Abstract
Background
Previous neuroimaging research has examined static local brain activity changes in patients with anti-N-methyl-d-aspartate receptor (anti-NMDAR) encephalitis. However, the dynamic properties of local brain activity in anti-NMDAR encephalitis remain unknown.
Methods
This study used a combination of the amplitude of low-frequency fluctuation (ALFF) method and a sliding-window dynamic analysis approach to examine the time-varying local brain activity changes in anti-NMDAR encephalitis.
Results
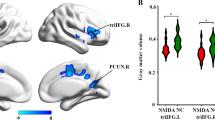
Results showed that patients with anti-NMDAR encephalitis exhibited increased dynamic ALFF (dALFF) variability in the left inferior occipital gyrus compared to healthy controls (HCs), while the patients exhibited decreased sALFF in widespread regions, including the left inferior frontal gyrus, left medial frontal gyrus, bilateral putamen, left medial superior frontal gyrus. dALFF had superior classification performance in distinguishing anti-NMDAR encephalitis patients from HCs over sALFF, but sALFF was correlated with multiple clinical and neuropsychological measures.
Conclusions
These findings may shed light on anti-NMDAR encephalitis brain dysfunction from the perspective of dynamic local brain activity. sALFF and dALFF analyses provide complementary information, emphasizing the potential usefulness of combining sALFF and dALFF in elucidating the neuropathological mechanisms of autoimmune encephalitis and may ultimately inform future disease diagnosis.



Similar content being viewed by others
Data availability
All data generated or used during the study are available from the corresponding author by request.
References
Allen, E. A., Damaraju, E., Plis, S. M., Erhardt, E. B., Eichele, T., & Calhoun, V. D. (2014). Tracking whole-brain connectivity dynamics in the resting state. Cerebral Cortex (New York, NY : 1991), 24(3), 663–76. https://doi.org/10.1093/cercor/bhs352
Ashburner, J. (2007). A fast diffeomorphic image registration algorithm. NeuroImage, 38(1), 95–113. https://doi.org/10.1016/j.neuroimage.2007.07.007
Bacchi, S., Franke, K., Wewegama, D., Needham, E., Patel, S., & Menon, D. (2018). Magnetic resonance imaging and positron emission tomography in anti-NMDA receptor encephalitis: A systematic review. Journal of Clinical Neuroscience : Official Journal of the Neurosurgical Society of Australasia, 52, 54–59. https://doi.org/10.1016/j.jocn.2018.03.026
Barkhof, F., Haller, S., & Rombouts, S. A. (2014). Resting-state functional MR imaging: A new window to the brain. Radiology, 272(1), 29–49. https://doi.org/10.1148/radiol.14132388
Brier, M. R., Day, G. S., Snyder, A. Z., Tanenbaum, A. B., & Ances, B. M. (2016). N-methyl-D-aspartate receptor encephalitis mediates loss of intrinsic activity measured by functional MRI. Journal of Neurology, 263(6), 1083–1091. https://doi.org/10.1007/s00415-016-8083-6
Burn, J. P. (1992). Reliability of the modified Rankin Scale. Stroke, 23(3), 438.
