Abstract
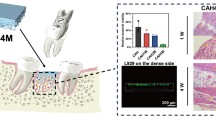
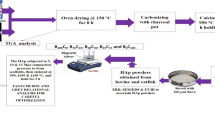
This study aims to find which lattice type and which ingredient is the best for the bone lattice for future grafting operations. Four types of lattice parts with micro and high porosity were designed to resemble the human bone structure and reach its light-weight and high surface area properties. Hydroxyapatite (HA) and tricalcium phosphate (TCP) were used in the photopolymer resin mixture for (Digital Light Processing) DLP 3D printing to give high bioactivity capability to the parts. In conclusion, microporosity HA- and TCP-doped parts were printed successfully with the DLP technique. Bioactivity tests were carried out with parts that were soaked in simulated body fluid (SBF). There is no significant weight difference in lattice parts in the time. Four weeks are sufficient time for the test. End of 2 weeks, calcium phosphate particles with around a diameter of 50-75 µm, and end of 4 weeks, calcium phosphate particles with around a diameter of 80-225 µm were observed. Apatite precipitation areas were grown on the surface in time. SEM and XRD results indicate that HA-doped and TCP-doped specimens are bioactive. A more mass increase was observed in the HA-doped specimen compared to the TCP-doped specimen.












Similar content being viewed by others
References
H.N. Chia and B.M. Wu, Recent Advances in 3D Printing of Biomaterials, J. Biol. Eng, 2015, 9(1), p 1–15.
S. Derakhshanfar, R. Mbeleck, K. Xu, X. Zhang, W. Zhong and M. Xing, 3D Bioprinting for biomedical Devices and Tissue Engineering: A Review of Recent Trends and Advances, Bioact. Mater., 2018, 3(2), p 144–156. https://doi.org/10.1016/j.bioactmat.2017.11.008
L.C. Hwa, S. Rajoo, A.M. Noor, N. Ahmad and M.B. Uday, Recent Advances in 3D Printing of Porous Ceramics: A Review, Curr. Opin. Solid State Mater. Sci., 2017, 21(6), p 323–347. https://doi.org/10.1016/j.cossms.2017.08.002
H. Jodati, B. Yılmaz and Z. Evis, A Review of Bioceramic Porous Scaffolds for Hard Tissue Applications: Effects of Structural Features, Ceram. Int., 2020, 46(10), p 15725.
N.H. Hart, S. Nimphius, T. Rantalainen, A. Ireland, A. Siafarikas and R.U. Newton, Mechanical Basis of Bone Strength: Influence of Bone Material, Bone Structure and Muscle Action, J Musculoskelet Neuronal Interact, 2017, 17(3), p 114–139.
J.D. Currey, The Structure and Mechanics of Bone, J Mater Sci, 2012, 47(1), p 41–54. https://doi.org/10.1007/s10853-011-5914-9
M. Guvendiren, J. Molde, R.M.D. Soares and J. Kohn, Designing Biomaterials for 3D Printing, ACS Biomater Sci. Eng., 2016, 2(10), p 1679–1693.
A. Butscher, M. Bohner, S. Hofmann, L. Gauckler and R. Müller, Structural and Material Approaches to Bone Tissue Engineering in Powder-based Three-dimensional Printing, Acta Biomater, 2011, 7(3), p 907–920. https://doi.org/10.1016/j.actbio.2010.09.039
L. Yuan, S. Ding and C. Wen, Additive Manufacturing Technology for Porous Metal Implant Applications and Triple Minimal Surface Structures: A Review, Bioact. Mater., 2019, 4(1), p 56–70. https://doi.org/10.1016/j.bioactmat.2018.12.003
D. Liu, W. Nie, D. Li, W. Wang, L. Zheng and J. Zhang, 3D Printed PCL / SrHA Sca Ff Old for Enhanced Bone Regeneration, Chem. Eng., 2018, 362, p 269–279.
R.K. Kankala, X.M. Xu, C.G. Liu, A.Z. Chen and S. Bin Wang, 3D-Printing of Microfibrous Porous Scaffolds Based on Hybrid Approaches for Bone Tissue Engineering, Polym. (Basel), 2018, 10(7), p 1–17.
