Abstract
Summary
This study determines outcomes and costs of similar hip fracture patients that were discharged from hospital to a rehabilitation facility or to the community within 1 year. Community patients had worse outcomes and lower costs compared to rehabilitation facility patients. This study contributes to understanding hip fracture quality of care.
Purpose
The purpose of this study is to determine the impact on mortality and rehospitalization, as well as health system cost, of similar hip fracture patients being discharged to an inpatient rehabilitation facility or directly to the community within 1 year in Ontario, Canada.
Methods
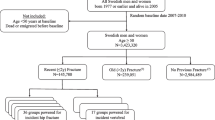
This was a retrospective study of a propensity-matched cohort completed from the health system perspective. Administrative databases were used to identify and match two groups of older adults (total n = 18,773) discharged alive from acute care for hip fracture repair: patients discharged to inpatient rehabilitation were matched to patients discharged to the community.
Results
A higher proportion of patients discharged to the community (27–42%) died or were rehospitalized (SDhighipr = 0.21, SDlowipr = 0.33) and had substantially lower health system costs (SDhighipr = 0.65, SDlowipr = 0.42) up to 1 year post-acute discharge compared to similar patients discharged to inpatient rehabilitation facilities (IPR) (10–11%).
Conclusions
This study demonstrates that similar hip fracture patients are discharged to different post-acute settings (i.e., home-based rehabilitation and inpatient rehabilitation) and have different outcomes, thereby calling into question the appropriateness of post-acute rehabilitation delivery in Ontario, Canada. Future research should focus on determining how trade-offs in resource allocation between settings would impact patient outcomes.
Similar content being viewed by others
References
Cooper C, Campion G, Melton LJ (1992) Hip fractures in the elderly: a world-wide projection. Osteoporos Int 2(6):285–289
Stevens JA, Rudd RA (2013) The impact of decreasing U.S. hip fracture rates on future hip fracture estimates. Osteoporos Int 24(10):2725–2728
Brown JP, Josse RG (2002) Clinical practice guidelines for the diagnosis and management of osteoporosis in Canada. Can Med Assoc J 167(10):S1–S34
Magaziner J et al (2000) Recovery from hip fracture in eight areas of function. J Gerontol A Biol Sci Med Sci 55(9):M498–M507
Nikitovic M et al (2013) Direct health-care costs attributed to hip fractures among seniors: a matched cohort study. Osteoporos Int 24:659–669
Stukel TA et al (2012) Association of hospital spending intensity with mortality and readmission rates in Ontario hospitals. J Am Medical Assoc 10:1037–1045
Haentjens P et al (2001) The economic cost of hip fractures among elderly women. A one-year, prospective, observational cohort study with matched-pair analysis. Belgian Hip Fracture Study Group. J Bone Joint Surg Am 4:493–500
Pasco JA et al (2005) The human cost of fracture. Osteoporos Int 16(12):2046–2052
Norton R et al (2000) Declines in physical functioning attributable to hip fracture among older people: a follow-up study of case control participants. Disabil Rehabil 22(8):345–351
Dai K et al (2007) Estimation of resource utilization associated with osteoporotic hip fracture and level of post-acute care in China. Curr Med Res Opin 23(12):2937–2943
Health Quality Ontario and Ontario Ministry of Health and Long Term Care. Quality-based procedures: clinical handbook for hip fracture. Health Quality Ontario and Ministry of Ontario Health and Long-Term Care, Editors. 2013, Government of Ontario: http://health.gov.on.ca/en/pro/programs/ecfa/docs/qbp_hipfracture.pdf. p. 1–79
National-Institute-for-Health-and-Clinical-Excellence. Hip fracture in adults. 2012: https://www.nice.org.uk/guidance/qs16/resources/hip-fracture-in-adults-2098488670405
Scotland Intercollegiate Guidelines Network: Part of NHS Quality Improvement Scotland (2009) Management of hip fracture in older people: a national clinical guideline. Edinburgh, Scotland, p 1–45. http://www.sign.ac.uk/assets/sign111.pdf
National Institute for Health and Clinical Excellence (2011) NICE clinical guideline: The management of hip fractures in adults. National Clinical Guideline Centre, NICE, London
Bradley EH et al (2005) Quality improvement efforts and hospital performance: rates of beta-blocker prescription after acute myocardial infraction. Med Care 43:282–292
Drew S et al (2014) Describing variation in the delivery of secondary fracture prevention after hip fracture: an overview of 11 hospitals within one regional area in England. Osteoporos Int 25(10):2427–2433
Aharanoff G et al (2004) Predictors of discharge to a skilled nursing facility following hip fracture surgery in New York State. Gerontology 50:298–302
Pitzul, K.B., et al., Post-acute pathways among hip fracture patients: a system-level analysis. BMC Health Serv Res, 2016. 16(275)
