Abstract
Background
Many studies have analyzed the impact of sleeve gastrectomy (SG) on weight loss and/or the evolution of obesity-related comorbid conditions, but few have reported the long-term outcomes after surgery. The objective of this study was to investigate the outcomes after SG on weight loss, obesity-related comorbid conditions, quality of life (QoL), and GERD symptoms (GERDS) beyond 5 years.
Methods
A prospective database was retrospectively searched for the following factors: gender, age, anthropometrics, presence of comorbid conditions, QoL (BAROS questionnaire), and presence of GERDS. The data were analyzed before and at 1 and 6 years after surgery.
Results
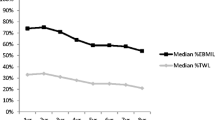
Of the 64 patients included, 32.8% were lost to follow-up (76% during the first postoperative year). A complete follow-up of >5 years was obtained for 41 patients. Before surgery, mean excess BMI was 22 ± 7 kg/m2, and 26.8% of patients had GERDS. Percent excess BMI loss was 55 ± 30% at 1 year and 48 ± 27% at 6 years. Preoperative BMI and absence of type 2 diabetes (T2D) before surgery were the only independent variables for long-term failure. Six years after SG, remission from metabolic comorbidities was as follows: 50% for T2D, 28% for blood hypertension, 58% for dyslipidemia, and 33% for sleep-apnea syndrome. Thirty percent of patients with preoperative GERD had resolution of symptoms at 6 years whereas 9 patients (32%) had de novo GERD. QoL was improved for 62% of patients at 6 years.
Conclusion
The benefits of SG on weight loss, resolution of comorbidities, and QoL were maintained in the long term for most patients.






Similar content being viewed by others
References
Eschwege E, Charles MA, Basdevant A. ObEpi Roche 2012. Enquête épidémiologique nationale sur le surpoids et l’obésité. 6ème ed. Mississauga: Publisher Hoffmann-La Roche Ltd; 2012. http://www.roche.fr/content/dam/roche_france/fr_FR/doc/obepi_2012.pdf.
Ogden CL, Caroll MD, Kit BK, et al. Prevalence of childhood and adult obesity in the United States, 2011-2012. JAMA. 2014;311(8):806–14. doi:10.1001/jama.2014.732.
Prospective Studies Collaboration, Whitlock G, Lewington S, et al. Body-mass index and cause-specific mortality in 900 000 adults: collaborative analyses of 57 prospective studies. Lancet. 2009 Mar 28;373(9669):1083–96.
Colquitt JL, Pickett K, Loveman E, et al. Surgery for weight loss in adults. Cochrane Database Syst Rev. 2014;8:CD003641. doi:10.1002/14651858.CD003641.
Sovik TT, Aasheim ET, Taha O, et al. Weight loss, cardiovascular risk factors, and quality of life after gastric bypass and duodénal switch: a randomised trial. Ann Intern Med. 2011;155:281–91. doi:10.7326/0003-4819-155-5-201109060-00005.
National Institute for Clinical Excellence. Obesity: the prevention, identification, assessment and management of overweight and obesity in adults and children: clinical guidelines. London: Publisher National Institute for Health and Clinical Excellence (UK); 2006. Bookshelf ID: NBK264165
Obésité: prise en charge chirurgicale chez l’adulte. Synthèse des recommandations de bonne pratique. Haute Autorité de Santé, Saint-Denis La Plaine, 2011; www.has-sante.fr
Iannelli A, Dainese R, Piche T, et al. Laparoscopic sleeve gastrectomy for morbid obesity. World J Gastroenterol. 2008;14(6):821–7.
Stenard F, Iannelli A. Laparoscopic sleeve gastrectolmy and gastroesophageal reflux. World J Gastroenterol. 2015;21(36):10348–57. doi:10.3748/wjg.v21 .i36.10348.
Wolf AM, Falcone AR, Kortner B, et al. BAROS: an effective system to evaluate the results of patients after bariatric surgery. Obes Surg. 2000;10(5):445–50.
Reinhold RB. Critical analysis of long term weight loss following gastric bypass. Surg Gynecol Obstet. 1982;155(3):385–94.
Himpens J, Dobbeleir J, Peeters G. Long-term results of laparoscopic sleeve gastrectomy for obesity. Ann Surg. 2010 Aug;252(2):319–24. doi:10.1097/SLA.0b013e3181e90b31.
Diamantis T, Apostolou KG, Alexandrou A, et al. Review of long-term weight loss results after laparoscopic sleeve gastrectomy. Surg Obes Relat Dis. 2014;10(1):177–83. doi:10.1016/j.soard.2013.11.007.
McVay MA, Friedman KE, Applegate KL, et al. Patient predictors of follow-up care attendance in Roux-en-Y gastric bypass patients. Surg Obes Relat Dis. 2013;9(6):956–62. doi:10.1016/j.soard.2012.11.005.
Sockalingam S, Cassin S, Hawa R, et al. Predictors of post-bariatric surgery appointment attendance: the role of relationship style. Obes Surg. 2013;23(12):2026–32. doi:10.1007/s11695-013-1009-9.