J. Schmid, S. Schwarz, M. Fischer, S. Sudhop, H. Clausen-Schaumann, M. Schieker and R. Huber, A Laser-Cutting-Based Manufacturing Process for the Generation of Three-Dimensional Scaffolds for Tissue Engineering Using Polycaprolactone/Hydroxyapatite Composite Polymer, J. Tissue Eng., 2019 https://doi.org/10.1177/2041731419859157
S. Qiao, D. Wu, Z. Li, Y. Zhu, F. Zhan, H. Lai and Y. Gu, The Combination of Multi-Functional Ingredients-Loaded Hydrogels and Three-Dimensional Printed Porous Titanium Alloys for Infective Bone Defect Treatment, J. Tissue Eng., 2020 https://doi.org/10.1177/2041731420965797
A. Diez-Escudero, H. Harlin, P. Isaksson and C. Persson, Porous Polylactic Acid Scaffolds for Bone Regeneration: A Study of Additively Manufactured Triply Periodic Minimal Surfaces and Their Osteogenic Potential, J Tissue Eng, 2020 https://doi.org/10.1177/2041731420956541
S. Bose, S. Vahabzadeh and A. Bandyopadhyay, Bone Tissue Engineering using 3D Printing, Mater. Today, 2013, 16(12), p 496–504. https://doi.org/10.1016/j.mattod.2013.11.017
Z. Chen, Z. Li, J. Li, C.C. Liu, C. Lao, Y. Fu, C.C. Liu, Y. Li, P. Wang and Y. He, 3D Printing of Ceramics: A Review, J Eur Ceram. Soc, 2019, 39(4), p 661–687. https://doi.org/10.1016/j.jeurceramsoc.2018.11.013
J. Zhang, D. Huang, S. Liu, X. Dong, Y. Li, H. Zhang, Z. Yang, Q. Su, W. Huang, W. Zheng and W. Zhou, Zirconia Toughened Hydroxyapatite Biocomposite Formed by a DLP 3D Printing Process for Potential Bone Tissue Engineering, Mater. Sci. Eng. C, 2019, 105, p 110054. https://doi.org/10.1016/j.msec.2019.110054
O. Guillaume, M.A. Geven, C.M. Sprecher, V.A. Stadelmann, D.W. Grijpma, T.T. Tang, L. Qin, Y. Lai, M. Alini, J.D. de Bruijn, H. Yuan, R.G. Richards and D. Eglin, Surface-enrichment with Hydroxyapatite Nanoparticles in Stereolithography-fabricated Composite Polymer Scaffolds Promotes Bone Repair, Acta Biomater, 2017, 54, p 386–398. https://doi.org/10.1016/j.actbio.2017.03.006
X. Yin, N. Travitzky and P. Greil, Three-Dimensional Printing of Nanolaminated Ti3AlC2 Toughened TiAl3–Al2O3 Composites, J. Am. Ceram Soc., 2007, 90(7), p 2128–2134. https://doi.org/10.1111/j.1551-2916.2007.01668.x
Z. Chen, J. Li, C. Liu, Y. Liu, J. Zhu and C. Lao, Preparation of High Solid Loading and Low Viscosity Ceramic Slurries for Photopolymerization-based 3D Printing, Ceram. Int., 2019, 45(9), p 11549–11557. https://doi.org/10.1016/j.ceramint.2019.03.024
S.C. Cox, J.A. Thornby, G.J. Gibbons, M.A. Williams and K.K. Mallick, 3D Printing of Porous Hydroxyapatite Scaffolds Intended for use in Bone Tissue Engineering Applications, Mater. Sci. Eng, 2015, 47, p 237–247. https://doi.org/10.1016/j.msec.2014.11.024
R. Melcher, N. Travitzky, C. Zollfrank and P. Greil, 3D Printing of Al2O3/Cu–O Interpenetrating Phase Composite, J. Mater. Sci., 2011, 46(5), p 1203–1210. https://doi.org/10.1007/s10853-010-4896-3
B. Nan, X. Yin, L. Zhang and L. Cheng, Three-Dimensional Printing of Ti3SiC2-Based Ceramics, J. Am. Ceram. Soc., 2011, 94(4), p 969–972. https://doi.org/10.1111/j.1551-2916.2010.04257.x
K. Zhang, C. Xie, G. Wang, R. He, G. Ding, M. Wang, D. Dai and D. Fang, High Solid Loading, Low Viscosity Photosensitive Al2O3 Slurry for Stereolithography Based Additive Manufacturing, Ceram. Int, 2019, 45(1), p 203–208. https://doi.org/10.1016/j.ceramint.2018.09.152
J. Schmidt, H. Elsayed, E. Bernardo and P. Colombo, Digital Light Processing of Wollastonite-Diopside Glass-Ceramic Complex Structures, J. Eur. Ceram. Soc., 2018, 38(13), p 4580–4584. https://doi.org/10.1016/j.jeurceramsoc.2018.06.004
R.J. Huang, Q.G. Jiang, H.D. Wu, Y.H. Li, W.Y. Liu, X.X. Lu and S.H. Wu, Fabrication of Complex Shaped Ceramic Parts with Surface-Oxidized Si 3 N 4 Powder Via Digital Light Processing Based Stereolithography Method, Ceram. Int., 2019, 45(4), p 5158–5162. https://doi.org/10.1016/j.ceramint.2018.11.116
S.L. Sherman, O. Kadioglu, G.F. Currier, J.P. Kierl and J. Li, Accuracy of Digital Light Processing Printing of 3-dimensional Dental Models, Am. J. Orthod. Dentofac, 2020, 157(3), p 422–428. https://doi.org/10.1016/j.ajodo.2019.10.012
T. Kokubo and H. Takadama, How Useful Is SBF in Predicting in Vivo Bone Bioactivity?, Biomaterials, 2006, 27(15), p 2907–2915.
