Abstract
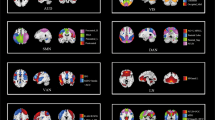
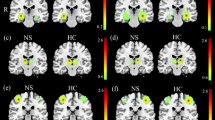
A timely and effective evaluation of the suicidal ideation bears practical meaning, particularly for the depressive who tend to disguise the real suicide intent and without obvious symptoms. Measuring individual ideation of the depression with uncertain or transient suicide crisis is the purpose. Resting-state fMRI data were collected from 78 depressed patients with variable clinical suicidal crisis. Thirty subjects were well labeled as extremely serious individuals with suicide attempters or as without suicidal ideation. A feature mask was constructed via the two sample t-test on their regional conncectivities. Then, a semi-supervised machine learning frame using the feature mask was designed to assist in clarifying gradation of suicidal susceptibility for the residual forty-eight vaguely defined subjects, by a way of Iterative Self-Organizing Data analysis techniques (ISODATA). Such semi-supervised model was designed purposely to block out the effect of disease itself on the suicide intendancy evaluation. The vague-labeled patients were divided into another two different stages relating to their suicidal susceptibility. The distance ratio of each subject to the two well-defined extreme groups in the feature space can be utilized as the suicide risk index. The re-evaluation of the Nurses’ Global Assessment of Suicide Risk (NGASR) via experts blind to original HAM-D rates was significantly correlated with the model estimation. The constructed model suggested its potential to examine the risk of suicidal in an objective way. The functional connectivity, locating mostly within the frontal-temporal circuit and involving the default mode network (DMN), were well integrated to discriminative the gradual susceptibility of suicidal.






Similar content being viewed by others
References
Angell, M. (2011). Diagnostic and statistical manual of mental disorders, 4th edition. New York Review Of Books, 58(12), 20–22.
Arbabshirani, M. R., Plis, S., Sui, J., & Calhoun, V. D. (2017). Single subject prediction of brain disorders in neuroimaging: Promises and pitfalls. NeuroImage, 145, 137–165. https://doi.org/10.1016/j.neuroimage.2016.02.079.
Bolshakova, N., & Azuaje, F. (2003). Cluster validation techniques for genome expression data. Signal Processing, 83(4), 825–833. https://doi.org/10.1016/S0165-1684(02)00475-9.
Chase, H. W., Segreti, A. M., Keller, T. A., Cherkassky, V. L., Just, M. A., Pan, L. A., & Brent, D. A. (2017). Alterations of functional connectivity and intrinsic activity within the cingulate cortex of suicidal ideators. Journal of Affective Disorders, 212, 78–85.
Cigrang, J. A., Balderrama-Durbin, C., Snyder, D. K., Talcott, G. W., Tatum, J., Baker, M., Cassidy, D., Sonnek, S., Smith Slep, A. M., & Heyman, R. E. (2015). Predictors of suicidal ideation across deployment: A prospective study. Journal of Clinical Psychology, 71(9), 828–842. https://doi.org/10.1002/jclp.22192.
Colle, R., Chupin, M., Cury, C., Vandendrie, C., Gressier, F., Hardy, P., Falissard, B., Colliot, O., Ducreux, D., & Corruble, E. (2015). Depressed suicide attempters have smaller hippocampus than depressed patients without suicide attempts. Journal of Psychiatric Research, 61, 13–18. https://doi.org/10.1016/j.jpsychires.2014.12.010.
Cutcliffe, J. R., & Barker, P. (2004). The Nurses' global assessment of suicide risk (NGASR) developing a tool for clinical practice. Journal of Psychiatric and Mental Health Nursing, 11(4), 393–400.
Deshpande, G., Baxi, M., Witte, T., & Robinson, J. L. (2016). A neural basis for the acquired capability for suicide. Frontiers in Psychiatry, 7, https://doi.org/10.3389/fpsyt.2016.00125.
