Abstract
Background
Use of a preoperative diet before bariatric surgery to improve postoperative complications and weight loss has been reported. However, evidence supporting this diet for laparoscopic sleeve gastrectomy (LSG) is insufficient. We aimed to investigate postoperative outcomes influenced by preoperative diet before LSG.
Methods
This study included 247 patients who underwent LSG after preoperative weight management. They were classified according to preoperative weight changes (group 1, weight gain; group 2, 0–3.0% total weight loss (TWL); group 3, 3.1–5.0% TWL; group 4, >5.1% TWL) and investigated for early postoperative complications and weight loss at 1 year.
Results
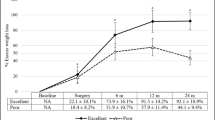
There were 37 patients in group 1, 79 in group 2, 64 in group 3, and 67 in group 4. There were no statistical differences in initial physical status among the 4 groups. The median BMI declined to 27.6 kg/m2 in the entire group. Although the average %TWL during the combined preoperative and postoperative periods showed no statistical differences (P = 0.69), the average %TWL during the postoperative period decreased gradually as the extent of preoperative weight loss increased (P = 0.01). The early postoperative complication rate for the entire group was 6.9%; it tended to be lower as the extent of preoperative weight loss increased. However, a multiple logistic regression model demonstrated that the preoperative diet was not a statistical predictor of reduced early postoperative complications (P = 0.28).
Conclusion
The extent of preoperative weight loss statistically affected postoperative weight loss. A preoperative diet might have minor advantages in reducing the risk of early postoperative complications.


Similar content being viewed by others
Change history
11 February 2019
In Table 2 on p. 2517 the heading for Group 3 should read as follows:
11 February 2019
In Table 2 on p. 2517 the heading for Group 3 should read as follows:
11 February 2019
In Table 2 on p. 2517 the heading for Group 3 should read as follows:
11 February 2019
In Table 2 on p. 2517 the heading for Group 3 should read as follows:
11 February 2019
In Table 2 on p. 2517 the heading for Group 3 should read as follows:
11 February 2019
In Table 2 on p. 2517 the heading for Group 3 should read as follows:
References
Angrisani L, Satonicola A, Iovino P, et al. Bariatric surgery worldwide 2013. Obes Surg. 2015;25:1822–32.
Seki Y, Kasama K, Hashimoto K. Long-term outcome of laparoscopic sleeve gastrectomy in morbidly obese Japanese patients. Obes Surg. 2016;26(1):138–45.
Brethauer SA, Kim J, el Chaar M, et al. Standardized outcomes reporting in metabolic and bariatric surgery. Obes Surg. 2015;11(3):489–506.
Fris RJ. Preoperative low energy diet diminishes liver size. Obes Surg. 2004;14(9):1165–70.
Colles SL, Dixon JB, Marks P, et al. Preoperative weight loss with a very-low-energy diet: quantitation of changes in liver and abdominal fat by serial imaging. Am J Clin Nutr. 2006;84(2):301–11.
Kalinowski P, Paluszkiewicz R, Wróblewski T. Ghrelin, leptin, and glycemic control after sleeve gastrectomy versus roux-en-Y gastric bypass-results of a randomized clinical trial. Surg Obes Relat Dis. 2016;13(2):181–8.
Noel P. Marius Nedelcu David, NoccaRevised, et al. sleeve gastrectomy: another option for weight loss failure after sleeve gastrectomy. Surg Endosc. 2014;28:1096–102.
Gagner M, Deitel M, Kalberer TL, et al. The second international consensus summit for sleeve gastrectomy, march 19-21, 2009. Surg Obes Relat Dis. 2009;5:476–85.
Braghetto I, Cort C, Herquiñigo D, et al. Evaluation of the radiological gastric Capacityand evolution of the BMI 2–3 years after sleeve gastrectomy. Obes Surg. 2009;19(9):1262–9.
Lauti M, Kularatna M, Hill G, et al. Weight gain following sleeve gastrectomy-a systematic review. Obes Surg. 2016;26:1326–34.
Alvarado R, Alami RS, Hsu G, et al. The impact of preoperative weight loss in patients undergoing laparoscopic roux-en-Y gastric bypass. Obes Surg. 2005;15(9):1282–6.
Brethauer SA, Hammel JP, Schauer PR. Systematic review of sleeve gastrectomy as staging and primary bariatric procedure. Surg Obes Relat Dis. 2009;5(4):469–75.
Shi X, Karmali S, Sharma AM, et al. A review of laparoscopic sleeve gastrectomy for morbid obesity. Obes Surg. 2010;20(8):1171–7.
Benotti PN, Still CD, Wood GC, et al. Preoperative weight loss before bariatric surgery. Arch Surg. 2009;144(12):1150–5.
Still CD, Benotti P, Wood GC, et al. Outcome of preoperative weight loss in high-risk patients undergoing gastric bypass surgery. Arch Surg. 2007;142(10):994–8.
Van Nieuwenhove Y, Dambrauskas Z, Campillo-Soto A, et al. Preoperative very low-calorie diet and operative outcome after laparoscopic gastric bypass: a randomized multicenter study. Arch Surg. 2011;146(11):1300–5.
DeMaria EJ, Portenier D. Wolfe l. obesity surgery mortality risk score: proposal for a clinically useful score to predict mortality risk in patients undergoing gastric bypass. Surg Obes Relat Dis. 2007;3(2):134–40.
Sarela AI, Dexter SP, McMahon MJ. Use of the obesity surgery mortality risk score to predict complications of laparoscopic bariatric surgery. Obes Surg. 2011;21(11):1698–703.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no competing interests.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed Consent
Informed consent was obtained from all individual participants included in this study.
Grant Information and an Acknowledgment of Grant Support
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Rights and permissions
About this article
Cite this article
Watanabe, A., Seki, Y., Haruta, H. et al. Preoperative Weight Loss and Operative Outcome After Laparoscopic Sleeve Gastrectomy. OBES SURG 27, 2515–2521 (2017). https://doi.org/10.1007/s11695-017-2697-3
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-017-2697-3