Abstract
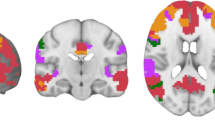
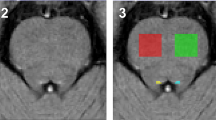
The association between gray matter (GM) density and neurophysiologic changes is still unclear in amyotrophic lateral sclerosis (ALS). We evaluated the relationship between GM density and motor system integrity combining voxel-based morphometry (VBM) and transcranial magnetic stimulation (TMS) in ALS. We included 17 ALS patients and 22 healthy controls (HC) who underwent 3D-T1-weighted imaging. Among the ALS group, we applied left motor cortex single-pulse TMS. We used whole-brain VBM comparing ALS and HC in GM density. We also conducted regression analysis to examine correlations between GM density and the following TMS parameters: motor evoked potential (MEP)/M ratio and central motor conduction time (CMCT). We found significantly decreased GM density in ALS patients in several frontal, temporal, parietal/occipital and cerebellar regions (p < 0.001 uncorrected; cluster-extent threshold k = 100 voxels per cluster). With regards to TMS parameters, ALS patients showed mostly increased MEP/M ratio and modest prolongation of CMCT. MEP/M ratio was associated with GM density in (a) rolandic operculum/inferior frontal gyrus/precentral gyrus; anterior cingulate gyrus; inferior temporal gyrus; superior parietal lobule; cuneus; superior occipital gyrus and cerebellum (positive association) and (b) paracentral lobule/supplementary motor area (negative association). CMCT was associated with GM density in (a) inferior frontal gyrus and middle cingulated gyrus (positive association) and (b) superior parietal lobule; cuneus and cerebellum (negative association). Our findings support a significant interaction between motor and extra-motor structural and functional changes and highlight that motor and extra-motor GM integrity may underlie TMS parameters of motor function in ALS patients.


Similar content being viewed by others
Abbreviations
- ALS:
-
Amyotrophic lateral sclerosis
- ALSFRS-R:
-
Revised Amyotrophic Lateral Sclerosis Functional Rating Scale
- APB:
-
Abductor pollicis brevis
- bvFTD:
-
Behavioral variant of frontotemporal dementia
- CMCT:
-
Central motor conduction time
- CSF:
-
Cerebrospinal fluid
- cTBS:
-
Continuous theta burst stimulation
- EMG:
-
Electromyographic
- fMRI:
-
Functional magnetic resonance imaging
- FWE:
-
Family-wise error
- FWHM:
-
Full-width-at-halfmaximum
- GM:
-
Gray matter
- HC:
-
Healthy control
- HR_3DT1w:
-
High resolution 3D–T1-weighted
- LMN:
-
Lower motor neuron
- MEP:
-
Motor evoked potentials
- MNI:
-
Montreal Neurological Institute
- MRI:
-
Magnetic resonance imaging
- MT:
-
Motor threshold
- RMT:
-
Resting motor threshold
- SMA:
-
Supplementary motor area
- SPM8:
-
Statistical Parametric Mapping
- T2-FLAIR:
-
T2-Fluid attenuation inversion recovery
- TE:
-
Echo time
- TIV:
-
Total intracranial volume
- TMS:
-
Transcranial magnetic stimulation
- TR:
-
Time of repetition
- TST:
-
Triple-stimulation technique
- UMN:
-
Upper motor neuron
- VBM:
-
Voxel-based morphometry
- WM:
-
White matter
References
Agosta, F., Ferraro, P. M., Riva, N., Spinelli, E. G., Chiò, A., Canu, E., et al. (2016). Structural brain correlates of cognitive and behavioral impairment in MND. Human Brain Mapping, 37, 1614–1626.
Agosta, F., Valsasina, P., Absinta, M., Riva, N., Sala, S., Prelle, A., et al. (2011). Sensorimotor functional connectivity changes in amyotrophic lateral sclerosis. Cerebral Cortex, 21, 2291–2298.
Armand, J. (1982). The origin, course and terminations of corticospinal fibers in various mammals. Progress in Brain Research, 57, 329–360.
Bae, J. S., Ferguson, M., Tan, R., Mioshi, E., Simon, N., Burrell, J., et al. (2016). Dissociation of structural and functional integrities of the motor system in amyotrophic lateral sclerosis and behavioral-variant frontotemporal dementia. Journal of Clinical Neurology, 12, 209–217.