M.S. Zafar, I. Farooq, M. Awais, S. Najeeb, Z. Khurshid and S. Zohaib, Bioactive Surface Coatings for Enhancing Osseointegration of Dental Implants, Biomed. Ther. Clin. Appl. Bioact. Glas., 2019 https://doi.org/10.1016/B978-0-08-102196-5.00011-2
J. Wilson, Metallic Biomaterials: State of the Art and New Challenges, Fundam. Biomater. Met., 2018 https://doi.org/10.1016/B978-0-08-102205-4.00001-5
S.V. Dorozhkin, Calcium Orthophosphates in Nature, Biology and Medicine, Materials, 2009, 2, p 399–498.
L. Barnes, I.R. Cooper, I.M. Mehdawi and A. Young, Antibacterial Composite Restorative Materials for Dental Applications, Biomater Med Device –Assoc. Infect, 2015 https://doi.org/10.1533/9780857097224.2.199
H. Yuan, D. Barbieri, X. Luo, C.A. Van Blitterswijk, ve J.D. De Bruijn, Calcium phosphates and bone induction, Comprehensive Biomaterials II, Elsevier, 2017, s 333–349.
James Eric N., Hanna Craig, ve L.S. Nair, Chapter 16 - Nanobiomaterials for Tissue Engineering Applications, A. Vishwakarma, P. Sharpe, S. Shi, ve M.B.T.-S.C.B. and T.E. in D.S. Ramalingam, Ed., (Boston), Academic Press, 2015, s 221–234, doi:https://doi.org/10.1016/B978-0-12-397157-9.00018-7.
T. Maconachie, M. Leary, B. Lozanovski, X. Zhang, M. Qian, O. Faruque and M. Brandt, SLM Lattice Structures: properties, Performance, Applications and Challenges, Mater Des, 2019, 183, p 108137. https://doi.org/10.1016/j.matdes.2019.108137
A. Zargarian, M. Esfahanian, J. Kadkhodapour, S. Ziaei-Rad and D. Zamani, On the Fatigue Behavior of Additive Manufactured Lattice Structures, Theor. Appl. Fract. Mech., 2019, 100, p 225–232.
Z. Liu, H. Liang, T. Shi, D. Xie, R. Chen, X. Han, L. Shen, C. Wang and Z. Tian, Additive Manufacturing of Hydroxyapatite Bone Scaffolds Via Digital Light Processing and in vitro Compatibility, Ceram. Int., 2019, 45(8), p 11079–11086. https://doi.org/10.1016/j.ceramint.2019.02.195
H. Shao, J. He, T. Lin, Z. Zhang, Y. Zhang and S. Liu, 3D Gel-printing of Hydroxyapatite Scaffold for Bone Tissue Engineering, Ceram. Int., 2019, 45(1), p 1163–1170. https://doi.org/10.1016/J.CERAMINT.2018.09.300
O. Santoliquido, P. Colombo and A. Ortona, Additive Manufacturing of Ceramic Components by Digital Light Processing: A Comparison Between the “Bottom-up” and the “Top-down” Approaches, J. Eur. Ceram. Soc., 2019, 39(6), p 2140–2148. https://doi.org/10.1016/j.jeurceramsoc.2019.01.044
D. Kang, S. Park, Y. Son, S. Yeon, S.H. Kim and I. Kim, Multi-lattice Inner Structures for High-strength and Light-weight in Metal Selective Laser Melting Process, Mater. Des., 2019, 175, p 107786. https://doi.org/10.1016/j.matdes.2019.107786
J. Schmidt and P. Colombo, Digital Light Processing of Ceramic Components from Polysiloxanes, J. Eur. Ceram. Soc., 2018, 38(1), p 57–66. https://doi.org/10.1016/j.jeurceramsoc.2017.07.033
J. Schmidt, A.A. Altun, M. Schwentenwein and P. Colombo, Complex Mullite Structures Fabricated via Digital Light Processing of a Preceramic Polysiloxane with Active Alumina Fillers, J. Eur. Ceram. Soc., 2019, 39(4), p 1336–1343. https://doi.org/10.1016/j.jeurceramsoc.2018.11.038
S. Gómez, M.D. Vlad, J. López and E. Fernández, Design and Properties of 3D Scaffolds for Bone Tissue Engineering, Acta Biomater., 2016, 42, p 341–350.
