Abstract
Background
A current management dilemma in laparoscopic sleeve gastrectomy (LSG) patients is the development of significant gastroesophageal reflux symptoms after surgery. Treatment is typically directed towards reducing acid reflux despite the surgical removal of parietal cell mass. In contrast, laparoscopic Roux-en-Y gastric bypass (LRYGB) has been known to reduce or resolve preoperative reflux symptoms. The objective of this study was to determine the incidence of preoperative and postoperative reflux of LSG and LRYGB patients, and review reflux treatment type and response.
Methods
A retrospective chart review was performed for patients undergoing either LSG or LRYGB between January 2010 and December 2012 as part of the Weight Wise program, Royal Alexandra Hospital, Edmonton, Canada.
Results
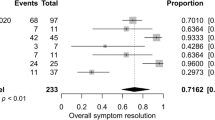
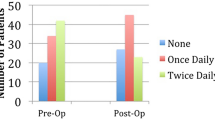
A total of 387 cases were included in our review. We observed a significant reduction in BMI postoperatively for both LSG and LRYGB groups (p < 0.001). Between surgical groups, preoperative proton-pump inhibitor (PPI) use was not significantly different; however, at 1 month (p < 0.05) to 1–2 years (p < 0.001), there was significantly increased PPI use in patients after LSG in comparison to LRYGB. Of the LSG patients that continued their PPI treatment after surgery, 58 % increased, 42 % continued the same, and 0 % decreased their dose 1 year after surgery.
Conclusions
Reflux symptoms are significantly increased after LSG in comparison to LRYGB patients. In addition, LSG patients more frequently require initiation of reflux treatment after surgery than that of LRYGB patients. Patients reported postoperative reflux symptom relief with acid-suppressant therapies.



Similar content being viewed by others
References
Todkar J, Shah S, Shah P, et al. Long-term effects of laparoscopic sleeve gastrectomy in morbidly obese subjects with type 2 diabetes mellitus. Surg Obes Relat Dis. 2010;6:142–5.
Snyder-Marlow G, Taylor D, Lenhard J. Nutrition care for patients undergoing laparoscopic sleeve gastrectomy for weight loss. Am Diet Assoc. 2010;110(4):600–7.
Roa P, Kaidar-Person O, Pinto D, et al. Laparoscopic sleeve gastrectomy as treatment for morbid obesity: technique and short-term outcome. Obes Surg. 2006;16:1323–6.
Jacobs M, Bisland W, Gomez E, et al. Laparoscopic sleeve gastrectomy: a retrospective review of 1- and 2-year results. Surg Endosc. 2010;24:781–5.
Lakdawala M, Bhasker A, Mulchandani D, et al. Comparison between the results of laparoscopic sleeve gastrectomy and laparoscopic Roux-en-Y gastric bypass in the Indian population: a retrospective 1 year study. Obes Surg. 2010;20:1–6.
Weiner R, Weiner S, Pomhoff I, et al. Laparoscopic sleeve gastrectomy—influence of sleeve size and resected gastric volume. Obes Surg. 2007;17:1297–305.
Melissas J, Koukouraki S, Askoxylakis J, et al. Sleeve gastrectomy: a restrictive procedure? Obes Surg. 2007;17(1):57–62.
Nocca D, Krawczykowsky D, Bomans B, et al. A prospective multicenter study of 163 sleeve gastrectomies: results at 1 and 2 years. Obesity Surgery. 2008;18:560–5.
DuPree C, Blair K, Steele S, et al. Laparoscopic sleeve gastrectomy in patients with preexisting gastroesophageal reflux disease: a national analysis. JAMA Surgery. 2014;February:E1-7.
Madalosso C, Gurski R, Callegari-Jacques S, et al. The impact of gastric bypass on gastroesophageal reflux disease in patients with morbid obesity. Ann Surg. 2010;251(2):244–8.
Sarkhosh K, Birch D, Sharma A, et al. Complications associated with laparoscopic sleeve gastrectomy for morbid obesity: a surgeon’s guide. Can J Surg. 2013;56(5):347–52.
Carabotti M, Silecchia G, Greco F, et al. Impact of laparoscopic sleeve gastrectomy on upper gastrointestinal symptoms. Obes Surg. 2013;23:1551–7.
National Institutes of Health. Clinical guidelines on the identification, evaluation, and treatment of overweight and obesity in adults: the evidence report. Obes Res. 1998;6(6):464.
Tuckman B. Selecting a statistical test in: conducting educational research. 5th ed. Wadsworth: Harcourt Brace College Publishers; 1999. p. Table 37.1.
Braghetto I, Lanzarini E, Korn O, et al. Manometric changes of the lower esophageal sphincter after sleeve gastrectomy in obese patients. Obes Surg. 2010;20:357–62.
Friedenberg F, Xanthopoulos M, Foster G, et al. The association between gastroesophageal reflux disease and obesity. Am J Gastroenterol. 2008;103(8):2111–22.
Carter P, LeBlanc K, Hausmann M, et al. Association between gastroesophageal reflux disease and laparoscopic sleeve gastrectomy. Surg Obes Relat Dis. 2011;7:569–74.