Barker, A. T., Freeston, I. L., Jalinous, R., & Jarratt, J. A. (1987). Magnetic stimulation of the human brain and peripheral nervous system: an introduction and the results of an initial clinical evaluation. Neurosurgery, 20, 100–109.
Baumer, D., Butterworth, R., Menke, R. A. L., Talbot, K., Hofer, M., & Turner, M. R. (2014). Progressive hemiparesis (Mills Syndrome) with aphasia in amyotrophic lateral sclerosis. Neurology, 82, 457–458.
Bede, P., Bokde, A. L., Byrne, S., Elamin, M., McLaughlin, R. L., Kenna, K., et al. (2013a). Multiparametric MRI study of ALS stratified for the C9orf72 genotype. Neurology, 81, 361–369.
Bede, P., Bokde, A., Elamin, M., Byrne, S., McLaughlin, R. L., Jordan, N., et al. (2013b). Grey matter correlates of clinical variables in amyotrophic lateral sclerosis (ALS): a neuroimaging study of ALS motor phenotype heterogeneity and cortical focality. Journal of Neurology, Neurosurgery and Psychiatry, 84, 766–773.
Bede, P., & Hardiman, O. (2014). Lessons of ALS imaging: Pitfalls and future directions - A critical review. Neuroimage Clinical, 4, 436–443.
Bede, P., Elamin, M., Byrne, S., McLaughlin, R. L., Kenna, K., Vajda, A., et al. (2015). Patterns of cerebral and cerebellar white matter degeneration in ALS. Journal of Neurology, Neurosurgery and Psychiatry, 86, 468–470.
Bede, P., Iyer, P. M., Schuster, C., Elamin, M., Mclaughlin, R. L., Kenna, K., et al. (2016). The selective anatomical vulnerability of ALS: ‘disease-defining’ and ‘disease-defying’ brain regions. Amyotrophic Lateral Sclerosis and Frontotemporal Degeneration, 17, 561–570.
Bede, P., & Hardiman, O. (2017). Longitudinal structural changes in ALS: a three time-point imaging study of white and gray matter degeneration. Amyotrophic Lateral Sclerosis and Frontotemporal Degeneration, 2017; 1–10. https://doi.org/10.1080/21678421.2017.1407795.
Berardelli, A., Inghilleri, M., Formisano, R., Accornero, N., & Manfredi, M. (1987). Stimulation of motor tracts in motor neuron disease. Journal of Neurology, Neurosurgery and Psychiatry, 50, 732–737.
Braak, H. (1976). A primitive gigantopyramidal field buried in the depth of the cingulate sulcus of the human brain. Brain Research, 109, 219–223.
Braak, H., Ludolph, A. C., Neumann, M., Ravits, J., & Del Tredici, K. (2017). Pathological TDP-43 changes in Betz cells differ from those in bulbar and spinal α-motoneurons in sporadic amyotrophic lateral sclerosis. Acta Neuropathologica, 133, 79–90.
Brettschneider, J., Del Tredici, K., Toledo, J. B., Robinson, J. L., Irwin, D. J., Grossman, M., et al. (2013). Stages of pTDP-43 pathology in amyotrophic lateral sclerosis. Annals of Neurology, 74, 20–38.
Brodal, A. (1969). Neurological Anatomy in Relation to Clinical Medicine. New York: Oxford University Press.
Brooks, B. R., Miller, R. G., Swash, M., & Munsat, T. L. World Federation of Neurology Research Group on Motor Neuron Diseases. (2000). El Escorial revisited: revised criteria for the diagnosis of amyotrophic lateral sclerosis. Amyotrophic Lateral Sclerosis and Other Motor Neuron Disorders, 1, pp. 293–299.
Caspers, S., Zilles, K., Laird, A. R., & Eickhoff, S. B. (2010). ALE meta-analysis of action observation and imitation in the human brain. Neuroimage, 50, 1148–1167.
Cavanna, A. E., & Trimble, M. R. (2006). The precuneus: a review of its functional anatomy and behavioural correlates. Brain, 129, 564–583.
Cedarbaum, J. M., Stambler, N., Malta, E., Fuller, C., Hilt, D., Thurmond, B., et al. (1999). The ALSFRS-R: a revised ALS functional rating scale that incorporates assessments of respiratory function. BDNF ALS Study Group (Phase III). Journal of Neurological Sciences, 169, 13–21.
