Abstract
Summary
A meta-analysis was performed to explore the association of coronary artery disease (CAD) with bone mineral density (BMD). Low BMD was not found to be associated with prevalence of CAD. Though the BMD of CADs is significantly lower than that of non-CADs, the confounding effect of aging could not be excluded as CADs might be more prevalent in older patients.
Purpose/introduction
The clinical association of coronary artery disease (CAD) with bone mineral density (BMD) has been increasingly reported, but findings on the relationship between the two age-related processes are conflicting. The aim of our study was to conduct a meta-analysis to evaluate the associations between CAD and BMD.
Methods
We searched PubMed, Embase, and Cochrane Library. Odds ratio (OR) and 95% confidence interval (CI) were pooled to assess the association between low BMD and the prevalence of CAD. For continuous data, standardized mean difference (SMD) with its 95% CI was pooled. Correlation coefficients of BMD and Gensini score were pooled after being transformed by Fischer z-transformation. Subgroup and meta-regression analyses were performed to explore the sources of heterogeneity.
Results
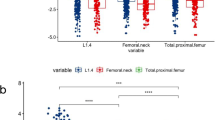
The meta-analysis involved 4170 participants from 11 studies. Pooled ORs for the incidence of CAD in patients with low BMD versus patients with normal BMD was 1.58 (95% CI 0.99–2.52, P = 0.06), and no statistical difference was found in men and women subgroups. After confounding age, the combined OR was 1.60 (95% OR 0.69–3.72, P = 0.27). Pooling data for comparing BMD of CADs and non-CADs were − 0.28 (95% CI − 0.47 to − 0.09, P = 0.004) in femoral neck and calcaneus, − 0.42 (95% CI − 0.89–0.05, P = 0.08) in lumbar spine, and − 0.25 (95% CI − 0.40 to − 0.11, P = 0.000) in the overall. A significance was detected in pooled correlation analysis between CAG Gensini score and BMD (COR = − 0.4435 [− 0.6647; − 0.1508], P = 0.004). No sources of heterogeneity were acquired, and no publication bias was identified.
Conclusions
Low BMD was not associated with the prevalence of CAD. Without age adjustment, the BMD of CADs is significantly lower than that of non-CADs, and the patients with lower BMD are inclined to more severe coronary artery lesions.





Similar content being viewed by others
Abbreviations
- BMD:
-
Bone mineral density
- CAD:
-
Coronary artery disease
- CAG:
-
Coronary angiography
- CI:
-
Confidence interval
- DXA:
-
Dual-energy X-ray absorptiometry
- NOS:
-
Newcastle-Ottawa Scale
- OR:
-
Odds ratio
- SMD:
-
Standardized mean difference
- PRISMA:
-
Preferred Reporting Items for Systematic Reviews and Meta-Analyses
- QUS:
-
Quantitative ultrasound
- WHO:
-
World Health Organization
References
Ma L, Wu Y, Wang W, Chen W (2018) Interpretation of the report on cardiovascular diseases in China (2017). Chin J Cardiovasc Med 23:3–6
Hauger AV, Bergland A, Holvik K, Ståhle A, Emaus N, Strand BH (2018) Osteoporosis and osteopenia in the distal forearm predict all-cause mortality independent of grip strength: 22-year follow-up in the population-based Tromsø study. Osteoporos Int 29(11):2447–2456
Leboime A, Confavreux CB, Mehsen N, Paccou J, David C, Roux C (2010) Osteoporosis and mortality. Joint Bone Spine 77:S107–S112
Stambler I, Jin K, Lederman S, Barzilai N, Olshansky SJ, Omokaro E, Barratt J, Anisimov VN, Rattan S, Yang S (2018) Aging health and R&D for healthy longevity must be included into the WHO work program. Aging Dis 9(2):331–333
Laroche M, Pécourneau V, Blain H, Breuil V, Chapurlat R, Cortet B, Sutter B, Degboe Y (2017) Osteoporosis and ischemic cardiovascular disease. Joint Bone Spine 84(4):427–432
