Abstract
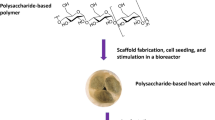
Tissue engineering heart valves (TEHV) may be the most promising valve substitute, but the study has been relatively stagnant in the recent five years due to the special position, function and mechanical property of heart valves. It is one of the key factors to select an ideal scaffold material in the construction of TEHV. And this article will briefly review the current research and progress on the scaffolds of TEHV, especially based on Chinese works.
Similar content being viewed by others
References
Shinoka T, Breuer C K, Tanel R E, Zund G, Miura T, Ma P X, Langer R, Vacanti J P, Mayer J E Jr. Tissue engineering heart valves: valve leaflet replacement study in a lamb model. Ann Thorac Surg, 1995, 60(6 Suppl): S513–S516
Steinhoff G, Stock U, Karim N, Mertsching H, Timke A, Meliss R R, Pethig K, Haverich A, Bader A. Tissue engineering of pulmonary heart valves on allogenic acellular matrix condutis: in vivo restoration of valve tissue. Circulation, 2000, 102(19 Suppl 3): III50–III55
Hoerstrup S P, Sodian R, Daebritz S, Wang J, Bacha E A, Martin D P, Moran A M, Guleserian K J, Sperling J S, Kaushal S, Vacanti J P, Schoen F J, Mayer J E Jr. Functional living trileaflet heart valves grown in vitro. Circulation, 2000, 102(19 Suppl 3): III44–III49
O’Brien M F, Goldstein S, Walsh S, Black K S, Elkins R, Clarke D. The SynerGraft valve: a new acellular (nonglutar-aldehyde-fixed) tissue heart valve for autologous recellularization first experimental studies before clinical implantation. Semin Thorac Cardiovasc Surg, 1999, 11(4 Suppl 1): 194–200
Simon P, Kasimir M T, Seebacher G, Weigel G, Ullrich R, Salzer-Muhar U, Rieder E, Wolner E. Early failure of the tissue engineered porcine heart valve Synergraft in pediatric patients. Eur J Cardiothorac Surg, 2003, 23(6): 1002–1006
Hu P. Surgical implants for tissue engineering and the processing, modification and application of biomaterials. Zhongguo Yiliao Qixie Zazhi, 2006, 12(7): 13–21 (in Chinese)
Song Q, Shi J W, Dong N G, Sun Z Q. The progress on tissue engineering heart valves. Zhonghua Shiyan Waike Zazhi, 2003, 20(4): 381–383 (in Chinese)
Flanagan T C, Pandit A. Living artificial heart valve alternatives. Eur Cell Mater, 2003, 6(1): 28–45
Dong N G, Sun Z Q, Shi J W, Zund G. Experimental construction of tissue engineering heart valves. Zhonghua Shiyan Waike Zazhi, 2002, 19(1): 88–90 (in Chinese).
Boontheekul T, Mooney D J. Protein-based signaling systems in tissue engineering. Curr Opin Biotechnol, 2003, 14(5): 559–565
Dong N G, Ye X F, Shi J W, Song Q, Sun Z Q. Comparison on decellularizing approaches of biological scaffold with porcine aortic valve for tissue engineering heart valve. Zhonghua Shiyan Waike Zazhi, 2005, 22(3): 377 (in Chinese)
Erdbrügger W, Konertz W, Dohmen P M, Posner S, Ellerbrok H, Brodde O E, Robenek H, Modersohn D, Pruss A, Holinski S, Stein-Konertz M, Pauli G. Decellularized xenogenic heart valves reveal remodeling and growth potential in vivo. Tissue Eng, 2006, 12(8): 2059–2068
Lichtenberg A, Tudorache I, Cebotari S, Ringes-Lichtenberg S, Sturz G, Hoeffler K, Hurscheler C, Brandes G, Hilfiker A, Haverich A. In vitro re-endothelialization of detergent decellularized heart valves under simulated physiological dynamic conditions. Biomaterials, 2006, 27(23): 4221–4229
Kasimir M T, Rieder E, Seebacher G, Nigisch A, Dekan B, Wolner E, Weigel G, Simon P. Decellularization does not eliminate thrombogenicity and inflammatory stimulation in tissue-engineered porcine heart valves. J Heart Valve Dis, 2006, 15(2): 278–286
Rieder E, Kasimir M T, Silberhumer G, Seebacher G, Wolner E, Simon P, Weigel G. Decellularization protocols of porcine heart valves differ importantly in efficiency of cell removal and susceptibility of the matrix to recellularization with human vascular cells. J Thorac Cardiovasc Surg, 2004, 127(2): 399–405
Shi J W, Dong N G. Application of RGD peptides in the field of tissue engineering. Zhonghua Shiyan Waike Zazhi, 2005, 22(9): 1150–1152 (in Chinese)
Bayless K J, Salazar R, Davis G E. RGD-dependent vacuolation and lumen formation observed during endothelial cell morphogenesis in three-dimensional fibrin matrices involves the alpha (v) beta (3) and alpha(5)beta(1) integrins. Am J Pathol, 2000, 156(5): 1673–1683
Stamm C, Khosravi A, Grabow N, Schmohl K, Treckmann N, Drechsel A, Nan M, Schmitz K P, Haubold A, Steinhoff G. Biomatrix/polymer composite material for heart valve tissue engineering. Ann Thorac Surg, 2004, 78(6): 2084–2092
Stock U A, Vacanti J P, Mayer Jr J E, Wahlers T. Tissue engineering of heart valves — current aspects. Thorac Cardiovasc Surg, 2002, 50(3): 184–193