Cheah, B. C., Vucic, S., Krishnan, A. V., & Kiernan, M. C. (2010). Riluzole, neuroprotection and amyotrophic lateral sclerosis. Current Medicinal Chemistry, 17, 1942–1959.
Chenji, S., Jha, S., Lee, D., Brown, M., Seres, P., Mah, D., et al. (2016). Investigating Default Mode and Sensorimotor Network Connectivity in Amyotrophic Lateral Sclerosis. PLoS One, 11, e0157443.
Christidi, F., Karavasilis, E., Ferentinos, P., Xirou, S., Velonakis, G., Rentzos, M., et al. (2017). Investigating the neuroanatomical substrate of pathological laughing and crying in amyotrophic lateral sclerosis with multimodal neuroimaging techniques. Amyotrophic Lateral Sclerosis and Frontotemporal Degeneration. https://doi.org/10.1080/21678421.2017.1386689.
Christidi, F., Karavasilis, E., Riederer, F., Zalonis, I., Ferentinos, P., Velonakis, G., et al. (2017). Gray matter and white matter changes in non-demented amyotrophic lateral sclerosis patients with or without cognitive impairment: A combined voxel-based morphometry and tract-based spatial statistics whole-brain analysis. Brain Imaging and Behavior. https://doi.org/10.1007/s11682-017-9722-y.
Cosottini, M., Pesaresi, I., Piazza, S., Diciotti, S., Cecchi, P., Fabbri, S., et al. (2012). Structural and functional evaluation of cortical motor areas in Amyotrophic Lateral Sclerosis. Experimental Neurology, 234, 169–180.
Day, B. L., Dressler, D., Maertens de Noordhout, A., Marsden, C. D., Nakashima, K., Rothwell, J. C., et al. (1989). Electric and magnetic stimulation of human motor cortex: surface EMG and single motor unit responses. The Journal of Physiology (London), 412, 449–473.
De Marco, M., Merico, A., Berta, G., Segato, N., Citton, V., Baglione, A., et al. (2015). Morphometric correlates of dysarthric deficit in amyotrophic lateral sclerosis. Amyotrophic Lateral Sclerosis and Frontotemporal Degeneration, 16, 464–472.
Desiato, M. T., & Caramia, M. D. (1997). Towards a neurophysiological marker of amyotrophic lateral sclerosis as revealed by changes in cortical excitability. Electroencephalography and Clinical Neurophysiology, 105, 1–7.
Devinsky, O., Morrell, M. J., & Vogt, B. A. (1995). Contributions of anterior cingulate cortex to behavior. Brain, 118, 279–306.
Di Lazzaro, V., Oliviero, A., Saturno, E., Pilato, F., Dileone, M., Sabatelli, M., et al. (2004). Motor cortex stimulation for amyotrophic lateral sclerosis: time for a therapeutic trial? Clinical Neurophysiology, 115, 1479–1485.
Di Lazzaro, V., Pellegrino, G., Ranieri, F., Florio, L., Musumeci, G., Caulo, M., et al. (2017). Effects of repetitive TMS of the motor cortex on disease progression and on glutamate and GABA levels in ALS: a proof of principle study. Brain Stimulation. https://doi.org/10.1016/j.brs.2017.05.003.
Di Lazzaro, V., Ranieri, F., Capone, F., Pilato, F., Profice, P., Pellegrino, G., et al. (2014). Motor cortex stimulation for ALS: open label extension study of a previous small trial. Brain Stimulation, 2014, 7, 141–150.
Di Lazzaro, V., Ziemann, U., & Lemon, R. N. (2008). State of the art: physiology of transcranial motor cortex stimulation. Brain Stimulation, 1, 345–362.
Dum, R. P., & Strick, P. L. (1993). Cingulate Motor Areas. In B. A. Vogt & M. Gabriel (Eds.), Neurobiology of Cingulate Cortex and Limbic Thalamus. Boston, MA: Birkhäuser.
Eisen, A., Entezari-Taher, M., & Stewart, H. (1996). Cortical projections to spinal motoneurons: changes with aging and amyotrophic lateral sclerosis. Neurology, 46, 1396–1404.
Eisen, A., Lemon, R., Kiernan, M. C., Hornberger, M., & Turner, M. R. (2015). Does dysfunction of the mirror neuron system contribute to symptoms in amyotrophic lateral sclerosis? Clinical Neurophysiology, 126, 1288–1294.
Eisen, A., Shytbel, W., Murphy, K., & Hoirch, M. (1990). Cortical magnetic stimulation in amyotrophic lateral sclerosis. Muscle & Nerve, 13, 146–151.