N. Abbasi, S. Hamlet, R.M. Love and N.-T. Nguyen, Porous Scaffolds for Bone Regeneration, J. Sci. Adv. Mater Devices, 2020, 5(1), p 1–9. https://doi.org/10.1016/j.jsamd.2020.01.007
F.P.W. Melchels, K. Bertoldi, R. Gabbrielli, A.H. Velders, J. Feijen and D.W. Grijpma, Mathematically Defined Tissue Engineering Scaffold Architectures Prepared by Stereolithography, Biomaterials, 2010, 31(27), p 6909–6916. https://doi.org/10.1016/j.biomaterials.2010.05.068
H.A. Zaharin, A.M.A. Rani, F.I. Azam, T.L. Ginta, N. Sallih, A. Ahmad, N.A. Yunus and T.Z.A. Zulkifli, Effect of Unit Cell Type and Pore Size on Porosity and Mechanical Behavior of Additively Manufactured Ti6Al4V Scaffolds, Materials (Basel), 2018, 11(12), p 2402.
D. Ali and S. Sen, Finite Element Analysis of Mechanical Behavior, Permeability and Fluid Induced Wall Shear Stress of High Porosity Scaffolds with Gyroid and Lattice-based Architectures, J. Mech. Behav. Biomed. Mater., 2017, 75, p 262–270. https://doi.org/10.1016/j.jmbbm.2017.07.035
C. Yan, L. Hao, A. Hussein and D. Raymont, Evaluations of Cellular Lattice Structures Manufactured Using Selective Laser Melting, Int. J. Mach. Tools Manuf., 2012, 62, p 32–38. https://doi.org/10.1016/j.ijmachtools.2012.06.002
V.V. Kostov-Kytin, E. Dyulgerova, R. Ilieva and V. Petkova, Powder X-ray Diffraction Studies of Hydroxyapatite and β-TCP Mixtures Processed by High Energy Dry Milling, Ceram. Int., 2018, 44(7), p 8664–8671. https://doi.org/10.1016/j.ceramint.2018.02.094
C. Drouet, Apatite Formation: Why It May Not Work as Planned, and How to Conclusively Identify Apatite Compounds, Biomed Res Int., 2013, 2013, p 1–12.
T. Kokubo, F. Miyaji, H.-M. Kim and T. Nakamura, Spontaneous Formation of Bonelike Apatite Layer on Chemically Treated Titanium Metals, J. Am. Ceram. Soc., 1996, 79(4), p 1127–1129. https://doi.org/10.1111/j.1151-2916.1996.tb08561.x
S. Sarig and F. Kahana, Rapid Formation of Nanocrystalline Apatite, J. Cryst. Growth, 2002, 237–239, p 55–59.
X.B. Chen, Y.C. Li, P.D. Hodgson and C. Wen, The Importance of Particle Size in Porous Titanium and Nonporous Counterparts for Surface Energy and Its Impact on Apatite Formation, Acta Biomater., 2009, 5(6), p 2290–2302.
L. Jonášová, F.A. Müller, A. Helebrant, J. Strnad and P. Greil, Biomimetic Apatite Formation on Chemically Treated Titanium, Biomaterials, 2004, 25(7–8), p 1187–1194.
Acknowledgment
This study is a part of a Master’s Thesis carried out by Muhammed Enes DOKUZ at Necmettin Erbakan University, Institute of Science. Mesut UYANER and Mustafa AYDIN are the advisors of this thesis. This research was financially supported by Necmettin Erbakan University Scientific Research Projects Coordinatorship (Grant no. 191319013). Also, we wish to thank Kutahya Dumlupınar University Advanced Research Center (ILTEM) for facilitating laboratories, devices, and equipment. Marmara University Metallurgy and Materials Engineering Department member Dr. Oğuzhan Gündüz provided us TCP powder used in this study. Çanakkale Onsekiz Mart University Bioengineering Department member Dr. Özgür Özay and Ph.D. candidate Alper Önder gave support to prepare SBF. The authors especially thank them for their valuable contribution to their study.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This invited article is part of a special topical focus in the Journal of Materials Engineering and Performance on Additive Manufacturing. The issue was organized by Dr. William Frazier, Pilgrim Consulting, LLC; Mr. Rick Russell, NASA; Dr. Yan Lu, NIST; Dr. Brandon D. Ribic, America Makes; and Caroline Vail, NSWC Carderock
Rights and permissions
About this article
Cite this article
Dokuz, M.E., Aydın, M. & Uyaner, M. Production of Bioactive Various Lattices as an Artificial Bone Tissue by Digital Light Processing 3D Printing. J. of Materi Eng and Perform 30, 6938–6948 (2021). https://doi.org/10.1007/s11665-021-06067-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11665-021-06067-7