Szekanecz Z, Kerekes G, Kardos Z, Baráth Z, Tamási L (2016) Mechanisms of inflammatory atherosclerosis in rheumatoid arthritis. Curr Immunol Rev 12(1):35–46
Shimizu H, Nakagami H, Osako MK, Hanayama R, Kunugiza Y, Kizawa T, Tomita T, Yoshikawa H, Ogihara T, Morishita R (2008) Angiotensin II accelerates osteoporosis by activating osteoclasts. FASEB J 22(7):2465–2475
Sage AP, Lu J, Atti E, Tetradis S, Ascenzi MG, Adams DJ, Demer LL, Tintut Y (2011) Hyperlipidemia induces resistance to PTH bone anabolism in mice via oxidized lipids. J Bone Miner Res 26(6):1197–1206
Tarakida A, Iino K, Abe K, Taniguchi R, Higuchi T, Mizunuma H, Nakaji S (2011) Hypercholesterolemia accelerates bone loss in postmenopausal women. Climacteric 14(1):105–111
Lampropoulos CE, Papaioannou I, D’cruz DP (2012) Osteoporosis—a risk factor for cardiovascular disease? Nat Rev Rheumatol 8(10):587–598
Varma R, Aronow WS, Basis Y, Singh T, Kalapatapu K, Weiss MB, Pucillo AL, Monsen CE (2008) Relation of bone mineral density to frequency of coronary heart disease. Am J Cardiol 101(8):1103–1104
Erbilen E, Yazici S, Özhan H, Bulur S, Ordu S, Yazici M (2007) Relationship between angiographically documented coronary artery disease and low bone mass in men. Circ J 71(7):1095–1098
Sinnott B, Syed I, Sevrukov A, Barengolts E (2006) Coronary calcification and osteoporosis in men and postmenopausal women are independent processes associated with aging. Calcif Tissue Int 78(4):195–202
Tekin GO, Kekilli E, Yagmur J, Uckan A, Yagmur C, Aksoy Y, Turhan H, Yetkin E (2008) Evaluation of cardiovascular risk factors and bone mineral density in post menopausal women undergoing coronary angiography. Int J Cardiol 131(1):66–69
Ye C, Xu M, Wang S, Jiang S, Chen X, Zhou X, He R (2016) Decreased bone mineral density is an independent predictor for the development of atherosclerosis: a systematic review and meta-analysis. PLoS One 11(5):e0154740
Moher D, Liberati A, Tetzlaff J, Altman DG, Group P (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med 6(7):e1000097
Stang A (2010) Critical evaluation of the Newcastle-Ottawa scale for the assessment of the quality of nonrandomized studies in meta-analyses. Eur J Epidemiol 25(9):603–605
Von Elm E, Altman DG, Egger M, Pocock SJ, Gøtzsche PC, Vandenbroucke JP, Initiative S (2014) The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. Int J Surg 12(12):1495–1499
Jüni P, Witschi A, Bloch R, Egger M (1999) The hazards of scoring the quality of clinical trials for meta-analysis. JAMA 282(11):1054–1060
Marcovitz PA, Tran HH, Franklin BA, O’Neill WW, Yerkey M, Boura J, Kleerekoper M, Dickinson CZ (2005) Usefulness of bone mineral density to predict significant coronary artery disease. Am J Cardiol 96(8):1059–1063
Beer S, Saely C, Hoefle G, Rein P, Vonbank A, Breuss J, Gaensbacher B, Muendlein A, Drexel H (2010) Low bone mineral density is not associated with angiographically determined coronary atherosclerosis in men. Osteoporos Int 21(10):1695–1701
Hajsadeghi S, Khamseh M-E, Larijani B, Abedin B, Vakili-Zarch A, Meysamie A-P, Yazdanpanah F (2011) Bone mineral density and coronary atherosclerosis. J Saudi Heart Assoc 23(3):143–146
Iranpour D, Pourbehi M, Afroozandeh M, Davoodi N, Bidel-Khoshbakht S, Nabipour I, Javadi H, Seyedabad M, Assadi M (2014) Bone mineral density is not related to angiographically diagnosed coronary artery disease. Hell J Nucl Med
Alissa EM, Alnahdi WA, Alama N, Ferns GA (2015) Bone mineral density and cardiovascular risk factors in postmenopausal women with coronary artery disease. BoneKEy reports 4
Liu N, Chen J, Zhang K, Tang Z (2016) A community-based study of the relationship between coronary artery disease and osteoporosis in Chinese postmenopausal women. Coron Artery Dis 27(1):59–64