Melissas J, Braghetto I, Molina JC, et al. Gastroesophageal reflux disease and sleeve gastrectomy. Obes Surg. 2015;25(12):2430–5. doi:10.1007/s11695-015-1906-1.
Petersen WV, Meile T, Küper MA, et al. Functional importance of laparoscopic sleeve gastrectomy for lower esophageal sphincter in patients with morbid obesity. Obes Surg. 2012;22(3):360–6. doi:10.1007/s11695-011-0536-5.
DuPree CE, Blair K, Steele SR, et al. Laparoscpic sleeve gastrectomy in patients with preexisting gastroesophageal reflux disease: a national analysis. JAMA Surg. 2014;149(4):328–34. doi:10.1001/jamasurg.2013.4323.
Miguel GP, Azevedo JL, de Souza PH, et al. Erosive esophagitis after bariatric surgery: banded vertical gastrectomy versus banded Roux-en-Y gastric bypass. Obes Surg. 2011;21(2):167–72. doi:10.1007/s11695-010-0321-x.
Nini E, Slim K, Scesa JL, et al. Evaluation of laparoscopic bariatric surgery using the BAROS score. Ann Chir. 2002;127(2):107–14.
Moorehead MK, Ardelt-Gattinger E, Lechner H, et al. The validation of the Moorehead-Ardelt quality of life questionnaire II. Obes Surg. 2003 Oct;13(5):684–92. doi:10.1381/096089203322509237.
Driscoll S, Gregory DM, Fardy JM, et al. Long-term health-related quality of life in bariatric surgery patients: a systematic review and meta-analysis. Obesity. 2016;24(1):60–70. doi:10.1002/oby.21322.
Fezzi M, Kolotkin RL, Nedelcu M, et al. Improvement in quality of life after laparoscopic sleeve gastrectomy. Obes Surg. 2011 Aug;21(8):1161–7. doi:10.1007/s11695-011-0361-x.
Alley JB, Fenton SJ, Harnisch MC, et al. Quality of life after sleeve gastrectomy and adjustable gastric banding. Surg Obes Relat Dis. 2012 Feb;8(1):31–40. doi:10.1016/j.soard.2011.03.009.
Iannelli A, Schneck AS, Noel P, et al. Re-sleeve gastrectomy for failed laparoscopic sleeve gastrectomy: a feasibility study. Obes Surg. 2011 Jul;21(7):832–5. doi:10.1007/s11695-010-0290-0.
Iannelli A, Debs T, Martin F, et al. Laparoscopic conversion of sleeve gastrectomy to Roux-en-Y gastric bypass: indications and preliminary results. Surg Obes Relat Dis. 2016;12 doi:10.1016/j.soard.2016.04.008.
Moszkowicz D, Rau C, Guenzi M, et al. Laparoscopic omega-loop gastric bypass for the conversion of failed sleeve gastrectomy: early experience. J Visc Surg. 2013 Dec;150(6):373–8. doi:10.1016/j.jviscsurg.2013.08.010.
Iannelli A, Schneck A-S, Topart P, et al. Laparoscopic sleeve gastrectomy followed by duodenal switch in selected patients versus single-stage duodenal switch for superobesity: case-control study. Surg Obes Relat Dis. 2013 Aug;9(4):531–8. doi:10.1016/j.soard.2012.02.003.
Martini F, Paolino L, Marzano E, et al. Single-anastomosis pylorus-preserving bariatric procedure: review of the literature. Obes Surg. 2016;26(10):2503–15. doi:10.1007/s11695-016-2310-1.
Nedelcu M, Noel P, Iannelli A, et al. Revised sleeve gastrectomy (re-sleeve). Surg Obes Relat Dis. 2015;11(6):1282–8. doi:10.1016/j.soard.2015.02.009.
Lee W-J, Ser K-H, Chong K, et al. Laparoscopic sleeve gastrectomy for diabetes treatment in nonmorbidly obese patients: efficacy and change of insulin secretion. Surgery. 2010 May 1;147(5):664–9. doi:10.1016/j.surg.2009.10.059.
Aminian A, Brethauer SA, Andalib A, et al. Can sleeve gastrectomy “cure” diabetes? Long-term metabolic effects of sleeve gastrectomy in patients with type 2 diabetes. Ann Surg. 2016;264(4):674–81. doi:10.1097/SLA.0000000000001857.
Jiménez A, Ceriello A, Casamitjana R, et al. Remission of type 2 diabetes after Roux-en-Y gastric bypass or sleeve gastrectomy is associated with distinct glycemic profile. Ann Surg. 2015;261(2):316–22. doi:10.1097/SLA.0000000000000586.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Each author completed the COI form.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
For this retrospective study, formal consent is not required.
Informed Consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Chuffart, E., Sodji, M., Dalmay, F. et al. Long-Term Results After Sleeve Gastrectomy for Gastroesophageal Reflux Disease: a Single-Center French Study. OBES SURG 27, 2890–2897 (2017). https://doi.org/10.1007/s11695-017-2698-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-017-2698-2