Abstract
Background
There is a strong association between sleep-disordered breathing (SDB) and obesity. However, there are no studies addressed to determining the prevalence of SDB in morbidly obese premenopausal women, the most frequent group of patients requiring bariatric surgery. To evaluate the prevalence and characteristics of sleep apnea-hypopnea syndrome (SAHS) and obesity hypoventilation syndrome (OHS) in morbidly obese pre-menopausal women included in a program of bariatric surgery.
Methods
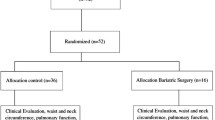
A total of 88 consecutive morbidly obese pre-menopausal women (38.3 ± 8.1 years, body mass index (BMI) 48.0 ± 6.7 kg/m2) being evaluated for bariatric surgery at the outpatient obesity unit of a university hospital were prospectively recruited. SDB examinations included a non-attended respiratory polygraphy, pulmonary function testing, and an awake arterial gasometry. SAHS was defined as an apnea-hypopnea index (AHI) ≥10 events per hour and patients were divided in non-SAHS (AHI <10), mild (AHI: 10–20), moderate (AHI: 21–30), and severe (AHI >30). OHS was defined as the presence of hypercapnia (PaCO2 > 45). Somnolence was evaluated using the Epworth sleepiness scale.
Results
A total of 66 (75.0%) obese patients had SAHS: 25 (28.4%) mild, 14 (15.9%) moderate, and 27 (30.6%) severe. Seven (7.9%) obese patients presented OHS. Excessive daily somnolence was recorded in only 11 (16.6%) of the obese women with SAHS. In multiple regression analysis, BMI was the only variable independently associated with SAHS severity.
Conclusions
Due to its high prevalence and severity, it should be recommended to investigate SDB in all morbidly obese pre-menopausal women awaiting bariatric surgery even in the absence of excessive daytime sleepiness.

Similar content being viewed by others
References
Flegal KM, Carroll MD, Ogden CL, et al. Prevalence and trends in obesity among US adults, 1999–2000. JAMA. 2002;288:1723–7.
Neira M, de Onis M. The Spanish strategy for nutrition, physical activity and the prevention of obesity. Br J Nutr. 2006;96(Suppl 1):S8–11.
Pope G, Birkmeyer J, Finlayson S. National trends in utilization and in-hospital outcomes of bariatric surgery. J Gastrointest Surg. 2002;6:855–61.
Lecube A, Fort JM, Baena JA, et al. Initial experience with 150 consecutive gastric bypass: an approach to the learning curve of bariatric procedures. Obes Metab. 2007;3:175–82.
Young T, Skatrud J, Peppard PE. Risk factors for obstructive sleep apnea in adults. JAMA. 2004;291:2013–6.
Young T, Peppard PE, Taheri S. Excess weight and sleep-disordered breathing. J Appl Physiol. 2005;99:1592–9.
Peppard PE, Young T, Palta M, et al. Prospective study of the association between sleep-disordered breathing and hypertension. N Engl J Med. 2000;342:1378–84.
Shamsuzzaman AS, Somers VK. Fibrinogen, stroke, and obstructive sleep apnea: an evolving paradigm of cardiovascular risk. Am J Respir Crit Care Med. 2000;162:2018–20.
Marin JM, Carrizo SJ, Vicente E, et al. Long-term cardiovascular outcomes in men with obstructive sleep apnoea-hypopnoea with or without treatment with continuous positive airway pressure: an observational study. Lancet. 2005;365:1046–53.
Yaggi HK, Concato J, Kernan WN, et al. Obstructive sleep apnea as a risk factor for stroke and death. N Engl J Med. 2005;353:2034–41.
Marti S, Sampol G, Muñoz X, et al. Mortality in severe sleep apnoea/hypopnoea patients: impact of treatment. Eur Respir J. 2002;20:1511–8.
Berg G, Delaive K, Manfreda J, et al. The use of health-care resources in obesity hypoventilation syndrome. Chest. 2001;120:377–83.
Nowbar S, Burkart KM, Gonzales R, et al. Obesity-associated hypoventilation in hospitalized patients: prevalence, effects, and outcome. Am J Med. 2004;116:1–7.
Perez de Llano LA, Golpe R, Ortiz Piquer M, et al. Short-term and long-term effects of nasal intermittent positive pressure ventilation in patients with obesity-hypoventilation syndrome. Chest. 2005;128:587–94.
Engleman HM, Martin SE, Deary IJ, et al. Effect of CPAP therapy on daytime function in patients with mild sleep apnoea/hypopnoea syndrome. Thorax. 1997;52:114–9.
Baldwin CM, Griffith KA, Nieto FJ, et al. The association of sleep-disordered breathing and sleep symptoms with quality of life in the Sleep Heart Health Study. Sleep. 2001;24:96–105.
George CF. Reduction in motor vehicle collisions following treatment of sleep apnoea with nasal CPAP. Thorax. 2001;56:508–12.
Young T, Palta M, Dempsey J, et al. The occurrence of sleep-disordered breathing among middle age adults. N Engl J Med. 1993;328:1230–5.
Redline S, Kump K, Tishler PV, et al. Gender differences in sleep disordered breathing in a community-based sample. Am J Respir Crit Care Med. 1994;149:722–6.
Bixler EO, Vgontzas AN, Lin HM, et al. Prevalence of sleep-disordered breathing in women: effects of gender. Am J Respir Crit Care Med. 2001;163:608–13.