Cai, L., Liang, Y., Huang, H., Zhou, X., & Zheng, J. (2020). Cerebral functional activity and connectivity changes in anti-N-methyl-D-aspartate receptor encephalitis: A resting-state fMRI study. NeuroImage Clinical, 25, 102189. https://doi.org/10.1016/j.nicl.2020.102189
Chen, Z., Zhou, J., Wu, D., Ji, C., Luo, B., & Wang, K. (2022). Altered executive control network connectivity in anti-NMDA receptor encephalitis. Annals of Clinical and Translational Neurology, 9(1), 30–40. https://doi.org/10.1002/acn3.51487
Costafreda, S. G., Fu, C. H., Lee, L., Everitt, B., Brammer, M. J., & David, A. S. (2006). A systematic review and quantitative appraisal of fMRI studies of verbal fluency: Role of the left inferior frontal gyrus. Human Brain Mapping, 27(10), 799–810. https://doi.org/10.1002/hbm.20221
Cui, Q., Sheng, W., Chen, Y., Pang, Y., Lu, F., Tang, Q., Han, S., Shen, Q., Wang, Y., Xie, A., Huang, J., Li, D., Lei, T., He, Z., & Chen, H. (2020). Dynamic changes of amplitude of low-frequency fluctuations in patients with generalized anxiety disorder. Human Brain Mapping, 41(6), 1667–1676. https://doi.org/10.1002/hbm.24902
Dalmau, J., Gleichman, A. J., Hughes, E. G., Rossi, J. E., Peng, X., Lai, M., Dessain, S. K., Rosenfeld, M. R., Balice-Gordon, R., & Lynch, D. R. (2008). Anti-NMDA-receptor encephalitis: Case series and analysis of the effects of antibodies. The Lancet Neurology, 7(12), 1091–1098. https://doi.org/10.1016/s1474-4422(08)70224-2
Dalmau, J., Lancaster, E., Martinez-Hernandez, E., Rosenfeld, M. R., & Balice-Gordon, R. (2011). Clinical experience and laboratory investigations in patients with anti-NMDAR encephalitis. The Lancet Neurology, 10(1), 63–74. https://doi.org/10.1016/s1474-4422(10)70253-2
Deakin, J., Lennox, B. R., & Zandi, M. S. (2014). Antibodies to the N-methyl-D-aspartate receptor and other synaptic proteins in psychosis. Biological Psychiatry, 75(4), 284–291. https://doi.org/10.1016/j.biopsych.2013.07.018
Deng, S., Franklin, C. G., O’Boyle, M., Zhang, W., Heyl, B. L., Jerabek, P. A., Lu, H., & Fox, P. T. (2022). Hemodynamic and metabolic correspondence of resting-state voxel-based physiological metrics in healthy adults. NeuroImage, 250, 118923. https://doi.org/10.1016/j.neuroimage.2022.118923
du Boisgueheneuc, F., Levy, R., Volle, E., Seassau, M., Duffau, H., Kinkingnehun, S., Samson, Y., Zhang, S., & Dubois, B. (2006). Functions of the left superior frontal gyrus in humans: A lesion study. Brain : A Journal of Neurology, 129(Pt 12), 3315–3328. https://doi.org/10.1093/brain/awl244
Folstein, M. F., Folstein, S. E., & McHugh, P. R. (1975). “Mini-mental state”. A practical method for grading the cognitive state of patients for the clinician. Journal of psychiatric research, 12(3), 189–98. https://doi.org/10.1016/0022-3956(75)90026-6
Fryer, S. L., Roach, B. J., Ford, J. M., Turner, J. A., van Erp, T. G., Voyvodic, J., Preda, A., Belger, A., Bustillo, J., O’Leary, D., Mueller, B. A., Lim, K. O., McEwen, S. C., Calhoun, V. D., Diaz, M., Glover, G., Greve, D., Wible, C. G., Vaidya, J., … Mathalon, D. H. (2015). Relating Intrinsic Low-Frequency BOLD Cortical Oscillations to Cognition in Schizophrenia. Neuropsychopharmacology : Official Publication of the American College of Neuropsychopharmacology, 40(12), 2705–2714. https://doi.org/10.1038/npp.2015.119
Gonzalez-Castillo, J., Hoy, C. W., Handwerker, D. A., Robinson, M. E., Buchanan, L. C., Saad, Z. S., & Bandettini, P. A. (2015). Tracking ongoing cognition in individuals using brief, whole-brain functional connectivity patterns. Proceedings of the National Academy of Sciences of the United States of America, 112(28), 8762–8767. https://doi.org/10.1073/pnas.1501242112