Eisen, A., Turner, M. R., & Lemon, R. (2014). Tools and talk: an evolutionary perspective on the functional deficits associated with amyotrophic lateral sclerosis. Muscle & Nerve, 49, pp. 469–477.
Eisen, A. A., & Shtybel, W. (1990). Clinical experience with transcranial magnetic stimulation. Muscle and Nerve, 13, 995–1011.
Emeryk-Szajewska, B., Kopec, J., & Karwanska, A. (1997). The reorganization of motor units in motor neuron disease. Muscle & Nerve, 20, 306–315.
Fallini, C., Bassell, G. J., & Rossoll, W. (2012). The ALS disease protein TDP-43 is actively transported in motor neuron axons and regulates axon outgrowth. Human Molecular Genetics, 21, 3703–3718.
Fekete, T., Zach, N., Mujica-Parodi, L. R., & Turner, M. R. (2013). Multiple kernel learning captures a systems-level functional connectivity biomarker signature in amyotrophic lateral sclerosis. PLoS One, 8, e85190.
Filimon, F., Nelson, J. D., Hagler, D. J., & Sereno, M. I. (2007). Human cortical representations for reaching: mirror neurons for execution, observation, and imagery. Neuroimage, 37, 1315–1328.
Filimon, F., Rieth, C. A., Sereno, M. I., & Cottrell, G. W. (2015). Observed, executed, and imagined action representations can be decoded from ventral and dorsal areas. Cerebral Cortex, 25, 3144–3158.
Floeter, M. K., Katipally, R., Kim, M. P., Schanz, O., Stephen, M., Danielian, L., et al. (2014). Impaired corticopontocerebellar tracts underlie pseudobulbar affect in motor neuron disorders. Neurology, 83, 620–627.
Floyd, A. G., Yu, Q. P., Piboolnurak, P., Tang, M. X., Fang, Y., Smith, W. A., et al. (2009). Transcranial magnetic stimulation in ALS: utility of central motor conduction tests. Neurology, 72, 498–504.
Fountoulakis, K. N., Tsolaki, M., Chantzi, H., & Kazis, A. (2000). Mini-Mental State Examination (MMSE): A validation study in Greece. American Journal of Alzheimers’ Diseases and Other Dementias, 15, 342–345.
Fuqing, Z., Honghan, G., Fangjun, L., Ying, Z., Yufeng, Z., Renshi, X., et al. (2013). Altered motor network functional connectivity in amyotrophic lateral sclerosis: a resting-state functional magnetic resonance imaging study. Neuroreport, 24, 657–662.
Furtula, J., Johnsen, B., Frandsen, J., Rodell, A., Christensen, P. B., Pugdahl, K., et al. (2013). Upper motor neuron involvement in amyotrophic lateral sclerosis evaluated by triple stimulation technique and diffusion tensor MRI. Journal of Neurology, 260, 1535–1544.
Geevasinga, N., Menon, P., Yiannikas, C., Kiernan, M. C., & Vucic, S. (2014). Diagnostic utility of cortical excitability studies in amyotrophic lateral sclerosis. European Journal of Neurology, 21, 1451–1457.
Geyer, S., Matelli, M., Luppino, G., & Zilles, K. (2000). Functional neuroanatomy of the primate isocortical motor system. Anatomy and Embryology (Berlin), 202, 443–474.
Goldstein, L. H., & Abrahams, S. (2013). Changes in cognition and behaviour in amyotrophic lateral sclerosis: nature of impairment and implications for assessment. Lancet Neurology, 12, 368–380.
Grapperon, A. M., Verschueren, A., Duclos, Y., Confort-Gouny, S., Soulier, E., Loundou, A. D., et al. (2014). Association between structural and functional corticospinal involvement in amyotrophic lateral sclerosis assessed by diffusion tensor MRI and triple stimulation technique. Muscle & Nerve, 49, pp. 551–557.
Grèzes, J., & Decety, J. (2001). Functional anatomy of execution, mental simulation, observation, and verb generation of actions: a meta-analysis. Human Brain Mapping, 12, 1–19.
Grieve, S. M., Menon, P., Korgaonkar, M. S., Gomes, L., Foster, S., Kiernan, M. C., et al. (2015). Potential structural and functional biomarkers of upper motor neuron dysfunction in ALS. Amyotrophic Lateral Sclerorsis and Frontotemporal Degeneration, 17, 85–92.
