Abstract
Backround
Diabetes surgery in nonobese or moderately obese patients is an emerging topic. The identification of preoperative factors predicting diabetes outcome following bariatric surgery, especially for metabolic nonresponders, is imperative.
Methods
Between 2005 and 2011, 235 patients underwent bariatric surgery for morbid obesity. Eighty-two of 235 patients had type 2 diabetes mellitus (T2DM). Data from this subgroup were investigated with univariate and multivariate analyses to identify predictors for metabolic nonresponse after surgery.
Results
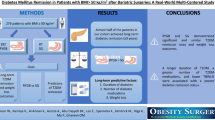
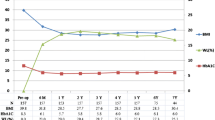
Diabetes did not improve in 17/82 patients within 3 months after surgery. No correlation between excess body weight loss and metabolic response was detected. In univariate analysis, preoperative duration of diabetes was significantly longer in the nonresponder group (9.146 vs. 6.270 years; *p = 0.016), preoperative HbA1c levels were significantly higher among the nonresponders than among the responders (8.341 vs. 7.781 %; *p = 0.033), and more patients in the nonresponder group were reliant on a multi-drug approach preoperatively (*p = 0.045). In multivariate analysis, age, preoperative doses of insulin, and preoperative oral antidiabetics showed positive correlation to metabolic nonresponse after surgery (*p = 0.04; *p = 0.021; *p = 0.021). Metabolic failure rate was lower after Roux-en-Y gastric bypass compared to other bariatric procedures (**p = 0.008).
Conclusions
A long history of preoperative T2DM, high preoperative HbA1c levels, and a preoperative therapy consisting of diverse approaches to diabetes treatment may be factors predicting failure of diabetes improvement in the early postoperative course after bariatric surgery. Age, preoperative insulin, and oral antidiabetic medication can be regarded as independent, significant predictors for metabolic outcome after bariatric surgery.
Similar content being viewed by others
References
Rubino F, Gagner M. Potential of surgery for curing type 2 diabetes mellitus. Ann Surg. 2002;236(5):554–9.
Rubino F. Is type 2 diabetes an operable intestinal disease? A provocative yet reasonable hypothesis. Diabetes Care. 2008;31 Suppl 2:290–6.
Buchwald H, Avidor Y, Braunwald E, et al. Bariatric surgery: a systematic review and meta-analysis. JAMA. 2004;292(14):1724–37.
Rubino F, Kaplan LM, Schauer PR, et al. The Diabetes Surgery Summit consensus conference: recommendations for the evaluation and use of gastrointestinal surgery to treat type 2 diabetes mellitus. Ann Surg. 2010;251(3):399–405.
Alberti KG, Zimmet PZ. Definition, diagnosis and classification of diabetes mellitus and its complications. Part 1: diagnosis and classification of diabetes mellitus provisional report of a WHO consultation. Diabet Med. 1998;15(7):539–53.
Rosenstock J, Banarer S, Fonseca VA, et al. The 11-beta-hydroxysteroid dehydrogenase type 1 inhibitor INCB13739 improves hyperglycemia in patients with type 2 diabetes inadequately controlled by metformin monotherapy. Diabetes Care. 2010;33(7):1516–22.
Dixon JB, Zimmet P, Alberti KG, et al. Bariatric surgery: an IDF statement for obese Type 2 diabetes(1). Diabet Med. 2011;28(6):628–42.
Gregg EW, Cheng YJ, Narayan KM, et al. The relative contributions of different levels of overweight and obesity to the increased prevalence of diabetes in the United States: 1976–2004. Prev Med. 2007;45(5):348–52.
Cohen R, Pinheiro JS, Correa JL, et al. Laparoscopic Roux-en-Y gastric bypass for BMI < 35 kg/m2: a tailored approach. Surg Obes Relat Dis. 2006;2(3):401–4. discussion 04.
Lee WJ, Wang W, Lee YC, et al. Effect of laparoscopic mini-gastric bypass for type 2 diabetes mellitus: comparison of BMI > 35 and <35 kg/m2. J Gastrointest Surg. 2008;12(5):945–52.
Scopinaro N, Adami GF, Papadia FS, et al. Effects of biliopanceratic diversion on type 2 diabetes in patients with BMI 25 to 35. Ann Surg. 2011;253(4):699–703.
de Paula AL, Macedo AL, Prudente AS, et al. Laparoscopic sleeve gastrectomy with ileal interposition (“neuroendocrine brake”)—pilot study of a new operation. Surg Obes Relat Dis. 2006;2(4):464–7.
Gianos M, Abdemur A, Fendrich I, et al. Outcomes of bariatric surgery in patients with body mass index <35 kg/m2. Surg Obes Relat Dis. 2011;8(1):25–30.
Li Q, Chen L, Yang Z, et al. Metabolic effects of bariatric surgery in type 2 diabetic patients with BMI <35 kg/m2. Diabetes Obes Metab. 2011;14(3):262–70.
Hall TC, Pellen MG, Sedman PC, et al. Preoperative factors predicting remission of type 2 diabetes mellitus after Roux-en-Y gastric bypass surgery for obesity. Obes Surg. 2010;20(9):1245–50.
Schauer PR, Burguera B, Ikramuddin S, et al. Effect of laparoscopic Roux-en Y gastric bypass on type 2 diabetes mellitus. Ann Surg. 2003;238(4):467–84. discussion 84-5.
Huang CK, Shabbir A, Lo CH, et al. Laparoscopic Roux-en-Y gastric bypass for the treatment of type II diabetes mellitus in Chinese patients with body mass index of 25–35. Obes Surg. 2011;21(9):1344–9.
Hamza N, Abbas MH, Darwish A, et al. Predictors of remission of type 2 diabetes mellitus after laparoscopic gastric banding and bypass. Surg Obes Relat Dis. 2011;7(6):691–6.
Shukla AP, Ahn SM, Patel RT, et al. Surgical treatment of type 2 diabetes: the surgeon perspective. Endocrine. 2011;40(2):151–61.
Rubino F, Schauer PR, Kaplan LM, et al. Metabolic surgery to treat type 2 diabetes: clinical outcomes and mechanisms of action. Annu Rev Med. 2010;61:393–411.
Benaiges D, Goday A, Ramon JM, et al. Laparoscopic sleeve gastrectomy and laparoscopic gastric bypass are equally effective for reduction of cardiovascular risk in severely obese patients at one year of follow-up. Surg Obes Relat Dis. 2011;7(5):575–80.
Lakdawala MA, Bhasker A, Mulchandani D, et al. Comparison between the results of laparoscopic sleeve gastrectomy and laparoscopic Roux-en-Y gastric bypass in the Indian population: a retrospective 1 year study. Obes Surg. 2010;20(1):1–6.
Lee WJ, Ser KH, Chong K, et al. Laparoscopic sleeve gastrectomy for diabetes treatment in nonmorbidly obese patients: efficacy and change of insulin secretion. Surgery. 2010;147(5):664–9.
Conflict of interest
All authors declare to have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
Christian Jurowich and Andreas Thalheimer contributed equally to this work.
Rights and permissions
About this article
Cite this article
Jurowich, C., Thalheimer, A., Hartmann, D. et al. Improvement of Type 2 Diabetes Mellitus (T2DM) After Bariatric Surgery—Who Fails in the Early Postoperative Course?. OBES SURG 22, 1521–1526 (2012). https://doi.org/10.1007/s11695-012-0676-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-012-0676-2