Abstract
Background
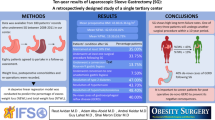
Good results obtained after laparoscopic sleeve gastrectomy (LSG), in terms of weight loss and morbidity, have been reported in few recent studies. Our team has designed a multicenter prospective study for the evaluation of the effectiveness and feasibility of this operation as a restrictive procedure.
Methods
From January 2003 to September 2006, 163 patients (68% women) with an average age of 41.57 years, were operated on with a LSG. Indications for this procedure were morbid obese [body mass index (BMI) > 40 kg/m2] or severe obese patients (BMI > 35 kg/m2) with severe comorbidities (diabetes, sleep apnea, hypertension…) with high-volume eating disorders and superobese patients (BMI > 50 kg/m2).
Results
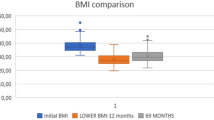
The average BMI was 45.9 kg/m2. Forty-four patients (26.99%) were superobese, 84 (51.53%) presented with morbid obesity, and 35 (21.47%) were severe obese patients. Prospective evaluations of excess weight loss, mortality, and morbidity have been analyzed. Laparoscopy was performed in 162 cases (99.39%). No conversion to laparotomy had to be performed. There was no operative mortality. Perioperative complications occurred in 12 cases (7.36%). The reoperation rate was 4.90% and the postoperative morbidity was 6.74% due to six gastric fistulas (3.66%), in which four patients (2.44%) had a previous laparoscopic adjustable gastric banding. Long-term morbidity was caused by esophageal reflux symptoms (11.80%). The percentage of loss in excessive body weight was 48.97% at 6 months, 59.45% at 1 year (120 patients), 62.02% at 18 months, and 61.52% at 2 years (98 patients). No statistical difference was noticed in weight loss between obese and extreme obese patients.
Conclusions
The sleeve gastrectomy seems to be a safe and effective restrictive bariatric procedure to treat morbid obesity in selected patients. LSG may be proposed for volume-eater patients or to prepare superobese patients for laparoscopic gastric bypass or laparoscopic duodenal switch. However, weight regained, quality of life, and evolution of morbidities due to obesity need to be evaluated in a long-term follow up.




Similar content being viewed by others
References
Marceau P, Hould F-S, et al. Biliopancreatic diversion with duodénal switch. World J Surg. 1998;22:947–54.
Regan JP, Inabnet WB, Gagner M, Pomp A. Early experience with two-stage laparoscopic Roux-en-Y gastric bypass as an alternative in the super-super obese patient. Obes Surg. 2003;13:861–4.
Silecchia G, Boru C, Pecchia A, Rizzello M, Casella G, Leonetti F, et al. Effectiveness of laparoscopic sleeve gastrectomy (first stage of biliopancreatic diversion with duodenal switch) on co-morbidities in super-obese high-risk patients. Obes Surg. 2006;16(9):1138–44.
Cottam D, Qureshi FG, Mattar SG, Sharma S, Holover S, Bonanomi G, et al. Laparoscopic sleeve gastrectomy as an initial weight-loss procedure for high-risk patients with morbid obesity. Surg Endosc. 2006;20(6):859–63.
Hamoui N, Anthone GJ, Kaufman HS, Crookes PF. Sleeve gastrectomy in the high-risk patient. Obes Surg. 2006;16(11):1445–9.
Himpens J, Dapri G, Cadiere GB. A prospective randomised study between laparoscopic adjustable gastric bandind and laparoscopic isolated sleeve gastrectomy: results after 1 and 3 years. Obes Surg. 2006;16:1450–6.
Han SM, Kim WW, Oh JH. Results of laparoscopic sleeve gastrectomy at 1 year in morbidly obese Korean patients. Obes Surg. 2005;15:1469–75.
Roa PE, Kaidar-Person O, Pinto D, Cho M, Szomstein S, Rosenthal RJ. Laparoscopic sleeve gastrectomy as treatment for morbid obesity: technique and short-term outcome. Obes Surg. 2006;16(10):1323–6.
Almogy G, Crookes PF, Anthone GJ. Longitudinal gastrectomy as a treatment for the high-risk super-obese patient. Obes Surg. 2004;14:492–7.
Milone L, Strong V, Gagner M. Laparoscopic sleeve gastrectomy is superior to endoscopic intragastric balloon as a first stage procedure for super-obese patients (BMI > or =50). Obes Surg. 2005;15:612–7.
Mognol P, Chosidow D, Marmuse JP. Laparoscopic sleeve gastrectomy as an initial bariatric operation for high-risk patients: initial results in 10 patients. Obes Surg. 2005;15:1030–3.
MacLean LD, Rhode BM, Forse RA, Nohr C. Surgery for obesity. An update of a randomized trial. Obes Surg. 1995;5:145–53.
Forsell P, et al. A gastric band with adjustable inner diameter for obesity surgery. Obes Surg. 1993;3:303–6.
Forsell P, Hellers G, Hell E. The Swedish Adjustable Gastric Banding (SAGB) for morbid obesity—weight loss, complications, pouch volume, and stoma diameter in a four-year follow-up. Acta Chir Aust. 1998;30:161–5.
Nocca D, Aggarwal R, Blanc P, Gallix B, Di Mauro GL, Millat B, et al. Laparoscopic vertical banded gastroplasty: a multicenter prospective study of 200 procedures. Surg Endosc. 2007;21:870–4.
Langer FB, Reza Hoda MA, Bohdjalian A, Felberbauer FX, Zacherl J, Wenzl E, et al. Sleeve gastrectomy and gastric banding: effects on plasma ghrelin levels. Obes Surg. 2005;15:1024–9.
Ueda K, Gagner M, Milone L, Bardaro SJ, Gong K. Sleeve gastrectomy with wrapping using polytetrafluoroethylene to prevent gastric enlargement in a porcine model. Surg Obes Relat Dis. 2007 March 30; [Epub ahead of print].
Consten EC, Gagner M, Pomp A, Inabnet WB. Decreased bleeding after laparoscopic sleeve gastrectomy with or without duodenal switch for morbid obesity using a stapled buttressed absorbable polymer membrane. Obes Surg. 2004;14:1360–6.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Nocca, D., Krawczykowsky, D., Bomans, B. et al. A Prospective Multicenter Study of 163 Sleeve Gastrectomies: Results at 1 and 2 Years. OBES SURG 18, 560–565 (2008). https://doi.org/10.1007/s11695-007-9288-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-007-9288-7