Han, J., & Ma, L. (2006). Functional magnetic resonance imaging study of the brain in patients with amyotrophic lateral sclerosis. Chinese Medical Sciences Journal, 21, 228–233.
Hoffstaedter, F., Grefkes, C., Caspers, S., Roski, C., Fox, P. T., Zilles, K., et al. (2012). Functional connectivity of the mid-cingulate cortex. Klinische Neurophysiologie, 43, p. P128.
Huynh, W., Simon, N. G., Grosskreutz, J., Turner, M. R., Vucic, S., & Kiernan, M. C. (2016). Assessment of the upper motor neuron in amyotrophic lateral sclerosis. Clinical Neurophysiology, 127, 2643–2660.
Karandreas, N., Papadopoulou, M., Kokotis, P., Papapostolou, A., Tsivgoulis, G., & Zambelis, T. (2007). Impaired interhemispheric inhibition in amyotrophic lateral sclerosis. Amyotrophic Lateral Sclerosis, 8, 112–118.
Kaufmann, P., Pullman, S. L., Shungu, D. C., Chan, S., Hays, A. P., Del Bene, M. L., et al. (2004). Objective tests for upper motor neuron involvement in amyotrophic lateral sclerosis (ALS). Neurology, 62, 1753–1757.
Keller, J., Bohm, S., Aho-Ozhan, H. E. A., Loose, M., Gorges, M., Kassubek, J., et al. (2017). Functional reorganization during cognitive function tasks in patients with amyotrophic lateral sclerosis. Brain Imaging and Behavior. https://doi.org/10.1007/s11682-017-9738-3.
Kew, J. J., Goldstein, L. H., Leigh, P. N., Abrahams, S., Cosgrave, N., Passingham, R. E., et al. (1993). The relationship between abnormalities of cognitive function and cerebral activation in amyotrophic lateral sclerosis. A neuropsychological and positron emission tomography study. Brain, 116, 1399–1323.
Keysers, C., & Gazzola, V. (2009). Expanding the mirror: vicarious activity for actions, emotions, and sensations. Current Opinion in Neurobiology, 19, 666–671.
Kim, H. J., Oh, S. I., de Leon, M., Wang, X., Oh, K. W., Park, J. S., et al. (2017). Structural explanation of poor prognosis of amyotrophic lateral sclerosis in the non-demented state. European Journal of Neurology, 24, 122–129.
Konrad, C., Henningsen, H., Bremer, J., Mock, B., Deppe, M., Buchinger, C., et al. (2002). Pattern of cortical reorganization in amyotrophic lateral sclerosis: a functional magnetic resonance imaging study. Experimental Brain Research, 143, 51–56.
Konrad, C., Jansen, A., Henningsen, H., Sommer, J., Turski, A., Brooks, B. R., et al. (2006). Subcortical reorganization in amyotrophic lateral sclerosis. Experimental Brain Research, 172, 361–369.
Ligidakis, K., Piperos, P., Karandreas, N., & Dimitriou, D. (1990). Investigation of the central motor neuron using the method of transcranial magnetic stimulation. Encephalos, 27, 64–72. [articleGreek].
Lule, D., Diekmann, V., Kassubek, J., Jurt, A., Birbaumer, N., Ludolph, A. C., et al. (2007). Cortical plasticity in amyotrophic lateral sclerosis: motor imagery and function. Neurorehabilitation and Neural Repair, 21, 518–526.
Mackenzie, I. R., Frick, P., & Neumann, M. (2014). The neuropathology associated with repeat expansions in the C9ORF72 gene. Acta Neuropathologica Scandinavica, 127, 347–357.
Menke, R. A., Proudfoot, M., Wuu, J., Andersen, P. M., Talbot, K., Benatar, M., et al. (2016). Increased functional connectivity common to symptomatic amyotrophic lateral sclerosis and those at genetic risk. Journal of Neurology, Neurosurgery and Psychiatry, 87, 580–588.
Menon, P., Kiernan, M. C., & Vucic, S. (2015). Cortical hyperexcitability precedes lower motor neuron dysfunction in ALS. Clinical Neurophysiology, 126, 803–809.
Miller, M. W. (1987). The origin of corticospinal projection neurons in rat. Experimental Brain Research, 67, 339–351.
Mills, K. R., & Nithi, K. A. (1998). Peripheral and central motor conduction in amyotrophic lateral sclerosis. Journal of the Neurological Sciences, 159, 82–87.