Graus, F., Titulaer, M. J., Balu, R., Benseler, S., Bien, C. G., Cellucci, T., Cortese, I., Dale, R. C., Gelfand, J. M., Geschwind, M., Glaser, C. A., Honnorat, J., Höftberger, R., Iizuka, T., Irani, S. R., Lancaster, E., Leypoldt, F., Prüss, H., Rae-Grant, A., … Dalmau, J. (2016). A clinical approach to diagnosis of autoimmune encephalitis. The Lancet Neurology, 15(4), 391–404. https://doi.org/10.1016/s1474-4422(15)00401-9
Guo, Y., Lv, X., Wei, Q., Wu, Y., Chen, Y., Ji, Y., Hou, Q., Lv, H., Zhou, N., Wang, K., & Tian, Y. (2022). Impaired neurovascular coupling and cognitive deficits in anti-N-methyl-D-aspartate receptor encephalitis. Brain Imaging and Behavior, 16(3), 1065–1076. https://doi.org/10.1007/s11682-021-00588-4
Hutchison, R. M., Womelsdorf, T., Allen, E. A., Bandettini, P. A., Calhoun, V. D., Corbetta, M., Della Penna, S., Duyn, J. H., Glover, G. H., Gonzalez-Castillo, J., Handwerker, D. A., Keilholz, S., Kiviniemi, V., Leopold, D. A., de Pasquale, F., Sporns, O., Walter, M., & Chang, C. (2013). Dynamic functional connectivity: Promise, issues, and interpretations. NeuroImage, 80, 360–378. https://doi.org/10.1016/j.neuroimage.2013.05.079
Ismail, F. S., & Faustmann, P. M. (2020). Astrocytes and their potential role in anti-NMDA receptor encephalitis. Medical Hypotheses, 139, 109612. https://doi.org/10.1016/j.mehy.2020.109612
Lee, T. M., & Chan, C. C. (2000). Stroop interference in Chinese and English. Journal of Clinical and Experimental Neuropsychology, 22(4), 465–471. https://doi.org/10.1076/1380-3395(200008)22:4;1-0;ft465
Lee, T., Yuen, K., & Chan, C. (2002). Normative data for neuropsychological measures of fluency, attention, and memory measures for Hong Kong Chinese. Journal of Clinical and Experimental Neuropsychology, 24(5), 615–632. https://doi.org/10.1076/jcen.24.5.615.1001
Leonardi, N., & Van De Ville, D. (2015). On spurious and real fluctuations of dynamic functional connectivity during rest. NeuroImage, 104, 430–436. https://doi.org/10.1016/j.neuroimage.2014.09.007
Leypoldt, F., Buchert, R., Kleiter, I., Marienhagen, J., Gelderblom, M., Magnus, T., Dalmau, J., Gerloff, C., & Lewerenz, J. (2012). Fluorodeoxyglucose positron emission tomography in anti-N-methyl-D-aspartate receptor encephalitis: Distinct pattern of disease. Journal of Neurology, Neurosurgery, and Psychiatry, 83(7), 681–686. https://doi.org/10.1136/jnnp-2011-301969
Lezak, M. D., Howieson, D. B., Loring, D.W., & Fischer JS. 2004 Neuropsychological assessment: Oxford University Press, USA
Li, J., Duan, X., Cui, Q., Chen, H., & Liao, W. (2019). More than just statics: Temporal dynamics of intrinsic brain activity predicts the suicidal ideation in depressed patients. Psychological Medicine, 49(5), 852–860. https://doi.org/10.1017/s0033291718001502
Liao, W., Li, J., Ji, G. J., Wu, G. R., Long, Z., Xu, Q., Duan, X., Cui, Q., Biswal, B. B., & Chen, H. (2019). Endless Fluctuations: Temporal Dynamics of the Amplitude of Low Frequency Fluctuations. IEEE Transactions on Medical Imaging, 38(11), 2523–2532. https://doi.org/10.1109/tmi.2019.2904555
Liu, W., Yang, J., Chen, K., Luo, C., Burgunder, J., Gong, Q., & Shang, H. (2016). Resting-state fMRI reveals potential neural correlates of impaired cognition in Huntington’s disease. Parkinsonism & Related Disorders, 27, 41–46. https://doi.org/10.1016/j.parkreldis.2016.04.017
Maeder-Ingvar, M., Prior, J. O., Irani, S. R., Rey, V., Vincent, A., & Rossetti, A. O. (2011). FDG-PET hyperactivity in basal ganglia correlating with clinical course in anti-NDMA-R antibodies encephalitis. Journal of Neurology, Neurosurgery, and Psychiatry, 82(2), 235–236. https://doi.org/10.1136/jnnp.2009.198697