Schenke-Layland K, Riemann I, Opitz F, König K, Halbhuber K J, Stock U A. comparative study of cellular and extracellular matrix composition of native and tissue engineered heart valves. Matrix Biol, 2004, 23(2): 113–125
Shangguan Y Y, Wang Y W, Wu Q, Chen G Q. The mechanical properties and in vitro biodegradation and biocompatibility of UV-treated poly (3-hydroxybutyrate-co-3-hydroxyhexanoate). Biomaterials, 2006, 27(11): 2349–2357
Lutolf M P, Hubbell J A. Synthetic biomaterials as instructive extracellular microenvironments for morphogenesis in tissue engineering. Nat Biotechnol, 2005, 23(1): 47–55
Lutolf M P, Weber F E, Schmoekel H G, Schense J C, Kohler T, Müller R, Hubbell J A. Repair of bone defects using synthetic mimetics of collagenous extracellular matrices. Nat Biotechnol, 2003, 21(5): 513–518
Lutolf M P, Lauer-Fields J L, Schmoekel H G, Metters A T, Weber F E, Fields G B, Hubbell J A. Synthetic matrix metalloproteinase-sensitive hydrogels for the conduction of tissue regeneration: engineering cell-invasion characteristics. Proc Natl Acad Sci USA, 2003, 100(9): 5413–5418
Halstenberg S, Panitch A, Rizzi S, Hall H, Hubbell J A. Biologically engineered protein-graft-poly (ethylene glycol) hydrogels: a cell adhesive and plasmin-degradable biosynthetic material for tissue repair. Biomacromolecules, 2002, 3(4): 710–723
Qi H X, Hu P, Xu J, Wang A J. Encapsulation of drug reservoirs in fibers by emulsion electrospinning: morphology characterization and preliminary release assessment. Biomacromolecules, 2006, 7(8): 2327–2330
Yoon K, Kim K, Wang X F, Fang D F, Hsiao B S, Chu B. High flux ultrafiltration membranes based on electrospun nanofibrous PAN scaffolds and chitosan coating. Polymer, 2006, 47(8): 2434–2441
Hersel U, Dahmen C, Kessler H. RGD modified polymers: biomaterials for stimulated cell adhesion and beyond. Biomaterials, 2003, 24(24): 4385–4415
Myles J L, Burgess B T, Dickinson R B. Modification of the adhesive properties of collagen by covalent grafting with RGD peptides. J Biomater Sci Polym Ed, 2000, 11(1): 69–86
Yang D Z, Hao J. Surface modification of biomaterials with poplypeptides. Guowai Yixue Shengwu Yixue Gongcheng Fence, 2004, 27(2): 65–68 (in Chinese)
Shi J W, Dong N G, Sun Z Q. Immobilization of RGD peptides onto decellularized valve scaffolds to promote cell adhesion. J Wuhan Univ Technol Mater Sci Ed, 2007, 22(4): 686–690
Shi J W, Dong N G, Sun Z Q, Qiu Y M. The role of RGD peptides and transforming growth factor-β1 in TEHV construction. Zhonghua Yi Xue Za Zhi, 2006, 86(29): 2074–2077 (in Chinese)
Dong N G, Qiu Y M, Shi J W. Applications of transforming growth factor — betal on construction of tissue engineering heart valves in vitro. Zhonghua Yi Xue Za Zhi, 2007, 87(23): 1622–1626 (in Chinese)
Hong H, Dong N G, Shi J W. Amplex Red fluorometric assay for detection of lysyl oxidase in tissue engineered heart valve. Zhongguo Xiong Xin Xueguan Linchuang Zazhi, 2007, 14(1): 27–30 (in Chinese)
Dong N G, Ye X F, Sun Z Q, Shi J W, Qiu Y M, Chen J J. Experimental study on mechanical properties of decellularized porcine aortic valve and effects of precoating methods of biological scaffold on histocompatibility. Zhonghua Wai Ke Za Zhi, 2007, 45(16): 1128–1131 (in Chinese)
Mott J D, Werb Z. Regulation of matrix biology by matrix metalloproteinases. Curr Opin Cell Biol, 2004, 16(5): 558–564
Shinoka T. Tissue engineered heart valves: autologous cell seeding on bio-degradable polymer scaffold. Artif Organs, 2002, 26(5): 402–406
Engelmayr G C Jr, Rabkin E, Sutherland F W, Schoen F J, Mayer J E Jr, Sacks M S. The independent role of cyclic flexure in the early in vitro development of an engineered heart valve tissue. Biomaterials, 2005, 26(2): 175–187
Sodian R, Hoerstrup S P, Sperling J S, Daebritz S, Martin D P, Moran A M, Kim B S, Schoen F J, Vacanti J P, Mayer J E Jr. Early in vivo experience with tissue-engineered trileaflet heart valves. Circulation, 2000, 102(19 Suppl 3): III22–III29
Davis M E, Hsieh P C, Grodzinsky A J, Lee R T. Custom design of the cardiac microenvironment with biomaterials. Circ Res, 2005, 97(1): 8–15
Author information
Authors and Affiliations
Corresponding author
Additional information
__________
Translated from Chinese Journal of Experimental Surgery, 2007, 24(3): 261–263 [译自: 中华实验外科杂志]
Rights and permissions
About this article
Cite this article
Dong, N., Shi, J., Hu, P. et al. Current progress on scaffolds of tissue engineering heart valves. Front. Med. China 2, 229–234 (2008). https://doi.org/10.1007/s11684-008-0043-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11684-008-0043-9