Miscio, G., Pisano, F., Mora, G., & Mazzini, L. (1999). Motor neuron disease: usefulness of transcranial magnetic stimulation in improving the diagnosis. Clinical Neurophysiology, 110, 975–981.
Mohammadi, B., Kollewe, K., Samii, A., Dengler, R., & Münte, T. F. (2011). Functional neuroimaging at different disease stages reveals distinct phases of neuroplastic changes in amyotrophic lateral sclerosis. Human Brain Mapping, 32, 750–758.
Mohammadi, B., Kollewe, K., Samii, A., Krampfl, K., Dengler, R., & Munte, T. F. (2009). Changes of resting state brain networks in amyotrophic lateral sclerosis. Experimental Neurology, 217, 147–153.
Molenberghs, P., Cunnington, R., & Mattingley, J. B. (2009). Is the mirror neuron system involved in imitation? A short review and meta-analysis. Neuroscience & Biobehavioral Reviews, 33, 975–980.
Molenberghs, P., Cunnington, R., & Mattingley, J. B. (2012). Brain regions with mirror properties: a meta-analysis of 125 human fMRI studies. Neuroscience & Biobehavioral Reviews, 36, 341–349.
Montuschi, A., Iazzolino, B., Calvo, A., Moglia, C., Lopiano, L., Restagno, G., et al. (2015). Cognitive correlates in amyotrophic lateral sclerosis: a population-based study in Italy. Journal of Neurology, Neurosurgery, and Psychiatry, 86, 168–173.
Murray, N. M. F. (1999). Motor Evoked Potentials. In M. Aminoff (Ed.), Electrodiagnosis in clinical neurology (4th edn.). Elsevier Saunders, pp. 549–568.
Neary, D., Snowden, J. S., Gustafson, L., Passant, U., Stuss, D., Black, S., et al. (1998). Frontotemporal lobar degeneration: a consensus on clinical diagnostic criteria. Neurology, 51, 1546–1554.
Phukan, J., Elamin, M., Bede, P., Jordan, N., Gallagher, L., Byrne, S., et al. (2012). The syndrome of cognitive impairment in amyotrophic lateral sclerosis: a population-based study. Journal of Neurology, Neurosurgery, and Psychiatry, 83, 102–108.
Pouget, J., Trefouret, S., & Attarian, S. (2000). Transcranial magnetic stimulation (TMS): compared sensitivity of different motor response parameters in ALS. Amyotrophic Lateral Sclerosis and Other Motor Neuron Disorders, 1, pp. S45-S49.
Poujois, A., Schneider, F. C., Faillenot, I., Camdessanche, J. P., Vandenberghe, N., Thomas-Anterion, C., et al. (2013). Brain plasticity in the motor network is correlated with disease progression in amyotrophic lateral sclerosis. Human Brain Mapping, 34, 2391–2401.
Pradat, P.-F., & El Mendili, M. M. (2014). Neuroimaging to investigate multisystem involvement and provide biomarkers in amyotrophic lateral sclerosis. BioMed Research International, 2014, 467560.
Prell, T., & Grosskreutz, J. (2013). The involvement of the cerebellum in amyotrophic lateral sclerosis. Amyotrophic Lateral Sclerosis and Frontotemporal Dementia, 14, 507–515.
Ringholz, G. M., Appel, S. H., Bradshaw, M., Cooke, N. A., Mosnik, D. M., & Schulz, P. E. (2005). Prevalence and patterns of cognitive impairment in sporadic ALS. Neurology, 65, 586–590.
Sach, M., Winkler, G., Glauche, V., Liepert, J., Heimbach, B., Koch, M. A., et al. (2004). Diffusion tensor MRI of early upper motor neuron involvement in amyotrophic lateral sclerosis. Brain, 127, 340–350.
Sarica, A., Cerasa, A., Valentino, P., Yeatman, J., Trotta, M., Barone, S., et al. (2017). The corticospinal tract profile in amyotrophic lateral sclerosis. Human Brain Mapping, 38, 727–739.
Schmidt, R., Verstraete, E., de Reus, M. A., Veldink, J. H., van den Berg, L. H., & van den Heuvel, M. P. (2014). Correlation between structural and functional connectivity impairment in amyotrophic lateral sclerosis. Human Brain Mapping, 35, 4386–4395.