Langer F, Hoda M, Bohdjalian A, et al. Sleeve gastrectomy and gastric banding: effects on plasma ghrelin levels. Obes Surg. 2005;15:1024–9.
Katz P, Gerson L, Vela M. Diagnosis and management of gastroesophageal reflux disease. Am J Gastroenterol. 2013;108:308–2.
Akkary E, Duffy A, Bell R. Deciphering the sleeve: technique, indications, efficacy, and safety of sleeve gastrectomy. Obes Surg. 2008;18:1323–9.
Herbella F, Vicentine F, Del Grande J, et al. Postprandial proximal gastric acid pocket and gastric pressure in patients after gastric surgery. Neurogastroenterol Mot. 2011;23:52–e4.
Roslin M. Comment on: association between gastroesophageal reflux disease and laparoscopic sleeve gastrectomy. Surg Obes Relat Dis. 2011;7:572–4.
Triantafyllidis G, Lazoura O, Sioka E, et al. Anatomy and complications following laparoscopic sleeve gastrectomy: radiological evaluation and imaging pitfalls. Obes Surg. 2011;21:473–8.
Jacques Himpens M, Giovanni Dapri M, Guy Bernard C. A prospective randomized study between laparoscopic gastric banding and laparoscopic isolated sleeve gastrectomy: results after 1 and 3 years. Obes Surg. 2006;16:1450–6.
Chiu S, Birch D, Shi X, et al. Effect of sleeve gastrectomy on gastroesophageal reflux disease: a systematic review. Surg Obes Relat Dis. 2011;7:510–5.
Cottam D, Qureshi F, Mattar S, et al. Laparoscopic sleeve gastrectomy as an initial weight-loss procedure for high-risk patients with morbid obesity. Surg Endosc. 2006;20:859–63.
Han S, Kim W, Oh J. Results of laparoscopic sleeve gastrectomy (LSG) at 1 year in morbidly obese Korean patients. Obes Surg. 2005;15:1469–75.
Parikh M, Issa R, McCrillis A, et al. Surgical strategies that may decrease leak after laparoscopic sleeve gastrectomy. Ann Surg. 2013;257(2):231–7.
Rosenthal R, International Sleeve Gastrectomy Expert Panel. International sleeve gastrectomy expert panel consensus statement: best practice guidelines based on experience of >12,000 cases. Surg Obes Relat Dis. 2012;8(1):8–19.
Kohn G, Price R, Demeester S, et al. SAGES guidelines committee. Guidelines for the management of hiatal hernia. California: Society of American Gastrointestinal and Endoscopic Surgeons; 2013. Available from: http://www.sages.org/publications/guidelines/guidelines-for-the-management-of-hiatal-hernia/.
Bohdjalian A, Langer F, Shakeri-Leidenmuhler S, et al. Sleeve gastrectomy as sole and definitive bariatric procedure: 5-year results for weight loss and ghrelin. Obes Surg. 2010;20:535–40.
Cremonini F, Ziogas D, Chang H, et al. Meta-analysis: the effects of placebo treatment on gastro-oesophageal reflux disease. Alimentary Pharmacol Therapy. 2010;32(1):29–42.
Del Genio G, Tolone S, Limongelli P, et al. Sleeve gastrectomy and development of “de novo” gastroesophageal reflux. Obes Surg. 2014;24(1):71–7.
Peterli R, Borbely Y, Kern B, et al. Early results of the swiss multicentre bypass or sleeve study (SM-BOSS). Ann Surg. 2013;258(5):690–5.
Deitel M, Gagner M, Erickson A, et al. Third international summit: current status of sleeve gastrectomy. Surg Obes Relat Dis. 2011;7:749–5.
Crookes P. Physiology of reflux disease: role of the lower esophageal sphincter. Surg Endosc. 2006;20:S462–6.
Jacobsen S, Olesen S, Dirksen C, et al. Changes in gastrointestinal hormone responses, insulin sensitivity, and beta-cell function within 2 weeks after gastric bypass in non-diabetic subjects. Obes Surg. 2012;22:1084–96.
Laffin M, Chau J, Gill R, et al. Sleeve gastrectomy and gastroesophageal reflux disease. J Obes. 2013;1–6.
Conflict of Interest
Authors Ms. Sheppard, Dr. Sadowski, and Dr. Karmali have no conflict of interest. Drs. de Gara and Birch have contributions from Ethicon Johnson & Johnson and Stryker in the manner of surgical equipment for resident training.
Statement of Consent
Informed consent was waived for all participants in the study as approved by the University of Alberta Human Research Ethics Board.
Statement of Human and Animal Rights
For this type of study (retrospective), formal consent is not required.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sheppard, C.E., Sadowski, D.C., de Gara, C.J. et al. Rates of Reflux Before and After Laparoscopic Sleeve Gastrectomy for Severe Obesity. OBES SURG 25, 763–768 (2015). https://doi.org/10.1007/s11695-014-1480-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-014-1480-y