Mlinac, M. E., & Feng, M. C. (2016). Assessment of Activities of Daily Living, Self-Care, and Independence. Archives of Clinical Neuropsychology : The Official Journal of the National Academy of Neuropsychologists, 31(6), 506–516. https://doi.org/10.1093/arclin/acw049
Nasreddine, Z. S., Phillips, N. A., Bédirian, V., Charbonneau, S., Whitehead, V., Collin, I., Cummings, J. L., & Chertkow, H. (2005). The Montreal Cognitive Assessment, MoCA: A brief screening tool for mild cognitive impairment. Journal of the American Geriatrics Society, 53(4), 695–699. https://doi.org/10.1111/j.1532-5415.2005.53221.x
Obeso, J. A., Rodriguez-Oroz, M. C., Stamelou, M., Bhatia, K. P., & Burn, D. J. (2014). The expanding universe of disorders of the basal ganglia. Lancet (london, England), 384(9942), 523–531. https://doi.org/10.1016/s0140-6736(13)62418-6
Peer, M., Prüss, H., Ben-Dayan, I., Paul, F., Arzy, S., & Finke, C. (2017). Functional connectivity of large-scale brain networks in patients with anti-NMDA receptor encephalitis: An observational study. The Lancet Psychiatry, 4(10), 768–774. https://doi.org/10.1016/s2215-0366(17)30330-9
Probasco, J. C., Solnes, L., Nalluri, A., Cohen, J., Jones, K. M., Zan, E., Javadi, M. S., & Venkatesan, A. (2018). Decreased occipital lobe metabolism by FDG-PET/CT: An anti-NMDA receptor encephalitis biomarker. Neurology(R) Neuroimmunology & Neuroinflammation, 5(1), e413. https://doi.org/10.1212/nxi.0000000000000413
Schrouff, J., Rosa, M. J., Rondina, J. M., Marquand, A. F., Chu, C., Ashburner, J., Phillips, C., Richiardi, J., & Mourão-Miranda, J. (2013). PRoNTo: Pattern recognition for neuroimaging toolbox. Neuroinformatics, 11(3), 319–337. https://doi.org/10.1007/s12021-013-9178-1
Solnes, L. B., Jones, K. M., Rowe, S. P., Pattanayak, P., Nalluri, A., Venkatesan, A., Probasco, J. C., & Javadi, M. S. (2017). Diagnostic Value of (18)F-FDG PET/CT Versus MRI in the Setting of Antibody-Specific Autoimmune Encephalitis. Journal of Nuclear Medicine : Official Publication, Society of Nuclear Medicine, 58(8), 1307–1313. https://doi.org/10.2967/jnumed.116.184333
Sun, W., Zhang, M., Zhang, Y., Li, B., & Li, Y. (2021). Brain Intrinsic Functional Activity in Relation to Metabolic Changes in Alzheimer’s Disease: A Simultaneous PET/fMRI study. Annual International Conference of the IEEE Engineering in Medicine and Biology Society IEEE Engineering in Medicine and Biology Society Annual International Conference, 2021, 3467–3470. https://doi.org/10.1109/embc46164.2021.9630966
Swick, D., Ashley, V., & Turken, A. U. (2008). Left inferior frontal gyrus is critical for response inhibition. BMC Neuroscience, 9, 102. https://doi.org/10.1186/1471-2202-9-102
Talati, A., & Hirsch, J. (2005). Functional specialization within the medial frontal gyrus for perceptual go/no-go decisions based on “what,” “when,” and “where” related information: An fMRI study. Journal of Cognitive Neuroscience, 17(7), 981–993. https://doi.org/10.1162/0898929054475226
Thompson, G. J., Magnuson, M. E., Merritt, M. D., Schwarb, H., Pan, W. J., McKinley, A., Tripp, L. D., Schumacher, E. H., & Keilholz, S. D. (2013). Short-time windows of correlation between large-scale functional brain networks predict vigilance intraindividually and interindividually. Human Brain Mapping, 34(12), 3280–3298. https://doi.org/10.1002/hbm.22140