Schoenfeld, M. A., Tempelmann, C., Gaul, C., Kuhnel, G. R., Duzel, E., Hopf, J. M., et al. (2005). Functional motor compensation in amyotrophic lateral sclerosis. Journal of Neurology, 252, 944–952.
Schulte-Mattler, W. J., Muller, T., & Zierz, S. (1999). Transcranial magnetic stimulation compared with upper motor neuron signs in patients with amyotrophic lateral sclerosis. Journal of the Neurological Sciences, 170, 51–56.
Schulthess, I., Gorges, M., Muller, H. P., Lule, D., Del Tredici, K., Ludolph, A. C., & Kassubek, J. (2016). Functional connectivity changes resemble patterns of pTDP-43 pathology in amyotrophic lateral sclerosis. Scientific Reports, 6, 38391.
Shen, D., Cui, L., Fang, J., Cui, B., Li, D., & Tai, H. (2016). Voxel-Wise Meta-Analysis of Gray Matter Changes in Amyotrophic Lateral Sclerosis. Frontiers in Aging Neuroscience, 30, 64.
Stefan, K., Kunesch, E., Benecke, R., & Classen, J. (2001). Effects of riluzole on cortical excitability in patients with amyotrophic lateral sclerosis. Annals of Neurology, 49, 536–539.
Strigaro, G., Ruge, D., Chen, J. C., Marshall, L., Desikan, M., Cantello, R., et al. (2015). Interaction between visual and motor cortex: a transcranial magnetic stimulation study. The Journal of Physiology, 593, 2365–2377.
Tan, R. H., Devenney, E., Dobson-Stone, C., Kwok, J. B., Hodges, J. R., Kiernan, M. C., et al. (2014). Cerebellar Integrity in the Amyotrophic Lateral Sclerosis - Frontotemporal Dementia Continuum. PLoS ONE, 9(8), e105632.
Thompson, P. D., Day, B. L., Rothwell, J. C., Dick, J. P., Cowan, J. M., Asselman, P., et al. (1987). The interpretation of electromyographic responses to electrical stimulation of the motor cortex in disease of the upper motor neurone. Journal of the Neurological Sciences, 80, 91–110.
Triggs, W. J., Menkes, D., Onorato, J., Yan, R. S., Young, M. S., Newell, K., et al. (1999). Transcranial magnetic stimulation identifies upper motor neuron involvement in motor neuron disease. Neurology, 53, 605–611.
Tsermentseli, S., Leigh, P. N., & Goldstein, L. H. (2012). The anatomy of cognitive impairment in amyotrophic lateral sclerosis: more than frontal lobe dysfunction. Cortex, 48, 166–182.
Turner, M. R., & Kiernan, M. C. (2012). Does interneuronal dysfunction contribute to neurodegeneration in amyotrophic lateral sclerosis? Amyotrophic Lateral Sclerosis, 13, 245–250.
Turner, M. R., Kiernan, M. C., Leigh, P. N., & Talbot, K. (2009). Biomarkers in amyotrophic lateral sclerosis. The Lancet Neurology, 8, 94–109.
Turner, M. R., & Vestraete, E. (2015). What does imaging reveal about the pathology of amyotrophic lateral sclerosis? Current Neurology and Neuroscience Reports, 15, 45–56.
Uozumi, T., Tsuji, S., & Murai, Y. (1991). Motor potentials evoked by magnetic stimulation of the motor cortex in normal subjects and patients with motor disorders. Electroencephalography and Clinical Neurophysiology, 81, 251–256.
van der Graaff, M. M., de Jong, J. M., Baas, F., & de Visser, M. (2009). Upper motor neuron and extra-motor neuron involvement in amyotrophic lateral sclerosis: a clinical and brain imaging review. Neuromuscular Disorders, 19, 53–58.
Verstraete, E., Turner, M. R., Grosskreutz, J., Filippi, M., & Benatar, M. on Behalf of the Attendees of the 4th NISALS Meeting. (2015). Mind the gap: the mismatch between clinical and imaging metrics in ALS. Amyotrophic Lateral Sclerosis and Frontotemporal Degeneration, 16, 524–529.
Vucic, S., & Kiernan, M. C. (2006). Novel threshold tracking techniques suggest that cortical hyperexcitability is an early feature of motor neuron disease. Brain, 129, 2436–2446.
Vucic, S., & Kiernan, M. C. (2013). Utility of transcranial magnetic stimulation in delineating amyotrophic lateral sclerosis pathophysiology. Handbook of Clinical Neurology, 116, 561–575.