Desmyter, S., van Heeringen, C., & Audenaert, K. (2011). Structural and functional neuroimaging studies of the suicidal brain. Progress in Neuro-Psychopharmacology and Biological Psychiatry, 35(4), 796–808. https://doi.org/10.1016/j.pnpbp.2010.12.026.
Ding, G., Jiang, Q., Li, L., Zhang, L., Zhang, Z. G., Soltanian-Zadeh, H., Li, Q., Whitton, P. A., Ewing, J. R., & Chopp, M. (2006). Characterization of cerebral tissue by MRI map ISODATA in embolic stroke in rat. Brain Research, 1084(1), 202–209. https://doi.org/10.1016/j.brainres.2006.02.054.
Ding, Y., Lawrence, N., Olie, E., Cyprien, F., le Bars, E., Bonafe, A., et al. (2015). Prefrontal cortex markers of suicidal vulnerability in mood disorders: A model-based structural neuroimaging study with a translational perspective. Translational Psychiatry, 24(5), 1.
Feis, D.-L., Schoene-Bake, J.-C., Elger, C., Wagner, J., Tittgemeyer, M., & Weber, B. (2013). Prediction of post-surgical seizure outcome in left mesial temporal lobe epilepsy. NeuroImage: Clinical, 2(0), 903–911. https://doi.org/10.1016/j.nicl.2013.06.010.
Filipovych, R., Davatzikos, C., & Alzheimer's Disease Neuroimaging, I. (2011a). Semi-supervised pattern classification of medical images: Application to mild cognitive impairment (MCI). Neuroimage, 55(3), 1109–1119. https://doi.org/10.1016/j.neuroimage.2010.12.066.
Filipovych, R., Resnick, S. M., & Davatzikos, C. (2011b). Semi-supervised cluster analysis of imaging data. NeuroImage, 54(3), 2185–2197. https://doi.org/10.1016/j.neuroimage.2010.09.074.
First, M. B. (1997). User's guide for the structured clinical interview for DSM-IV axis II personality disorders : SCID-II. Washington, DC: American Psychiatric Press.
Golub, T. R., Slonim, D. K., Tamayo, P., Huard, C., Gaasenbeek, M., Mesirov, J. P., Coller, H., Loh, M. L., Downing, J. R., Caligiuri, M. A., Bloomfield, C. D., & Lander, E. S. (1999). Molecular classification of cancer: Class discovery and class prediction by gene expression monitoring. Science, 286(5439), 531–537.
Hamilton, M. (1960). A rating scale for depression. Journal of Neurology, Neurosurgery, and Psychiatry, 23, 56–62.
Hectors, S. J., Jacobs, I., Strijkers, G. J., & Nicolay, K. (2014). Multiparametric MRI analysis for the identification of high intensity focused ultrasound-treated tumor tissue. PLoS One, 9(6), e99936. https://doi.org/10.1371/journal.pone.0099936.
Johnston, J. A. Y., Wang, F., Liu, J., Blond, B. N., Wallace, A., Liu, J., et al. (2017). Multimodal Neuroimaging of Frontolimbic structure and function associated with suicide attempts in adolescents and young adults with bipolar disorder. American Journal of Psychiatry, appi.ajp.2016.2011, https://doi.org/10.1176/appi.ajp.2016.15050652.
Just, M. A., Pan, L., Cherkassky, V. L., McMakin, D. L., Cha, C., Nock, M. K., & Brent, D. (2017). Machine learning of neural representations of suicide and emotion concepts identifies suicidal youth. Nature Human Behaviour, 1(12), 911–919. https://doi.org/10.1038/s41562-017-0234-y.
Kasper, S., Montgomery, S. A., Möller, H.-J., van Oers, H. J. J., Jan Schutte, A., Vrijland, P., & van der Meulen, E. A. (2010). Longitudinal analysis of the suicidal behaviour risk in short-term placebo-controlled studies of mirtazapine in major depressive disorder. World Journal of Biological Psychiatry, 11(1), 36–44. https://doi.org/10.3109/15622970701691503.