Titulaer, M. J., McCracken, L., Gabilondo, I., Armangué, T., Glaser, C., Iizuka, T., Honig, L. S., Benseler, S. M., Kawachi, I., Martinez-Hernandez, E., Aguilar, E., Gresa-Arribas, N., Ryan-Florance, N., Torrents, A., Saiz, A., Rosenfeld, M. R., Balice-Gordon, R., Graus, F., & Dalmau, J. (2013). Treatment and prognostic factors for long-term outcome in patients with anti-NMDA receptor encephalitis: An observational cohort study. The Lancet Neurology, 12(2), 157–165. https://doi.org/10.1016/s1474-4422(12)70310-1
Troyer, A. K. (2000). Normative data for clustering and switching on verbal fluency tasks. Journal of Clinical and Experimental Neuropsychology, 22(3), 370–378. https://doi.org/10.1076/1380-3395(200006)22:3;1-v;ft370
von Schwanenflug, N., Krohn, S., Heine, J., Paul, F., Prüss, H., & Finke, C. (2022). State-dependent signatures of anti-N-methyl-d-aspartate receptor encephalitis. Brain Communications, 4(1), fcab298. https://doi.org/10.1093/braincomms/fcab298
Wang, R., Lai, X. H., Liu, X., Li, Y. J., Chen, C., Li, C., Chi, X. S., Zhou, D., & Hong, Z. (2018). Brain magnetic resonance-imaging findings of anti-N-methyl-D-aspartate receptor encephalitis: A cohort follow-up study in Chinese patients. Journal of Neurology, 265(2), 362–369. https://doi.org/10.1007/s00415-017-8707-5
Wu, P., Pang, X., Liang, X., Wei, W., Li, X., Zhao, J., & Zheng, J. (2022). Correlation analysis between regional homogeneity and executive dysfunction in anti-N-methyl-D-aspartate receptor encephalitis patients. European Journal of Neurology, 29(1), 277–285. https://doi.org/10.1111/ene.15119
Yan, C. G., Wang, X. D., Zuo, X. N., & Zang, Y. F. (2016). DPABI: Data Processing & Analysis for (Resting-State) Brain Imaging. Neuroinformatics, 14(3), 339–351. https://doi.org/10.1007/s12021-016-9299-4
Zang, Y. F., He, Y., Zhu, C. Z., Cao, Q. J., Sui, M. Q., Liang, M., Tian, L. X., Jiang, T. Z., & Wang, Y. F. (2007). Altered baseline brain activity in children with ADHD revealed by resting-state functional MRI. Brain & Development, 29(2), 83–91. https://doi.org/10.1016/j.braindev.2006.07.002
Zhang, T., Duan, Y., Ye, J., Xu, W., Shu, N., Wang, C., Li, K., & Liu, Y. (2018). Brain MRI Characteristics of Patients with Anti-N-Methyl-D-Aspartate Receptor Encephalitis and Their Associations with 2-Year Clinical Outcome. AJNR American Journal of Neuroradiology, 39(5), 824–829. https://doi.org/10.3174/ajnr.A5593
Zheng, R., Chen, Y., Jiang, Y., Wen, M., Zhou, B., Li, S., Wei, Y., Yang, Z., Wang, C., Cheng, J., Zhang, Y., & Han, S. (2021). Dynamic Altered Amplitude of Low-Frequency Fluctuations in Patients With Major Depressive Disorder. Frontiers in Psychiatry, 12, 683610. https://doi.org/10.3389/fpsyt.2021.683610
Funding
This work was supported by funding from the National Natural Science Foundation of China (32071054).
Author information
Authors and Affiliations
Contributions
Dongpeng Wu, Yuanyuan Guo, Chenglong Li designed the study. Dongpeng Wu, Yuanyuan Guo, Xiaonan Pang, Si Xu, Juanjuan Zhang, Ling Wei, and Qianqian Li collected and analyzed the data. Dongpeng Wu and Yuanyuan Guo drafted the manuscript. Jing Du, Yanghua Tian, and Kai Wang revised the draft.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethical approval
All the experiment procedures performed in this study was approved by the ethics committee of the Anhui Medical University and were conducted in accordance with the Helsinki Declaration and its later amendments or comparable ethical standards. All participants provided informed written consent.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wu, D., Guo, Y., Li, C. et al. Dynamic and static changes of amplitude of low-frequency fluctuations in anti‑N‑methyl‑D‑aspartate receptor encephalitis. Brain Imaging and Behavior 17, 652–663 (2023). https://doi.org/10.1007/s11682-023-00790-6
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11682-023-00790-6