Block AJ, Wynne JW, Boysen PG. Sleep-disordered breathing and nocturnal oxygen desaturation in postmenopausal women. Am J Med. 1980;69:75–9.
Young T, Peppard PE, Gottlieb DJ. Epidemiology of obstructive sleep apnea: a population health perspective. Am J Respir Crit Care Med. 2002;165:1217–39.
Gastrointestinal surgery for severe obesity. National Institutes of Health Conference Statement. Am J Clin Nutr. 1992;55:615S–9.
International Diabetes Federation: The IDF consensus worldwide definition of the metabolic syndrome [article online], 2005. Available from www.idf.org/webdata/docs/IDFmetasyndromedefinition.pdf.
American Diabetes Association. Diagnosis and classification of diabetes mellitus. Diabetes Care. 2005;28:S37–42.
Esnaola S, Duran J, Infante-Rivard C, et al. Diagnostic accuracy of a portable device (Mesam IV) in suspected sleep apnoea. Eur Respir J. 1996;9:2597–605.
Lloberes P, Sampol G, Levy G, et al. Influence of setting on unattended respiratory monitoring in the sleep apnoea-hypopnoea syndrome. Eur Respir J. 2001;16:530–4.
Quanjer PH, Tammeling GJ, Cotes LE. Lung volumes and forced ventilatory flows. Eur Respir J. 1996;6(suppl 16):41–52.
Roca J, Sanchis J, Agusti-Vidal A, et al. Spirometric reference values from a Mediterranean population. Bull Eur Physiopathol Respir. 1986;22:217–24.
Johns MW. A new method for measuring daytime sleepiness: the Epworth sleepiness scale. Sleep. 1991;14:540–5.
Hiestand DM, Britz P, Goldman M, et al. Prevalence of symptoms and risk of sleep apnea in US population: results from the National Sleep Foundation sleep in America 2005 poll. Chest. 2006;130:780–6.
Resta O, Foschino-Barbaro MP, Legari G, et al. Sleep-related breathing disorders, loud snoring and excessive daytime sleepiness in obese subjects. Int J Obes Relat Metab Disord. 2001;25:669–75.
Sloan EP, Shapiro CM. Obstructive sleep apnea in a consecutive series of obese women. Int J Eating Disord. 1995;17:167–73.
Shinohara E, Kihara S, Yamashita S, et al. Visceral fat accumulation as an important risk factor for obstructive sleep apnoea syndrome in obese subjects. J Intern Med. 1997;241:11–8.
Guilleminault C, Quera Salva MA, Partinen M, et al. Women and the obstructive sleep apnoea syndrome. Chest. 1998;93:104–9.
Krystal A, Edinger J, Wohlgemuth W, et al. Sleep in peri-menopausal and post-menopausal women. Sleep Med Rev. 1998;2:243–53.
Dixon JB, Dixon ME, Anderson ML, et al. Daytime sleepiness in the obese: not as simple as obstructive sleep apnea. Obesity (Silver Spring). 2007;15:2504–11.
Pillar G, Lavie P. Psychiatric symptoms in sleep apnea syndrome: effects of gender and respiratory disturbance index. Chest. 1998;114:697–703.
Young T, Hutton R, Finn L, et al. The gender bias in sleep apnea diagnosis. Are women missed because they have different symptoms? Arch Intern Med. 1996;156:2445–51.
Pack AI, Maislin G. Who should get treated for sleep apnea? Ann Intern Med. 2001;134:1065–7.
Punjabi NM, Polotsky VY. Disorders of glucose metabolism in sleep apnea. J Appl Physiol. 2005;99:1998–2007.
Kono M, Tatsumi K, Saibara T, et al. Obstructive sleep apnea syndrome is associated with some components of metabolic syndrome. Chest. 2007;131:1387–92.
Vgontzas AN. Does obesity play a major role in the pathogenesis of sleep apnoea and its associated manifestations via inflammation, visceral adiposity, and insulin resistance? Arch Physiol Biochem. 2008;114:211–23.
Lecube A, Sampol G, Lloberes P, et al. Diabetes is an independent risk factor for severe nocturnal hypoxemia in obese patients. A case-control study. PLoS One. 2009;4:e4692.
Gupta R, Parvizi J, Hanssen AD, et al. Postoperative complication in patients with obstructive sleep apnea syndrome undergoing hip or knee replacement: a case-control study. Mayo Clin Proc. 2001;76:897–905.
Hwang S, Shakir N, Limann B, et al. Association of sleep-disordered breathing with postoperative complications. Chest. 2008;133:1128–34.
Acknowledgments
This study was supported by grants from Novo Nordisk Pharma (01/0066), the CIBER de Diabetes y Enfermedades Metabólicas Asociadas (CIBERDEM), and CIBER Enfermedades Respiratorias (CIBERER). CIBERDEM and CIBERER are initiatives of the Instituto de Salud Carlos III (ISCIII).
Conflict of interest
The authors have declared that no conflicts of interest exist with the subject of the study.
Author information
Authors and Affiliations
Corresponding author
Additional information
The contributions of A.L. and G.S. should be considered equal.
Rights and permissions
About this article
Cite this article
Lecube, A., Sampol, G., Lloberes, P. et al. Asymptomatic Sleep-disordered Breathing in Premenopausal Women Awaiting Bariatric Surgery. OBES SURG 20, 454–461 (2010). https://doi.org/10.1007/s11695-009-0033-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-009-0033-2