McEwen, B. S. (2015). Biomarkers for assessing population and individual health and disease related to stress and adaptation. Metabolism, 64(3 Suppl 1), S2–S10. https://doi.org/10.1016/j.metabol.2014.10.029.
Moradi, E., Pepe, A., Gaser, C., Huttunen, H., & Tohka, J. (2015). Machine learning framework for early MRI-based Alzheimer's conversion prediction in MCI subjects. NeuroImage, 104, 398–412. https://doi.org/10.1016/j.neuroimage.2014.10.002.
Pan, L. A., Ramos, L., Segreti, A., Brent, D. A., & Phillips, M. L. (2015). Right superior temporal gyrus volume in adolescents with a history of suicide attempt. The British Journal of Psychiatry, 206(4), 339–340. https://doi.org/10.1192/bjp.bp.114.151316.
Power, J. D., Barnes, K. A., Snyder, A. Z., Schlaggar, B. L., & Petersen, S. E. (2012). Spurious but systematic correlations in functional connectivity MRI networks arise from subject motion. Neuroimage, 59(3), 2142–2154. https://doi.org/10.1016/j.neuroimage.2011.10.018.
Schwarzkopf, D., de Haas, B., & Rees, G. (2012). Better ways to improve standards in brain-behavior correlation analysis. Frontiers in Human Neuroscience, 6(119).
Shen, Q., Ren, H., Fisher, M., & Duong, T. Q. (2005). Statistical prediction of tissue fate in acute ischemic brain injury. Journal of Cerebral Blood Flow and Metabolism, 25(10), 1336–1345. https://doi.org/10.1038/sj.jcbfm.9600126.
Sokolowski, M., Wasserman, J., & Wasserman, D. (2015). An overview of the neurobiology of suicidal behaviors as one meta-system. Molecular Psychiatry, 20(1), 56–71. https://doi.org/10.1038/mp.2014.101.
Soloff, P. H., & Fabio, A. (2008). Prospective predictors of suicide attempts in borderline personality disorder at one, two, and two-to-five year follow-up. Journal of Personality Disorders, 22(2), 123–134. https://doi.org/10.1521/pedi.2008.22.2.123.
Tang, Y., Jiang, W., Liao, J., Wang, W., & Luo, A. (2013). Identifying individuals with antisocial personality disorder using resting-state fMRI. [article]. PLoS One, 8(4), 1–9. https://doi.org/10.1371/journal.pone.0060652.
Taylor, W. D., Boyd, B., McQuoid, D. R., Kudra, K., Saleh, A., & MacFall, J. R. (2015). Widespread white matter but focal gray matter alterations in depressed individuals with thoughts of death. Progress in Neuro-Psychopharmacology and Biological Psychiatry, 62, 22–28. https://doi.org/10.1016/j.pnpbp.2015.05.001.
van Heeringen, K., Bijttebier, S., Desmyter, S., Vervaet, M., & Baeken, C. (2014). Is there a neuroanatomical basis of the vulnerability to suicidal behavior? A coordinate-based meta-analysis of structural and functional MRI studies. Frontiers in Human Neuroscience, 8(824).
Zeng, L. L., Shen, H., Liu, L., Wang, L., Li, B., Fang, P., Zhou, Z., Li, Y., & Hu, D. (2012). Identifying major depression using whole-brain functional connectivity: A multivariate pattern analysis. Brain, 135(Pt 5), 1498–1507. https://doi.org/10.1093/brain/aws059.
Funding
The work was supported by the grants of: the National High-tech Research and Development Program of China (2015AA020509); the National Natural Science Foundation of China (81571639, 81371522, 61372032); the Clinical MedicineTechnology Foundation of Jiangsu Province (BL2014009).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no conflict of interest
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Dai, Z., Shen, X., Tian, S. et al. Gradually evaluating of suicidal risk in depression by semi-supervised cluster analysis on resting-state fMRI. Brain Imaging and Behavior 15, 2149–2158 (2021). https://doi.org/10.1007/s11682-020-00410-7
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11682-020-00410-7