Abstract
Objective
To evaluate the effects of auricular acupoint bloodletting (AB) and auricular acupressure (AA) on sleep quality and the levels of melatonin (MT), glutamic acid (Glu), and γ -aminobutyric acid (GABA) in college students with primary insomnia, and to explore the possible mechanism.
Methods
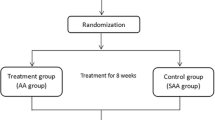
Totally 74 college students at Hebei University of Chinese Medicine with primary insomnia were selected from October 2019 to October 2020. All patients were assigned to AB+AA group (37 cases, received combination of AB and AA) and AA group (37 cases, received only AA on the same acupoints) by a random number table. Each group was treated twice a week for 4 weeks. The Pittsburgh Sleep Quality Index (PSQI) score, Chinese medicine (CM) syndrome score, total effective rate, serum concentrations of MT, Glu, and GABA, and Glu/GABA ratio were compared between the two groups after treatment and at follow-up. The safety of therapy was also evaluated.
Results
After 4-week treatment, the total scores of PSQI, each PSQI component score, and the CM syndrome scores in both groups all decreased (P<0.05); the serum MT concentrations in both groups all increased (P<0.05). The concentrations of Glu and GABA in the AB+AA group were significantly higher than those in the AA group after treatment (P<0.05). However, there was no significant difference in the ratio of Glu/GABA in both groups before and after treatment (P>0.05). At follow-up, the CM syndrome score in the AB+AA group was significantly lower than that in the AA group (P<0.05). There was no significant difference between the two groups in total effective rates and adverse events (P>0.05).
Conclusions
Both AB+AA and AA can relieve insomnia symptoms, but a stronger long-term effect were observed for AB+AA. AB+AA can promote the secretion of MT, increase the levels of Glu and GABA more effective than AA, and regulate their imbalance, and thus it may be benificial for treating insomnia.
Similar content being viewed by others
References
Yin X, Gou M, Xu J, Dong B, Yin P, Masquelin F, et al. Efficacy and safety of acupuncture treatment on primary insomnia: a randomized controlled trial. Sleep Med 2017;37:193–200.
Carotenuto M, Gallai B, Parisi L, Roccella M, Esposito M. Acupressure therapy for insomnia in adolescents: a polysomnographic study. Neuropsychiatr Dis Treat 2013;9:157–162.
Chinese Sleep Research Society. Healthy sleep, intelligence and brain protection—2019 World Sleep Day Chinese theme release [EB/OL]. Accessed March 16, 2019. Available at http://www.zgsmyjh.org.html.
Miller MB, Deroche CB, Freeman LK, Park CJ, Hall NA, Sahota PK, et al. Cognitive behavioral therapy for insomnia among young adults who are actively drinking: a randomized pilot trial. Sleep 2021;44:zsaa171.
Edinger JD, Arnedt JT, Bertisch SM, Carney CE, Harrington JJ, Lichstein KL, et al. Behavioral and psychological treatments for chronic insomnia disorder in adults: an American Academy of Sleep Medicine clinical practice guideline. J Clin Sleep Med 2021;17:255–262.
de Zambotti M, Goldstone A, Colrain IM, Baker FC. Insomnia disorder in adolescence: diagnosis, impact, and treatment. Sleep Med Rev 2018;39:12–24.
Zhang P, Li YP, Wu HJ, Zhao ZX. Guidelines for diagnosis and treatment of insomnia in Chinese adults (2017). Chin J Neurol (Chin) 2018;51:324–335.
Huang J, Shen M, Qin X, Huang Y. Effectiveness of auricular acupuncture for insomnia: an overview of systematic reviews. Evid Based Complement Alternat Med 2020;2020:6920902.
Vieira A, Reis AM, Matos LC, Machado J, Moreira A. Does auriculotherapy have therapeutic effectiveness? An overview of systematic reviews. Complement Ther Clin Pract 2018;33:61–70.