Alan B, Akpolat V, Aktan A, Alan S (2016) Relationship between osteopenic syndrome and severity of coronary artery disease detected with coronary angiography and Gensini score in men. Clin Interv Aging 11:377
Guan X-q, Xue Y-j, Wang J, Ma J, Li Y-c, Zheng C, Wu S-z (2018) low bone mineral density is associated with global coronary atherosclerotic plaque burden in stable angina patients. Clin Interv Aging 13:1475
Samelson EJ, Kiel DP, Broe KE, Zhang Y, Cupples LA, Hannan MT, Wilson PW, Levy D, Williams SA, Vaccarino V (2004) Metacarpal cortical area and risk of coronary heart disease: the Framingham study. Am J Epidemiol 159(6):589–595
Veronese N, Stubbs B, Crepaldi G, Solmi M, Cooper C, Harvey NC, Reginster JY, Rizzoli R, Civitelli R, Schofield P (2017) Relationship between low bone mineral density and fractures with incident cardiovascular disease: a systematic review and meta-analysis. J Bone Miner Res 32(5):1126–1135
Wu M, Rementer C, Giachelli CM (2013) Vascular calcification: an update on mechanisms and challenges in treatment. Calcif Tissue Int 93(4):365–373
Doherty TM, Asotra K, Fitzpatrick LA, Qiao J-H, Wilkin DJ, Detrano RC, Dunstan CR, Shah PK, Rajavashisth TB (2003) Calcification in atherosclerosis: bone biology and chronic inflammation at the arterial crossroads. Proc Natl Acad Sci 100(20):11201–11206
Persy V, D’Haese P (2009) Vascular calcification and bone disease: the calcification paradox. Trends Mol Med 15(9):405–416
Mao P-J, Zhang C, Tang L, Xian Y-Q, Li Y-S, Wang W-D, Zhu X-H, Qiu H-L, He J, Zhou Y-H (2013) Effect of calcium or vitamin D supplementation on vascular outcomes: a meta-analysis of randomized controlled trials. Int J Cardiol 169(2):106–111
Lewis JR, Radavelli-Bagatini S, Rejnmark L, Chen JS, Simpson JM, Lappe JM, Mosekilde L, Prentice RL, Prince RL (2015) The effects of calcium supplementation on verified coronary heart disease hospitalization and death in postmenopausal women: a collaborative meta-analysis of randomized controlled trials. J Bone Miner Res 30(1):165–175
An T, Hao J, Sun S, Li R, Yang M, Cheng G, Zou M (2017) Efficacy of statins for osteoporosis: a systematic review and meta-analysis. Osteoporos Int 28(1):47–57
Liu J, Zhu L-P, Yang X-L, Huang H-L, Ye D-Q (2013) HMG-CoA reductase inhibitors (statins) and bone mineral density: a meta-analysis. Bone 54(1):151–156
Yue J, Zhang X, Dong B, Yang M (2010) Statins and bone health in postmenopausal women: a systematic review of randomized controlled trials. Menopause 17(5):1071–1079
Peterson RA, Brown SP (2005) On the use of beta coefficients in meta-analysis. J Appl Psychol 90(1):175–181
Rajzbaum G, Bézie Y (2006) Postmenopausal osteoporosis and atheroma. Joint Bone Spine 73(6):661–666
Funding
This work was supported by a grant from a project supported by the National Natural Science Foundation of China (81503627), First-class Discipline Open Fund of Chinese Medicine (2018ZYX02), and Scientific Research Project of Hunan Provincial Department of Education (18K070).
Author information
Authors and Affiliations
Contributions
Hao Liang conceived and designed the research. Hao Liang and Yonghui Zhang performed the statistical analysis. Hao Liang drafted the manuscript. Bing He and Yonghui Zhang made the critical revision of the manuscript in key intellectual content. Bing He and Haijiao Wang acquired the data and performed the methodological quality assessment.
Corresponding author
Ethics declarations
Conflicts of interests
None.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Zhang, Y., He, B., Wang, H. et al. Associations between bone mineral density and coronary artery disease: a meta-analysis of cross-sectional studies. Arch Osteoporos 15, 24 (2020). https://doi.org/10.1007/s11657-020-0691-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11657-020-0691-1