Abstract
Background
Patients who have undergone bariatric surgery have increased risks of developing micronutrient deficiencies. Translational research investigating the actual micronutrient intake of bariatric patients is limited. We examined the micronutrient intake of a multicentre cohort of laparoscopic adjustable gastric banding patients 1 year post-surgery. These data were compared to micronutrient recommendations for the general population.
Methods
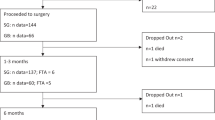
Consecutive patients from three bariatric surgery facilities in Melbourne, Australia, were invited to participate 12 months post-operatively. A validated food frequency questionnaire was posted to 215 prospective participants.
Results
Of the 52 participants, micronutrient intakes from food and fluids alone were below population recommendations for calcium, folate, magnesium, potassium, retinol equivalents, thiamin and vitamin E. Males did not meet the recommended intakes for zinc, and iron intakes in pre-menopausal women were insufficient. Intakes lower than recommended levels for these micronutrients suggest inadequate intake of foods from vegetable, dairy, lean meat (or alternatives) and wholegrains. Micronutrient intakes below recommended levels in this patient group can be further explained by their macronutrient intakes that suggested diets of poor nutrient density. Recommendations for supplementation in this group have wide variations, usually having been developed through the presence of clinical and biochemical deficiencies.
Conclusions
Nutritional supplementation should be more extensive in scope and dosage than is currently recommended by some professional guidelines. Further long-term studies are needed to explore both macro- and micronutrient intakes on the morbidity and mortality of this patient population.
Similar content being viewed by others
References
Sjöström L, Narbro K, Sjöström CD, et al. Effects of bariatric surgery on mortality in Swedish obese subjects. N Engl J Med. 2007;357(8):741–52.
American Society for Metabolic and Bariatric Surgery. Metabolic and bariatric surgery fact sheet. (2012). http://s3.amazonaws.com/publicASMBS/Resources/Fact-Sheets/Metabolic-Bariatric-Surgery-Fact-Sheet-ASMBS2012.pdf. Accessed 19 Feb 2013
Australian Institute of Health and Welfare. Weight loss surgery in Australia. Cat. No. HSE 91. Canberra: AIHW. 2010. http://www.aihw.gov.au/publication-detail/?id=6442472385. Accessed 15 Jan 2013
Shankar P, Boylan M, Sriram K. Micronutrient deficiencies after bariatric surgery. Nutrition. 2010;26(11):1031–7.
Mechanick JI, Youdim A, Jones DB, et al. Clinical practice guidelines for the perioperative nutritional, metabolic, and nonsurgical support of the bariatric surgery patient—2013 update: cosponsored by American Association of Clinical Endocrinologists, the Obesity Society, and American Society for Metabolic & Bariatric Surgery. Endocr Prac. 2013;19(2):e1–36.
Parkes E. Nutritional management of patients after bariatric surgery. Am J Med Sci. 2006;331(4):207–13.
Dodsworth A, Warren-Forward H, Baines S. A systematic review of dietary intake after laparoscopic adjustable gastric banding. J Hum Nutr Diet. 2011;24(4):327–41.
Ernst B, Thurnheer M, Wilms B, et al. Differential changes in dietary habits after gastric bypass versus gastric banding operations. Obes Surg. 2009;19(3):274–80.
Pournaras DJ, le Roux CW. After bariatric surgery, what vitamins should be measured and what supplements should be given? Clin Endocr. 2009;71:322–5.
McGrice M, Porter J. What are gastric banding patients eating one year post-surgery? Obes Surg. 2012;22(12):1855–8.
Toh SY, Zarshenas N, Jorgensen J. Prevalence of nutrient deficiencies in bariatric patients. Nutrition. 2009;25(11):1150.
Aills L, Blankenship J, Buffington C, et al. ASMBS allied health nutritional guidelines for the surgical weight loss patient. Surg Obes Relat Dis. 2008;4(5):S73–S108.
Dietitians Association of Australia. Best practice guidelines for the treatment of overweight and obesity. 2005. http://daa.collaborative.net.au/files/DINER/Obesity%20Guidelines%20(Final).pdf. Accessed 4 Jan 2011
Giles GG, Ireland PD. Dietary questionnaire for epidemiological studies (version 2). Melbourne: The Cancer Council Victoria. 1996. http://www.cancervic.org.au/about-our-research/epidemiology/nutritional_assessment_services. Accessed 10 Jan 2013
Hodge A, Patterson AJ, Brown WJ, et al. The Anti-Cancer Council of Victoria FFQ: relative validity of nutrient intakes compared with weighed food records in young to middle-aged women in a study of iron supplementation. Aust NZ J Public Health. 2000;24(6):576–83.
Department of Health and Ageing, National Health and Medical Research Council. Nutrient reference values for Australia and New Zealand including Recommended Dietary Intakes. 2006, www.nhmrc.gov.au/_files_nhmrc/publications/attachments/n35.pdf. Accessed 12 Dec 2011
Colossi FG, Casagrande D, Chatkin R, et al. Need for multivitamin use in the postoperative period of gastric bypass. Obes Surg. 2008;18(2):187–91.
Gasteyger C, Suter M, Calmes JM, et al. Changes in body composition, metabolic profile and nutritional status 24 months after gastric banding. Obes Surg. 2006;16:243–50.
Giusti V, Gasteyger C, Suter M, et al. Gastric banding induces negative bone remodelling in the absence of secondary hyperparathyroidism: potential role of serum C telepeptides for follow-up. Int J Obes. 2005;29:1429–535.
Nadler EP, Heekoung AY, Ren CJ, et al. An update on 73 US obese pediatric patients treated with laparoscopic adjustable gastric banding: comorbidity resolution and compliance data. J Pediatr Surg. 2008;43:141–6.
Sola E, Morillas C, Garzon S, et al. Rapid onset of Wernicke's encephalopathy following gastric restrictive surgery. Obes Surg. 2003;13:661–2.
Ledoux S, Msika S, Moussa F, et al. Comparison of nutritional consequences of conventional therapy of obesity, adjustable gastric banding and gastric bypass. Obes Surg. 2006;16:1041–9.
Gardner C, Kim S, Bersamin A, et al. Micronutrient quality of weight-loss diets that focus on macronutrients: results from the A to Z study. Am J Clin Nutr. 2010;92:304–12.
Gibson RS. Principles of nutritional assessment. 2nd ed. New York: Oxford University Press; 2005.
Conflict of Interest
Melanie McGrice owns a private dietetic practice in Melbourne and has accepted paid speaking engagements on bariatric surgery for Nestle and Diabetes Australia. Judi Porter declares no competing interests.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
McGrice, M.A., Porter, J.A. The Micronutrient Intake Profile of a Multicentre Cohort of Australian LAGB Patients. OBES SURG 24, 400–404 (2014). https://doi.org/10.1007/s11695-013-1101-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-013-1101-1