Tan HJ, Lan Y, Wu FS, Zhang HD, Wu L, Wu X, et al. Auricular acupuncture for primary insomnia: a systematic review based on GRADE system. Chin Acupunct Moxibust (Chin) 2014;34:726–730.
Soltani S, Chauvette S, Bukhtiyarova O, Lina JM, Dubé J, Seigneur J, et al. Sleep-wake cycle in young and older mice. Front Syst Neurosci 2019;13:51.
Zhang TB, Hou PG. Progress on physiological activities of melatonin and its mechanisms. J Qiqihar Univ Med (Chin) 2015;36:1671–1673.
Sun YN, Qiao T, Zhang LD. Effect and mechanism comment of traditional Chinese medicine on insomnia. Chin Archiv Tradit Chin Med (Chin) 2017;35:1873–1876.
Mental Medical Branch of Chinese Medical Association. Chinese classification and diagnostic criteria of mental disorders, 3rd ed. Jinan: Shandong Science and Technology Press;2001:112–113.
National Administration of Traditional Chinese Medicine. Diagnostic, syndrome classification and curative effect evaluation of insomnia—Chinese medicine industry standard of the People’s Republic of China, diagnosis and curative effect of Chinese medicine internal diseases (ZY/T001.1-94). J Liaoning Univ Chin Med (Chin) 2016;18:247.
Backhaus J, Junghanns K, Broocks A, Riemann D, Hohagen F. Test-retest reliability and validity of the Pittsburgh Sleep Quality Index in primary insomnia. J Psychosom Res 2002;53:737–740.
Lv YQ, Feng GS. Sample size estimation methods in medical research. Chron Pathematol J (Chin) 2016;17:359–361.
Li PY. Ear needle bloodlettings plus auricular plaster therapy in treating insomnia [Dissertation]. Guangzhou: Guangzhou University of Chinese Medicine;2010.
General Administration of Quality Supervision, Inspection and Quarantine of the People’s Republic of China, Standardization Administration of the People’s Republic of China, GB/T 13734-2008. Nomenclature and location of auricular points. Beijing: China Standards Press;2008.
Zheng B, Li M, Wang KL, Lv Y. Analysis of the reliability and validity of the Chinese version of Pittsburgh Sleep Quality Index among medical college students. J Peking Univ (Health Sci, Chin) 2016;48:424–428.
Zheng XY, ed. Guidelines for clinical research of new drugs of traditional Chinese medicine (trial). Beijing: China Medical Science and Technology Press;2002:109.
Bai J, Wang D, Liu Z, Zhang J, Liu L, Han Y. Simultaneous determination of amino acid and monoamine neurotransmitters in serum by high performance liquid chromatography coupled with precolumn derivatization. Chin J Chromatography (Chin) 2020;38:923–928.
Lu L, Liu J, Mo S, Chen H. The effect of auricular plaster therapy on insomnia in patients with rheumatoid arthritis. Med Acupunct 2019;31:130–133.
Mysliwiec V, Martin JL, Ulmer CS, Chowdhuri S, Brock MS, Spevak C, et al. The management of chronic insomnia disorder and obstructive sleep apnea: synopsis of the 2019 U.S. Department of Veterans Affairs and U.S. Department of Defense clinical practice guidelines. Ann Intern Med 2020;172:325–336.
Ran WZ, Chen ZG. Necessity of classification of collateral level from the perspective of “long-term illness involving collaterals”. J Basic Chin Med (Chin) 2019; 25:883–884,981.
Cao SQ, Shen YP, Cai WG, Chen HG. Analysis of the superficial venulles theory and pricking blood therapy in Inner Canon of Huangdi. China J Tradit Chin Med Pharm (Chin) 2015;30:341–344.
Wang Z, Ma W, eds. Encyclopedia of Chinese pricking blood therapy. Hefei: Anhui Science and Technology Press;2017:54–74.
