach J, et al. Influence of activity levels and energy intake on percent excess weight loss after Roux-en-Y gastric bypass. Obes Surg. 2011;21(11):1731–8.
Forbush SW, Nof L, Echternach J, et al. Influence of activity on quality of life scores after RYGBP. Obes Surg. 2011;21(8):1296–304.
Konttinen H, Peltonen M, Sjostrom L, et al. Psychological aspects of eating behavior as predictors of 10-y weight changes after surgical and conventional treatment of severe obesity: results from the Swedish obese subjects intervention study. Am J Clin Nutr. 2015;101(1):16–24.
Wee CC, Apovian CM, Blackburn GL et al. Expectations for weight loss and willingness to accept risk among patients seeking weight loss surgery. Arch Surg 2012.
Kolotkin RL, Crosby RD, Kosloski KD, et al. Development of a brief measure to assess quality of life in obesity. Obes Res. 2001;9(2):102–11.
Karlsson J, Persson LO, Sjostrom L, et al. Psychometric properties and factor structure of the Three-Factor Eating Questionnaire (TFEQ) in obese men and women. Results from the Swedish Obese Subjects (SOS) study. Int J Obes Relat Metab Disord. 2000;24(12):1715–25.
Sallis JF, Haskell WL, Wood PD, et al. Physical activity assessment methodology in the Five-City Project. Am J Epidemiol. 1985;121(1):91–106.
Wee CC, Mukamal KJ, Huskey KW, et al. High-risk alcohol use after weight loss surgery. Surg Obes Relat Dis. 2014;10(3):508–13.
Limbach KE, Ashton K, Merrell J, et al. Relative contribution of modifiable versus non-modifiable factors as predictors of racial variance in roux-en-Y gastric bypass weight loss outcomes. Obes Surg. 2014;24(8):1379–85.
Acknowledgments
The study was funded by a grant from the National Institutes of Health (R01DK073302, PI Wee). Dr. Wee is also supported by a NIH Midcareer Mentorship Award (K24DK087932). The funder had no role in the design and conduct of the study; collection, management, analysis, and interpretation of the data; and preparation, review, or approval of the manuscript. Ms. Chiodi had full access to the data and takes responsibility for the integrity and accuracy of the data.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
The study was funded by a grant from the National Institutes of Health (R01DK073302, PI Author 1). Author 1 is also supported by a NIH Midcareer Mentorship Award (K24DK087932).
Conflict of Interest
Author 3 reports grants from National Institutes of Health, from Myos, from Aspire Bariatrics, and from GI Dynamics; grants and personal fees from Amylin, from Sanofi-Aventis, from Orexigen, and from Takeda; personal fees from Merck, from Johnson & Johnson, from Arena, from Nutrisystem, from Zafgen, from EnteroMedics, and from NovoNordisk for work unrelated to the current project. Author 2 reports stock options as a consultant for Allurion. All other authors declare they have no conflict of interest.
Ethical Statement
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Consent Statement
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Wee, C.C., Jones, D.B., Apovian, C. et al. Weight Loss After Bariatric Surgery: Do Clinical and Behavioral Factors Explain Racial Differences?. OBES SURG 27, 2873–2884 (2017). https://doi.org/10.1007/s11695-017-2701-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-017-2701-y