Vucic, S., Nicholson, G. A., & Kiernan, M. C. (2008). Cortical hyperexcitability may precede the onset of familial amyotrophic lateral sclerosis. Brain, 131, 1540–1550.
Vucic, S., Ziemann, U., Eisen, A., Hallett, M., & Kiernan, M. C. (2013a). Transcranial magnetic stimulation and amyotrophic lateral sclerosis: pathophysiological insights. Journal of Neurology Neurosurgery and Psychiatry, 84, 1161–1170.
Vucic, S., Lin, C. S., Cheah, B. C., Murray, J., Menon, P., Krishnan, A. V., et al. (2013b). Riluzole exerts central and peripheral modulating effects in amyotrophic lateral sclerosis. Brain, 136, 1361–1370.
Wagner, T., Eden, U., Fregni, F., Valero-Cabre, A., Ramos-Estebanez, C., Pronio-Stelluto, V., et al. (2008). Transcranial magnetic stimulation and brain atrophy: a computer-based human brain model study. Experimental Brain Research, 186, 539–550.
Walberg, F., & Brodal, A. (1953). Pyramidal tract fibres from temporal and occipital lobes. Brain, 76, 491–508.
Wenderoth, N., Debaere, F., Sunaert, S., & Swinnen, S. (2005). The role of anterior cingulate cortex and precuneus in the coordination of motor behaviour. European Journal of Neurosciences, 22, 235–246.
Wong, J. C. T., Concha, L., Beaulieu, C., Johnston, W., Allen, P. S., & Kalra, S. (2007). Spatial profiling of the corticospinal tract in amyotrophic lateral sclerosis using diffusion tensor imaging. Journal of Neuroimaging, 17, 234–240.
Zanette, G., Forgione, A., Manganotti, P., Fiaschi, A., & Tamburin, S. (2008). The effect of repetitive transcranial magnetic stimulation on motor performance, fatigue and quality of life in amyotrophic lateral sclerosis. Journal of the Neurological Sciences, 270, 18–22.
Zhang, J., Yin, X., Zhao, L., Evans, A. C., Song, L., Xie, B., et al. 2014. Regional alterations in cortical thickness and white matter integrity in amyotrophic lateral sclerosis. Journal of Neurology, 261, 412–421.
Zhou, C., Hu, X., Hu, J., Liang, M., Yin, X., Chen, L., et al. (2016). Altered brain network in amyotrophic lateral sclerosis: a resting graph theory-based network study at voxel-wise level. Frontiers in Neuroscience, 10, 204.
Zhou, F., Gong, H., Li, F., Zhuang, Y., Zang, Y., Xu, R., et al. (2013). Altered motor network functional connectivity in amyotrophic lateral sclerosis: a resting-state functional magnetic resonance imaging study. Neuroreport, 24, 657–662.
Acknowledgements
The study did not receive any funding. F.C. was supported by the IKY FELLOWSHIPS OF EXCELLENCE FOR POSTGRADUATE STUDIES IN GREECE - SIEMENS PROGRAM (SPHA:11118/13a) and IKY SHORT TERMS PROGRAM (2013-ΠΕ2-SHORT TERMS-18671). We acknowledge Odysseas Benekos, Giannis Spandonis and the Philips Medical System for providing all necessary research keys for MRI sequence acquisition. We also acknowledge the radiologists-technologists of Research Radiology & Medical Imaging Department (Ioannis Gkerles, Christos Lioulios, Anestis Passalis, Efstathios Xenos) for conducting participants’ MR scanning. Finally, we would like to thank patients with ALS and their families, as well as healthy volunteers for their willingness to participate to the present study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical publication statement
We confirm that we have read the Journal’s position on issues involved in ethical publication and affirm that this report is consistent with those guidelines.
Conflict of interest
The authors declare no conflicts of interest.
Additional information
Foteini Christidi and Efstratios Karavasilis shared first authorship. Ioannis Evdokimidis and Nikolaos Karandreas shared last authorship.
Rights and permissions
About this article
Cite this article
Christidi, F., Karavasilis, E., Velonakis, G. et al. Motor and extra-motor gray matter integrity may underlie neurophysiologic parameters of motor function in amyotrophic lateral sclerosis: a combined voxel-based morphometry and transcranial stimulation study. Brain Imaging and Behavior 12, 1730–1741 (2018). https://doi.org/10.1007/s11682-018-9841-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11682-018-9841-0