Bao N, Wang Q, Sun YH, Yang K, Kong LJ, Sun YH, et al. Rule of clinical application of auricular acupuncture based on data mining. Acupunct Res (Chin) 2017;42:90–94.
Ye MZ, Hu ZC. Integration and development of ear apex in auricular point therapy. Shanghai J Acupunct Moxibust (Chin) 2021;40:777–780.
Lan Y, Wu X, Wu L, Zhang HD, Liang FR. Combination of ancient and modern theories on the selection of auricular points for insomnia. Lishizhen Med Mater Med Res (Chin) 2015;26:426–428.
Chen H, She YF, Gao YY, Song XD, Fan XS, Shi XL, et al. Comparative study on the academic thought of bloodletting for expelling pathogens between Jin-Yuan Dynasties and Ming-Qing Dynasties. Chin Acupunct Moxibust (Chin) 2021;41:813–817.
Song YJ, Fan XS, Li MY, Zhang J, Geng JR, Liang X, et al. Treatment of acne vulgaris with auricular acupoint pricking-bloodletting plus auricular point sticking therapy: a randomized controlled study. J Acupunct Tuina Sci (Chin) 2019;17:196–202.
Huang XY, Zhu JM, Zhan YC, Li BK. Study on sleep quality of Chinese college students based on PSQI and cognition of influencing factors of TCM. World J Sleep Med (Chin) 2019;6:891–894.
Meng Q, Zhang J, Kang J, Wu Y. Effects of sound environment on the sleep of college students in China. Sci Total Environ 2020;705:135794.
Wang XQ, Qin S, Wu WZ, Liu CY, Shang HT, Wan QY, et al. Effect of electroacupuncture on serum melatonin and dopamine in aged insomnia. Chin Acupunct Moxibust (Chin) 2021;41:501–504.
Zheng XN, Wu XF, Guo X, Xie LN, Xie ZQ, Wei XR, et al. Manual acupuncture stimulation of paired acupoints can relieve sleep disorder possibly by upregulating pineal melatonin protein and its receptor mRNA levels in the suprachiasmatic nucleus in insomnia rats. Acupunct Res (Chin) 2018;43:360–364.
Luppi PH, Clément O, Garcia SV, Brischoux F, Fort P. New aspects in the pathophysiology of rapid eye movement sleep behavior disorder: the potential role of glutamate, gamma-aminobutyric acid, and glycine. Sleep Med 2013;14:714–718.
Gvilia I. Underlying brain mechanisms that regulate sleep-wakefulness cycles. Int Rev Neurobiol 2010;93:1–21.
Author information
Authors and Affiliations
Corresponding author
Additional information
Conflict of Interest
The authors declare that they have no conflict of interest.
Author Contributions
Chen H and She YF were involved in the study design and writing the manuscript. Shi XL helped to guide the trial design and revise the manuscript. Yuan XR and Huo YX were responsible for recruiting patients. Zhang MJ and Wu JA contributed to the study operation and data analysis. Sun H and Liu DN were responsible for the evaluation of outcomes. All the authors have read and approved the final manuscript.
Supported by the College Student Innovation and Entrepreneurship Training Program in Hebei Province, China (No. S201914432019S)
Electronic Supplementary Material
11655_2022_3581_MOESM1_ESM.pdf
Effect of Auricular Acupoint Bloodletting plus Auricular Acupressure on Sleep Quality and Neuroendocrine Level in College Students with Primary Insomnia: A Randomized Controlled Trial
Rights and permissions
About this article
Cite this article
Chen, H., Zhang, Mj., Wu, Ja. et al. Effect of Auricular Acupoint Bloodletting plus Auricular Acupressure on Sleep Quality and Neuroendocrine Level in College Students with Primary Insomnia: A Randomized Controlled Trial. Chin. J. Integr. Med. 28, 1096–1104 (2022). https://doi.org/10.1007/s11655-022-3581-0
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11655-022-3581-0