Buntin MB et al (2010) Medicare spending and outcomes after postacute care for stroke and hip fracture. Med Care 48:776–784
Ghazipura M (2013) Community versus inpatient rehabilitation in hip fracture patients: a rapid review. Health Quality Ontario, Toronto, pp 1–20
Edgren J et al (2015) Effects of a home-based physical rehabilitation program on physical disability after hip fracture: a randomized controlled trial. J Am Directors Assoc 16(4):351–357
Latham NK et al (2014) Effect of a home-based exercise program on functional recovery following rehabilitation after hip fracture. J Am Med Assoc 311(7):700–708
Government-of-Ontario. Facts about Ontario. 2013 November 11th, 2013]
Chesworth BM et al (2001) Home care after hip fracture in a health planning region. Canadian Public Health Review 92(5):380–384
ICES. Health services data. 2013 November 12th 2013]
Austin PC (2011) An introduction to propensity score methods for reducing the effects of confounding in observational studies. Multivar Behav Res 46:399–424
Pollock FH et al (2015) Readmission within 30 days of discharge after hip fracture care. Orthopedics 38(1):e7–13
Heyes GJ et al (2015) Predictors for readmission up to 1 year following hip fracture. Archives of Trauma Research 4(2):e27123
Hu F et al (2012) Preoperative predictors for mortality following hip fracture surgery: a systematic review and meta-analysis. Injury 43(6):676–685
Khan MA et al (2012) Causes and predictors of early re-admission after surgery for a fracture of the hip. British Journal of Bone and Joint Surgery 94(5):690–697
French DD et al (2008) Rehospitalization after hip fracture: predictors and prognosis from a national veterans study. J Am Geriatric Soc 56(4):705–710
Teixeira A et al (2009) Outcomes in older patients after surgical treatment for hip fracture: a new approach to characterise the link between readmissions and the surgical stay. Age Ageing 38(5):584–589
Radinovic K et al (2014) Estimating the effect of incident delirium on short-term outcomes in aged hip fracture patients through propensity score analysis. Geriatr Gerontol Int 15(7):848–855
Austin PC (2010) Optimal caliper widths for propensity-score matching when estimating differences in means and differences in proportions in observational studies. Pharm Stat 10:150–161
Wodchis, W.P., et al., Guidelines on person-level costing using administrative databases in Ontario, Health-System-Performance-Research-Network, Editor. 2013: http://www.hsprn.ca/activities/papers/hsprn_case_costing_vol1_2013.pdf
Austin PC (2009) Using the standardized difference to compare the prevalence of a binary variable between two groups in observational research. Commun Stat-Simul Comput 38(6):1228–1234
Rosenbaum PR (2002) Observational studies. Springer Verlag, New York
Peng L-N et al (2016) Survival benefits of post-acute care for older patients with hip fractures in Taiwan: a 5-year prospective cohort study. Geriatr Gerontol Int 16:28–36
Leland NE et al (2015) An examination of the first 30 days after patients are discharged to the community from hip fracture postacute care. Med Care 53:879–887
Cremieux PY, Ouellette P, Pilon C (1999) Health care spending as determinants of health outcomes. Health Econ 8:627–639
Skinner, J., Causes and consequences of regional variations in health care. In Handbook of health economics, M. Pauly, T. McGuire, and P.P. Barros, Editors. 2011, Elsevier B.C.: New York
Doig, E. and D. Amsters, The efficacy of community rehabilitation for aged clients after stroke—a review of the literature, Q. Health, Editor. 2006: Queensland, Australia p 1-34
Medical Advisory Secretariat, Physiotherapy rehabilitation after total knee or hip replacement: an evidence-based analysis. in Ontario Health Technology Assessment Series. 2005. p. 1–91
Health Quality Ontario and Ministry of Health and Long-Term Care, Quality-based procedures: clinical handbook for primary hip and knee replacement. H.Q. Ontario, Editor. 2013, Health Quality Ontario: Toronto p 95
Reznick L (2013) Research and data systems to promote equal access to postacute rehabilitation. Israel J Health Policy Res 2(1):28
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None.
Additional information
Sponsor’s Role
The opinions, results, and conclusions reported in this paper are those of the author and are independent from the funding sources. No endorsement by ICES or the Ontario MOHLTC is intended or should be inferred.
Electronic supplementary material
Supplementary Table S1
(DOC 30 kb)
Supplementary Table S2
(DOC 40 kb)
Supplementary Table S3
(DOC 139 kb)
Supplementary Table S4
(DOC 36 kb)
Rights and permissions
About this article
Cite this article
Pitzul, K.B., Wodchis, W.P., Kreder, H.J. et al. Discharge destination following hip fracture: comparative effectiveness and cost analyses. Arch Osteoporos 12, 87 (2017). https://doi.org/10.1007/s11657-017-0382-8
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11657-017-0382-8